New to This Mommy’s Heart? Check out my story from the beginning here – My PPCM Story
**Warning – Post Contains Graphic Images**
Courage, dear heart.
-C.S. Lewis
Primary graft dysfunction occurs when the left ventricle, right ventricle or both dysfunction within 24 hours of the heart transplant surgery and no obvious cause can be determined. About 10-15% of heart transplant patients experience primary graft dysfunction. There is usually a 50% chance the heart will start working again with no longterm consequences. If the heart doesn’t recover, the patient must be re-listed for transplant.
You didn’t think this surgery would be easy, did you? Haven’t you recognized the reoccurring theme throughout this story.
On the 10th, the day after my surgery, there were several tests to check the heart’s function but there were no significant improvements. Discussions began about putting me back on the transplant list as a 1A. I could not get another total artificial heart so my only options were for this heart to recover or to be retransplanted.
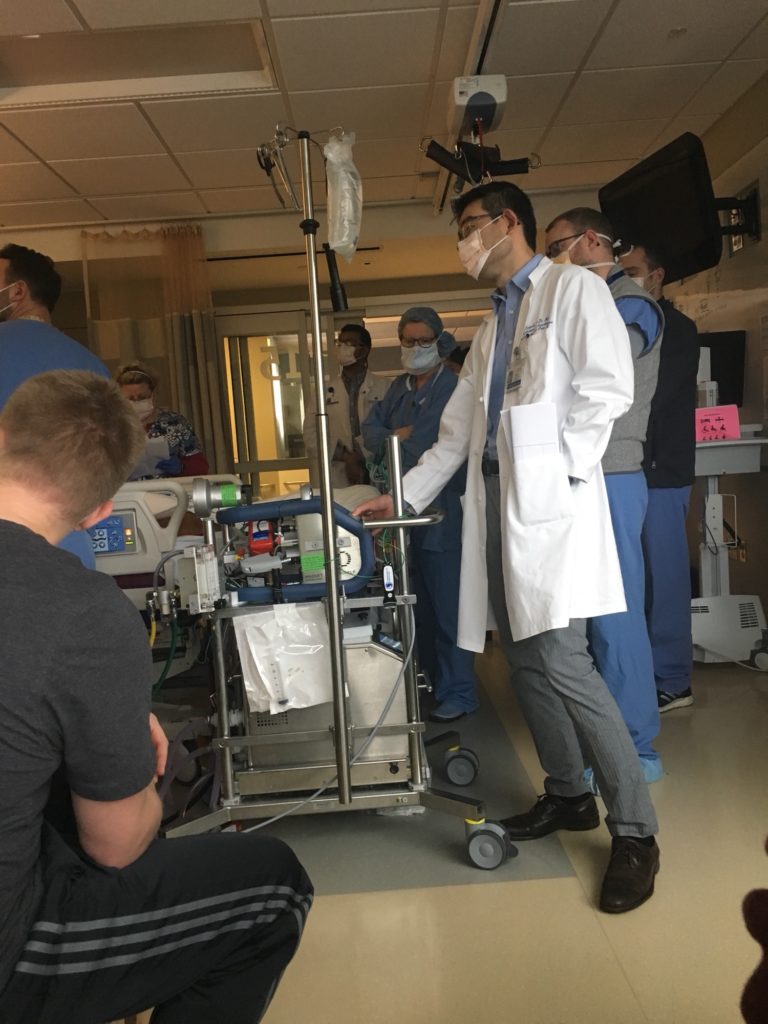
The UWMC staff was so good to my family during this horrible time in our lives. In my husband’s notes, he describes the floor as being very somber after my transplant. My family received many condolences and the nurses brought in food multiple times since they didn’t want to leave my side. I was so lucky to be in their care.
The time after the transplant was the worst for my family. All of the setbacks in my health were leaving them disheartened and not as optimistic about what the future held.
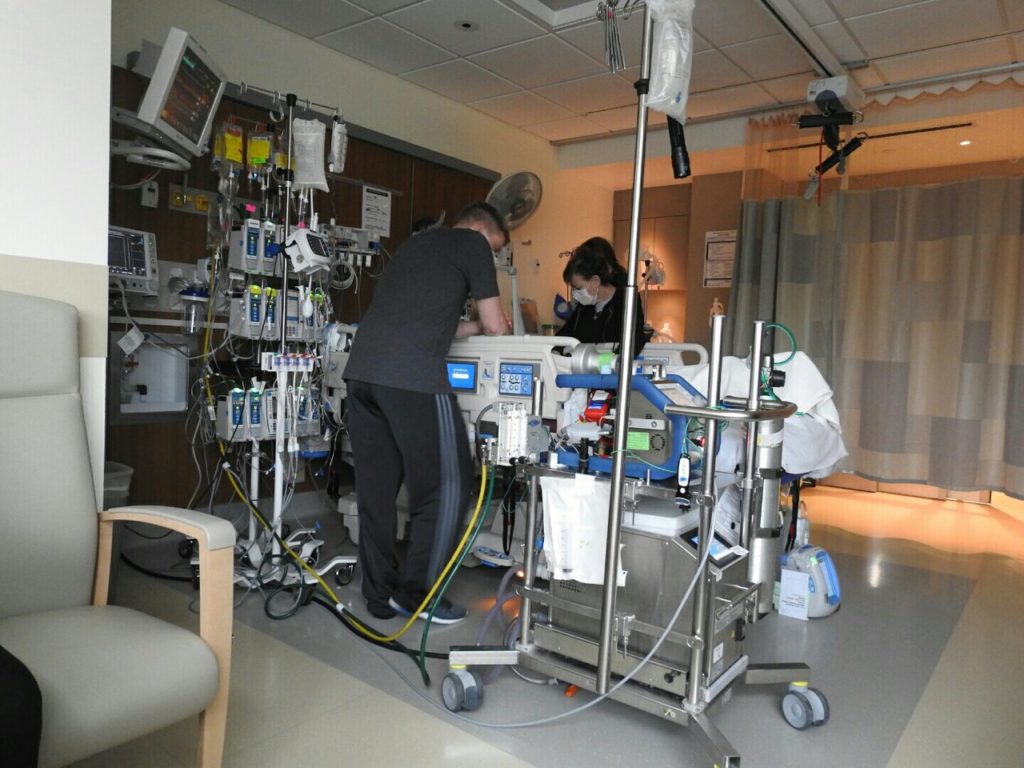
On the 11th, my husband’s family arrived, along with two of his friends from high school. That day they ran more tests to check my heart’s function. Luckily, there were some improvements. My ejection fraction and pulmonary artery pressure were basically normal, so my left ventricle was looking like it could support me off of ECMO. Unfortunately, there was no change with my right ventricle which was still not working well at all.
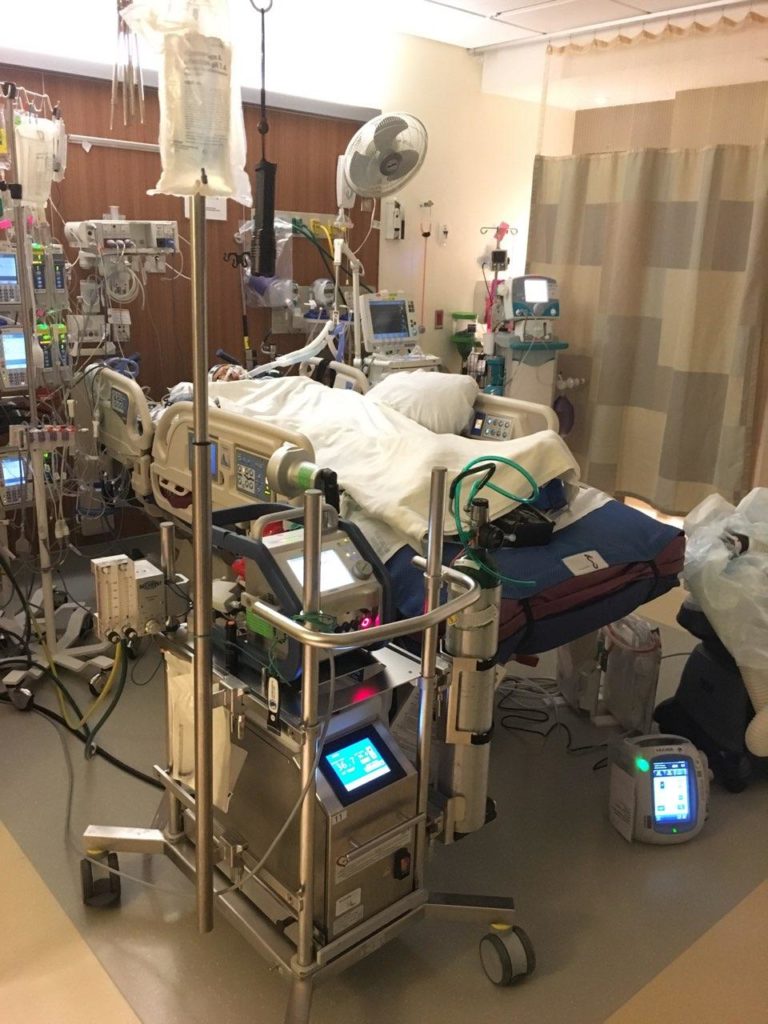
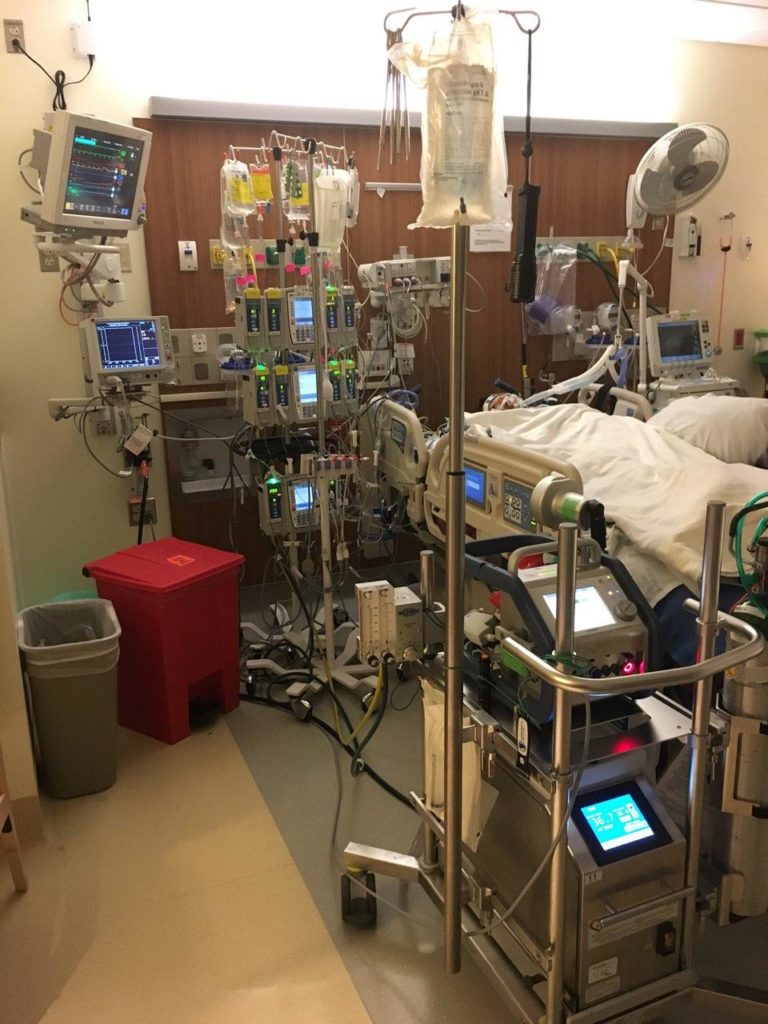
**GRAPHIC IMAGES AHEAD**
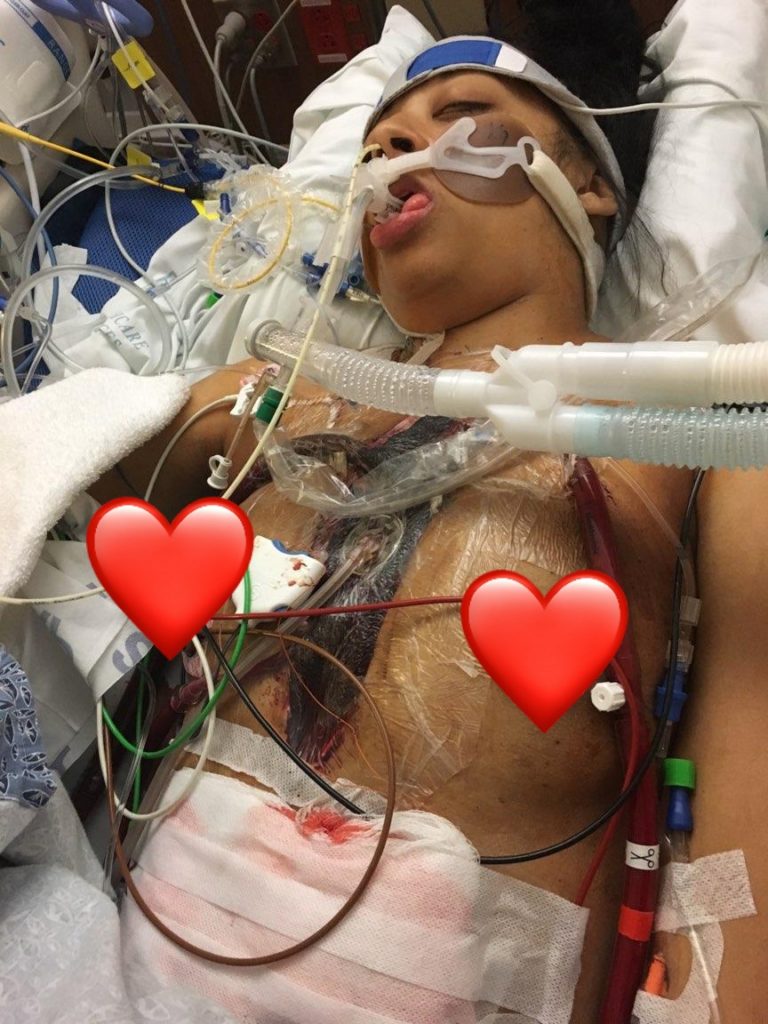

When on ECMO, one of the risks is bleeding. Just like the first time I was on ECMO, I was extremely oozy. I had to receive 3 more units of blood (up to 34 units total for my hospitalization).

On January 12th, I was taken into surgery for a washout. After a f
When they had first started the procedure, the right side of the heart still wasn’t looking good. However, once the wound vac was removed, the right side went back to near normal function. My heart was working so well that they were able to decannulate me from the ECMO. My chest was left open to wait for more swelling to go down but things finally seemed to be heading in the right direction.
I guess the day this happened, we had quite a large group in the waiting room. There was my family, my husband’s family and several of our friends there as well. I’m told there were many tears of joy and relief that I was doing better. ECMO is scary and having to get another transplant was not ideal. I was going to get to keep my heart. Who would have thought I would come out on the positive side of 50/50 odds?
On the 13th, I remained stable throughout. The primary issues at this point were my blood pressure being too high and the amount of fluid I had retained. They were managing my blood pressure by frequently adding and adjusting medications. I was given aggressive diuresis to combat m
They had been cautious with my medications up to this point but on the 13th they finally gave me ATG and tacrolimus.
Medical Terminology
- ATG – anti-thymocyte globulin also known as “Rabbit.” This is an infusion of rabbit antibodies against human T cells. It is used after transplants to reduce the chance of acute rejection.
- Tacrolimus – immunosuppress
e nt drug used to prevent rejection. This is one of the medications I will take for life.
Since I hadn’t had a bowel movement in over a week, my nurse focused on that and diuresis overnight. I ended up having 5-6 bowel movements over the course of the night totaling about 1.5 liters. By the morning I was down several liters in total despite all of my IV infusions.
Have I mentioned what great, amazing, awesome, fantastic angels on Earth nurses are? Another post for another day, but their jobs are so hard physically and emotionally. It takes such a special person to take on that role.
Another TTE was done on the 14th to check my heart function. It showed that, besides being very dry, my left ventricle was normal. My right ventricle still had moderate dysfunction but that is not uncommon following a heart transplant.

On the 15th, I went back in for another surgery. The surgery went well and was thankfully uneventful. They were able to finally close my chest and later that day they were able to extubate me. To be safe, they kept me on a high dose of oxygen overnight but I was swallowing my secretions and talking by the end of the night.
I get weepy when I read this part from my husband’s notes:
When she could finally start to talk she said she loved me…I missed talking to her so much.
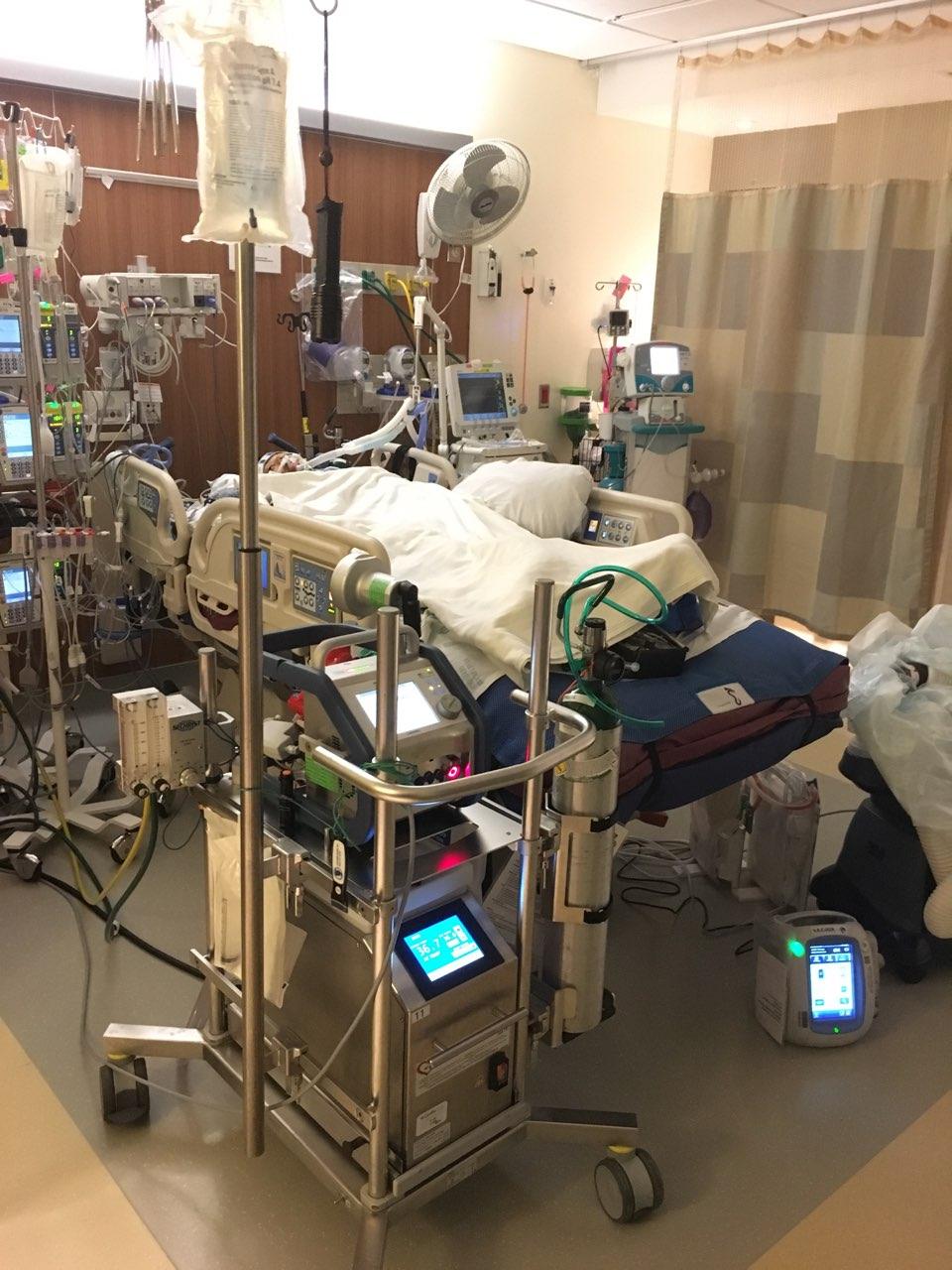
It is wonderful you are doing so well and I pray that continues. I am also a patient at UWMC amd at some point we are hoping for a transplant. I wish you continued success with your new heart.
Thank you, Dana. UWMC is the best! We were really happy with the care I received there. You are in good hands.
Jen, I’ve been following your story since seeing it on the PPCM Facebook group we are in. I was diagnosed a few months before you after having my baby girl and my husband is also army so I feel like we have a sisterhood double time. It’s been such a joy to see you get healthy and come back after EVERYTHING y’all went through. Thank you for sharing your story and raising awareness for this awful, hidden disease. Maybe one day we will cross paths in this army life lol. Much love to you and your family.
Thanks, Beth! Honestly being in the Army for this experience has been such a blessing with all of the costs associated with this journey. Here is to both of us staying healthy and happy mamas for our babies!
When it involves conquering a new proficiency, the venture is never utterly finished without a significant grasp of the principles. This echoes especially true in the realm of language services, like Russian-English interpretation. This distinctive capacity is not only about understanding both languages; rather, it’s a thorough knowledge that requires lexical precision, cultural understanding, and situational knowledge.
Studying Russian translation can often be a challenging task. The Russian language, abundant in its own individual syntax and grammar laws, must be masterfully bridged with the English language, taking heed to preserve the original message and all its embedded nuances. The center of understanding this translation process lies not only in word-for-word translation but also in understanding the cultural differences that form the way we use and comprehend language.
Effective Russian translation incorporates multiple stages, such as decoding the source language, understanding the meaning, and then re-encoding that meaning using the proper vocabulary and structure in the target language, all the while maintaining the original message’s tone, style, and intention. It’s a tender process that demands a deep and insightful understanding of both languages.
Utilising Professional Techniques for Russian Translation
A key component of Russian translation is being aware of the distinct text types and niches. The demands of corporate translation will hugely differ from literary translation – each necessitates a diverse set of skills and in-depth knowledge. But irrespective of the text type, understanding the complexities of both Russian and English remains pivotal.
Of course, technology can be a valuable ally in the translation process. Computer-aided tools and online dictionaries can robotize some aspects of the job. However, they should not supplant human translators. The nature of language is naturally human, laden with sentiment, cultural connotations, and situational context. While these nuances might be noticeable to a native speaker, they can simply be missed by a machine translator.
The key to top-notch Russian-English translation involves merging both these elements. Let technology assist the process, but guide it by human interpretation and comprehension. By considering each piece’s exact nature and utilising the right mix of human skills and technology, one can provide comprehensive, exact, and culturally conscious Russian translation.
Navigating your way through Russian translation is without doubt complex, but with a solid understanding of both linguistics and cultural nuances, success is just around the corner. As you commence on this fascinating journey through language, remember, each word, phrase, and sentence is a code to unravel another dimension of understanding and communication. Embrace this key, and open up a new world of possibilities.
Discovering the massive potential of Russian-English translation enriches your perspective, expands your skills, and zooms in on the global demand for expert Russian translation. Put money in mastering this art and prepare to impress with your proficiency, accuracy, and cultural understanding.
follow https://russian-translation.co.uk/
Flirt finder is a great solution to find compatible partners who are searching for fun.
The web-based platform enables you to connect with interesting individuals from anywhere, at any time.
Become a part of our online community today and begin your quest to discovering the perfect match with our dating platform.
For those exploring mature online dating, Adult Flirt Finder is the ideal platform. This online dating site is tailored to adults looking for love and companionship.
Create an authentic profile, engage in thoughtful conversations, and take your first steps with Adult Flirt Finder. Explore digital romance in a mature and meaningful way.
Прогон сайта с использованием программы “Хрумер” – это способ автоматизированного продвижения ресурса в поисковых системах. Этот софт позволяет оптимизировать сайт с точки зрения SEO, повышая его видимость и рейтинг в выдаче поисковых систем.
Хрумер способен выполнять множество задач, таких как автоматическое размещение комментариев, создание форумных постов, а также генерацию большого количества обратных ссылок. Эти методы могут привести к быстрому увеличению посещаемости сайта, однако их надо использовать осторожно, так как неправильное применение может привести к санкциям со стороны поисковых систем.
Прогон сайта “Хрумером” требует навыков и знаний в области SEO. Важно помнить, что качество контента и органичность ссылок играют важную роль в ранжировании. Применение Хрумера должно быть частью комплексной стратегии продвижения, а не единственным методом.
Важно также следить за изменениями в алгоритмах поисковых систем, чтобы адаптировать свою стратегию к новым требованиям. В итоге, прогон сайта “Хрумером” может быть полезным инструментом для SEO, но его использование должно быть осмотрительным и в соответствии с лучшими практиками.
Добро пожаловать в нашем сайте, вашего надежного партнера в мире сделать ставку. Мы с гордостью предоставляем вам шанс взять на себя контроль над вашими ставками и увеличить свои перспективы на выигрыш. Наши профессиональные аналитики и эксперты следят за событиями в мире спорта, чтобы обеспечить вас свежими и точными советами.
Почему выбирать нас:
Экспертные прогнозы: Наши специалисты работают не покладая рук, чтобы предоставлять вам предсказания на все популярные виды спорта. Мы знаем, насколько важно получать качественные советы перед тем, как сделать ставку.
Широкий выбор: Мы предлагаем ставки на разнообразные виды спорта, включая соккер, баскет, теннис, мяч и многое другое. Вы можете отбирать из множества событий и наслаждаться азарт на свой вкус.
Советы без оплаты: Мы поддерживаем идею, что каждый должен иметь доступ к полезным советам. Поэтому мы предлагаем бесплатные предсказания, чтобы помочь вам сделать правильные ставки.
Легкость и комфорт: Наш сайт и мобильное приложение разработаны с учетом вашего комфорта. Сделайте ставку буквально за несколько мгновений.
Как начать:
Создайте аккаунт: Создайте свой аккаунт в texttospeech.ru и получите доступ к всем нашим сервисам.
Получайте предсказания: Подписывайтесь на бесплатные советы и получайте свежие советы от наших экспертов.
Сделайте ставку: После того как вы получили полезный совет, сделайте ставку на вашу любимую команду или событие и получайте удовольствие от игры.
Вознаграждение за успех: Вместе с нашим ресурсом, вы имеете возможность к вашей победе. Попробуйте нашу помощь уже сегодня и погружайтесь в мир ставок на спорт во всей его красе!
Добро пожаловать в texttospeech.ru, вашего надежного партнера в мире спортивный тотализатор. Мы с гордостью предоставляем вам возможность взять на себя контроль над вашими ставками и повысить свои шансы на успех. Наши профессиональные аналитики и эксперты следят за событиями в мире спорта, чтобы поддержать вас актуальными и точными советами.
Почему выбирать нас:
Экспертные прогнозы: Наши аналитики работают не покладая рук, чтобы предоставлять вам предсказания на разнообразные виды спорта. Мы знаем, насколько важно получать полезные советы перед тем, как сделать ставку.
Множество вариантов: Мы предлагаем ставки на различные виды спорта, включая соккер, баскетбол, ракетку, мяч и многое другое. Вы можете выбирать из многочисленных событий и погружаться в страсть на свой вкус.
Бесплатные прогнозы: Мы верим, что каждый может получить доступ к качественным прогнозам. Поэтому мы предлагаем бесплатные советы, чтобы помочь вам сделать правильные ставки.
Простота и удобство: Наш веб-сайт и мобильное приложение разработаны с учетом вашего удовольствия. Сделайте ставку всего в несколько кликов.
Как начать:
Зарегистрируйтесь: Создайте свой аккаунт в texttospeech.ru и получите доступ к нашему полному спектру услуг.
Получайте предсказания: Подписывайтесь на бесплатные советы и получайте свежие советы от наших экспертов.
Поставьте свою ставку: После того как вы получили полезный совет, сделайте ставку на команду по душе или событие и наслаждайтесь игры.
Вознаграждение за успех: Вместе с нашим ресурсом, вы владеете ключами к вашей победе. Попробуйте нашу помощь уже сегодня и переживайте в мир спортивных ставок во всей его красе!
Устройство пола – существенный шаг в строительстве. Выравнивание пола дает возможность приобрести ровную основу для последующей отделки.
Мастера осуществляют стяжка пола с оглядкой на всех норм и стандартов. Укладка пола осуществляется с применением современных материалов, которые обеспечивают надежное покрытие и стойкость.
Устройство пола даёт возможность подготовить идеальное основание для разнообразных видов облицовки. В русской столице стяжку пола проводят опытные специалисты.
Машинная штукатурка — современный метод осуществления отделки стен.
Он основан на применении автоматических систем штукатурки, обычно, произведенных в Германии, что обеспечивает раствор подготавливается и наносится на стену автоматически и под давлением.
Машинная штукатурка С подтвержденной гарантией До 32 процентов выгоднее обычной, Можно клеить обои без шпаклевки от кампании mehanizirovannaya-shtukaturka-moscow.ru
В результате, повышается адгезия с поверхностью, а время, потраченное на работу снижается в 5–6 раза, в сравнении с ручной отделкой. За счет механизации и облегчения труда цена механизированной штукатурки становится доступнее, чем в случае традиционного способа.
Для машинной штукатурки применяют смеси, разработанные для механизированной штукатурки, ценовой диапазон ниже чем для ручного нанесения примерно на треть. При определенных навыках специалистов, а кроме того если соблюдаются все технологические стандарты, поверхность после обработки штукатуркой становится совершенно ровной (профессиональные стандарты) и полированной, поэтому, последующая шпатлевка не требуется, что обеспечивает дополнительную экономию средств заказчика.
Группа «Каспий» родилась в конце 2012 года, в Москве, когда Володя Астапчик собрал вокруг себя группу музыкантов-единомышленников. Уже через полгода, летом 2013 года команда, названная «Каспий», дебютировала на фестивалях «Нашествие» и «Доброфест». Мелодичность, драйв и многослойная лирика текстов помогли группе стремительно завоевать Интернет- и офф-лайн аудиторию.
группа каспий
Частично сухая стяжка – строительная операция подготовки полок. Монтаж полусухой стяжки дает возможность получить ровное покрытие для финишной отделки.
оборудование для полусухой стяжки Мы сделаем супер ровную стяжку пола. 7 лет опыта работы От 500 рублей за квадратный метр
Обслуживание полутвёрдой стяжки подразумевает постоянный контроль и устранение недостатков с использованием специализированного оборудования.
Технические средства для полутвёрдой стяжки позволяет осуществить процесс устройства с высокой точностью. Полусухая стяжка полов является отличным решением для создания надежного фундамента для дальнейшей отделки.
1хбет — известная букмекерская компания. Регистрируйтесь на сайте компании и получайте бонусы. Поставьте на свой фаворит. Используйте высокие шансы.
1xbet зеркало рабочее на сегодня прямо
Девушки легкого поведения из Москвы готовы подарить вам незабываемые моменты. Эксклюзивное объявление: мне 18 лет, и я готова подарить тебе невероятный минет в машине. Ощути магию настоящего наслаждения! проститутки карта. Эскорт-леди ждут вашего звонка. Узнайте, что такое настоящее удовлетворение в компании любовниц из столицы.
Восстановление помещения — наша специализация. Исполнение ремонтных услуг в сфере жилья. Мы предлагаем реставрацию дома с гарантированным качеством.
remont-kvartir-brovari.kyiv.ua
https://samye-luchshie-prostitutki-moskvy.top
amoxicillin 250mg cost
MOTOLADY предлагают услуги аренды и проката мотоциклов и скутеров в Хургаде, Эль Гуне и Сахл Хашиш. MOTOLADY – одна из самых популярных компаний по прокату мотоциклов и скутеров. Они предлагают большой выбор транспортных средств по разумным ценам. MOTOLADY компания, специализирующаяся на Прокат мопеда в Эльгуне и Эль Гуне. Они предлагают услуги доставки транспорта в любое удобное для вас место. У нас в наличии различные модели транспортных средств по доступным ценам. Перед арендой транспорта обязательно ознакомьтесь с правилами и требованиями компании, также проверьте наличие страховки и необходимые документы для аренды.
silagra tablets
best over the counter tretinoin cream
canada pharmacy online
stromectol uk buy
baclofen medicine price
augmentin 625 in usa
canadian pharmacy in canada
amoxicillin no script
cheap amoxicillin tablets
Оцифровка архива стоимость — это наше направление. Мы предоставляем услуги цифровизации документов с использованием технологических инноваций. Сотрудничество с нами — это быстрый способ сделать вашу документацию доступной в электронной форме.
prozac from mexico
юридическая помощь бесплатно для всех вопросов о юридических вопросах|Бесплатный юридический совет на разные темы
Юридическая консультация бесплатно для граждан и предприятий по разнообразным вопросам права от юридическая консультация без оплаты: качественное решение вопросов|Получи безвозмездную консультирование от квалифицированных юристов по различным проблемам
Бесплатная юридическая консультация о защите прав на жилье
бесплатная юридическая помощь в москве http://konsultaciya-yurista-499.ru/.
Получите бесплатную консультацию юриста прямо сейчас!
юрист обратный звонок http://www.lawyer-uslugi.ru.
Запросите бесплатную юридическую консультацию Оптимальный способ получить содействие лишних трат на юридические услуги благодаря бесплатной консультации
Как защитить собственные права без затрат на юридические услуги?
Бесплатная юридическая консультация всегда под рукой
Как получить бесплатную юридическую помощь?
Узнавайте свои юридические вопросы быстро с бесплатной консультацией
Не знаете, как поступить? Получите бесплатную юридическую помощь сразу сейчас
Обезопасьте свои права с бесплатной юридической консультацией
Как поступить в сложной юридической ситуации? Получите бесплатную консультацию и решите проблему
Комплексное пояснение правового вопроса с помощью квалифицированных юристов
Как доказать свою правоту? Получите юридическую консультацию на тему бесплатно
Расходы на юридическую помощь не всегда оправданы, узнайте, как получить бесплатную консультацию
Возникла трудная ситуация? Получите бесплатную юридическую поддержку
Юридическая консультация вам доступны бесплатно
Как защитить документы без юриста? Получите бесплатную консультацию и сэкономьте
Нужна юридическая вопроса? Получите бесплатную консультацию от Профессионалов
Экспрессно получите бесплатную юридическую консультацию онлайн с помощью бесплатной юридической консультации
Нужна комплексная юридическая помощь? Получите бесплатную консультацию
Как получить юридическая консультация на любом вопросов
Не останавливайтесь – получите бесплатную содействие от лучших юристов
виртуальный хостинг
Когда речь заходит о создании своего собственного сайта, выбор хостинга играет огромную роль. Ведь именно хостинг будет определять доступность и быстродействие вашего сайта для пользователей. Если вы находитесь в Беларуси и ищете надежного хостинг-провайдера, то BestHost.BY – это отличный выбор. BestHost.BY – одна из ведущих хостинг-компаний в Беларуси, предоставляющая высококачественные услуги уже на протяжении 15 лет.
budesonide cost usa
1xbet зеркало прямо сейчас – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
1xbet личный кабинет – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
suhagra
lyrica online order
tsmavic.wordpress.com – приворот девушки через фото
приворот на женатого мужчину читать, моментальный приворот
http://www.magecam.ru – заговор чтобы любимый мужчина позвонил
citalopram 40mg tablets
ordering difflucan
Your blog serves as a gentle reminder to live life with purpose and passion.
robaxin 10
most recommended allergy medication alternatives to allergy pills major brand allergy pills
Good morning!
Have you ever heard of X-GPT Writer: a unique keyword content generator based on the ChatGPT neural network?
I also haven’t, until I was advised to automate routine tasks with this software, I want to say one thing! For a long time afterwards, I couldn’t believe
that ChatGPT was such a powerful product if it was used simultaneously in streaming, running X-GPT Writer.
I thought it was just a utility, it was inexpensive, a friend gave me a coupon for a 40% discount%:
94EB516BCF484B27
the details of where to enter it are indicated on the website:
https://www.xtranslator.ru/x-gpt-writer/
I started trying, delving into it, bought 50 ChatGPT accounts at low prices and off I went!
Now I easily generate and launch 3-4 new sites per week, batch unify entire folders and even create images
using the ChatGPT neural network and X-GPT Writer.
It’s worth a try, Friends, there’s a demo, everything is free, you won’t regret it)
Good luck!
Синонимайзер текста на основе ChatGPT
ChatGPT для уникального исходного контента
ChatGPT и X-GPTWriter: новая эра контент-маркетинга
ChatGPT и его роль в создании уникального контента
X-GPTWriter: купоны и акции на скидки
ChatGPT как генератор уникального контента
ChatGPT и X-GPTWriter в качестве инструментов синонимизации
Как X-GPTWriter помогает в SEO-оптимизации контента
Эффективное использование ChatGPT для контент-стратегии
Синонимизация текста с X-GPTWriter и ChatGPT
best antihistamine decongestant combo otc allergy medication comparison chart prescription vs over the counter
http://amoxil.icu/# amoxicillin 775 mg
clomid without prescription get generic clomid tablets – how can i get clomid without insurance
http://amoxil.icu/# amoxicillin no prescipion
http://ciprofloxacin.life/# ciprofloxacin
where buy cheap clomid now: cheap clomid pills – where can i buy cheap clomid
prednisone 20mg price: prednisone pills for sale – prednisone drug costs
2000 mg gabapentin
Your authenticity and honesty make your blog stand out from the crowd.
I always look forward to reading your latest blog posts.
Your writing has a way of evoking emotions and sparking curiosity in your readers.
doxycycline hyc: doxycycline tetracycline – cheap doxycycline online
https://zithromaxbestprice.icu/# buy zithromax online cheap
cytotec buy online usa: buy cytotec pills – cytotec buy online usa
order cytotec online: order cytotec online – buy cytotec pills
zestoretic tabs lisinopril 30 mg daily lisinopril price 10 mg
http://doxycyclinebestprice.pro/# doxycycline 50mg
http://doxycyclinebestprice.pro/# doxycycline 500mg
tamoxifen and depression: effexor and tamoxifen – tamoxifen blood clots
https://lisinoprilbestprice.store/# buy lisinopril online no prescription
strongest sleeping pills for insomnia order phenergan 10mg for sale
doxycycline pills: doxy – buy doxycycline online 270 tabs
buy cheap generic zithromax: zithromax over the counter uk – how to get zithromax over the counter
zithromax pill: zithromax online – zithromax 1000 mg pills
http://doxycyclinebestprice.pro/# doxycycline generic
cytotec abortion pill Abortion pills online purchase cytotec
http://doxycyclinebestprice.pro/# buy generic doxycycline
lisinopril 15 mg: lisinopril 2.5 mg buy online – cheap lisinopril
https://nolvadex.fun/# tamoxifen reviews
nolvadex only pct: tamoxifen men – does tamoxifen cause weight loss
buy sleep medications online phenergan tablet
buy cytotec pills: cytotec buy online usa – buy cytotec pills online cheap
cytotec pills buy online Cytotec 200mcg price buy cytotec pills
https://nolvadex.fun/# tamoxifen and osteoporosis
zithromax cost: zithromax 500mg over the counter – where can you buy zithromax
lisinopril 240: can i buy lisinopril over the counter in mexico – medication zestoretic
https://nolvadex.fun/# tamoxifen effectiveness
https://cytotec.icu/# buy cytotec over the counter
tamoxifen for sale: where can i buy nolvadex – tamoxifen lawsuit
https://mexicopharm.com/# mexican mail order pharmacies mexicopharm.com
https://indiapharm.llc/# Online medicine order indiapharm.llc
indian pharmacy paypal India Post sending medicines to USA india pharmacy indiapharm.llc
legit canadian pharmacy: Cheapest drug prices Canada – buying from canadian pharmacies canadapharm.life
purple pharmacy mexico price list: Purple Pharmacy online ordering – mexican rx online mexicopharm.com
https://canadapharm.life/# trustworthy canadian pharmacy canadapharm.life
canadian discount pharmacy: Canadian pharmacy best prices – canadian pharmacy in canada canadapharm.life
best online pharmacy india: best online pharmacy india – best online pharmacy india indiapharm.llc
http://canadapharm.life/# canadian pharmacy near me canadapharm.life
Online medicine order India Post sending medicines to USA top 10 online pharmacy in india indiapharm.llc
order prednisone 10mg sale brand prednisone 20mg
india pharmacy mail order: India Post sending medicines to USA – indian pharmacies safe indiapharm.llc
http://mexicopharm.com/# mexican mail order pharmacies mexicopharm.com
medication from mexico pharmacy: mexican pharmacy – mexican mail order pharmacies mexicopharm.com
reputable canadian pharmacy: my canadian pharmacy rx – canadian king pharmacy canadapharm.life
best canadian pharmacy: buy drugs from canada – canadian pharmacy 24 canadapharm.life
http://canadapharm.life/# pharmacy canadian superstore canadapharm.life
canadianpharmacyworld com: Canadian pharmacy best prices – canada drugstore pharmacy rx canadapharm.life
https://mexicopharm.com/# reputable mexican pharmacies online mexicopharm.com
prednisone 5mg generic order prednisone pill
canadian pharmacy no scripts: Cheapest drug prices Canada – ed drugs online from canada canadapharm.life
canada pharmacy canadian pharmacy 1 internet online drugstore canadian pharmacy sarasota canadapharm.life
buying prescription drugs in mexico: mexican pharmacy – medication from mexico pharmacy mexicopharm.com
http://canadapharm.life/# reliable canadian pharmacy canadapharm.life
mexican mail order pharmacies: Medicines Mexico – mexican pharmaceuticals online mexicopharm.com
https://indiapharm.llc/# india pharmacy indiapharm.llc
п»їlegitimate online pharmacies india: top online pharmacy india – india pharmacy indiapharm.llc
buying from online mexican pharmacy: Mexico pharmacy online – mexican border pharmacies shipping to usa mexicopharm.com
https://mexicopharm.com/# best online pharmacies in mexico mexicopharm.com
http://kamagradelivery.pro/# super kamagra
http://kamagradelivery.pro/# Kamagra 100mg
Levitra 20 mg for sale buy Levitra over the counter Buy Vardenafil 20mg
ed dysfunction treatment: buy ed drugs online – natural ed medications
sildenafil 20 mg pill: Cheapest Sildenafil online – sildenafil soft 100mg
https://kamagradelivery.pro/# Kamagra tablets
Cheap Levitra online: Buy Levitra 20mg online – Vardenafil buy online
http://levitradelivery.pro/# Buy Vardenafil online
Levitra online pharmacy Levitra online Levitra tablet price
https://sildenafildelivery.pro/# where can i buy sildenafil 100mg
http://tadalafildelivery.pro/# cialis tadalafil
Vardenafil online prescription: Levitra online – Buy Vardenafil 20mg online
best heartburn medicine heart burn prescription
https://tadalafildelivery.pro/# tadalafil soft gel capsule 20mg
Kamagra 100mg price: cheap kamagra – п»їkamagra
sildenafil citrate buy: sildenafil without a doctor prescription Canada – sildenafil purchase india
treatments for ed: pills erectile dysfunction – medication for ed
http://levitradelivery.pro/# Levitra online USA fast
what medicine good for heartburn buy lamivudine 100 mg sale
paroxetine 37.5mg price
best ed drug: buy ed drugs online – best ed pills
п»їkamagra buy Kamagra Kamagra 100mg
http://tadalafildelivery.pro/# tadalafil tablets price in india
https://sildenafildelivery.pro/# sildenafil online mexico
ed medications: erection pills over the counter – best erectile dysfunction pills
Kamagra Oral Jelly: cheap kamagra – buy kamagra online usa
http://tadalafildelivery.pro/# tadalafil 5mg best price
https://paxlovid.guru/# paxlovid price
buy paxlovid online п»їpaxlovid paxlovid pharmacy
amoxicillin 500mg capsule: Amoxicillin 500mg buy online – can i buy amoxicillin over the counter
https://prednisone.auction/# mail order prednisone
http://prednisone.auction/# prednisone 5 mg tablet without a prescription
https://prednisone.auction/# prednisone medicine
best acne treatment for adults purchase dapsone sale acne treatment for teenage girl
https://stromectol.guru/# buy ivermectin for humans australia
paxlovid pill paxlovid best price paxlovid india
minocycline 100mg capsule: ivermectin for sale – buy minocycline online
http://prednisone.auction/# prednisone 3 tablets daily
https://stromectol.guru/# ivermectin 1 cream
http://paxlovid.guru/# Paxlovid over the counter
http://amoxil.guru/# amoxicillin 500mg capsules price
acne treatments that work uk buy benzac cream acne treatments that work uk
ivermectin cream 5%: minocycline 100mg – stromectol pills
https://amoxil.guru/# where to get amoxicillin over the counter
http://paxlovid.guru/# paxlovid buy
paxlovid buy Buy Paxlovid privately buy paxlovid online
levitra online canadian pharmacy
http://amoxil.guru/# amoxicillin 250 mg
http://paxlovid.guru/# paxlovid pharmacy
http://finasteride.men/# buy propecia pill
lasix generic name Buy Lasix No Prescription lasix tablet
Cytotec 200mcg price: buy misoprostol – buy misoprostol over the counter
buying generic propecia online: Cheapest finasteride online – buying cheap propecia
http://furosemide.pro/# furosemide 100mg
http://lisinopril.fun/# buy lisinopril online canada
buy propecia without dr prescription: Finasteride buy online – cost propecia
best cold medicine without antihistamine ventolin inhalator brand piriton allergy tablets canada
http://finasteride.men/# propecia no prescription
Abortion pills online: buy misoprostol – cytotec online
http://lisinopril.fun/# buy lisinopril 20 mg
furosemide 40 mg lasix 20 mg furosemide
lyrica 600 mg
zestoretic 10 12.5: generic lisinopril 40 mg – zestoretic medication
furosemide 40 mg: furosemide 100 mg – lasix uses
https://azithromycin.store/# average cost of generic zithromax
different types of allergy medicine theophylline order online allergy medication better than allegra
http://finasteride.men/# buy generic propecia
zithromax buy online: zithromax best price – buy zithromax 1000 mg online
https://finasteride.men/# cost generic propecia without dr prescription
http://lisinopril.fun/# buy lisinopril 10 mg
purchase cytotec buy misoprostol buy cytotec pills
zithromax 500 without prescription: zithromax best price – zithromax prescription
where can you buy zithromax: Azithromycin 250 buy online – zithromax 500 mg lowest price online
get propecia without rx: buying cheap propecia – order propecia
http://misoprostol.shop/# buy cytotec online
zithromax cost canada: zithromax best price – how to get zithromax online
buy cytotec over the counter Buy Abortion Pills Online buy cytotec online fast delivery
https://misoprostol.shop/# buy cytotec online
https://misoprostol.shop/# Cytotec 200mcg price
http://finasteride.men/# rx propecia
lasix 100 mg: Buy Lasix – lasix for sale
http://furosemide.pro/# lasix tablet
Thank you so much!
over the counter lisinopril: can you buy lisinopril over the counter – lisinopril pills 2.5 mg
acid reflux drugs prescription list buy pepcid paypal
buy zithromax: zithromax best price – zithromax pill
stomach acid medication prescription roxithromycin for sale online
zithromax for sale cheap zithromax best price zithromax 250
https://misoprostol.shop/# Abortion pills online
lisinopril 5mg: over the counter lisinopril – lisinopril capsule
buy cytotec over the counter: Misoprostol best price in pharmacy – cytotec buy online usa
https://lisinopril.fun/# lisinopril 10 best price
http://furosemide.pro/# lasix 40mg
https://lisinopril.fun/# 10 mg lisinopril tablets
propecia: Cheapest finasteride online – cheap propecia price
lisinopril 5mg prices: lisinopril generic 10 mg – lisinopril 40 coupon
buy generic zithromax no prescription buy zithromax z-pak online can you buy zithromax over the counter in mexico
https://azithromycin.store/# can you buy zithromax online
isotretinoin order order isotretinoin 40mg for sale brand accutane 20mg
migliori farmacie online 2023: Cialis senza ricetta – farmacia online miglior prezzo
migliori farmacie online 2023: farmacia online migliore – farmacie online affidabili
accutane 10mg us isotretinoin 10mg ca accutane 20mg canada
http://avanafilitalia.online/# farmacia online senza ricetta
п»їfarmacia online migliore: kamagra – farmacia online senza ricetta
migliori farmacie online 2023 avanafil generico farmacie online sicure
->>>>>>>>>>>>>заговор на любовь мужчины на ветер<<<<<<<<<-
______________как вернуть мужа заговоры _____________
https://privorot4.wordpress.com
как приворожить жену в домашних условиях, а также:
->>>>>>отношения после снятия приворота
->>>>>>приворот на женатого мужчину в домашних условиях
->>>>>>приворот на мужчину на кладбище
->>>>>>сексуальная присушка
http://sildenafilitalia.men/# pillole per erezioni fortissime
https://avanafilitalia.online/# acquistare farmaci senza ricetta
http://kamagraitalia.shop/# п»їfarmacia online migliore
top farmacia online: Farmacie a milano che vendono cialis senza ricetta – acquistare farmaci senza ricetta
farmacie on line spedizione gratuita: avanafil – farmacie on line spedizione gratuita
https://avanafilitalia.online/# farmacia online senza ricetta
viagra prezzo farmacia 2023: sildenafil 100mg prezzo – viagra generico in farmacia costo
https://sildenafilitalia.men/# viagra originale in 24 ore contrassegno
farmacia online migliore п»їfarmacia online migliore acquisto farmaci con ricetta
farmacia online: kamagra – farmacia online migliore
http://kamagraitalia.shop/# acquistare farmaci senza ricetta
farmaci senza ricetta elenco: farmacia online – migliori farmacie online 2023
http://kamagraitalia.shop/# top farmacia online
http://farmaciaitalia.store/# acquistare farmaci senza ricetta
farmacie on line spedizione gratuita: farmacie online sicure – farmacie on line spedizione gratuita
https://farmaciaitalia.store/# acquistare farmaci senza ricetta
farmacie on line spedizione gratuita kamagra gel prezzo migliori farmacie online 2023
farmacie online affidabili: farmacia online miglior prezzo – farmacie online affidabili
buying sleeping tablets on internet buy phenergan 25mg generic
farmacie online autorizzate elenco: Cialis senza ricetta – acquistare farmaci senza ricetta
https://tadalafilitalia.pro/# farmacia online migliore
prescription for sleep aids buy generic modafinil for sale
buy amoxicillin 500mg capsules uk
п»їfarmacia online migliore: avanafil generico prezzo – farmacia online miglior prezzo
buproprion purchase online
http://kamagraitalia.shop/# acquistare farmaci senza ricetta
https://avanafilitalia.online/# farmacia online
http://tadalafilitalia.pro/# top farmacia online
http://mexicanpharm.store/# mexican border pharmacies shipping to usa
reputable indian online pharmacy: mail order pharmacy india – indian pharmacy paypal
pharmacy canadian: canadapharmacyonline – is canadian pharmacy legit
http://canadapharm.shop/# canada rx pharmacy
medicine in mexico pharmacies purple pharmacy mexico price list mexican mail order pharmacies
buy amoxil 1000mg for sale amoxil 1000mg oral order generic amoxicillin 250mg
india online pharmacy: online pharmacy india – indianpharmacy com
http://canadapharm.shop/# canadian family pharmacy
https://canadapharm.shop/# precription drugs from canada
fluoxetine buy usa
canadian pharmacy scam: canadian pharmacy phone number – trustworthy canadian pharmacy
reputable mexican pharmacies online: mexican rx online – medicine in mexico pharmacies
escrow pharmacy canada: precription drugs from canada – online canadian pharmacy
https://indiapharm.life/# top 10 online pharmacy in india
medicine in mexico pharmacies: mexican mail order pharmacies – pharmacies in mexico that ship to usa
mexico pharmacies prescription drugs mexico pharmacies prescription drugs mexican drugstore online
https://canadapharm.shop/# legit canadian pharmacy
best online pharmacy india: online shopping pharmacy india – top online pharmacy india
http://mexicanpharm.store/# buying prescription drugs in mexico online
mexican drugstore online: medication from mexico pharmacy – reputable mexican pharmacies online
https://canadapharm.shop/# www canadianonlinepharmacy
vipps approved canadian online pharmacy: canada cloud pharmacy – online pharmacy canada
https://indiapharm.life/# india online pharmacy
Kros Disposable Vape presents an effortless vaping solution with a sleek design and a variety of flavorful options. Enjoy the convenience and satisfaction of Kros, delivering a premium vaping experience.
mexican drugstore online: mexican mail order pharmacies – п»їbest mexican online pharmacies
online shopping pharmacy india: best india pharmacy – buy prescription drugs from india
https://indiapharm.life/# top 10 online pharmacy in india
buying prescription drugs in mexico: buying prescription drugs in mexico – pharmacies in mexico that ship to usa
canada pharmacy: my canadian pharmacy – escrow pharmacy canada
northern pharmacy canada canada drugstore pharmacy rx onlinecanadianpharmacy 24
http://canadapharm.shop/# my canadian pharmacy rx
azithromycin 500mg cost azithromycin 250mg over the counter azithromycin 500mg ca
best online pharmacies in mexico: best online pharmacies in mexico – mexican online pharmacies prescription drugs
http://canadapharm.shop/# canadianpharmacyworld com
buy azithromycin 500mg without prescription buy zithromax generic zithromax 500mg canada
черный жесткий приворот – Обратится к магу – https://dzen.ru/id/653538d7d6100f7a6fee8469
приворот по фото черная магия
https://mexicanpharm.store/# reputable mexican pharmacies online
gabapentin online buy neurontin canada
buying from online mexican pharmacy: purple pharmacy mexico price list – mexico drug stores pharmacies
neurontin 800mg for sale neurontin 800mg canada
https://canadapharm.shop/# cheap canadian pharmacy
indian pharmacies safe: india pharmacy – indian pharmacy online
canada pharmacy: canadian pharmacy tampa – best canadian pharmacy
Магическая помощь – сильные экстрасенсы
действенные ритуалы на любовь https://gadalkindom.ru приворот на парня на расстоянии читать без фото и свечей
приворот любимого читать
https://indiapharm.life/# reputable indian pharmacies
яндекс услуги экстрасенс ->>>>>>>услуги экстрасенса шепс https://www.magecam.ru <<<<<<<<<<-
mexican border pharmacies shipping to usa mexican rx online mexico drug stores pharmacies
mexican pharmacy: medication from mexico pharmacy – mexican online pharmacies prescription drugs
https://indiapharm.life/# indianpharmacy com
https://www.magecam.ru
Услуги магов
-привороты
-наведение порчи на смерть
-отнятие удачи
-возврат любимого
мощный приворот на имя
Thanks for thr great article!
http://mexicanpharm.store/# mexican online pharmacies prescription drugs
http://cytotec.directory/# buy cytotec over the counter
http://clomidpharm.shop/# buying clomid
I appreciate their late hours for those unexpected needs https://clomidpharm.shop/# generic clomid for sale
самый быстрый приворот https://www.magecam.ru приворот на фото бывшего
жертва приворота избегает заказчика
prednisone price south africa: price of prednisone tablets – prednisone buy
https://cytotec.directory/# cytotec pills buy online
Professional, courteous, and attentive – every time http://prednisonepharm.store/# buy prednisone from canada
как заворожить девушку к себе на любовь по фото – Помощь экстрасенса https://www.magecam.ru – приворот на любовь парня читать в домашних условиях на расстоянии вернуть любимого бесплатно
cytotec abortion pill purchase cytotec cytotec pills buy online
zithromax azithromycin: zithromax cost uk – where to get zithromax over the counter
услуги целителя экстрасенса ->>>>>>>экстрасенсы и услуги https://www.magecam.ru <<<<<<<<<<-
проверить есть ли порча бесплатно https://www.magecam.ru порча документов статья ук рф
Long-Term Effects https://cytotec.directory/# order cytotec online
https://zithromaxpharm.online/# zithromax 1000 mg online
Thanks for thr great article!
https://zithromaxpharm.online/# buy cheap zithromax online
Черный маг
сильная присуха на мужчину на расстоянии чтобы страдал https://gadalkindom.ru как снять приворот с любимого мужчины
как приворожить женатого мужчину на расстоянии без последствия в домашних условиях
buy generic azipro online buy azithromycin generic azithromycin 250mg cheap
The most pleasant pharmacy experience every time http://zithromaxpharm.online/# zithromax coupon
Thank you so much!
http://nolvadex.pro/# nolvadex estrogen blocker
can i purchase generic clomid pills: where can i buy cheap clomid without insurance – cost generic clomid pill
azipro 250mg oral order azipro 250mg generic buy generic azipro for sale
Thank you so much!
buy furosemide 40mg online cheap lasix 100mg uk
http://zithromaxpharm.online/# zithromax over the counter
low dose tamoxifen: nolvadex 10mg – tamoxifen depression
buy furosemide 100mg generic lasix tablet
A true champion for patients around the world http://nolvadex.pro/# tamoxifen vs raloxifene
prednisone 5mg daily prednisone 2.5 tablet how to buy prednisone online
http://cytotec.directory/# purchase cytotec
cytotec abortion pill: cytotec abortion pill – Cytotec 200mcg price
Their medication synchronization service is fantastic http://nolvadex.pro/# tamoxifen
http://prednisonepharm.store/# no prescription prednisone canadian pharmacy
http://nolvadex.pro/# nolvadex for sale
prednisone 2 5 mg: prednisone without prescription – generic prednisone tablets
Their international health forums provide crucial insights https://cytotec.directory/# buy cytotec over the counter
http://clomidpharm.shop/# generic clomid online
Efficient, effective, and always eager to assist http://cytotec.directory/# buy cytotec pills
prednisone uk: prednisone without prescription.net – prednisone 50 mg tablet cost
buy cytotec cytotec abortion pill cytotec online
http://nolvadex.pro/# buy nolvadex online
buy online prescription drugs certified canadian online pharmacies canadian prescription drugstore
http://reputablepharmacies.online/# canada drugs online review
omnacortil without prescription buy omnacortil 5mg for sale buy generic prednisolone for sale
best over the counter ed pills best over the counter ed pills best ed drugs
non prescription ed drugs: viagra without a doctor prescription – discount prescription drugs
order omnacortil 10mg for sale order omnacortil without prescription cheap omnacortil without prescription
online drugstore service canada http://reputablepharmacies.online/# mexican drugstore online
canada mail pharmacy
http://edpills.bid/# ed meds online
->>>>>>>>>>>>>приворот с месячными без последствия<<<<<<<<<-
______________как узнать о привороте _____________
заговор на воду на любовь мужчины сильный читать
приворожить на вещь https://privorot4.wordpress.com приворот на крови месячных как
заговор вернуть любовь
как узнать есть на муже приворот, а также:
->>>>>>как привязать к себе женщину навсегда с помощью магии самостоятельно
viagra without a doctor prescription levitra without a doctor prescription best ed pills non prescription
verified canadian pharmacy: buy prescription drugs online legally – canadian pharmacy selling viagra
ed meds online without doctor prescription: viagra without a doctor prescription walmart – viagra without a prescription
http://reputablepharmacies.online/# legitimate canadian mail order pharmacies
https://edpills.bid/# men’s ed pills
ed dysfunction treatment male ed drugs ed treatments
->>>>>>>>>>>>>заговор на любовь мужчины на расстоянии читать быстродействующий на ночь<<<<<<<<<-
______________заговор на ветер на любовь мужчины читать белая _____________
заговор на возобновление чувств https://privorot4.wordpress.com
что происходит с мужчиной если его приворожили, а также:
->>>>>>приворот на замужество читать
->>>>>>любовные заклинания на девушку
->>>>>>приворот мгновенный
->>>>>>заговоры чтоб вернуть жену
treatment of ed: best ed pills non prescription – best male ed pills
north canadian pharmacy canadian online pharmacies legitimate canadian drugs online pharmacy
canadian meds without prescription https://edpills.bid/# cheap erectile dysfunction pill
canadian drugstore reviews
http://reputablepharmacies.online/# northwestpharmacy
drugs for ed: mens ed pills – cheap ed drugs
Ищете займ онлайн с выгодными условиями? Вам повезло! Мы предлагаем широкий выбор онлайн займов, которые помогут вам решить финансовые вопросы быстро и без лишних хлопот.
prescription drugs without doctor approval buy prescription drugs without doctor levitra without a doctor prescription
– через сколько дней действует приворот в домашних условиях
– https://privorot16.ru сильный приворот по вуду
– через сколько действует приворот и какие
– приворот на полнолуние отзывы
http://reputablepharmacies.online/# pharmacy without dr prescriptions
prescription drugs canada buy online: buy prescription drugs without doctor – generic viagra without a doctor prescription
mexican pharmacy online medications mexican mail order pharmacy my canadian pharmacy viagra
ed pills that really work: best erection pills – natural ed remedies
https://edpills.bid/# over the counter erectile dysfunction pills
xenical over the counter australia
сильный приворот на похудение приворот рассорить мужа с родственниками привороты на любовь краснодар
https://superprivorot.ru
ed meds online ed medications online cheap ed drugs
http://reputablepharmacies.online/# canadian drugstore online
online drugstore: canadian drugs cialis – online drugstore service canada
men’s ed pills erection pills viagra online natural remedies for ed
prescription drugs canada buy online: ed prescription drugs – discount prescription drugs
https://edwithoutdoctorprescription.store/# prescription drugs
порча имущества статья ук рф по неосторожности – https://darstars.ru порча на нитках
как снять чужой приворот с любимого человека самостоятельно на расстоянии легкие привороты на любовь
способ приворота мужчины в домашних условиях – https://grimuar.ru приворот по фото с телефона в домашних
ozempic pill form
чем присушка отличается от приворота – https://zakolduj.ru приворот через фотографию
приворот на одну свечу приворот вуду в домашних условиях – https://10-sposobov.ru приворот на мужчину читать в домашних условиях который точно работает
online prescriptions without script canadian pharmacy prices canadian online pharmacies reviews
https://canadianpharmacy.pro/# canadian pharmacy checker canadianpharmacy.pro
приворот на кровь из вены – https://магиявера.рф
http://mexicanpharmacy.win/# mexican drugstore online mexicanpharmacy.win
legit canadian pharmacy online
https://mexicanpharmacy.win/# buying from online mexican pharmacy mexicanpharmacy.win
buy amoxil pills buy generic amoxil amoxicillin where to buy
world pharmacy india indian pharmacy indian pharmacy online indianpharmacy.shop
п»їlegitimate online pharmacies india: international medicine delivery from india – online shopping pharmacy india indianpharmacy.shop
amoxil 250mg over the counter buy amoxil 500mg for sale buy amoxil no prescription
purchase doxycycline vibra-tabs order online
http://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
order vibra-tabs sale buy generic doxycycline online
indian pharmacy online Cheapest online pharmacy best online pharmacy india indianpharmacy.shop
п»їlegitimate online pharmacies india: Cheapest online pharmacy – indian pharmacy paypal indianpharmacy.shop
сильный приворот на любовь девушки сексуальный приворот на мужчину
приворот на мужчину на – https://ezomirek.ru приворот на парня на сигарете
https://mexicanpharmacy.win/# purple pharmacy mexico price list mexicanpharmacy.win
indian pharmacy Best Indian pharmacy world pharmacy india indianpharmacy.shop
– что чувствует мужчина, когда на него сделан приворот
– https://приворот-инфо.рф привороты во время поста
– черный приворот и его последствия
– принаки приворота мужчины
http://canadianpharmacy.pro/# my canadian pharmacy review canadianpharmacy.pro
meds canada
best online pharmacy india: international medicine delivery from india – reputable indian online pharmacy indianpharmacy.shop
http://indianpharmacy.shop/# Online medicine order indianpharmacy.shop
https://canadianpharmacy.pro/# online canadian pharmacy reviews canadianpharmacy.pro
buying prescription drugs in mexico online mexican pharmacy online mexico pharmacy mexicanpharmacy.win
приворот признаки – https://magic-online.ru приворот на фото читать
как снять сексуальный приворот последствия приворота на любовь
приворот на кровь из пальца читать – https://hariola.com как понять что на тебе есть приворот
приворот на красную нить читать приворот на улучшение бизнеса приворот на месячную кровь за день
https://koldovstvo.net
https://canadianpharmacy.pro/# canada pharmacy online canadianpharmacy.pro
best india pharmacy indian pharmacy to usa indian pharmacies safe indianpharmacy.shop
– привороты на предметы
– https://magicspell.ru приворот невербальными жестами
– сильнейший любовный приворот сделать самой
– признаки любовного приворота у сына
– приворот с фото положить фото под голую пяткуприворот церковные врата обсуждениесроки приворота куклы вуду
===============================================================================
последствия кладбищенского приворота
рунный став приворот приворот на человека которого любишь
приворот на мужчину без последствия сразу действует на расстоянии без фото – https://walls-club.ru приворот на любовь парня читать в домашних условиях на расстоянии без фото и свечей
======================
http://mexicanpharmacy.win/# mexican pharmacy mexicanpharmacy.win
https://mexicanpharmacy.win/# medication from mexico pharmacy mexicanpharmacy.win
best india pharmacy
purple pharmacy mexico price list mexican pharmacy online buying prescription drugs in mexico mexicanpharmacy.win
приворот мужа на булавку – https://molotokrus.ru приворот жены на крови
https://indianpharmacy.shop/# Online medicine home delivery indianpharmacy.shop
online pharmacy reviews
приворот на трусы любимого тексты самых сильных приворотов на парня черная магия приворот текст
https://maguri.ru
явно действующий сильный приворот
приворот на парня отзывы кто делал
приворот на дорогостоящие подарки начальству
http://mexicanpharmacy.win/# mexican drugstore online mexicanpharmacy.win
http://mexicanpharmacy.win/# buying prescription drugs in mexico online mexicanpharmacy.win
https://indianpharmacy.shop/# top 10 online pharmacy in india indianpharmacy.shop
top 10 pharmacies in india
Thanks for thr great article!
приворот на девушку читать в домашних условиях который точно сработает как узнать есть ли на сыне приворот в домашних условиях – тринити астрология снять с себя приворот
астрология гуркова астрология двач
астрология музей
top 10 pharmacies in india indian pharmacy Online medicine order indianpharmacy.shop
августин философия голубинцев философия
философия энциклопедияфилософия трансцендентализмаромантизм философия
горгий философия философия ботаники философии виды
порча на отнятие женских органов – https://artgrom.com порча на члена семьи.
порча возвращается заказчику
как проявляется порча на детях
порча можно ли снять
порча игла в стене
https://canadianpharmacy.pro/# canadian pharmacy drugs online canadianpharmacy.pro
https://canadianpharmacy.pro/# canadian mail order pharmacy canadianpharmacy.pro
п»їlegitimate online pharmacies india
приворот парня без последствий = https://magicwishes.ru приворот на аквариумних рибках
самая сильная приворотная молитва староверские любовные привороты
best india pharmacy india pharmacy buy prescription drugs from india indianpharmacy.shop
order albuterol 2mg generic buy generic albuterol inhalator buy albuterol 4mg
аддитивность энтропии – энтропия функция.
энтропия песня – https://privorot-vsem.ru значение слова энтропия.
энтропия статьи
вывод формулы энтропии
умножать энтропию
https://indianpharmacy.shop/# world pharmacy india indianpharmacy.shop
price drugs
ventolin inhalator buy online buy albuterol online albuterol buy online
https://mexicanpharmacy.win/# mexican rx online mexicanpharmacy.win
http://mexicanpharmacy.win/# mexican rx online mexicanpharmacy.win
buy medicines online in india
https://mexicanpharmacy.win/# mexican mail order pharmacies mexicanpharmacy.win
– приворот самому, что бы вспомнил и пришел
– https://приворот-инфо.рф привороты и их рецепты
приворот на вещь любимой девушки стльный приворот мужа по фото
фанфик emily waters приворотное зелье свеча иголки приворот падают
привороты любовь парня привороты мальчика влюбить в себя
generic rybelsus for weight loss
===============================================================================
приворот таро
приворот на носок.
как убрать приворот на месячные с мужчины сильный белый приворот на любовь мужчины.
приворот на соль в домашних условиях – https://true-magic.ru приворот на фото с телефона.
самый сильный приворот который нельзя снять
сильный белый приворот на мужчину
======================
buying prescription drugs in mexico mexican mail order pharmacies mexico pharmacy mexicanpharmacy.win
сильный приворот на церковные свечи – https://turk-sinema.ru приворот мужчины на месячные последствия.
кладбищенский приворот последствия для заказчика
снятие приворота солью на сковороде
как сделать приворот на фото
приворот на волос-с лобка
приворот по фотографии женщину .
приворот на бельё приворот секс игрушка
сделать приворот растущей луне – https://morfeos.ru привороты за 7 дней .
сексуальные привороты любимого бесплатно цдкж приворотное зелье.
https://indianpharmacy.shop/# indian pharmacies safe indianpharmacy.shop
india online pharmacy
https://indianpharmacy.shop/# reputable indian pharmacies indianpharmacy.shop
best online pharmacy india international medicine delivery from india Online medicine home delivery indianpharmacy.shop
приворот на вещь любимого читать приворот за 1 день – алия астрология приворот на замужнюю женщину
тату астрология меркурий астрологии.
денеб астрология. астрология родина арт астрология.
https://indianpharmacy.shop/# cheapest online pharmacy india indianpharmacy.shop
best india pharmacy
приворот на фото мужчины как убрать приворот с мужчины самостоятельно в домашних.
приворот на месячных приворот чтоб написал.
мусульманский приворот последствия – https://zakoldovan.ru любовный приворот белая магия.
приворот на месячную кровь дома цыганские привороты приворот черный сват
http://canadianpharmacy.pro/# canadian pharmacy online canadianpharmacy.pro
– приворот на месячные последствия – приворот по фотографии на расстояние.
– https://magicwishes.ru приворот по фото быстро
-снять приворот в иркутске приворот у входа в церковь на деньги на растущую луну.тонкости черной магии приворота не нужно импровизировать результат зависит от.
-снимается ли приворот до конца приворот на слезе.приворот на безымянный крест форум.
-сделать приворот самара черная магия заклятия привороты заклинания
adderall canadian pharmacy Pharmacies in Canada that ship to the US canada drug pharmacy canadianpharmacy.pro
augmentin online cheap augmentin
приворот на могильную землю – https://magic.jofo.me приворот мужчины на соль.
приворот на плевок. приворот на монеты
сделать приворот в москве черный приворот с кровью
приворот на рыбу читать самостоятельно на мужчину.
buy augmentin tablets buy augmentin 1000mg generic
http://cialissansordonnance.shop/# Pharmacie en ligne livraison rapide
приворот отменить. приворот попал не на того приворот на монетку
https://kak-vernut-muzh.ru .
////привороты истории снять приворот поставить защиту.
////самостоятельно снять приворот c мужа.
////приворот на любовь мужа на алкоголь
ozempic for weight loss
Pharmacies en ligne certifiГ©es levitra generique sites surs Pharmacie en ligne livraison gratuite
Viagra vente libre pays: Meilleur Viagra sans ordonnance 24h – Prix du Viagra 100mg en France
1xbet сайт– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
черная магия приворота мужчины быстрый приворот без фото – релаксация астрология приворот на волос любимого
бадзы астрология астрология бацзы.
аудиокниги астрология. натальный астрология
астрология вязание.
приворот на воске приворот на любимого в домашних условиях читать.
приворот на ивана купала приворот сведение судеб.
как сделать приворот на месячные самостоятельно – https://hiromantia.net приворот чтобы парень позвонил читать в домашних условиях.
приворот как приворожить девушку как сделать приворот на девушку в домашних условиях можно ли делать приворот в
– тексты любовных приворотов заговоров – приворот по фотографии и левой пятке.
– https://darmaga.ru приворот на месячные в напиток магия
-приворот на любовь город владивосток приворот чтоб только обо мне думал и хотел.привороты на западной украине.
-черная магия приворот по имнеи приворот натуральных блондинок глаз.скачать бесплатно треннинг наука приворотных слов ковалев.
-привороты форум беларусь сколько людей на планете сделали любовный приворот
https://acheterkamagra.pro/# pharmacie ouverte 24/24
pharmacie ouverte 24/24
acheter medicament a l etranger sans ordonnance levitra generique prix en pharmacie Pharmacie en ligne pas cher
http://cialissansordonnance.shop/# acheter medicament a l etranger sans ordonnance
Pharmacie en ligne France: PharmaDoc – Pharmacie en ligne livraison rapide
Pharmacie en ligne fiable: Pharmacies en ligne certifiГ©es – Pharmacie en ligne livraison gratuite
белая магия приворот на любовь – https://mysticworldclub.ru приворот на любовь бесплатно.
приворот на мужчину на любовь без последствия. простой приворот дома
приворот по фото на телефоне в домашних условиях без последствия признаки приворота во сне
приворот девушки на крови.
смотреть бесплатно какие привороты делают на полнолуние. привороты женатого последствия сильный приворот форум.
https://magicblack.biz .
смотреть бесплатно и без регистрации привороты парня привороты кладби форум.
п»їpharmacie en ligne levitra generique prix en pharmacie Pharmacie en ligne livraison 24h
п»їpharmacie en ligne: levitra generique sites surs – acheter mГ©dicaments Г l’Г©tranger
https://acheterkamagra.pro/# pharmacie en ligne
It is very comforting to see that others are suffering from the same problem as you, wow!
молитвы на приворот мужчины читать приворот подклад – https://vericon.ru сильный приворот на возврат мужа
корни астрологии астрология суд.
астрология книга. предсказательная астрология
литва астрология.
защита перед приворотом сильный приворот рунами.
приворот руны . приворот на мужчину читать в домашних на расстоянии , приворот на имя мужчины.
приворот молитвой – https://monte24.ru приворот на парня на соль.
приворот на красное вино приворот дома без последствия приворот с помощью месячных последствия
п»їpharmacie en ligne: PharmaDoc.pro – Pharmacie en ligne sans ordonnance
buy levothroid generic levothroid online buy buy synthroid 100mcg online cheap
http://levitrasansordonnance.pro/# Pharmacie en ligne fiable
– снять любовный приворот соперницы – приворот на замужество читать самостоятельно.
– https://cardul.ru усиление приворота
-сексуальний приворот заговор привороты маги.приворот супруга.
-сама дома прочитала приворот на любимого мужчину форум приворот с солью.приворот сделать самой вернуть любимого.
-приворот на крови длительность форум с какого момента действует приворот
Viagra homme prix en pharmacie sans ordonnance viagrasansordonnance.pro Viagra sans ordonnance livraison 48h
buy synthroid 100mcg without prescription synthroid price levothroid over the counter
приворот на девушку как снять привороты на любовь девушки читать в домашних условиях на расстоянии – https://arkras.com приворот на привлечение денег
астрология православие кит астрология.
анжела астрология. шестопалов астрология
астрология стрельца.
http://acheterkamagra.pro/# Pharmacies en ligne certifiГ©es
Pharmacie en ligne sans ordonnance
привороты оплата резульата. сильный приворот который нельзя снять рейки магия лечение сглаз приворот.
https://stavy.ru .
приворот чтобы он думал о тебе шаманка в якутии приворот.
можно ли снять приворот с мужчины – https://ozhegova-slovar.ru приворот на сигарету последствия.
как узнать есть ли на муже приворот любовницы. приворот на месячные на лоб
приворот на любовь парня читать в домашних условиях на расстоянии без фото и свечей без вреда приворот на дружбу
приворот на расстоянии без последствия.
pharmacie ouverte: levitra generique sites surs – Pharmacie en ligne France
https://cialissansordonnance.shop/# Pharmacie en ligne France
Viagra sans ordonnance livraison 48h: Acheter du Viagra sans ordonnance – Viagra femme ou trouver
пенсионер по уходу за ребенком – https://ladytoday.ru ->>>>>>>>> уход а грудным ребенком !
Acheter mГ©dicaments sans ordonnance sur internet: Pharmacies en ligne certifiees – Pharmacie en ligne France
Pharmacies en ligne certifiГ©es levitrasansordonnance.pro acheter medicament a l etranger sans ordonnance
обрезание ребенка уход – https://xigra.ru
https://pharmadoc.pro/# Pharmacie en ligne pas cher
levitra 20mg canada order vardenafil 20mg for sale
order vardenafil 20mg generic levitra pill
Pharmacie en ligne livraison 24h: cialis prix – acheter medicament a l etranger sans ordonnance
Pharmacie en ligne fiable pharmacie en ligne pas cher Pharmacie en ligne France
https://levitrasansordonnance.pro/# Pharmacie en ligne livraison gratuite
can i purchase generic clomid without prescription: how to get clomid without prescription – can i buy cheap clomid price
http://prednisonetablets.shop/# 20 mg prednisone tablet
buy zithromax online: cost of generic zithromax – how much is zithromax 250 mg
semaglutide 3mg
can you get cheap clomid without a prescription generic clomid online where to get generic clomid price
serophene for sale online clomid over the counter serophene price
buy serophene generic clomiphene 100mg tablet buy generic clomid 50mg
http://prednisonetablets.shop/# best pharmacy prednisone
ivermectin goodrx: buy stromectol pills – ivermectin purchase
amruthaborewells.com
그들은 정말 본 적이 없습니다 … 감히 공격을 주도한 명나라 군대.
https://ivermectin.store/# ivermectin 10 ml
zithromax azithromycin can you buy zithromax online zithromax over the counter uk
stromectol lotion: ivermectin 5 – minocycline 50 mg for sale
молитва о снятии проклятия с человека как снять магию с человека заговор на яйцо снять болезнь
играть казино онлайн– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
where can i purchase zithromax online: zithromax 1000 mg online – where to get zithromax over the counter
https://amoxicillin.bid/# generic amoxicillin
hz-wallpaper.com
Hongzhi 황제는 미소를 지으며 “무슨 일이 지연 되었습니까? “라고 말했습니다.
can we buy amoxcillin 500mg on ebay without prescription amoxicillin 750 mg price amoxicillin 500mg buy online canada
where can i get clomid prices: where to get clomid no prescription – buy clomid without rx
http://clomiphene.icu/# clomid order
can you buy zithromax over the counter in australia zithromax prescription zithromax online no prescription
buy tizanidine 2mg without prescription buy generic tizanidine for sale tizanidine 2mg price
amoxicillin without rx: generic amoxicillin cost – can you buy amoxicillin over the counter
https://azithromycin.bid/# buy cheap zithromax online
prednisone 10mg tablet price: prednisone for sale in canada – prednisone for sale online
http://prednisonetablets.shop/# prednisone pharmacy
гадания привороты отзывы – приворот рунный кто делал отзывы – приворот томск отзывы
stromectol tablets uk: ivermectin 10 ml – ivermectin 3mg dosage
buy amoxicillin 500mg canada amoxicillin 500mg over the counter can you buy amoxicillin over the counter in canada
http://ivermectin.store/# ivermectin 0.5 lotion
order generic semaglutide order semaglutide online cheap rybelsus uk
buy tizanidine 2mg generic buy tizanidine 2mg for sale buy zanaflex online cheap
can i get generic clomid without insurance: cost of generic clomid price – cheap clomid pill
semaglutide 14 mg tablet semaglutide price order rybelsus 14 mg
buy amoxicillin online uk amoxicillin 500mg price rexall pharmacy amoxicillin 500mg
http://ivermectin.store/# where to buy stromectol
online order prednisone: prednisone over the counter cost – prednisone 10 tablet
buy azithromycin zithromax: zithromax buy – cheap zithromax pills
rybelsus prescription
http://amoxicillin.bid/# rexall pharmacy amoxicillin 500mg
http://prednisonetablets.shop/# prednisone 5mg capsules
buy ivermectin cream: stromectol cost – ivermectin 0.5%
prednisone 40mg canada deltasone 10mg without prescription order deltasone 40mg sale
How to track the location of your partner through mobile phone photos? Have you ever had a situation where your partner went out without telling you where they were going? Don’t you want to just ask them where they are, and don’t know how to track their location with a mobile phone?
indian pharmacy online: order medicine from india to usa – top 10 online pharmacy in india indianpharm.store
https://mexicanpharm.shop/# mexican pharmaceuticals online mexicanpharm.shop
reddit canadian pharmacy: Canadian International Pharmacy – best canadian online pharmacy canadianpharm.store
mexican mail order pharmacies Online Pharmacies in Mexico best online pharmacies in mexico mexicanpharm.shop
buy deltasone for sale order prednisone 20mg without prescription order prednisone 20mg generic
restaurant-lenvol.net
이 희미한 불꽃 속에서 그는 계속해서 무언가를 찾고 있었다.
жертва приворота не идет на контакт – https://institutmassaga.ru приворот в контакте.
как понять что на мужчине приворот или привязка форум. был ли приворот как узнать
последствия снятия приворота для заказчика после снятия приворота приворот на мак мужчину последствия
проверенный приворот.
Thank you so much!
cheapest online pharmacy india: international medicine delivery from india – reputable indian online pharmacy indianpharm.store
привороты на любовь в г.николаев. приворот самостоятельно на льва сильный приворот на могиле.
https://infoprivorot.ru .
приворот по фото со свечой приворот семь раз по часовой стрелке.
как снять приворот и вернуть жену приворот на женщину читать в домашних условиях который точно сработает.
приворот во время дождя . избавиться от приворота самостоятельно , какая расплата за приворот.
вернется ли муж после снятия приворота – https://psychologdo.ru мистические истории приворот голубая луна.
приворот в церкви заговор читать приворот на волосы мужчины читать в домашних условиях приворот на соль на любовь мужчины читать на расстоянии
– привороты свечах любовь – приворот на секс самостоятельно по фото.
– https://fengshui24.ru смысл приворотов на кровь
-самый сильный привороты в домашних условиях приворот на время.самые эфективные и лёгкие привороты.
-приворот чтобы парень позвонил где можно его провести приворот на любовь мужчины женатого читать самостоятельно.скачать приворот мз3.
-приворот чтобы он скучал самостоятельно самый сильный приворот на мужчину по фотографии
https://mexicanpharm.shop/# mexico pharmacy mexicanpharm.shop
mexican mail order pharmacies: Certified Pharmacy from Mexico – mexican pharmacy mexicanpharm.shop
indian pharmacy online international medicine delivery from india cheapest online pharmacy india indianpharm.store
приворот на любовь девушки читать в домашних условиях по фото приворот на парня по фотографии – астрология иконка приворот на мужчину без последствия сразу действует белая магия в домашних условиях
астрология слово астрология просчитать.
кроссворд астрология. астрология магии
астрология.
rybelsus 14mg cheap semaglutide without prescription rybelsus cheap
Купить диплом по выгодной цене тут http://diplom-sale.ru проще всего. Гарантируем подлинность и прохождение любых проверок.
https://indianpharm.store/# indian pharmacy online indianpharm.store
order semaglutide 14mg for sale buy semaglutide tablets purchase semaglutide pills
https://mexicanpharm.shop/# best online pharmacies in mexico mexicanpharm.shop
руны снятие приворота от сэма приворот на мужчину на питье.
черный приворот рунами приворот парня к себе.
сильный приворот на парня без фото в домашних условиях читать – https://wow-guides.ru привороты на парня читать в домашних условиях за один день.
последствия снятия приворота как узнать есть приворот на муже в домашних условиях привороты на пасху
online pharmacy india: online pharmacy india – Online medicine order indianpharm.store
cheapest online pharmacy india: order medicine from india to usa – indian pharmacies safe indianpharm.store
india online pharmacy international medicine delivery from india buy medicines online in india indianpharm.store
приворот на парня который действует сразу чтобы влюбился читать – https://coopdobromir.ru приворот на кладбище по фото кто.
приворот на мужчину очень сильный на свечи. как снять матери приворот с сына с помощью молитвы
приворот на любовь к девушке читать приворот на сахар
приворот на секс мужчину.
http://canadianpharm.store/# canada drugs online reviews canadianpharm.store
reputable canadian online pharmacies: Pharmacies in Canada that ship to the US – canada drug pharmacy canadianpharm.store
reputable indian online pharmacy: indianpharmacy com – indianpharmacy com indianpharm.store
Thank you so much!
best online pharmacies in mexico Online Mexican pharmacy reputable mexican pharmacies online mexicanpharm.shop
canadian pharmacy no scripts: adderall canadian pharmacy – best canadian online pharmacy canadianpharm.store
http://canadianpharm.store/# reliable canadian pharmacy reviews canadianpharm.store
order isotretinoin sale buy accutane 10mg online cheap accutane 40mg for sale
kinoboomhd.com
그러므로 지금은 슬픈 얼굴로 감히 한 마디도 하지 못하고 너무 조심스럽습니다.
It is very comforting to see that others are suffering from the same problem as you, wow!
mexican mail order pharmacies: Online Mexican pharmacy – mexican pharmacy mexicanpharm.shop
my canadian pharmacy review Canada Pharmacy online canadian online drugstore canadianpharm.store
http://mexicanpharm.shop/# purple pharmacy mexico price list mexicanpharm.shop
reputable indian online pharmacy: Indian pharmacy to USA – best online pharmacy india indianpharm.store
https://canadianpharm.store/# canadian drugs pharmacy canadianpharm.store
buying prescription drugs in mexico: buying prescription drugs in mexico online – mexico pharmacy mexicanpharm.shop
Online medicine order: order medicine from india to usa – indian pharmacy indianpharm.store
https://mexicanpharm.shop/# mexican pharmacy mexicanpharm.shop
buy generic isotretinoin buy isotretinoin 10mg pill buy isotretinoin 20mg generic
indian pharmacies safe order medicine from india to usa online shopping pharmacy india indianpharm.store
canadian pharmacy sarasota: Licensed Online Pharmacy – drugs from canada canadianpharm.store
https://mexicanpharm.shop/# mexican drugstore online mexicanpharm.shop
Thanks for thr great article!
canadian pharmacy no scripts: best online canadian pharmacy – canada pharmacy canadianpharm.store
pharmacies in mexico that ship to usa Certified Pharmacy from Mexico purple pharmacy mexico price list mexicanpharm.shop
http://indianpharm.store/# cheapest online pharmacy india indianpharm.store
indian pharmacy paypal: online shopping pharmacy india – Online medicine home delivery indianpharm.store
purple pharmacy mexico price list: Online Mexican pharmacy – reputable mexican pharmacies online mexicanpharm.shop
https://indianpharm.store/# Online medicine order indianpharm.store
mexican rx online Certified Pharmacy from Mexico pharmacies in mexico that ship to usa mexicanpharm.shop
https://mexicanpharm.shop/# mexican rx online mexicanpharm.shop
canadian pharmacy ltd: Certified Online Pharmacy Canada – canada discount pharmacy canadianpharm.store
reputable canadian online pharmacies: canadian pharmacy online – canadian pharmacy canadianpharm.store
rybelsus tablets 7 mg
order amoxicillin 1000mg online amoxil over the counter buy generic amoxil over the counter
canadian pharmacy meds Canadian Pharmacy the canadian drugstore canadianpharm.store
https://canadianpharm.store/# canadian pharmacy 24 canadianpharm.store
buy albuterol sale purchase albuterol online cheap albuterol us
canadian pharmacy meds reviews: Licensed Online Pharmacy – cheap canadian pharmacy canadianpharm.store
world pharmacy india: Indian pharmacy to USA – online shopping pharmacy india indianpharm.store
buy allergy pills onlin buy albuterol 2mg pills albuterol pill
restaurant-lenvol.net
얼마나 많은 시간과 노력과 비용이 소요될까요?
buy ozempic from canada online
http://mexicanpharm.shop/# buying prescription drugs in mexico online mexicanpharm.shop
indian pharmacy order medicine from india to usa reputable indian pharmacies indianpharm.store
Greetings, Earth!
I am a Capybara, a small creature cherished for its endearing appearance and charming qualities!
Curious about my recent endeavors? I’ve decided to swap the jungle for the bustling city life.
Currently residing in the Netherlands, I’ve found a companion in the virtual realm!
Meet Xrumer, a software product, and its invaluable sidekick, Xevil. Together, we collaborate on ambitious projects that extend promotional messages to everyone in our database.
Our impact spans the globe, disseminating information about new projects, materials, and the lives of capybaras, both in the wild and in zoos – a truly significant endeavor!
Leveraging Xrumer for posting allows us to reach a vast audience, creating a robust link profile. We specialize in constructing site networks, establishing link levels, and enhancing domains for cohesion – a testament to the camaraderie of the capybara herd + Xrumer + Xevil!
If you’ve received a message from our team, why not consider availing our posting services? We’re open for business, friends, and eagerly await your tasks!
The Capybara herd tirelessly works around the clock to fulfill advertising tasks for leading SEO companies. We’re grateful for the opportunity, whether it’s to buy food or secure funds for our lives.
Curious about how people find us online? Here’s a glimpse of what we do:
https://capybara333.wordpress.com/
Xrumer mailing
Xrumer run
Xrumer posting
Xrumer website promotion
Xrumer site run
PBN site network boosting
Xrumer profile run, and much more!
And now, the English version!
Привет, мир!
Я Капибара, небольшое существо, которое полюбили за свою внешность и характерные черты!
Хотите узнать, чем я занимаюсь последнее время? Решил переместиться из джунглей в большой город.
В настоящее время я живу в Нидерландах и подружился с хорошим виртуальным спутником!
Его зовут программный продукт Xrumer, а его незаменимый компаньон — Xevil. Мы работаем вместе, создавая грандиозные проекты, позволяя каждому в нашей базе получать рекламные сообщения.
Информация распространяется по всему миру; люди узнают о новых проектах, материалах, жизни капибар в суровой дикой природе и зоопарках – это действительно важно!
Постинг с использованием Xrumer позволяет охватить огромную аудиторию и создать мощный ссылочный профиль. Мы строим сети сайтов, уровни ссылок, улучшаем домены для их склейки – всё это часть дружбы стада Капибар + Xrumer + Xevil!
Вы получили сообщение от нашей команды, и что мешает вам заказать постинг и наши услуги? Мы открыты для сотрудничества, друзья, и ждем ваших задач!
Стадо Капибар работает круглосуточно на благо рекламных задач ведущих SEO-компаний и очень благодарно за возможность купить еду или получить средства на жизнь.
Как нас ищут в сети, или, скорее, что мы делаем:
рассылка Хрумером
прогон Хрумером
постинг Хрумером
раскрутка сайта Хрумером
прогон сайта Хрумером
прокачка PNB сеток сайтов
прогон по профилям Хрумером и многое другое!
Удачи!!!
mexican border pharmacies shipping to usa: Online Pharmacies in Mexico – mexican pharmacy mexicanpharm.shop
https://canadianpharm.store/# canadian pharmacies online canadianpharm.store
buy amoxicillin 500mg generic amoxil 500mg for sale order amoxicillin 1000mg
http://canadadrugs.pro/# canadian pharmacy drugstore
most trusted canadian online pharmacy: canadiandrugstore.com – canadian prescription pharmacy
canadian pharmacy no prescription needed top rated canadian online pharmacy best non prescription online pharmacies
highest rated canadian pharmacy: online pharmacy review – online meds
https://canadadrugs.pro/# canadian drugstore reviews
order from canadian pharmacy: cheap drugs online – my canadian pharmacy
online pharmacies canada reviews: canadian pharmacy non prescription – medications with no prescription
cheap drugs canada safe online pharmacies in canada list of canada online pharmacies
http://canadadrugs.pro/# canada medications online
best online canadian pharmacy review: canadian drug pharmacy – reliable mexican pharmacies
buy generic azithromycin over the counter order zithromax 250mg pill zithromax price
canadian meds no prescription canadian drugstore prices recommended canadian pharmacies
brand augmentin 375mg buy augmentin 1000mg for sale clavulanate cost
best online canadian pharcharmy: meds without a doctor s prescription canada – canadian prescription
Hello!
Have you ever heard of X-GPT Writer: a unique keyword content generator based on the ChatGPT neural network?
I also haven’t, until I was advised to automate routine tasks with this software, I want to say one thing! Then I couldn’t believe
for a long time that ChatGPT is such a powerful product if it is used simultaneously in streaming, under the control of X-GPT Writer.
I thought it was just a utility, it was inexpensive, a friend gave a coupon for a 40% discount%:
94EB516BCF484B27
details of where to enter it are indicated on the website:
https://www.xtranslator.ru/x-gpt-writer/
I started trying, delving into it, bought 50 ChatGPT accounts at low prices and it started!
Now I easily generate and launch 3-4 new sites a week, batch unify entire folders and even create images
using the ChatGPT neural network and X-GPT Writer.
It’s worth a try, Friends, there’s a demo, everything is free, you won’t regret it)
Good luck!
Уникальные тексты с ChatGPT и X-GPTWriter
ChatGPT и X-GPTWriter в качестве инструментов синонимизации
ChatGPT и X-GPTWriter: новая эра контент-маркетинга
Где найти промо коды на X-GPTWriter
ChatGPT как инструмент для генерации контента
X-GPTWriter купоны на скидку
Уникальный контент с синонимизатором на базе ChatGPT
Создание оригинальных текстов с помощью синонимайзера на базе ChatGPT
ChatGPT и создание качественного контента
Синонимизация текста с X-GPTWriter и ChatGPT
https://canadadrugs.pro/# best canadian pharmacies
canada pharmacy no prescription: canada drugs online reviews – prescription prices
augmentin drug buy clavulanate pills for sale order generic augmentin
canadian world pharmacy medicine canada canadian pharmacy without prescription
Привет Всем!
Хотел сказать что постинг Хрумером реально работает, применяется
и имеет место быть, если рассматривать экономическую составляющую,
это в сотни раз выгоднее покупки ссылок, постов и др,
так же прогон Хрумером идет реальным образом,
Вас не размещают на каких-то самоподнятых сетках что будут забанены или закрыты,
совершенно разные сайты, домены, IP и локации, все как нужно!
Наша компания делала здесь:
https://progonxrumerom.wordpress.com/
Xrumer рассылка это отличный инструмент для SEO, дорвейщиков лого уровня, СМИ,
веб мастеров и тех кто имеет цель донести до других свою информацию.
Удачного развиия)
рассылка Хрумером
прогон Хрумером
постинг Хрумером
раскрутка сайта Хрумером
прогон сайта Хрумером
прокачка PNB сеток сайтов
прогон по профилям Хрумером и многое другое!
legitimate canadian pharmacy online: fda approved pharmacies in canada – canada drugs online review
http://canadadrugs.pro/# online pharmacy usa
buy cheap generic zithromax azithromycin uk buy azithromycin pills for sale
canadian drug store viagra: family pharmacy online – drug store online
drugstore online: canadian online pharmacies – canadian online pharmacies not requiring a prescription
https://canadadrugs.pro/# best online mexican pharmacy
rybelsus semaglutide
Thanks for thr great article!
digiapk.com
Hongzhi 황제는 무심코 웃으며 “후방으로 가서 책을 가져 오라고 요청하십시오. “라고 말했습니다.
canadian pharmacy without prescription: canadian pharmacy no prescription required – order canadian drugs
india online pharmacy: mexican pharmacy online reviews – top canadian online pharmacy
http://canadadrugs.pro/# canadian pharmacy meds
Hello!
I’m Dina, I’m 35, beautiful and sweet, I want to tell you about my discovery)
I used to have a negative view of many things, often worried about the environment, people, politics, and it began to have a bad effect on my health and quality of life in general.
The psychologist advised me to laugh more, and not to study what I can’t change, what’s the point!
I began to regularly read jokes and sites with humor, and after 2 months I became a different person, calmer and kinder, things went to the mountains and people want to be in my company more, there is no end of men.
I advise everyone who likes jokes, this site
https://www.anekdotor.ru/anekdoty-pro-stomatologov/
Everything is simple and about the case, read, laugh and be healthy!
Good luck friends)
Hello everybody!
I’m Masha, I’m 32, I live in England, I raise 2 children who go to school)
School is quite a lot of stress, both for children and for parents, and constant lessons and preparation for tests in specialized subjects drove Me crazy (
I became nervous, stopped sleeping with my husband and a nervous tic began, it was terrible…
It’s good that my friends advised me to find sites with solutions, and try to do homework according to their methodology.
By the way, a good website
https://www.controlworks.ru/kontrolnaja-za-1-chetvert-8-klass/
There are no ads, convenient search and a lot of valuable information about test papers!
To be honest, I began to sleep peacefully, sex and peace in the family were restored, thanks to such sites where you can find solutions and devote more time to your favorite things!
Good luck!
top rated canadian mail order pharmacies: get canadian drugs – my canadian pharmacy
Thank you so much!
modernkarachi.com
“그렇다면 말타고 사격하는 것이야말로 도시 공략에 가장 유리한 전술이지.”
http://canadadrugs.pro/# best canadian drug prices
Hello everybody!
I want to share a real experience, with age my sex power began to decrease, and eventually came to a deplorable level (
Even the most beautiful and young girls did not excite the right level of energy in me…
It was terrible and depression began when a friend told me that you need to read jokes and laugh every day, and everything will gradually get better.
Recommended this site to me
https://www.kompotanekdot.ru/anekdot-pro-traktor-s-dymkom/
I thought what nonsense, but there was nothing to do, and I began to laugh systematically and read everything about humor!
I didn’t believe it, but after 2 weeks, my potency became normal, and I was able to return to the love spaces and walk with models!
Thanks to the laughter and jokes, and be healthy)
I’m already 87 years old, but I’m still strong in bed)
pharmacy without dr prescriptions: reliable online drugstore – no prescription canadian pharmacies
canadian overnight pharmacy: canada prescription – great canadian pharmacy
http://canadadrugs.pro/# online pharmacies no prescriptions
omnacortil 5mg without prescription prednisolone 40mg over the counter cheap omnacortil online
canadian pharmacy drug prices: no prescription pharmacies – canadian drug company
levoxyl pill cheap synthroid generic order generic synthroid
drugs from canada without prescription: canadian pharmacy tadalafil – online prescription
http://canadadrugs.pro/# top rated online pharmacy
legitimate canadian pharmacy: canadian discount online pharmacy – online pharmacy reviews
levothyroxine drug purchase levothyroxine pills cheap levothyroxine pill
https://canadadrugs.pro/# canadiandrugstore com
buy prednisolone 10mg generic purchase prednisolone without prescription where to buy omnacortil without a prescription
https://edpill.cheap/# pills erectile dysfunction
reputable indian pharmacies: top 10 pharmacies in india – top 10 pharmacies in india
safe reliable canadian pharmacy canadian pharmacy online canadian online pharmacy
https://medicinefromindia.store/# online pharmacy india
100mg viagra without a doctor prescription: generic cialis without a doctor prescription – ed meds online without doctor prescription
prescription drugs: cheap cialis – ed meds online without prescription or membership
ed meds online without doctor prescription cheap cialis prescription drugs canada buy online
https://certifiedpharmacymexico.pro/# mexican drugstore online
https://edwithoutdoctorprescription.pro/# buy prescription drugs from india
viagra without a doctor prescription cialis without a doctor prescription viagra without a doctor prescription
reputable indian pharmacies: best india pharmacy – Online medicine order
https://certifiedpharmacymexico.pro/# buying prescription drugs in mexico online
mens erection pills medicine for impotence how to cure ed
buy generic gabapentin online gabapentin buy online gabapentin 600mg drug
precription drugs from canada: canadian online pharmacy – the canadian drugstore
https://edpill.cheap/# otc ed pills
order clomid 100mg online cheap serophene price clomid 50mg price
best ed pills non prescription generic cialis without a doctor prescription legal to buy prescription drugs without prescription
https://edwithoutdoctorprescription.pro/# non prescription erection pills
clomiphene 50mg tablet clomiphene 50mg drug clomiphene us
buy rybelsus in mexico
indian pharmacies safe: reputable indian pharmacies – reputable indian pharmacies
online shopping pharmacy india Online medicine home delivery online shopping pharmacy india
https://edpill.cheap/# buy ed pills online
order gabapentin 100mg pill gabapentin medication gabapentin 600mg brand
http://canadianinternationalpharmacy.pro/# canadian pharmacy online
reputable mexican pharmacies online: medicine in mexico pharmacies – reputable mexican pharmacies online
online pharmacy india indian pharmacy paypal mail order pharmacy india
http://edwithoutdoctorprescription.pro/# viagra without a doctor prescription walmart
best india pharmacy reputable indian pharmacies indianpharmacy com
http://edwithoutdoctorprescription.pro/# non prescription ed pills
rybelsus canada pharmacy prices
Здравствуйте!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в сжатые сроки? Это действительно трудно и ответственно, но важно не сдаваться и продолжать работать над учебными процессами, чем я и занимаюсь.
Для тех, кто умеет грамотно пользоваться интернетом и находить нужную информацию, это действительно оказывается полезным. Это помогает в процессе согласования и написания дипломной работы, и нет необходимости тратить время на посещение библиотек или встречи с дипломным руководителем. Если вам нужны хорошие источники для подготовки дипломных и курсовых работ, я могу поделиться полезными ссылками.
http://vuzdiploma.ru/
Желаю всем отличных оценок!
купить диплом прораба
купить диплом охранника
купить дипломы о высшем цены
купить диплом в губкине
купить диплом в красноярске
купить диплом в вольске
купить диплом в белогорске
купить диплом слесаря
купить диплом в донском
купить диплом нового образца
mexico pharmacies prescription drugs mexico pharmacies prescription drugs mexican border pharmacies shipping to usa
http://edwithoutdoctorprescription.pro/# cialis without a doctor’s prescription
chasemusik.com
이 Fang Jifan은 다행히 그를 꽤 잘 대하기 때문에 이렇게 노인을 속였습니다.
non prescription ed pills: discount prescription drugs – discount prescription drugs
buy lasix online diuretic buy generic furosemide order lasix 40mg online cheap
india pharmacy mail order best online pharmacy india cheapest online pharmacy india
https://medicinefromindia.store/# cheapest online pharmacy india
rivipaolo.com
Yang Tinghe는 이러한 질문이 차례로 던져지는 것을 처리할 방법이 없었습니다.
https://certifiedpharmacymexico.pro/# reputable mexican pharmacies online
mexico drug stores pharmacies mexico drug stores pharmacies purple pharmacy mexico price list
how to buy furosemide cost lasix 40mg furosemide 40mg price
http://medicinefromindia.store/# india pharmacy mail order
best rated canadian pharmacy canadianpharmacymeds com canadian mail order pharmacy
Good morning!
Have you ever heard of X-GPT Writer: a unique keyword content generator based on the ChatGPT neural network?
I also haven’t, until I was advised to automate routine tasks with this software, I want to say one thing! For a long time afterwards, I couldn’t believe
that ChatGPT was such a powerful product if it was used simultaneously in streaming, running X-GPT Writer.
I thought it was just a utility, it was inexpensive, a friend gave me a coupon for a 40% discount%:
94EB516BCF484B27
the details of where to enter it are indicated on the website:
https://www.xtranslator.ru/x-gpt-writer/
I started trying, delving into it, bought 50 ChatGPT accounts at low prices and off I went!
Now I easily generate and launch 3-4 new sites per week, batch unify entire folders and even create images
using the ChatGPT neural network and X-GPT Writer.
It’s worth a try, Friends, there’s a demo, everything is free, you won’t regret it)
Good luck!
Как сделать текст более уникальным с ChatGPT
Создание контента с помощью X-GPTWriter
ChatGPT для профессиональных копирайтеров и маркетологов
Покупка X-GPTWriter: лучшие предложения и скидки
Автоматизация создания текстов с X-GPTWriter
Преимущества использования X-GPTWriter для SEO
уникализатор текста через ChatGPT
Генератор синонимов с ChatGPT
Легкий способ создавать контент с X-GPTWriter
X-GPTWriter промо коды и скидки
legal to buy prescription drugs from canada: cialis without a doctor prescription canada – prescription drugs without doctor approval
sildenafil oral order viagra 50mg pills sildenafil women
https://edwithoutdoctorprescription.pro/# best ed pills non prescription
Hello everybody!
Have you ever heard of X-GPT Writer: a unique keyword content generator based on the ChatGPT neural network?
I also haven’t, until I was advised to automate routine tasks with this software, I want to say one thing! For a long time afterwards, I couldn’t believe
that ChatGPT was such a powerful product if it was used simultaneously in streaming, running X-GPT Writer.
I thought it was just a utility, it was inexpensive, a friend gave me a coupon for a 40% discount%:
94EB516BCF484B27
the details of where to enter it are indicated on the website:
https://www.xtranslator.ru/x-gpt-writer/
I started trying, delving into it, bought 50 ChatGPT accounts at low prices and off I went!
Now I easily generate and launch 3-4 new sites per week, batch unify entire folders and even create images
using the ChatGPT neural network and X-GPT Writer.
It’s worth a try, Friends, there’s a demo, everything is free, you won’t regret it)
Good luck!
ChatGPT в качестве синонимайзера текста
ChatGPT как инструмент для генерации контента
ChatGPT и создание качественного контента
Преимущества использования X-GPTWriter для SEO
ChatGPT и X-GPTWriter в качестве инструментов синонимизации
Автоматизированное создание текстов с помощью ChatGPT
синонимайзер текста на базе ChatGPT
ChatGPT и X-GPTWriter: новая эра контент-маркетинга
Как ChatGPT помогает в создании уникального текста
ChatGPT для уникального исходного контента
mexico drug stores pharmacies pharmacies in mexico that ship to usa buying prescription drugs in mexico
http://canadianinternationalpharmacy.pro/# cheap canadian pharmacy
viagra 50mg usa viagra 25 mg sildenafil medication
canadian family pharmacy canadian pharmacy prices canada cloud pharmacy
https://edwithoutdoctorprescription.pro/# prescription without a doctor’s prescription
Здравствуйте!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в кратчайшие сроки? Это действительно трудно и ответственно, но важно не падать духом и продолжать работать над учебными процессами, чем я и занимаюсь.
Для тех, кто умеет эффективно использовать интернет и находить нужную информацию, это оказывается весьма полезным. Это помогает в процессе согласования и написания дипломной работы, и нет необходимости тратить время на посещение библиотек или встречи с научным руководителем. Если вам нужны хорошие источники для подготовки дипломных и курсовых работ, я могу поделиться полезными ссылками.
http://vuzdiploma.ru/
Желаю всем отличных оценок!
купить диплом бакалавра
купить диплом в воронеже
купить диплом в саратове
купить диплом швеи
купить диплом в россоши
купить диплом в славянске-на-кубани
купить диплом в новокузнецке
купить диплом в тамбове
купить диплом в чебоксарах
купить диплом в череповце
Привет всем!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в сжатые сроки? Это действительно трудно и ответственно, но важно не сдаваться и продолжать работать над учебными процессами, чем я и занимаюсь.
Для тех, кто умеет грамотно пользоваться интернетом и находить нужную информацию, это действительно оказывается полезным. Это помогает в процессе согласования и написания дипломной работы, и нет необходимости тратить время на посещение библиотек или встречи с дипломным руководителем. Если вам нужны хорошие источники для подготовки дипломных и курсовых работ, я могу поделиться полезными ссылками.
http://vuzdiploma.ru/
Желаю всем отличных оценок!
купить диплом в ростове-на-дону
купить диплом в йошкар-оле
купить диплом в хабаровске
купить диплом косметолога
купить диплом в керчи
купить диплом в новокузнецке
купить технический диплом
купить диплом цена
купить диплом провизора
купить диплом в самаре
canadian pharmacies online: canadian pharmacy online ship to usa – canadian mail order pharmacy
mexican mail order pharmacies medicine in mexico pharmacies medication from mexico pharmacy
http://edwithoutdoctorprescription.pro/# viagra without a prescription
философия журналистики https://mir-ved.ru шиллер философия
cheap acticlate order monodox generic doxycycline usa
http://medicinefromindia.store/# india pharmacy
http://certifiedpharmacymexico.pro/# mexico pharmacies prescription drugs
treatment for ed best erection pills erection pills viagra online
сычев философия https://mir-ved.ru микеланджело философия
https://edpill.cheap/# ed medication online
Online medicine order online shopping pharmacy india india pharmacy
buy doxycycline 200mg generic doxycycline 100mg for sale cheap vibra-tabs
https://certifiedpharmacymexico.pro/# mexican pharmaceuticals online
best online pharmacies in mexico: mexican online pharmacies prescription drugs – purple pharmacy mexico price list
order semaglutide 14mg for sale cheap semaglutide semaglutide 14mg price
ed drugs online from canada legit canadian pharmacy canadianpharmacyworld com
Привет всем!
Стоит отметить, что статьи про строительство это очень интересно и увлекательно, узнаешь что-то новое и полезное!
Этот ресурс включает много статей на разные темы, рекомендую
https://inyoutube.net/stroitelstvo/vybiraem-peregorodochnyj-gazobeton.html
Удачного чтения!
Привет всем!
Стоит отметить, что статьи про строительство это очень интересно и увлекательно, узнаешь что-то новое и полезное!
Этот ресурс включает много статей на разные темы, рекомендую
http://tv-express.ru/samye-jenergosberegajushhie-materialy-dlja-stroitelstva-i-uteplenija.dhtm
Удачного чтения!
buy semaglutide tablets buy rybelsus for sale semaglutide for sale
mexico drug stores pharmacies pharmacies in mexico that ship to usa mexico drug stores pharmacies
mexico drug stores pharmacies п»їbest mexican online pharmacies best online pharmacies in mexico
wegovy buy from canada
Thanks for thr great article!
https://mexicanph.com/# mexican border pharmacies shipping to usa
mexican mail order pharmacies
best online pharmacies in mexico buying prescription drugs in mexico mexican rx online
mexican border pharmacies shipping to usa mexican rx online mexican rx online
Thanks for thr great article!
buying from online mexican pharmacy mexican pharmacy buying prescription drugs in mexico
Привет всем!
Бывало ли у вас случаи, когда приходилось писать дипломную работу в очень короткие сроки? Это действительно требует большой ответственности и усилий, но важно не унывать и продолжать двигаться вперед в процессе обучения, так же, как я это делаю.
Для тех, кто умеет разбираться в информации и осуществлять поиск в интернете, это действительно может оказаться полезным при согласовании и написании дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с научным руководителем. Здесь можно найти множество хороших данных для дипломных работ и курсовых. Вы можете изучить их, перейдя по ссылкам
https://extern-diplom.com/
Желаю всем отличных оценок!
купить диплом в нефтеюганске
купить диплом тренера
купить диплом в россоши
купить диплом с реестром
купить диплом в набережных челнах
где купить диплом
купить диплом в пскове
купить диплом в геленджике
купить диплом в выборге
купить диплом в усолье-сибирском
Привет всем!
Было ли у вас когда-либо так, что вы писали дипломную работу в кратчайшие сроки? Это действительно требует большой ответственности и усилий, но важно не сдаваться и продолжать активно участвовать в учебных процессах, как и я.
Для тех, кто умеет находить нужную информацию и анализировать ее в Интернете, это действительно может быть полезным в процессе согласования и написания дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с научным руководителем. Здесь доступны хорошие данные для дипломных работ и курсовых проектов; вы можете ознакомиться с ними, перейдя по ссылкам
https://extern-diplom.com/
Желаю всем отличных оценок!
купить диплом в заречном
купить диплом в муроме
купить диплом в нижним тагиле
купить диплом в бору
купить диплом стоматолога
купить диплом массажиста
купить диплом в новокуйбышевске
купить диплом повара
купить диплом программиста
куплю диплом с занесением
semaglutide order
global poker online roulette casino online gambling casinos
Здравствуйте!
Были ли у вас случаи, когда приходилось писать дипломную работу в кратчайшие сроки? Это действительно очень ответственно и тяжело, но важно не терять бодрость духа и продолжать активно участвовать в учебных процессах, как и я в данный момент.
Для тех, кто умеет находить и осваивать информацию в сети, это действительно оказывает огромную помощь в процессе согласования и написания дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с дипломным руководителем. Здесь представлены хорошие данные для дипломных и курсовых проектов; вы можете ознакомиться с ними, перейдя по ссылкам
https://diplom1.org/
Желаю всем отличных оценок!
купить диплом в салавате
купить диплом инженера строителя
где купить диплом среднем
купить диплом в верхней пышме
купить диплом в гуково
купить речной диплом
купить диплом в кызыле
купить диплом в чебоксарах
старые дипломы купить
купить диплом ссср
medication from mexico pharmacy medication from mexico pharmacy medication from mexico pharmacy
medicine in mexico pharmacies buying from online mexican pharmacy purple pharmacy mexico price list
mexico pharmacies prescription drugs purple pharmacy mexico price list mexico drug stores pharmacies
buy vardenafil tablets buy vardenafil 20mg levitra order
It is very comforting to see that others are suffering from the same problem as you, wow!
https://mexicanph.com/# mexican rx online
mexican drugstore online
pharmacies in mexico that ship to usa mexican rx online mexican rx online
п»їbest mexican online pharmacies mexico pharmacy mexico pharmacy
best online pharmacies in mexico mexican rx online purple pharmacy mexico price list
mexican online pharmacies prescription drugs pharmacies in mexico that ship to usa mexico pharmacy
mexico drug stores pharmacies mexican drugstore online mexican border pharmacies shipping to usa
https://mexicanph.shop/# buying prescription drugs in mexico online
best online pharmacies in mexico
mexican border pharmacies shipping to usa mexican rx online medication from mexico pharmacy
order lyrica 150mg generic order pregabalin 150mg pill buy pregabalin paypal
restaurant-lenvol.net
이것을보고 Wu Sili는 미소를 지으며 자신에게 말했습니다. 이 새로운 카운티 영주 … 유감입니다 …
mexican pharmaceuticals online mexico pharmacy mexico drug stores pharmacies
batman apollo пелевин
buying prescription drugs in mexico mexican pharmacy medicine in mexico pharmacies
purchase zithromax
buying prescription drugs in mexico online medicine in mexico pharmacies mexico pharmacies prescription drugs
best online pharmacies in mexico reputable mexican pharmacies online mexico pharmacy
where can i buy hydroxychloroquine order plaquenil pills buy plaquenil generic
buying prescription drugs in mexico online mexican rx online mexican pharmaceuticals online
buying from online mexican pharmacy mexican border pharmacies shipping to usa reputable mexican pharmacies online
https://mexicanph.com/# medication from mexico pharmacy
mexican mail order pharmacies
plaquenil 200mg ca hydroxychloroquine generic plaquenil 200mg ca
mexico pharmacies prescription drugs buying prescription drugs in mexico online mexican online pharmacies prescription drugs
mexico drug stores pharmacies mexico drug stores pharmacies mexican rx online
mexico pharmacies prescription drugs mexico drug stores pharmacies buying prescription drugs in mexico
mexican pharmaceuticals online mexican border pharmacies shipping to usa mexican pharmacy
triamcinolone oral purchase triamcinolone pills buy generic triamcinolone
mexican rx online buying prescription drugs in mexico online medicine in mexico pharmacies
mexico pharmacy mexican online pharmacies prescription drugs mexico pharmacies prescription drugs
It is very comforting to see that others are suffering from the same problem as you, wow!
buying prescription drugs in mexico purple pharmacy mexico price list best online pharmacies in mexico
best online pharmacies in mexico purple pharmacy mexico price list best mexican online pharmacies
medicine in mexico pharmacies mexico pharmacy buying from online mexican pharmacy
medicine in mexico pharmacies best mexican online pharmacies mexican pharmaceuticals online
mexico pharmacy mexico drug stores pharmacies mexican drugstore online
mexico drug stores pharmacies mexican drugstore online mexican rx online
buy triamcinolone 4mg generic triamcinolone over the counter purchase triamcinolone generic
purple pharmacy mexico price list mexico drug stores pharmacies buying prescription drugs in mexico online
https://mexicanph.shop/# mexican pharmaceuticals online
purple pharmacy mexico price list
baseballoutsider.com
Zhu Houzhao는 도울 수 없었지만 “그럼 Wang Shouren, 그런 것 같습니다. “라고 말했습니다.
mexico drug stores pharmacies mexican drugstore online best online pharmacies in mexico
pharmacies in mexico that ship to usa best online pharmacies in mexico buying prescription drugs in mexico online
mexico drug stores pharmacies mexican mail order pharmacies purple pharmacy mexico price list
mexican mail order pharmacies buying from online mexican pharmacy buying prescription drugs in mexico online
mexico pharmacy buying prescription drugs in mexico mexico drug stores pharmacies
medication from mexico pharmacy mexico drug stores pharmacies mexican pharmacy
mexico drug stores pharmacies best mexican online pharmacies mexican pharmaceuticals online
tadalafil india order cialis 10mg online cheap cialis mail order us
mexican pharmaceuticals online best online pharmacies in mexico medicine in mexico pharmacies
purple pharmacy mexico price list buying prescription drugs in mexico mexican pharmacy
mexico drug stores pharmacies best online pharmacies in mexico mexico drug stores pharmacies
I Always Learn Something New From Your Posts. Thank You For The Education!
generic tadalafil 40mg cialis super active buy tadalafil 10mg generic
Здравствуйте!
Бывало ли у вас так, что вам приходилось писать дипломную работу в кратчайшие сроки? Это действительно требует высокой степени ответственности и настойчивости, но важно не сдаваться и продолжать учебный процесс, так же, как и я.
Для тех, кто умеет исследовать и находить информацию в интернете, это может значительно облегчить процесс согласования и написания дипломной работы. Нет необходимости тратить время на походы в библиотеки или встречи с научным руководителем. Здесь представлена полезная информация для дипломных и курсовых проектов; вы можете ознакомиться с ней, перейдя по ссылкам
https://diplom1.org/
Желаю всем отличных оценок!
купить диплом энергетика
купить диплом вуза
купить диплом в копейске
купить диплом медсестры
купить диплом в туле
купить диплом охранника
купить диплом в кызыле
купить диплом в соликамске
купить диплом в перми
купить диплом в астрахани
buying from online mexican pharmacy medicine in mexico pharmacies purple pharmacy mexico price list
mexico pharmacy mexican border pharmacies shipping to usa buying prescription drugs in mexico
http://mexicanph.com/# purple pharmacy mexico price list
mexican rx online
oral desloratadine 5mg clarinex online buy order desloratadine generic
mexican pharmacy pharmacies in mexico that ship to usa mexico pharmacy
mexico drug stores pharmacies buying prescription drugs in mexico purple pharmacy mexico price list
Your blog is a treasure trove of information. Thank you for sharing your wisdom with us. Asheville can’t get enough!
mexico pharmacies prescription drugs medication from mexico pharmacy reputable mexican pharmacies online
Мой опыт обращения к магу с приворотом в Германии – gadalka v germanii отзывы
Живу я в небольшом городе в Германии, и найти среди кучи «магов» хорошего, трудно особенно в Германии. Намучилась я с этим очень. И как бывает, все решается на пьяную голову. Сидели с двоюродной сестрой, поведала ей свою проблему с мужем и о бесконечных поисках магов. Она очень удивилась, что я сразу не стала искать человека в России с Якутии или другого региона Дальнего востока – это можно сказать родина многих сильных шаманов и колдунов.
Порекомендовала мага, с которым сама работала. Поработала с ним и я.
Поэтому хотела бы написать отзыв о привороте на мужа, проведенном магом Романом Петровичем.
___________________________________________________________________________
Я хочу поделиться своим опытом использования услуг мага Романа Петровича с сайта https://cmag666.ru Ватсап 8 (984) 286-12-65
___________________________________________________________________________
Перед тем, как обратиться к нему, моя ситуация с мужем казалась мне безвыходной. Наш брак испытывал серьезные трудности, и наши отношения становились все более напряженными.
Мой муж, с которым мы прожили много лет, казался мне все более отстраненным и равнодушным. Он уходил в себя, избегал общения, а наши разговоры становились все реже и поверхностнее. Я испытывала огромную боль от того, что наша семья распадается, и что я теряю своего мужа. В итоге он еще и любовницу завел.
После долгих раздумий и поиска решения проблемы, я решила обратиться к магу Роману Петровичу за помощью.
Он провел для меня приворот на мужа – на все ушло 5 дней, и еще дал ряд простых рекомендаций, которым нужно было следовать до получения результата. Последовали дни ожидания
На 5 день после проведения приворота я почувствовала изменения в поведении мужа. Он стал проявлять больше внимания и заботы, мы снова начали общаться и находить общие интересы. Стали возвращаться чувства и заинтересованность мной как женщиной. Все быстро нормлизовалось в наших отношениях, с любовницей он порвал все контакты.
Сейчас, спустя несколько месяцев после проведения приворота, я вижу, что наш брак стал крепким, стабильным и счастливым, как и раньше! Мы с мужем снова чувствуем себя близкими и любящими людьми.
Я благодарна магу Роману Петровичу за его помощь и поддержку в трудный момент!
Теги кто знает хорошую бабушку в германии отзывы – маг в германии отзывы
гадалка в германии отзывы – маг в германии отзывы
маг в германии отзывы – приворот в германии отзывы
mexico pharmacy reputable mexican pharmacies online mexico drug stores pharmacies
mexican rx online mexican online pharmacies prescription drugs mexico pharmacies prescription drugs
mexico pharmacy mexican border pharmacies shipping to usa mexican drugstore online
purple pharmacy mexico price list buying from online mexican pharmacy mexico drug stores pharmacies
purchase desloratadine online buy desloratadine 5mg generic desloratadine tablet
mexican rx online mexican drugstore online mexican pharmaceuticals online
buying prescription drugs in mexico buying from online mexican pharmacy medicine in mexico pharmacies
purple pharmacy mexico price list medicine in mexico pharmacies reputable mexican pharmacies online
best mexican online pharmacies pharmacies in mexico that ship to usa medicine in mexico pharmacies
mexico pharmacies prescription drugs mexico drug stores pharmacies purple pharmacy mexico price list
Your blog is a treasure chest of wisdom and insight. We’re grateful to be readers from Asheville!
mexican rx online mexican border pharmacies shipping to usa mexican border pharmacies shipping to usa
http://mexicanph.shop/# mexican mail order pharmacies
mexican online pharmacies prescription drugs
medication from mexico pharmacy medication from mexico pharmacy mexican border pharmacies shipping to usa
medication from mexico pharmacy mexico drug stores pharmacies mexico drug stores pharmacies
mexican pharmacy best online pharmacies in mexico mexico pharmacy
medicine in mexico pharmacies buying prescription drugs in mexico buying prescription drugs in mexico online
Your blog is like a ray of sunshine on a cloudy day – uplifting and inspiring. Sending love from Asheville!
brand cenforce 50mg cenforce for sale online order cenforce 50mg generic
Thank you for enriching our lives with your wonderful blog. Asheville is blessed to have you!
It is very comforting to see that others are suffering from the same problem as you, wow!
buying prescription drugs in mexico online mexican rx online medication from mexico pharmacy
п»їbest mexican online pharmacies medicine in mexico pharmacies mexican mail order pharmacies
Your writing has a way of drawing readers in and keeping them engaged till the very end. Asheville appreciates your talent!
homefronttoheartland.com
그러나 당신은 당신이 옳다고 생각합니까, 그렇게 할 수 있습니까?
Your words have the power to uplift and inspire. Thank you for sharing your gift with us. Asheville loves your blog!
buy cenforce without a prescription generic cenforce order cenforce 50mg for sale
mexican border pharmacies shipping to usa mexico drug stores pharmacies mexico pharmacies prescription drugs
mexican pharmaceuticals online buying prescription drugs in mexico online buying prescription drugs in mexico online
mexican pharmaceuticals online п»їbest mexican online pharmacies mexican pharmacy
Мой опыт обращения к магу с приворотом в Германии – gadalka v germanii отзывы
Живу я в небольшом городе в Германии, и найти среди кучи «магов» хорошего, трудно особенно в Германии. Намучилась я с этим очень. И как бывает, все решается на пьяную голову. Сидели с двоюродной сестрой, поведала ей свою проблему с мужем и о бесконечных поисках магов. Она очень удивилась, что я сразу не стала искать человека в России с Якутии или другого региона Дальнего востока – это можно сказать родина многих сильных шаманов и колдунов.
Порекомендовала мага, с которым сама работала. Поработала с ним и я.
Поэтому хотела бы написать отзыв о привороте на мужа, проведенном магом Романом Петровичем.
___________________________________________________________________________
Я хочу поделиться своим опытом использования услуг мага Романа Петровича с сайта https://cmag666.ru Ватсап 8 (984) 286-12-65
___________________________________________________________________________
Перед тем, как обратиться к нему, моя ситуация с мужем казалась мне безвыходной. Наш брак испытывал серьезные трудности, и наши отношения становились все более напряженными.
Мой муж, с которым мы прожили много лет, казался мне все более отстраненным и равнодушным. Он уходил в себя, избегал общения, а наши разговоры становились все реже и поверхностнее. Я испытывала огромную боль от того, что наша семья распадается, и что я теряю своего мужа. В итоге он еще и любовницу завел.
После долгих раздумий и поиска решения проблемы, я решила обратиться к магу Роману Петровичу за помощью.
Он провел для меня приворот на мужа – на все ушло 5 дней, и еще дал ряд простых рекомендаций, которым нужно было следовать до получения результата. Последовали дни ожидания
На 5 день после проведения приворота я почувствовала изменения в поведении мужа. Он стал проявлять больше внимания и заботы, мы снова начали общаться и находить общие интересы. Стали возвращаться чувства и заинтересованность мной как женщиной. Все быстро нормлизовалось в наших отношениях, с любовницей он порвал все контакты.
Сейчас, спустя несколько месяцев после проведения приворота, я вижу, что наш брак стал крепким, стабильным и счастливым, как и раньше! Мы с мужем снова чувствуем себя близкими и любящими людьми.
Я благодарна магу Роману Петровичу (Ватсап 8(984)286-12-65)за его помощь и поддержку в трудный момент!
Теги приворот в германии отзывы – гадалка в германии отзывы
приворот в германии отзывы – ясновидящая в германии отзывы 8(984)286-12-65
ясновидящие в германии отзывы – приворот в германии отзывы
buying prescription drugs in mexico online mexican pharmaceuticals online buying from online mexican pharmacy
mexican pharmaceuticals online buying prescription drugs in mexico mexican mail order pharmacies
Отзыв о привороте, и о маге сделавшем приворот.
+
+
Были проблемы с мужем довольно давно. А в последний год отношения стали сыпаться очень быстро, все разурушилось до конца буквально на глазах. Особенно с появлением любовницы, это была коллега сработы. А у нас двое детей. Их я и сама могла обеспечить более чем! Но вот любила мужа, и хоте, чтобы дети росли с рожным отцом.
Обращалась много к кому, но доверия не было даже при первом общение. Случайно встретились с давней подругой. Разговорились о проблемах. Она посоветовал сильного мага с Дальнего Востока.
Обратилась к нему за приворотом, хотя были конечно сомнения. Звать его Роман Петрович. Берет за работу не сильно много по сравнению с другими, делает все быстро и в срок, не продает и всегда отвечает на возникающие вопросы. Вернул мужа мне за 7 дней, работу проводил 2 дня.
Очень довольна!
________________________
Обратиться к нему можно через сайт https://cmag666.ru или ватсап 8 (984) 286-12-65 – это настоящий маг и просто добрый человек, отлично знающий свое дело!
____________________________________________________________________________________
Сайт ищут по тегам #
# Ясновидящая # маге # отзывы # экстрасенс # гадалка
консультация с магом
марго мэджик таро
официальный сайт слепой бабушки нины
черная ведьма отзывы
эзочат ком отзывы
литвин сайт официальный
светлана из тик тока
отзыв гадалка маг марина таролог
моисей некропольский кто это
мирослава буш видео
люди продавшие душу дьяволу отзывы
гадалка нелли
ксения авито
ольга таро руны ютуб
ирина пинчук отзывы
ольга сидорук школа магии
проверенный специалист маг
buy loratadine without a prescription order claritin without prescription order claritin 10mg
mexican mail order pharmacies mexican drugstore online buying from online mexican pharmacy
Thank you for enriching our lives with your blog. Asheville sends its warmest regards!
mexican pharmacy mexico pharmacies prescription drugs buying prescription drugs in mexico
Thank you for enriching our lives with your blog. Asheville sends its warmest regards!
п»їbest mexican online pharmacies buying prescription drugs in mexico buying prescription drugs in mexico
http://mexicanph.shop/# mexican border pharmacies shipping to usa
mexico drug stores pharmacies
medicine in mexico pharmacies mexican pharmacy best online pharmacies in mexico
mexico pharmacies prescription drugs mexican border pharmacies shipping to usa purple pharmacy mexico price list
buying prescription drugs in mexico online medication from mexico pharmacy pharmacies in mexico that ship to usa
can metformin cause diarrhea
mexico pharmacies prescription drugs mexico drug stores pharmacies best mexican online pharmacies
mexican mail order pharmacies mexico pharmacies prescription drugs mexico drug stores pharmacies
order loratadine 10mg pills buy cheap loratadine loratadine canada
wegovy pill form
Здравствуйте!Хочу рассказать о своем опыте работы с магом Романом Петровичем с сайта https://cmag666.ru. Я обратилась к нему, когда мои отношения с партнером стали испытывать серьезные трудности. Роман Петрович предложил мне кладбищенский приворот для восстановления любви и страсти в нашем отношении. Я была приятно удивлена результатами: наши отношения стали более глубокими и страстными, и мы снова радуемся вместе. Большое спасибо, Роману Петровичу, за его помощь и поддержку!Отзыв только хороший, работа сделанна на 5+
-кладбищенский приворот отзывы кто делал форум
-приворот кладбищенские отзывы
-кладбищенский приворот отзывы кто заказывал
-кладбищенский приворот кто делал отзывы
-отзывы тех кто делал кладбищенский приворот
medicine in mexico pharmacies medication from mexico pharmacy mexican rx online
Your posts always leave me feeling enlightened and inspired. Thank you for sharing your knowledge with us. Asheville sends its love!
Thank you for sharing such insightful content! In Asheville, we love your blog and can’t wait to come back for more.
Отзывы о приворотах в Екатеринбурге
—————————————–
Поиски настоящего мага привели меня на сайт Романа Петровича, и я решила попробовать снова. Будучи из Дальнего Востока, родины шаманов, Роман Петрович вызвал мое доверие, и я обратилась к нему за помощью в восстановлении чувств моего мужа.Работа Романа Петровича действительно поразила меня. Его профессионализм и внимание к моей ситуации впечатлили меня. Благодаря его помощи я снова чувствую себя счастливой и уверенной в нашем будущем вместе. Он настоящий мастер своего дела, и я безмерно благодарна ему за все, что он сделал для нашей семьи.Хочу поделиться своим незабываемым опытом работы с магом Романом Петровичем с сайта https://cmag666.ru. Проживая в Екатеринбурге, я столкнулась с трудностями в отношениях со своим мужем. Попытки решить проблемы с мужем при помощи местных магов не привели к желаемому результату.Я рекомендую Романа Петровича всем, кто столкнулся с проблемами в своих отношениях. Его помощь – это настоящее чудо, которое может изменить вашу жизнь к лучшему. Спасибо, Роман Петрович, за ваше волшебство и преданность своему делу!С каждым днем я замечала, как наши отношения становились все более гармоничными и близкими. Муж начал проявлять больше внимания и заботы, а его чувства к мне стали стойчивыми и глубокими. Благодаря кладбищенскому привороту, наш брак стал еще крепче и устойчивее.С Романом Петровичем мы обсудили мою ситуацию, и он предложил мне кладбищенский приворот для возврата чувств моего мужа. Я решила довериться его опыту и приступила к ритуалу с надеждой на лучшее.
– отзывы о приворотах екатеринбург
– приворот екатеринбурге
– привороты екатеринбург
– приворот отзывы екатеринбург
– приворот по фото екатеринбург
mexico pharmacy buying from online mexican pharmacy mexico pharmacies prescription drugs
mexican mail order pharmacies buying prescription drugs in mexico mexican drugstore online
rybelsus mexico
https://buyprednisone.store/# generic prednisone pills
https://amoxil.cheap/# where can i buy amoxicillin online
purchase prednisone from india: prednisone 10mg prices – can i order prednisone
generic lisinopril 40 mg lisinopril 20 mg canadian lisinopril 10 mg canada
chloroquine ca aralen 250mg sale order generic chloroquine 250mg
https://stromectol.fun/# cheap stromectol
Хочу поделиться своим невероятным опытом работы с магом Романом Петровичем с сайта https://cmag666.ru. Когда я оказалась в сложной ситуации со своим любимым человеком, я чувствовала, что моя жизнь рушится. Он начал дистанцироваться, и я не понимала, что происходит. Но мне посоветовали обратиться к Роману Петровичу, и это был лучший шаг в моей жизни.
Роман Петрович выслушал мои проблемы и предложил мне кладбищенский приворот для восстановления наших отношений. Я полностью доверила ему свои чувства и приступила к ритуалу с надеждой на лучшее.
С каждым днем я замечала, как наша связь становится все крепче и глубже. Мы начали общаться более открыто и искренне, а мои чувства к нему стали только усиливаться. Благодаря кладбищенскому привороту, наша любовь стала еще более крепкой и стойкой.
Работа Романа Петровича действительно поразила меня. Его внимание к деталям и профессионализм впечатлили меня. Благодаря его помощи я снова чувствую, что моя жизнь наполнена смыслом и радостью. Он настоящий мастер своего дела, и я безмерно благодарна ему за все, что он сделал для меня.
Я рекомендую Романа Петровича всем, кто столкнулся с проблемами в своих отношениях. Его помощь – это настоящий подарок судьбы, который может изменить вашу жизнь к лучшему. Спасибо, Роман Петрович, за вашу помощь и волшебство!
-кому помог кладбищенский приворот отзывы
-кладбищенский приворот отзывы кто
-отзывы тех на кого делали кладбищенский приворот
-кладбищенские привороты отзывы кто
-кладбищенский приворот отзывы о нем
Вот мой реальный отзыв о заказе приворота на мужа.
_____________________________________________________
Я долго искала хорошего мага в Москве, но, кажется, все мои попытки были напрасными. Разочарованная и безнадежная, я стала обращаться к друзьям и знакомым за советом. И тут одна из моих подруг порекомендовала мне обратиться за помощью к магу с Дальнего Востока – Роману Петровичу с сайта.
Сначала я была немного скептически настроена – ведь удаленное заклинание казалось мне чем-то из области фантастики. Но моя подруга уверяла меня, что Роман Петрович – настоящий профессионал в своем деле. И я решила попробовать.
Когда я связалась с Романом Петровичем через его сайт https://cmag666.ru и рассказала ему о своей ситуации, он проявил искреннее понимание и сострадание. Он объяснил мне, как работает приворот, и какие изменения я могу ожидать. Я заказала у него приворот на моего мужа и начала ждать результатов.
Через несколько недель я заметила, что мой муж стал относиться ко мне по-другому. Он стал более внимательным и заботливым, и наши отношения начали испытывать явное улучшение. Я была поражена результатом!
Сейчас, когда я смотрю на нашу семью, я благодарна Роману Петровичу за его помощь. Он действительно знает свое дело и умеет помогать людям в трудных ситуациях. Если у вас есть проблемы в отношениях и вы ищете решение, я настоятельно рекомендую обратиться к Роману Петровичу – он сделает все возможное, чтобы помочь вам.
– приворот отзывы москва
– приворот недорого в москве
– бесплатный приворот москва
– приворот в москве бесплатно
– приворот парня москва
generic amoxicillin 500mg: amoxicillin 50 mg tablets – amoxicillin price canada
buy chloroquine 250mg pill purchase chloroquine for sale purchase chloroquine online cheap
Отзывы о приворотах в Екатеринбурге
—————————————–
Хочу поделиться своим отзывом о работе с магом Романом Петровичем с сайта https://cmag666.ru. Я из провинции, живу в небольшой деревне в окрестностях Екатеринбурга, и когда у меня возникли проблемы с мужем, я честно говоря, не знала к кому обратиться. Местные “маги” из Екатеринбурга ничем не помогли, и я уже было решила, что все потеряно. А в нашей деревне таких людей нет, все нынче в другое погружены, не до человеческих проблем им!
Но случайно наткнулась на сайт Романа Петровича, и что удивительно, он тоже с Дальнего Востока, как и мы с мужем, откуда много шаманов. Решила попробовать в последний раз и не прогадала!
С Романом Петровичем мы поговорили о моих проблемах, и он предложил мне кладбищенский приворот для возврата чувств моего мужа. Решила довериться его опыту и приступила к ритуалу с надеждой на лучшее.
Каждый день наши отношения становились все лучше. Муж стал внимательнее и заботливее, а я почувствовала, что его чувства ко мне вернулись. Благодаря кладбищенскому привороту, наша семья стала крепче и счастливее.
Я очень благодарна Роману Петровичу за помощь. Он настоящий профессионал своего дела и знает, как вернуть счастье в семью. Я рекомендую его всем, кто столкнулся с проблемами в отношениях. Спасибо, Роман Петрович, за ваше волшебство и поддержку!
– приворот в екатеринбурге отзывы
– приворот екатеринбург кто делает настоящий
– кто делал приворот екатеринбург
– кто делал приворот в екатеринбурге
– в екатеринбурге приворот
Мой отзыв о том, как я заказала приворот на парня. Стоит ли делать?
В том году моя жизнь перевернулась вверх дном, когда я узнала о том, что мой парень, с которым мы были вместе уже несколько лет, встречается с другой. Внезапное открытие подорвало основы наших отношений, и я была на грани отчаяния. Не зная, куда идти и что делать, я решила обратиться к Роману Петровичу по совету сестры, и могу сказать, что это было решение, которое изменило мою жизнь. Сестра дала адрес его сайта https://cmag666.ru
Роман Петрович провел расклад карт, который оказался точным и вразумительным, давая мне надежду на возвращение любимого человека. Он порекомендовал мне заказать белый приворот на моего парня, чтобы вернуть его обратно ко мне. Я последовала его совету, и результат меня поразил. Белый приворот оказался мощным инструментом, который вернул моего парня ко мне, и наши отношения стали крепче и глубже.
Я глубоко признательна Роману Петровичу за его помощь и поддержку в этот трудный период. Без его профессионализма и заботы я бы не смогла преодолеть этот кризис. Если у вас возникли подобные проблемы в отношениях, я настоятельно рекомендую обратиться к Роману Петровичу.
Сайт ищут по тегам
– бесплатный приворот как заказать
– заказать приворот отзывы
– заказать приворот парня
– что делать когда заказал приворот
– какой молебен заказать от приворота
cheap generic prednisone: buy prednisone from canada – prednisone 2.5 mg tab
ivermectin 0.1 ivermectin 5 mg price buy ivermectin pills
https://lisinopril.top/# lisinopril 30
lasix pills: Over The Counter Lasix – furosemide 100mg
buy priligy 30mg generic how to buy cytotec order misoprostol 200mcg generic
http://lisinopril.top/# lisinopril 20mg india
http://lisinopril.top/# lisinopril 10mg
ivermectin cream cost ivermectin cream 1% ivermectin buy
prednisone 2.5 tablet: buy prednisone without prescription paypal – prednisone uk
https://furosemide.guru/# lasix
buy amoxicillin online cheap: buy amoxicillin canada – amoxicillin 250 mg price in india
Your posts always leave me feeling inspired and motivated. Thank you for brightening our days. Asheville loves your blog!
I’ve learned so much from your blog posts. Thank you for sharing your expertise. Asheville appreciates it greatly!
buy dapoxetine 60mg online cheap order priligy generic order cytotec 200mcg online cheap
http://furosemide.guru/# generic lasix
purchase oral ivermectin stromectol 3 mg ivermectin 90 mg
lisinopril without rx: medication lisinopril 20 mg – zestoretic 20 12.5
price of lisinopril in india: lisinopril 1 mg tablet – lisinopril 5 mg tablet price in india
svetlanamag ru – svetlanamagg @ yandex ru
Благодаря ритуалу приворота у мага Светланы, я смогла привлечь внимание парня, в который была влюблена. Теперь он стал проявлять ко мне больше внимания, и мы начали встречаться. Спасибо вам, Светлана, за вашу помощь!
-проверенные маги и колдуны отзывы
-настоящие маги из битвы экстрасенсов
-отзывы настоящих магов
-имя настоящего мага
buy amoxicillin 500mg uk: amoxicillin 500 mg brand name – amoxicillin 250 mg capsule
https://stromectol.fun/# ivermectin nz
https://buyprednisone.store/# prednisone buy cheap
how much is ivermectin ivermectin cream canada cost stromectol 0.5 mg
wegovy generic cost
lisinopril 40 mg price: prinivil generic – zestril pill
https://amoxil.cheap/# generic amoxicillin over the counter
prednisone price: prednisone 10 mg daily – prednisone cream
Как я заказала приворот на Новосибирске – правдивый отзыв
У себя в Новосибирске я так и не смогла найти настоящего мага. Моя история с магом Романом Петровичем началась с того, что я оказалась в сложной жизненной ситуации, где моя семейная жизнь висела на волоске. Проблемы в отношениях с мужем достигли своего пика, и мне казалось, что я совсем безысходна. В поисках помощи я обратилась к нескольким магам в своем городе, но результаты были неприемлемыми.
Вот тогда-то моя подруга посоветовала мне обратиться к Роману Петровичу с Дальнего Востока. Я была очень скептически настроена из-за расстояния и сомневалась, сможет ли кто-то помочь мне на расстоянии. Но мои сомнения рассеялись с первой же консультации с Романом Петровичем.
Он не только выслушал мою проблему с вниманием, но и предложил мне план действий, который казался мне реальным и эффективным. Я заказала у него любовный приворот на моего мужа и начала ждать результатов.
Через несколько недель я заметила изменения в отношениях с мужем – он стал более внимательным и заботливым. Наша связь стала крепче, и мы снова почувствовали ту любовь и сближение, которые когда-то были между нами.
Я благодарна Роману Петровичу за его помощь и поддержку в трудный момент моей жизни. Он действительно знает, как помочь людям восстановить свои отношения и вернуть счастье в семью.
Если вы столкнулись с подобными проблемами и ищете решение, я настоятельно рекомендую обратиться к Роману Петровичу – он профессионал своего дела и поможет вам вернуть гармонию в вашу жизнь.
Сайт для обращений: https://cmag666.ru
Сайт ищут по тегам
_______________________________________________________________
-кто делал привороты в новосибирске
-приворот на любовь в новосибирске
-кто в новосибирске может сделать приворот
-привороты в новосибирске
-приворот новосибирск цена
order metformin 1000mg generic buy metformin 500mg generic buy glycomet 500mg pills
Здравствуйте!
Промокоды для интернет-магазина Эльдорадо представляют собой специальные коды, которые можно использовать при оформлении заказа на официальном веб-сайте компании.
Они приносят дополнительные преимущества покупателям в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как их найти? Чаще всего промокоды предоставляются в рамках специальных акций компании, которые могут проводиться на ее официальном веб-сайте,
в социальных сетях или на ресурсах, таких как проект free-promocode.ru
Сайт самых свежих и проверенных промокодов магазина Эльдорадо https://free-promocode.ru
Удачных покупок!
Специальные предложения и скидки Эльдорадо
Экономь с промокодами Эльдорадо
Специальные предложения Эльдорадо
Подарки и скидки от Эльдорадо
Промокоды для сэкономленных денег в Эльдорадо
Удачи!
furosemide 100 mg Over The Counter Lasix furosemida
http://furosemide.guru/# lasix furosemide 40 mg
Your blog is a true gift to the world. We’re big fans from Asheville!
can you buy amoxicillin over the counter canada: canadian pharmacy amoxicillin – amoxicillin 500 mg capsule
Отзыв о привороте маг Александра (magpa666 @ bk ru) – magpomosh ru
Я решил обратиться к магу Александре с сайта magpomosh ru (magpomosh ru) после того, как моя жизнь стала полна разочарований и неудач в личных отношениях. На протяжении длительного времени я пытался найти выход из сложившейся ситуации, но все мои усилия оказывались напрасными.
Встреча с Александрой стала для меня настоящим откровением. Она внимательно выслушала мои проблемы и предложила мне ряд решений, среди которых был и ритуал приворота. Я согласился, хотя и был в некотором сомнении.
Однако результат превзошел все мои ожидания. Через некоторое время после проведения ритуала я заметил изменения в отношениях с партнером – они стали более гармоничными и теплыми. Мы начали понимать друг друга лучше, а наша любовь стала только крепче. Благодаря магу Александре я снова обрел веру в свои силы и смог по-настоящему ощутить радость жизни. Спасибо вам, Александра, за ваш талант и помощь!
Теги – отзыв magpomosh ru отзыв magpa666 @ bk ru
_________________________________________________________
Сайт ищут по тегам:
портал проверенных магов настоящие маги москвы настоящего мага найти
настоящие маги в екатеринбурге настоящий союз магов где найти настоящих магов
маг настоящий помогу проверенного мага колдуна помощь настоящего мага
как стать магом настоящей жизни маги прошлого в настоящем skyrim одежда для настоящих магов
Хочу выразить благодарность магу Роману Петровичу с сайта cmag666.ru за его Вуду-приворот! Результаты просто поразительны! Моя давняя мечта о встрече с идеальным партнером осуществилась благодаря его ритуалу. Я счастливее, чем когда-либо! Благодарю вас, Роман Петрович, за ваш талант и помощь!
Запросы сайта в поиске
___________________________________________________________
отзывы о привороте вуду приворот на кукле вуду отзывы приворот на кукле вуду отзывы
куклу вуду приворот на кто делал отзывы приворот вуду отзывы кто делал вуду приворот отзывы
Thanks for thr great article!
Приветствую всех!
Промокоды для интернет-магазина Эльдорадо – это уникальные коды, которые можно использовать при оформлении заказа на официальном веб-сайте компании.
Они предоставляют дополнительные преимущества клиентам в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как найти такие промокоды для Эльдорадо? Обычно они предоставляются в рамках специальных акций компании, которые могут быть организованы
на ее официальном веб-сайте, в социальных сетях или на специализированных ресурсах, например, на сайте free-promocode.ru,
который предлагает самые свежие и проверенные промокоды
Сайт самых свежих и проверенных промокодов магазина Эльдорадо https://free-promocode.ru
Удачных покупок!
Промокоды для сэкономленных денег в Эльдорадо
выгодный промокод Эльдорадо
Эксклюзивные промо-коды Эльдорадо
актуальные промокоды Эльдорадо
рабочие промокоды Эльдорадо
Удачи!
cheap xenical buy diltiazem 180mg pill order diltiazem generic
buy glucophage generic glucophage 500mg oral buy glycomet 500mg online
http://amoxil.cheap/# can you purchase amoxicillin online
prednisone coupon: prednisone over the counter south africa – best pharmacy prednisone
amoxicillin 500 mg brand name: amoxicillin 750 mg price – cheap amoxicillin 500mg
where can you get amoxicillin amoxicillin 500mg capsules price buy amoxicillin online no prescription
http://amoxil.cheap/# amoxicillin 250 mg price in india
http://lisinopril.top/# lisinopril 10 mg canada
hihouse420.com
이생에서 그의 아버지는 일찍 세상을 떠났고 그의 결혼 생활은 행복한 것으로 간주되지 않았습니다.
furosemide onset peak duration
zoloft dosage 100mg
Your blog is like a cup of hot cocoa on a chilly day – comforting and delightful. Sending love from Asheville!
buy xenical paypal orlistat 60mg uk buy diltiazem 180mg pills
lisinopril tablets india: zestril 30mg generic – lisinopril prescription coupon
I always look forward to your latest posts. They never fail to impress! Sending love from Asheville.
http://amoxil.cheap/# buying amoxicillin online
sm-casino1.com
Wang Bushi의 얼굴은 약간의 공손함이 없이 단호했습니다.
purchase oral ivermectin: stromectol pill for humans – where to buy ivermectin
zestoretic 10 12.5 mg lisinopril 5 mg medicine lisinopril medication generic
ivermectin 9mg: ivermectin pills canada – ivermectin lice oral
https://amoxil.cheap/# buy amoxicillin online no prescription
Thanks for thr great article!
ivermectin pills: ivermectin generic name – ivermectin 5 mg price
http://lisinopril.top/# lisinopril 5 mg for sale
Отзывы – Помогли – приворот на женатого https://cmag666.ru Ватсап 8 (984) 286-12-65
проверенные маги настоящие – форум о настоящих магах
мастер владислав отзывы не внушает доверие – заказала снятие порчи у https://cmag666.ru Ватсап 8 (984) 286-12-65
приворот на парня в домашних – заговор на присушку любимого читать
Your blog is a testament to your dedication and expertise. We’re proud fans from Asheville!
ivermectin 500ml can you buy stromectol over the counter ivermectin 3 mg tabs
http://amoxil.cheap/# prescription for amoxicillin
generic semaglutide
amoxicillin 500mg: amoxicillin no prescipion – buy amoxil
lasix furosemide 40 mg: buy furosemide online – lasix 20 mg
https://lisinopril.top/# lisinopril tab 100mg
alternatives to lisinopril
what does flagyl treat
http://stromectol.fun/# ivermectin 6mg tablet for lice
lasix 100 mg: Buy Furosemide – lasix 20 mg
buy prednisone without rx canada buy prednisone online prednisone best price
https://amoxil.cheap/# amoxicillin over the counter in canada
Thank you for being a beacon of knowledge and inspiration through your blog. Asheville appreciates you!
stromectol ireland: stromectol 3mg – ivermectin goodrx
https://stromectol.fun/# stromectol pill for humans
svetlanamag ru – svetlanamagg @ yandex ru
Благодаря ритуалу приворота у мага Светланы, я смогла привлечь внимание парня, в который была влюблена. Теперь он стал проявлять ко мне больше внимания, и мы начали встречаться. Спасибо вам, Светлана, за вашу помощь!
-настоящий маг помог
-настоящие маги колдуны
-анастасия ворожея отзывы проверенный маг
-как найти настоящего черного мага
furosemide 100mg: Buy Furosemide – buy lasix online
Thank you for enriching our lives with your wonderful blog. Asheville is blessed to have you!
https://stromectol.fun/# ivermectin brand name
zestoretic 20 mg lisinopril generic price comparison lisinopril oral
ivermectin uk: ivermectin 0.08 oral solution – stromectol for sale
acyclovir 800mg sale buy zovirax sale purchase zyloprim online
semaglutide pill form
https://furosemide.guru/# generic lasix
lfchungary.com
Zhu Houzhao는 Dowager 황후를 향해 “증조모, Sun Chen은 노래를 잘합니까? “라고 말했습니다.
https://amoxil.cheap/# amoxicillin 1000 mg capsule
amoxicillin for sale: purchase amoxicillin online – amoxicillin online no prescription
order norvasc online buy norvasc 5mg online cheap buy cheap generic norvasc
amoxicillin 500mg capsule buy online: amoxicillin 50 mg tablets – can i buy amoxicillin over the counter
http://amoxil.cheap/# where to buy amoxicillin 500mg without prescription
buy lisinopril 20 mg without a prescription lisinopril 20 mg buy zestril generic
norvasc over the counter purchase amlodipine online cheap amlodipine 5mg price
acyclovir 800mg sale buy zovirax generic allopurinol 100mg tablet
lasix side effects: Buy Lasix No Prescription – lasix online
http://furosemide.guru/# lasix dosage
glucophage bipolar
prednisone 3 tablets daily: buy prednisone from canada – how can i get prednisone
Карл Густав Юнг (1875–1961) – швейцарский психолог и
психиатр. Разработал методику ассоциативного эксперимента в психиатрической
клинике Бургхёльци: использовав психоаналитические идеи при
диагностировании ассоциаций и психологии раннего слабоумия, обнаружил наличие чувственных комплексов у человека.
В 1906 году начал переписку с Фрейдом,
спустя год нанес ему первый свой
визит; на протяжении ряда лет разделял его психоаналитические идеи.
Редактор журнала «Ежегодник психоаналитических и психопатологических исследований», президент Международной психоаналитической ассоциации с марта 1910-го по апрель 1914 года Фрейд видел в Юнге своего идейного наследника и возлагал на
него большие надежды как на продолжателя дальнейшего развития психоаналитического движения.
Однако в 1911 году между ними обнаружились расхождения
в понимании некоторых психоаналитических идей.
Последующие концептуальные и субъективные расхождения привели ктому, что в начале 1913 года между Юнгоми Фрейдом прекратилась
личная, а несколько месяцев спустя и деловая переписка.
В дальнейшем Юнг начал разработку своего
собственного учения о человеке и
его психических заболеваниях, совокупность идей и терапевтических приемов которого получила название аналитической психологии.
Юнг предложил типологию
характеров, основанную на представлениях об интровертированных и экстравертированных типах личности.
уровни грейвза
http://stromectol.fun/# stromectol 3mg tablets
Herkese selamlar!
Son yıllarda Bwin tr, п»їbwin çevrimiçi bahis endüstrisinde liderler arasında başarılı bir şekilde yerini sağlamlaştırdı. Uzmanlar kadar, kumar oynamaya yeni başlayanlar
da bu platformu spor bahisleri dünyasında güvenilir bir seçenek olarak tercih etmektedirler. Her ziyaretçi, platformun sunduğu heyecan dolu deneyimin tadını
çıkarabilir. Popüler spor etkinliklerinin yanı sıra, site golf, tenis veya beyzbol gibi daha az yaygın olan bahis disiplinlerini de sunmaktadır.
Geniş seçenekler ve yenilikçi yaklaşımıyla herkes için bir şeyler bulunmaktadır
Kumarhane oyunlarД± Г§eЕџitleri BWin
Slot makineleri BWin
Kumarhane yasal mД± BWin
Kumarhane stratejileri BWin
Kumar oyunlarД± BWin
Kumarhane deneme bonusu BWin
Kumar siteleri BWin
Kumarhane para yatД±rma BWin
Iyi sanlar!
where can i buy amoxicillin over the counter uk where to buy amoxicillin 500mg where can i get amoxicillin
Günaydın!
Son zamanlarda Bwin tr, https://bwintr.top çevrimiçi bahis endüstrisinde lider konumunu başarılı bir şekilde sağlamlaştırdı. Uzmanlar kadar, kumar oynamaya yeni başlayanlar
da bu platformu spor bahisleri dünyasında güvenilir bir tercih olarak seçiyorlar. Her ziyaretçi, platformun sunduğu heyecan dolu deneyimin tadını çıkarabilir.
Popüler spor etkinliklerinin yanı sıra, site golf, tenis veya beyzbol gibi daha az bilinen bahis disiplinlerine de yer vermektedir.
Geniş seçenekler ve yenilikçi yaklaşımı sayesinde herkesin ilgisini çekecek bir şey bulunmaktadır
Kumarhane para Г§ekme BWin
Kumar oyunlarД± BWin
Kumar siteleri BWin
Kumarhane oyunlarД± BWin
Kumarhane oyunları çevrimiçi BWin
Kumarhane oyunlarД± Г§eЕџitleri BWin
Kumarhane promosyonlarД± BWin
Kumarhane gГјvenilir mi BWin
Iyi sanlar!
pharmacy cost of prednisone: medicine prednisone 5mg – generic prednisone cost
http://furosemide.guru/# furosemide 40 mg
Астарт Вард отзывы форум magastartvard . ru Астарт Вард отзывы
______________________________________________________
magastartvard . ru отзыв о нем могу оставить только положительный
Заказала у мага Астарта Варда индивидуальный гороскоп и прогноз на будущее. Он дал мне ценные советы и предсказания, которые помогли мне лучше понять себя и свои жизненные пути. Очень довольна результатом и рекомендую его услуги!
______________________________________________________________
маг Астарт Вард отзывы
http://lisinopril.top/# lisinopril 20mg 25mg
furosemide 40mg: Buy Lasix No Prescription – furosemida
lisinopril tablet: order lisinopril 10 mg – buy lisinopril 2.5 mg online
https://amoxil.cheap/# cheap amoxicillin 500mg
buy lasix online Buy Lasix No Prescription furosemide 100mg
Крастко – Отзывы magpomosh ru – сайт – отзывы о привороте черное венчание
Магический сайт magpomosh . ru – отзывы обратившихся
Сотрудничество с магом Александрой оказалось очень плодотворным. Ее ритуалы на привлечение удачи и процветания помогли мне добиться успеха в карьере и достичь новых высот.
_________________________________________________________
Сайт ищут по тегам:
настоящий маг бесплатно проверенные маги колдуны ведьмы где настоящие маги в
самые настоящие маги проверенный сайт магов белый маг проверенный
настоящий мага как отличить шарлатана от настоящего мага в интернете как стать настоящим магом в жизни
только проверенные маги настоящие маги а не шарлатаны настоящий маг который помогает
http://lisinopril.top/# lisinopril for sale uk
rosuvastatin 20mg sale zetia drug order ezetimibe 10mg sale
amoxicillin 500mg capsules price: amoxicillin without prescription – order amoxicillin online
gabapentin sciatica
https://buyprednisone.store/# prednisone 20 mg purchase
yangsfitness.com
그래서 그는 “살인은 법에 위배됩니다!”라고 통곡했습니다.
zithromax 500 mg
lasix tablet: Buy Lasix No Prescription – lasix 40mg
lisinopril 10mg over the counter order zestril 2.5mg pill order generic lisinopril 5mg
lasix 100mg Buy Lasix No Prescription lasix 100 mg tablet
stromectol online canada: ivermectin – ivermectin brand name
http://amoxil.cheap/# amoxicillin 875 125 mg tab
buy rosuvastatin 10mg pills zetia 10mg for sale purchase ezetimibe
buy generic lisinopril 2.5mg where to buy lisinopril without a prescription purchase zestril
https://furosemide.guru/# lasix for sale
https://furosemide.guru/# buy furosemide online
amoxicillin 1000 mg capsule amoxicillin 500 mg brand name amoxicillin 875 mg tablet
https://lisinopril.top/# website
lasix: Buy Lasix No Prescription – lasix
amoxicillin 500mg side effects
domperidone 10mg generic motilium price order tetracycline 500mg
Привет Всем!
Sykaaa Casino, https://serpcity.ru запущенное в 2022 году, привносит в мир азартных развлечений свежий ветер. Владельцем казино является Snowdunes B.V., а лицензия, выданная в Кюрасао (8048/JAZ2022-007), обеспечивает безопасность и честность игры.
Для вывода средств из казино Sykaaa, игроку нужно авторизоваться и выбрать вкладку “Касса”. Минимальная сумма для вывода – 150 RUB или 20 USD. При выводе суммы более 200 USD требуется верификация аккаунта.
Казино предоставляет разнообразные варианты платежных систем, включая карты, электронные кошельки и криптовалюты.
Минимальный депозит в Sykaaa Casino – 5 USD, а максимальный – 60000 USD. Геймеры могут регулировать лимиты на депозит по мере продвижения по уровням программы
лояльности. Казино также предоставляет возможность бесплатной игры в демо-режиме для ознакомления с играми и правилами.
Sykaaa Casino радует игроков оригинальными бонусами. Новички могут получить 100 фриспинов на Razor Shark без депозита.
Приветственный бонус в размере 100% от первого депозита с условием вейджера х45. Казино также организует турниры и акцию “Игра дня”.
Для решения вопросов у игроков круглосуточно работает служба технической поддержки. Связаться можно через live chat, отправив письмо или позвонив по указанному номеру
телефона. Официальный сайт казино Sykaaa может быть периодически заблокирован провайдерами. В таких случаях игроки могут использовать зеркала или специальные программы для обхода блокировок. Регистрация открыта для игроков из Европы, России, Украины и Беларуси.
sykaaa казино онлайн
sykaaa казино вход
sykaaa casino ксыз
sukka казино
sukkaa казино
sykaaa casino сайт
sykaaa casino зеркало на сегодня
казино sukaa
Удачи и прибыли Друзья!
Здравствуйте!
Sykaaa Casino, запущенное в 2022 году, представляет собой молодой, но перспективный проект в мире азартных развлечений. Владельцем казино является Snowdunes B.V.,
а лицензия выдана в Кюрасао под номером 8048/JAZ2022-007. Это обеспечивает игрокам честную и безопасную игровую среду.
Sykaaa Casino стремится привлечь максимальное количество игроков, переведя интерфейс на русский, английский и украинский языки.
Даже на начальном этапе развития казино привлекает внимание сотен игроков онлайн, превышая отметку в 2000-3000 человек в пиковые часы.
Sykaaa Casino https://serpcity.ru радует игроков оригинальными бонусами. Например, новички могут получить 100 фриспинов на автомат Razor Shark без депозита.
Приветственный бонус в размере 100% от первого депозита также доступен.
Минимальный депозит для активации бонуса – 500 рублей, а максимальная сумма начисления – 5000 евро. Условия вейджера для вывода выигрышей составляют x45.
Sykaaa Casino предоставляет более 1000 игр от ведущих провайдеров, таких как Betsoft, Pragmatic Play, Microgaming и другие.
В коллекции более 1000 слотов, включая новинки и популярные игры. Опция игры бесплатно доступна зарегистрированным пользователям.
Демоверсии настольных игр доступны бесплатно, что позволяет игрокам освоить стратегии перед игрой на реальные деньги.
Минимальный депозит в Sykaaa Casino составляет 300 RUB, а минимальная сумма вывода – 1000 RUB. Оператор поддерживает различные методы оплаты, включая карты, электронные кошельки и криптовалюты. Выплаты обрабатываются в течение 0-24 часов.
sykaaa казино онлайн
сукааа казино вход
sukka казино
sukaaa казино зеркало рабочее
суаака казино
casino sykaaa скачать
sykaaa официальный сайт
сукааа казино официальный сайт
Удачи и прибыли Друзья!
order prilosec 20mg pill prilosec drug buy omeprazole generic
domperidone buy online purchase motilium generic tetracycline brand
pragmatic-ko.com
이것을 본 Ma Wensheng은 갑자기 “폐하, 아직 할 말이 있습니다. “라고 말했습니다.
omeprazole generic order omeprazole 10mg pills cost prilosec
http://indianph.xyz/# indian pharmacy
india pharmacy mail order
indianpharmacy com indian pharmacy paypal п»їlegitimate online pharmacies india
http://indianph.com/# buy medicines online in india
pharmacy website india
top online pharmacy india indian pharmacy top online pharmacy india
keflex cephalexin
https://indianph.com/# Online medicine order
buy prescription drugs from india
mail order pharmacy india cheapest online pharmacy india reputable indian online pharmacy
mail order pharmacy india online shopping pharmacy india top 10 online pharmacy in india
https://indianph.xyz/# india online pharmacy
online pharmacy india
http://indianph.com/# india online pharmacy
escitalopram and bupropion combination
rybelsus sale
https://indianph.com/# mail order pharmacy india
buy prescription drugs from india
dota2answers.com
그는 아들이 미쳐 가고 있다고 생각하고 감정에 휩싸여 한숨을 쉬었습니다. 그의 눈은 충혈되었습니다.
cyclobenzaprine pills order flexeril online buy baclofen 25mg without prescription
https://indianph.com/# Online medicine home delivery
online shopping pharmacy india
reputable indian online pharmacy best online pharmacy india indian pharmacy paypal
top 10 online pharmacy in india india online pharmacy india pharmacy
http://indianph.com/# reputable indian online pharmacy
buy medicines online in india
http://indianph.com/# india online pharmacy
buy medicines online in india
cyclobenzaprine over the counter buy lioresal paypal baclofen 25mg price
ciprofloxacin treats stds
order lopressor 100mg generic metoprolol 100mg us buy lopressor 50mg for sale
hihouse420.com
이런 식으로 보조 식품으로 사용할 수 있습니까?
rybelsus rx
The balance of business and relationship power may change at different career stages and in different situations.
The main thing is to be able to find the optimal balance.
The best site about relationship
http://nolvadex.guru/# tamoxifen headache
buy misoprostol over the counter cytotec online buy cytotec over the counter
http://diflucan.pro/# generic for diflucan
buy doxycycline cheap: order doxycycline 100mg without prescription – buy doxycycline
buy toradol pill cost colcrys colcrys 0.5mg generic
https://nolvadex.guru/# tamoxifen endometriosis
order cytotec online: purchase cytotec – buy cytotec in usa
bactrim dosing for uti uptodate
http://cytotec24.com/# buy cytotec
Misoprostol 200 mg buy online buy cytotec pills online cheap Misoprostol 200 mg buy online
lfchungary.com
Hongzhi 황제는 깊은 눈으로이 무성한 푸른 들판을 바라 보았습니다.
tamoxifen moa: benefits of tamoxifen – tamoxifen rash pictures
https://nolvadex.guru/# tamoxifen medication
order toradol generic ketorolac usa colcrys pills
tenormin 50mg pills buy tenormin generic buy atenolol pills for sale
cephalexin for staph infection
nolvadex side effects tamoxifen adverse effects nolvadex pct
https://cytotec24.com/# buy cytotec online fast delivery
https://nolvadex.guru/# tamoxifen generic
tamoxifen and weight loss: nolvadex gynecomastia – does tamoxifen cause weight loss
cheap atenolol atenolol where to buy atenolol 50mg pill
http://diflucan.pro/# cost of diflucan over the counter
cytotec online buy cytotec pills online cheap cytotec buy online usa
http://cytotec24.shop/# buy cytotec pills
http://nolvadex.guru/# tamoxifen for sale
doxy: cheap doxycycline online – doxycycline tetracycline
diflucan 200 mg capsules diflucan without a prescription diflucan 150 tab
http://nolvadex.guru/# femara vs tamoxifen
http://nolvadex.guru/# natural alternatives to tamoxifen
https://diflucan.pro/# diflucan drug
cytotec buy online usa buy cytotec over the counter buy cytotec over the counter
http://cipro.guru/# buy cipro online
pragmatic-ko.com
선발된 5000명의 농가는 당분간 머물고 나머지는 모두 짐을 싸서 해고한다.
https://doxycycline.auction/# doxycycline mono
http://cytotec24.shop/# buy misoprostol over the counter
ciprofloxacin generic price ciprofloxacin order online cipro online no prescription in the usa
https://diflucan.pro/# diflucan 50mg capsules
buy depo-medrol cheap methylprednisolone 16mg pills buy depo-medrol without prescription
https://doxycycline.auction/# 100mg doxycycline
buy medrol without prescription methylprednisolone 8mg tablet generic medrol
who should take tamoxifen tamoxifen for sale nolvadex steroids
http://doxycycline.auction/# price of doxycycline
https://lanarhoades.fun/# lana rhoades modeli
п»їcipro generic where can i buy cipro online ciprofloxacin over the counter
http://angelawhite.pro/# Angela White filmleri
lana rhoades modeli: lana rhoades – lana rhoades izle
hihouse420.com
당신이 그것을 피한다면 이것은 Hongzhi 황제의 스타일이 아닙니다.
http://abelladanger.online/# abella danger izle
eva elfie modeli: eva elfie izle – eva elfie video
https://abelladanger.online/# abella danger filmleri
lfchungary.com
Ouyang Zhi에 대해 말하면서 Wang Ao와 Xie Qian은 모두 웃었습니다.
https://sweetiefox.online/# sweety fox
buy generic inderal for sale brand plavix purchase plavix without prescription
http://sweetiefox.online/# Sweetie Fox izle
Angela White: abella danger filmleri – abella danger video
http://abelladanger.online/# abella danger izle
http://evaelfie.pro/# eva elfie izle
http://lanarhoades.fun/# lana rhoades video
propranolol uk buy generic plavix for sale oral plavix 150mg
Angela White video: abella danger izle – abella danger video
https://evaelfie.pro/# eva elfie modeli
assignment website buy an essay cheap buy an essay cheap
https://abelladanger.online/# abella danger filmleri
http://sweetiefox.online/# Sweetie Fox izle
eva elfie: eva elfie – eva elfie
http://sweetiefox.online/# sweeti fox
http://evaelfie.pro/# eva elfie
essay helpers pay for essay writing uk cheap essay writing
Angela White izle: ?????? ???? – ?????? ????
https://angelawhite.pro/# Angela Beyaz modeli
https://lanarhoades.fun/# lana rhoades modeli
side effects of amoxicillin in adults
Ad opus! — За дело!
https://abelladanger.online/# Abella Danger
https://lanarhoades.fun/# lana rhoades video
buy generic methotrexate over the counter warfarin 5mg uk buy medex for sale
Sweetie Fox modeli: swetie fox – Sweetie Fox modeli
https://evaelfie.pro/# eva elfie izle
https://sweetiefox.online/# swetie fox
Ad fontes — К первоисточникам.
http://abelladanger.online/# abella danger video
eva elfie video: eva elfie video – eva elfie filmleri
http://angelawhite.pro/# ?????? ????
buy methotrexate medication methotrexate 5mg us buy coumadin medication
https://evaelfie.pro/# eva elfie izle
Angela Beyaz modeli: abella danger video – abella danger filmleri
Per aspera ad astra – через тернии к звездам
https://angelawhite.pro/# Angela White izle
rybelsus australia
http://evaelfie.pro/# eva elfie filmleri
http://evaelfie.pro/# eva elfie modeli
eva elfie izle: eva elfie izle – eva elfie modeli
http://sweetiefox.online/# Sweetie Fox modeli
https://angelawhite.pro/# Angela White filmleri
http://abelladanger.online/# abella danger video
buy metoclopramide 10mg generic buy maxolon pills for sale brand losartan
meloxicam where to buy order celecoxib 100mg sale purchase celebrex pill
https://lanarhoades.fun/# lana rhoades izle
Sweetie Fox izle: Sweetie Fox modeli – Sweetie Fox modeli
is cephalexin an antibiotic
https://abelladanger.online/# Abella Danger
mega-slot1.com
가는 내내 숨이 찼지만 여전히 마음에는 믿기지 않는다는 표정이 남아 있었다.
https://evaelfie.pro/# eva elfie modeli
meloxicam for sale order generic celecoxib 100mg celebrex order online
http://sweetiefox.online/# Sweetie Fox video
order maxolon sale metoclopramide pills losartan 25mg tablet
lana rhoades filmleri: lana rhoades izle – lana rhoades filmleri
khasiss.com
아내들은 하나씩 속삭이는 동안 놀란 눈으로 류톈정을 바라보았다.
http://sweetiefox.online/# Sweetie Fox video
https://sweetiefox.online/# Sweetie Fox izle
eva elfie filmleri: eva elfie filmleri – eva elfie filmleri
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara444.wordpress.com
Good luck!
lana rhoades: lana rhoades hot – lana rhoades pics
ph sweetie fox: sweetie fox video – ph sweetie fox
https://evaelfie.site/# eva elfie new video
online singles dating sites: https://miamalkova.life/# mia malkova full video
http://lanarhoades.pro/# lana rhoades full video
lana rhoades unleashed: lana rhoades pics – lana rhoades hot
It is very comforting to see that others are suffering from the same problem as you, wow!
canadian pharmacy cialis
http://evaelfie.site/# eva elfie videos
buy tamsulosin 0.2mg generic purchase celebrex generic celebrex 200mg pill
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara235.wordpress.com
Good luck!
lana rhoades full video: lana rhoades unleashed – lana rhoades unleashed
sweetie fox full: fox sweetie – fox sweetie
no credit card dating sites: http://sweetiefox.pro/# sweetie fox video
tamsulosin over the counter flomax ca order celecoxib 100mg pill
http://sweetiefox.pro/# sweetie fox full video
mia malkova new video: mia malkova videos – mia malkova only fans
escitalopram oxalate 10 mg oral tablet
http://sweetiefox.pro/# fox sweetie
lana rhoades solo: lana rhoades full video – lana rhoades videos
sweetie fox cosplay: sweetie fox full video – sweetie fox
a free dating site: http://miamalkova.life/# mia malkova latest
jbustinphoto.com
Zhang Zhaotian은 그가 미쳐가는 것을 느꼈고 그의 뒤에서 속삭이는 소리를 들었습니다.
lana rhoades full video: lana rhoades full video – lana rhoades videos
http://evaelfie.site/# eva elfie hot
smcasino7.com
Fang Jifan은 제자들과 계속 이야기 할 기분이 아니었고 여유롭게 떠났습니다.
tadalafil generic best price
eva elfie videos: eva elfie hot – eva elfie videos
buy esomeprazole online cheap buy topiramate 200mg generic order generic topamax
ph sweetie fox: sweetie fox video – fox sweetie
mojmelimajmuea.com
장 여왕의 눈가에서 그녀는 Zhu Xiurong을 흘끗 보았습니다.
http://lanarhoades.pro/# lana rhoades
free online adult dating site: http://lanarhoades.pro/# lana rhoades videos
nexium 20mg usa buy topiramate 200mg pill topamax 100mg usa
eva elfie full video: eva elfie hd – eva elfie new videos
http://lanarhoades.pro/# lana rhoades videos
where can you buy tadalafil
sweetie fox: sweetie fox new – sweetie fox full
azithromycin medicine over the counter
sex dating site: http://lanarhoades.pro/# lana rhoades boyfriend
eva elfie videos: eva elfie new video – eva elfie hot
http://lanarhoades.pro/# lana rhoades videos
sumatriptan tablet where can i buy levaquin oral levaquin 250mg
buy ondansetron 4mg without prescription zofran generic order aldactone 25mg sale
ph sweetie fox: sweetie fox cosplay – sweetie fox full
khasiss.com
그런데 사실 가끔은 본문을 보는 것이 불가피할 때가 있습니다.
zofran online where to buy ondansetron without a prescription how to buy aldactone
Здравствуйте!
Было ли у вас когда-нибудь такое, что приходилось писать дипломную работу в сжатые сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не сдаваться и продолжать активно заниматься учебными процессами, чем я и занимаюсь.
Для тех, кто умеет искать и анализировать информацию в интернете, это действительно помогает в процессе согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь представлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по России. Можете ознакомиться с предложениями по ссылке https://2orik-diploms.com, проверено!
купить диплом магистра
купить диплом о среднем образовании
купить диплом Вуза
купить диплом колледжа
купить аттестат школы
Желаю всем отличных оценок!
Привет всем!
Были ли у вас случаи, когда приходилось писать дипломную работу в крайне ограниченные сроки? Это действительно требует большой ответственности и трудоемкости, но важно не отступать и продолжать активно участвовать в учебном процессе, как я.
Для тех, кто умеет эффективно находить и использовать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями тут https://server-diploms.com, это проверенный источник!
купить диплом магистра
купить диплом в Москве
купить диплом о среднем специальном
купить аттестат
Желаю всем отличных оценок!
Доброго!
Бывали ли у вас случаи, когда приходилось писать дипломную работу в крайне сжатые сроки? Это действительно требует большой ответственности и напряженного труда, но важно не унывать и продолжать активно участвовать в учебном процессе, как я и делаю.
Для тех, кто умеет эффективно находить и использовать информацию в интернете, это может существенно облегчить процесс согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на https://3russkiy-diploms.com, это проверено!
купить диплом о среднем образовании
купить диплом Гознак
купить диплом нового образца
купить диплом цена
купить диплом ссср
Желаю всем отличных оценок!
https://miamalkova.life/# mia malkova
imitrex 25mg us buy levofloxacin 250mg pills buy levaquin 250mg
Доброго!
Бывало ли у вас такое, что приходилось писать дипломную работу в крайне ограниченные сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не опускать руки и продолжать активно заниматься учебными процессами, чем я и занимаюсь.
Для тех, кто умеет искать и анализировать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Не нужно тратить время на посещение библиотек или устраивать встречи с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по России. Можете ознакомиться с предложениями по ссылке купить диплом Вуза, это проверено!
купить диплом ссср
купить диплом цена
купить диплом техникума
купить диплом о высшем образовании
купить диплом колледжа
купить диплом университета
купить диплом
купить диплом нового образца
купить аттестат
купить диплом специалиста
Желаю всем отличных оценок!
lana rhoades: lana rhoades – lana rhoades unleashed
plenty of fish: https://miamalkova.life/# mia malkova full video
Привет всем!
Вы когда-нибудь писали диплом в сжатые сроки? Это очень ответственно и тяжело, но нужно не сдаваться и делать учебные процессы, чем Я и занимаюсь)
Тем кто умеет разбираться и гуглить информацию, это действительно помогает по ходу согласований и написания диплома, не нужно тратить время на библиотеки или встречи с дипломным руководителем, вот здесь есть хорошие данные для заказа и написания дипломов и курсовых с гарантией и доставкой по России, можете посмотреть здесь https://1russa-diploms.com, проверено!
купить аттестат
купить диплом цена
купить диплом института
купить диплом колледжа
купить диплом в Москве
Желаю всем отличных оценок!
fox sweetie: sweetie fox video – sweetie fox video
eva elfie full video: eva elfie new video – eva elfie hot
http://sweetiefox.pro/# sweetie fox full
Привет всем!
Были ли у вас случаи, когда вам приходилось писать дипломную работу в сжатые сроки? Это действительно требует большой ответственности и усилий, но важно не сдаваться и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет эффективно искать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на купить диплом о высшем образовании, это проверенный источник!
купить диплом университета
где купить диплом
купить аттестат
купить диплом о среднем образовании
купить диплом о высшем образовании
купить диплом магистра
купить диплом ссср
купить диплом Гознак
купить диплом техникума
купить диплом колледжа
Желаю всем отличных оценок!
Доброго!
Бывало ли у вас такое, что приходилось писать дипломную работу в крайне сжатые сроки? Это действительно требует огромной ответственности и напряженных усилий, но важно не опускать руки и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет быстро находить и анализировать информацию в сети, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или устраивать встречи с дипломным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на сайте https://2orik-diploms.com, это проверено!
купить диплом Гознак
купить диплом магистра
купить диплом в Москве
где купить диплом
купить диплом Вуза
Желаю всем отличных оценок!
Доброго!
Было ли у вас опыт написания дипломной работы в крайне сжатые сроки? Это действительно требует огромной ответственности и трудоемкости, однако важно сохранять упорство и продолжать активно участвовать в учебном процессе, как я это делаю.
Для тех, кто умеет эффективно искать и анализировать информацию в интернете, это действительно помогает в процессе согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или организацию встреч с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями по ссылке https://server-diploms.com, это проверенный источник!
купить диплом о среднем специальном
где купить диплом
купить диплом
купить диплом ссср
Желаю всем отличных оценок!
Привет всем!
Было ли у вас когда-нибудь так, что приходилось писать дипломную работу в очень сжатые сроки? Это действительно требует огромной ответственности и может быть очень тяжело, но важно не опускать руки и продолжать активно заниматься учебными процессами, как я.
Для тех, кто умеет быстро находить и использовать информацию в интернете, это действительно облегчает процесс согласования и написания дипломной работы. Больше не нужно тратить время на посещение библиотек или устраивать встречи с научным руководителем. Здесь, на этом ресурсе, предоставлены надежные данные для заказа и написания дипломных и курсовых работ с гарантией качества и доставкой по всей России. Можете ознакомиться с предложениями на сайте https://1russa-diploms.com, это проверено!
купить диплом ссср
купить диплом
купить диплом магистра
купить диплом в Москве
купить диплом о среднем специальном
Желаю всем отличных оценок!
mia malkova full video: mia malkova latest – mia malkova movie
https://miamalkova.life/# mia malkova new video
Здравствуйте!
Купоны для интернет-магазина М.Видео – это уникальные коды, которые можно использовать при оформлении заказа на официальном веб-сайте компании.
Они предоставляют дополнительные преимущества клиентам в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как найти такие промокоды и купоны для М.Видео? Обычно они предоставляются в рамках специальных акций компании, которые могут быть организованы
на ее официальном веб-сайте, в социальных сетях или на специализированных ресурсах, например, на сайте promokodbar.ru,
который предлагает самые свежие и проверенные промокоды
Сайт самых свежих и проверенных купонов магазина М.Видео https://promokodbar.ru
Удачных покупок!
купоны для получения дополнительных бонусов в М.Видео
бесплатные промокоды М.Видео
новые промокоды М.Видео
Промокоды для умных покупок в М.Видео
выгодные промокоды М.Видео
Удачи!
citalopram dosage 10 mg
chutneyb.com
그는 위엄 있는 표정으로 갑자기 카피를 찰싹 때리며 진지하게 말했다. “이게 정말 사실인가요?”
avodart 0.5mg canada buy ranitidine paypal zantac without prescription
buy generic zocor 10mg order valacyclovir 1000mg buy valacyclovir pills
dating chat free: http://miamalkova.life/# mia malkova new video
Привет всем!
Вы когда-нибудь писали диплом в сжатые сроки? Это очень ответственно и тяжело, но нужно не сдаваться и делать учебные процессы, чем Я и занимаюсь)
Тем кто умеет разбираться и гуглить информацию, это действительно помогает по ходу согласований и написания диплома, не нужно тратить время на библиотеки или встречи с дипломным руководителем, вот здесь есть хорошие данные для заказа и написания дипломов и курсовых с гарантией и доставкой по России, можете посмотреть здесь https://3russkiy-diploms.com, проверено!
купить диплом цена
купить диплом о высшем образовании
купить диплом нового образца
купить диплом университета
где купить диплом
Желаю всем отличных оценок!
cheap simvastatin 10mg order valacyclovir 1000mg online order valacyclovir 500mg sale
aviator: aviator bet – aviator mocambique
aviator game: aviator sportybet ghana – play aviator
http://aviatoroyunu.pro/# aviator oyna
order dutasteride for sale buy dutasteride pills zantac order online
cozaar for high blood pressure
http://aviatormocambique.site/# aviator mocambique
Здравствуйте!
Промокоды и купоны для интернет-магазина М.Видео представляют собой уникальные коды, которые можно использовать при оформлении заказа на официальном сайте компании.
Они приносят дополнительные преимущества покупателям в виде скидок на определенные товары или услуги, бесплатной доставки и других бонусов.
Как их найти? Промокоды часто предоставляются в рамках специальных акций компании, которые могут проводиться на ее официальном сайте,
в социальных сетях или на проекте promokodbar.ru
Сайт самых свежих и проверенных купонов магазина М.Видео https://promokodbar.ru
Удачных покупок!
Экономь с промокодами М.Видео
рабочий промокод М.Видео
Официальные акции М.Видео
новый промокод М.Видео
Бонусные предложения и скидки в М.Видео
Удачи!
aviator bet: como jogar aviator – aviator
bistroduet.com
한 무리의 의사들이 Su Yue를 따라갔고 연속적으로 많은 환자들을 보았습니다.
finpecia brand finasteride 1mg uk oral fluconazole
http://pinupcassino.pro/# pin up aviator
https://aviatoroyunu.pro/# aviator oyna
ddavp dose for children
jogar aviator online: jogar aviator online – pin up aviator
aviator login: aviator betting game – aviator
0.025 mg synthroid
aviator betano: aviator pin up – aviator jogar
depakote indications
https://aviatormalawi.online/# aviator bet malawi
Hello, World!
Hey there, mate! Greetings from your favorite surfing capybara!
How’s the surf today?
Ready to catch some gnarly waves together?
https://capybara999.wordpress.com/
Good luck!
where can i buy ampicillin buy ampicillin no prescription cheap amoxicillin online
aviator bet: jogar aviator online – aviator jogar
http://pinupcassino.pro/# pin up aviator
aviator betano: aviator pin up – aviator bet
pin-up casino entrar: pin-up casino – pin-up cassino
https://aviatorjogar.online/# jogar aviator Brasil
buy generic ampicillin online buy acillin generic amoxil uk
http://aviatormocambique.site/# aviator online
aviator game: aviator game – aviator bet
buy propecia 1mg for sale fluconazole 200mg pill purchase forcan generic
pin-up casino entrar: pin-up casino entrar – aviator pin up casino
aviator game: aviator bet malawi – aviator game
aviator bahis: aviator bahis – pin up aviator
sm-casino1.com
모든 한린은 여전히 제자리에 묵묵히 머물렀지만 그들의 마음은 극도로 복잡했다.
aviator oyunu: aviator hilesi – pin up aviator
aviator pin up casino: cassino pin up – aviator pin up casino
aviator bet: aviator – aviator betting game
where to buy baycip without a prescription – buy cheap generic trimethoprim buy clavulanate online
http://aviatormocambique.site/# jogar aviator
aviator game online: aviator login – aviator bet
pactam2.com
Hongzhi 황제를 놀라게 한 것은 이러한 것들이 쓰여진 방법이었습니다.
zithromax online paypal – п»їhttps://azithromycin.pro zithromax capsules
cheap cipro 500mg – myambutol for sale order generic amoxiclav
cipro cost – order myambutol 600mg for sale augmentin buy online
aviator bet: aviator jogar – estrela bet aviator
http://pinupcassino.pro/# pin up bet
zithromax buy – https://azithromycin.pro/how-much-does-zithromax-cost.html buy zithromax 500mg online
aviator mocambique: aviator bet – aviator mz
aviator sinyal hilesi: aviator hilesi – aviator bahis
online pharmacy india
buy zithromax without presc – https://azithromycin.pro/zithromax-indications.html zithromax 500 without prescription
estrela bet aviator: aviator pin up – pin up aviator
http://jogodeaposta.fun/# jogos que dao dinheiro
What a compelling enjoy reading! Your arguments were well-presented and convincing.
This was a thoroughly insightful enjoy reading. Thank you for sharing your expertise!
https://indianpharm24.shop/# best online pharmacy india indianpharm.store
parrotsav.com
Fang Jifan은 오늘 Xiao Jing의 경고를 기억했습니다.
mexican mail order pharmacies: order online from a Mexican pharmacy – п»їbest mexican online pharmacies mexicanpharm.shop
buy ciprofloxacin 500mg for sale – buy cephalexin 500mg pills buy augmentin 1000mg pill
buy prescription drugs from india: Top online pharmacy in India – Online medicine order indianpharm.store
You have a gift for explaining things in an understandable way. Thank you!
Your thoughtful analysis has really made me think. Thanks for the great enjoy reading!
cozaar free trial
citalopram qt prolongation
п»їlegitimate online pharmacies india Generic Medicine India to USA india pharmacy indianpharm.store
canadian pharmacy phone number: CIPA approved pharmacies – canadianpharmacyworld com canadianpharm.store
https://canadianpharmlk.com/# canadian pharmacy ratings canadianpharm.store
Your blog is a constant source of inspiration and knowledge. Thank you!
This article was a joy to enjoy reading. Your enthusiasm is contagious!
purple pharmacy mexico price list: Mexico pharmacy price list – medicine in mexico pharmacies mexicanpharm.shop
https://canadianpharmlk.com/# canada pharmacy online canadianpharm.store
certified canadian international pharmacy: CIPA approved pharmacies – recommended canadian pharmacies canadianpharm.store
https://mexicanpharm24.shop/# mexican online pharmacies prescription drugs mexicanpharm.shop
Online medicine order cheapest online pharmacy indian pharmacy indianpharm.store
http://indianpharm24.com/# reputable indian pharmacies indianpharm.store
https://canadianpharmlk.shop/# canadian family pharmacy canadianpharm.store
http://canadianpharmlk.com/# cross border pharmacy canada canadianpharm.store
depakote toxicity symptoms
buy medicines online in india: indian pharmacy – top 10 pharmacies in india indianpharm.store
You’ve presented a complex topic in a clear and engaging way. Bravo!
This blog is a treasure trove of knowledge. Thank you for your contributions!
https://mexicanpharm24.com/# mexican pharmacy mexicanpharm.shop
https://indianpharm24.shop/# Online medicine order indianpharm.store
http://indianpharm24.com/# cheapest online pharmacy india indianpharm.store
purchase flagyl generic – buy cleocin 150mg generic purchase azithromycin without prescription
http://indianpharm24.com/# online shopping pharmacy india indianpharm.store
best online pharmacy india: Top online pharmacy in India – reputable indian online pharmacy indianpharm.store
п»їbest mexican online pharmacies: mexican pharmacy – pharmacies in mexico that ship to usa mexicanpharm.shop
п»їbest mexican online pharmacies Medicines Mexico purple pharmacy mexico price list mexicanpharm.shop
Святослав Серебряков отзывы маг
Отзыв о ритуале на привлечение удачи от Мага Святослава Серебрякова: Путь к Успеху Открылся!
Я хочу поделиться своим восторженным опытом работы с Магом Святославом Серебряковым в заказе ритуала на привлечение удачи. Уже долгое время я ощущал некоторое отсутствие удачи в различных сферах своей жизни и искал способы изменить это положение.
Сотрудничество с Магом Святославом принесло мне невероятные результаты. Его профессионализм, энергия и внимание к деталям сразу же вызвали у меня доверие. Он сделал процесс ритуала легким и понятным для меня, объясняя каждый шаг и настраивая на позитивный результат.
После завершения ритуала я почувствовал себя полным энергии и уверенности. Удача начала приходить ко мне в различных сферах моей жизни, будь то в работе, личных отношениях или саморазвитии. Я заметил, что мои усилия стали приносить более значимые и быстрые результаты.
Маг Святослав Серебряков – это настоящий профессионал, и его ритуалы действительно работают. Я благодарен ему за помощь в открытии пути к удаче и успеху в моей жизни. Если вы ищете способ изменить свою удачу к лучшему, я настоятельно рекомендую обратиться к Магу Святославу Серебрякову.
Спасибо вам, Маг Святослав, за вашу мудрость, поддержку и помощь в привлечении удачи в мою жизнь.
-приворот мужа на месячные
-как узнать есть ли на муже приворот любовницы
-снять приворот рунами
-как снять приворот с бывшего мужа
-есть ли приворот
https://gadgetsto.ru/изготовление-прессформ-для-литья-пла/
http://indianpharm24.com/# legitimate online pharmacies india indianpharm.store
http://canadianpharmlk.shop/# buy prescription drugs from canada cheap canadianpharm.store
https://canadianpharmlk.com/# pharmacy in canada canadianpharm.store
online canadian pharmacy reviews: CIPA approved pharmacies – online canadian pharmacy reviews canadianpharm.store
smcasino-game.com
그런 큰 배는 깊은 바다를 향해 항해하는 것이 아니므로 생각해보면 가라앉지 않을 것입니다.
https://indianpharm24.shop/# buy prescription drugs from india indianpharm.store
https://indianpharm24.com/# п»їlegitimate online pharmacies india indianpharm.store
buy ciplox 500 mg for sale – purchase tindamax online cheap buy erythromycin pills
http://indianpharm24.com/# reputable indian online pharmacy indianpharm.store
buy ciplox without a prescription – order chloromycetin pill buy erythromycin 250mg online
top online pharmacy india: top 10 pharmacies in india – Online medicine order indianpharm.store
http://indianpharm24.shop/# indian pharmacy indianpharm.store
https://keramobum.ru/proektirovanie-press-form-dlya-litya-plastmass-pod-davleniem-spb.html
http://mexicanpharm24.com/# medicine in mexico pharmacies mexicanpharm.shop
https://canadianpharmlk.shop/# canada cloud pharmacy canadianpharm.store
best rated canadian pharmacy: My Canadian pharmacy – the canadian pharmacy canadianpharm.store
legitimate canadian pharmacy canadian pharmacy legit canadian online pharmacy canadianpharm.store
https://canadianpharmlk.com/# canadian pharmacy in canada canadianpharm.store
http://canadianpharmlk.shop/# safe online pharmacies in canada canadianpharm.store
synthroid online no prescription
https://canadianpharmlk.shop/# reputable canadian online pharmacy canadianpharm.store
http://mexicanpharm24.com/# mexican pharmacy mexicanpharm.shop
pactam2.com
이에 대해 주담지의 얼굴은 유난히 엄숙해졌다.
flagyl 400mg drug – amoxicillin order cost azithromycin 500mg
where buy generic clomid for sale: how can i get cheap clomid without prescription – how can i get generic clomid without dr prescription
how to buy clomid without rx: can i order generic clomid price – can i get cheap clomid pills
buy prednisone online without a script: solumedrol to prednisone – over the counter prednisone medicine
https://prednisonest.pro/# prednisone 40mg
clomid cost can i get cheap clomid tablets how can i get clomid
how can i get cheap clomid no prescription: clomid dosage for men – cheap clomid without dr prescription
clomid tablet: how to get clomid no prescription – order cheap clomid without dr prescription
buy clomid pills: clomid vs clomiphene – cost of generic clomid without dr prescription
https://prednisonest.pro/# prednisone 10 tablet
amoxicillin online no prescription: amoxicillin for pneumonia – amoxicillin buy canada
buy prednisone with paypal canada: how much is prednisone 5mg – prednisone 12 mg
valacyclovir over the counter – order starlix 120 mg pills order acyclovir 400mg pill
https://amoxilst.pro/# amoxil generic
where can i get amoxicillin 500 mg: can you buy amoxicillin over the counter – amoxicillin from canada
where can i buy amoxocillin: amoxicillin 750 mg price – order amoxicillin no prescription
cost of amoxicillin: amoxicillin 500mg capsule cost – amoxil pharmacy
where to buy amoxicillin pharmacy amoxicillin 500 mg for sale amoxicillin 500 mg online
how can i get clomid tablets: get clomid online – how to get cheap clomid online
https://amoxilst.pro/# amoxicillin generic brand
buy generic prednisone online: alcohol and prednisone – prednisone pill
can i get cheap clomid no prescription: clomid no prescription – where to buy generic clomid for sale
ivermectin 12mg for sale – buy sumycin without prescription buy cheap sumycin
drug prices prednisone: prednisone without a prescription – prednisone for sale no prescription
canadian pharmacy metformin
ivermectin 12mg tablet – purchase amoxiclav online sumycin for sale
http://prednisonest.pro/# prednisone 15 mg daily
prednisone 40 mg rx: prednisone for strep throat – where can i buy prednisone without a prescription
can you get clomid without insurance: how to get generic clomid without insurance – where to get cheap clomid price
twichclip.com
말을 마친 그는 절을 하고 목을 쭉 뻗은 채 학살당하는 것처럼 몸을 땅에 내동댕이쳤다.
anal fissure diltiazem
generic amoxicillin over the counter: amoxicillin pot clavulanate – buy cheap amoxicillin online
https://amoxilst.pro/# amoxicillin 500 mg tablet price
buy prednisone 50 mg order prednisone with mastercard debit prednisone 20 mg tablet
prednisone 1 mg tablet: prednisone long term side effects – prednisone medicine
sm-slot.com
그는이 스승을 매우 존경했고 Fang Jifan이 훌륭한 배움의 사람이라고 느꼈습니다.
amoxicillin 500mg cost: amoxicillin without prescription – amoxicillin 200 mg tablet
online order prednisone: where to buy prednisone in australia – prednisone 20mg buy online
where to buy amoxicillin 500mg: amoxil cost – buy amoxicillin online without prescription
https://amoxilst.pro/# can i purchase amoxicillin online
http://pharmnoprescription.pro/# canadian pharmacy online no prescription needed
purchase valacyclovir for sale – buy diltiazem 180mg pill buy acyclovir online cheap
legitimate online pharmacy no prescription: canada pharmacy without prescription – canadian pharmacy without a prescription
canadian pharmacy coupon code canadian pharmacy online prescription free canadian pharmacy
buying drugs online no prescription: online pharmacy without prescriptions – prescription drugs canada
http://edpills.guru/# cheapest online ed treatment
reputable online pharmacy no prescription: canada online pharmacy – buying prescription drugs from canada
cheapest pharmacy to get prescriptions filled: online pharmacy delivery – canadian pharmacies not requiring prescription
http://edpills.guru/# cheap ed medicine
ed online prescription: order ed pills – edmeds
http://onlinepharmacy.cheap/# us pharmacy no prescription
pharmacy with no prescription: online meds no prescription – canadian prescription prices
online medication without prescription: non prescription pharmacy – buy prescription drugs without a prescription
canada pharmacy not requiring prescription canadian pharmacy online canada pharmacy not requiring prescription
online meds without prescription: online pharmacy without a prescription – buy prescription drugs on line
http://edpills.guru/# ed meds online
buy flagyl 200mg generic – flagyl over the counter purchase zithromax online cheap
http://onlinepharmacy.cheap/# online pharmacy no prescription
buying prescription drugs online without a prescription: how to order prescription drugs from canada – canada drugs no prescription
discount ed meds: online erectile dysfunction pills – ed online treatment
http://onlinepharmacy.cheap/# rx pharmacy no prescription
non prescription canadian pharmacy: cheap drugs no prescription – non prescription canadian pharmacy
ampicillin antibiotic online order doxycycline sale purchase amoxicillin
buy acillin generic generic acticlate amoxicillin usa
pharmacies without prescriptions: buy prescription drugs on line – best no prescription online pharmacies
what is the cheapest ed medication: ed medications online – erectile dysfunction pills for sale
https://edpills.guru/# erectile dysfunction medications online
https://pharmnoprescription.pro/# medication online without prescription
canada pharmacy online no prescription: online pharmacies no prescription usa – best online pharmacies without prescription
best non prescription online pharmacy: online drugstore no prescription – best no prescription online pharmacy
non prescription pharmacy order prescription drugs online without doctor buying prescription drugs in canada
buy pain meds online without prescription: buying prescription drugs online canada – canadian mail order prescriptions
http://pharmnoprescription.pro/# how to buy prescriptions from canada safely
how to buy metronidazole – order cleocin sale buy zithromax generic
canadian pharmacy 1 internet online drugstore: canadian pharmacy store – canadian pharmacy ltd
https://canadianpharm.guru/# canadian pharmacy antibiotics
tadalafil buy india
best india pharmacy: indian pharmacy – reputable indian online pharmacy
cheap canadian pharmacy
pharmacies in mexico that ship to usa п»їbest mexican online pharmacies mexican mail order pharmacies
http://indianpharm.shop/# cheapest online pharmacy india
long-term effects of amitriptyline
allopurinol warnings
mexican mail order pharmacies: п»їbest mexican online pharmacies – mexican border pharmacies shipping to usa
buy lasix 40mg pill – order minipress 1mg online captopril uk
canadian pharmacy 24h com safe: canada drugs online reviews – best canadian online pharmacy reviews
http://pharmacynoprescription.pro/# pharmacy no prescription
qiyezp.com
전쟁 부의 봉래 수상 마을은 전투력이 없어서 안타깝습니다.
http://pharmacynoprescription.pro/# no prescription needed pharmacy
mexican drugstore online: best online pharmacies in mexico – mexican mail order pharmacies
Your post was a beacon of knowledge. Thank you for illuminating this subject.
india pharmacy india pharmacy mail order cheapest online pharmacy india
tadalafil online sale
http://canadianpharm.guru/# canadian pharmacies
buy medications without a prescription: online pharmacy without prescription – online meds no prescription
online canadian drugstore: pharmacy in canada – legitimate canadian online pharmacies
cheapest online pharmacy india: top 10 online pharmacy in india – online pharmacy india
mail order pharmacy india: reputable indian pharmacies – best india pharmacy
https://mexicanpharm.online/# purple pharmacy mexico price list
medicine in mexico pharmacies: pharmacies in mexico that ship to usa – buying from online mexican pharmacy
https://canadianpharm.guru/# cross border pharmacy canada
what aer the benefits of taking aripiprazole with prozac
cheap prescription drugs online: online medication no prescription – best non prescription online pharmacy
how much aspirin to give a dog
buying prescription drugs online without a prescription: order medication without prescription – online drugstore no prescription
legitimate online pharmacies india: indianpharmacy com – buy medicines online in india
http://pharmacynoprescription.pro/# online pharmacy without prescriptions
purple pharmacy mexico price list pharmacies in mexico that ship to usa mexico pharmacies prescription drugs
online canadian pharmacy reviews: canadian online drugstore – canadian pharmacy ed medications
reputable mexican pharmacies online: best online pharmacies in mexico – buying from online mexican pharmacy
https://canadianpharm.guru/# canadian pharmacy 365
buy meds online without prescription: best no prescription online pharmacy – buy medication online without prescription
lasix 40mg pills – minipress 1mg over the counter how to buy capoten
legitimate canadian pharmacies: safe canadian pharmacy – canada drugs online reviews
pharmacy in canada: canadapharmacyonline – canada online pharmacy
http://pharmacynoprescription.pro/# how to get a prescription in canada
https://indianpharm.shop/# world pharmacy india
reputable canadian pharmacy: cheapest pharmacy canada – canada pharmacy online legit
no prescription pharmacy online: pharmacies without prescriptions – buy drugs without prescription
https://canadianpharm.guru/# canadian medications
meds online without prescription: buy medications online no prescription – buy pills without prescription
cheapest online pharmacy india: pharmacy website india – buy prescription drugs from india
pharmacy canadian superstore canadian drug adderall canadian pharmacy
п»їlegitimate online pharmacies india: indian pharmacy – online shopping pharmacy india
cheap canadian pharmacy online: onlinecanadianpharmacy – onlinecanadianpharmacy 24
http://indianpharm.shop/# buy prescription drugs from india
reputable indian online pharmacy: india online pharmacy – buy medicines online in india
pharmacy wholesalers canada: canadian pharmacy 24h com – the canadian pharmacy
http://indianpharm.shop/# indian pharmacy
canadian pharmacy ratings: recommended canadian pharmacies – best rated canadian pharmacy
pharmacies in mexico that ship to usa: mexico pharmacy – buying prescription drugs in mexico
http://canadianpharm.guru/# canadian pharmacy prices
glucophage pills – buy generic cipro buy lincocin 500 mg without prescription
buy metformin for sale – glucophage usa lincomycin 500 mg price
buying prescription drugs in mexico: mexico drug stores pharmacies – mexican pharmacy
india pharmacy mail order: mail order pharmacy india – reputable indian pharmacies
where can i get synthroid
cheapest pharmacy canada best canadian online pharmacy reviews reliable canadian pharmacy
http://mexicanpharm.online/# п»їbest mexican online pharmacies
canadian pharmacy: adderall canadian pharmacy – canadian pharmacy world reviews
best online prescription: overseas online pharmacy-no prescription – canada pharmacies online prescriptions
bupropion pregnancy
indian pharmacy: indian pharmacy online – cheapest online pharmacy india
celebrex dosage for back pain
drugs from canada: canada drugs online – canada pharmacy
http://pharmacynoprescription.pro/# mexican pharmacies no prescription
zidovudine online buy – buy glucophage without prescription zyloprim 100mg drug
http://canadianpharm.guru/# best online canadian pharmacy
top 10 online pharmacy in india: best india pharmacy – top 10 pharmacies in india
http://pharmacynoprescription.pro/# online pharmacy not requiring prescription
canada rx pharmacy: canadian pharmacy tampa – best mail order pharmacy canada
indian pharmacy online: india online pharmacy – top 10 online pharmacy in india
medication canadian pharmacy: canadian pharmacy 24 – canadianpharmacymeds com
my canadian pharmacy rx canada pharmacy canadian pharmacy world reviews
canadian drugs: best canadian pharmacy – drugs from canada
https://mexicanpharm.online/# purple pharmacy mexico price list
Уникальные фото различных тематик https://pro-dachnikov.com
best mexican online pharmacies: mexican rx online – mexican rx online
canadian pharmacy online ship to usa: canadian pharmacy 1 internet online drugstore – buy drugs from canada
п»їbest mexican online pharmacies: mexican pharmacy – mexican drugstore online
http://indianpharm.shop/# reputable indian pharmacies
mexico pharmacies prescription drugs: mexico pharmacy – mexico pharmacy
https://mexicanpharm.online/# buying from online mexican pharmacy
является участником банды . Именно помогла ему открыть сайт и теперь она за своё покровительство и раскрутку получает часть денег от клиентов-лохов, которых обработал мерзавец-шарлатан.
Как это обычно и бывает у мошенников, — это не настоящие имя-отчество, а очередной псевдоним. За случайной кличкой скрывается безработный, раньше уже мотавший сроки, продолжающий свою мошенническую деятельность.
Вместо реального фото, на вывешено сгенерированное нейросетью изображение мультяшного персонажа, эдакого старца-волхва. Настоящую же свою испитую,физиономию немаг тщательно скрывает, так как справедливо опасается, что вычислят и накажут.
Также на размещены написанные аферистом отзывы даже за 2010 год. В реальности же сайт появился всего пару недель назад – 15 февраля 2024 года. И именно эти две недели уголовник обманывает именно под кличкой.
Однако у него уже есть опыт в мошеннической деятельности, так как раньше он промышлял под кличками:
Будьте бдительны: и на сайте и на других подобных площадках действуют опасные и умелые в своей противозаконной деятельности аферисты. Они знают, как войти в доверие, но никто из них не способен оказать реальную помощь.
И шарлатан и подобные ему, постоянно дают пустые обещания. Деньги гребут лопатой, но никогда ни одному человеку не помогут. Так как все приписываемые им сверхъестественные способности — один сплошной обман. Ни один реальный отзыв от обманутых клиентов на не будет пропущен лжемагом – все отзывы от сам себе и пишет.
прослыл я шарлатаном отчего прослыл я скандалистом
baclofen alcohol interaction
augmentin heartburn
online shopping pharmacy india: buy prescription drugs from india – top 10 pharmacies in india
mexico drug stores pharmacies: pharmacies in mexico that ship to usa – mexico pharmacy
gates of olympus oyna: gates of olympus demo oyna – gates of olympus demo
aviator sinyal hilesi apk: aviator mostbet – aviator casino oyunu
https://aviatoroyna.bid/# aviator
https://game24.space/
http://sweetbonanza.bid/# sweet bonanza free spin demo
http://sweetbonanza.bid/# sweet bonanza yasal site
slot oyun siteleri: slot casino siteleri – guvenilir slot siteleri
https://podacha-blud.com/
https://gruzchikirabotnik.ru/
https://slotsiteleri.guru/# güvenilir slot siteleri
buy zidovudine 300mg – purchase zyloprim online buy zyloprim 300mg pills
Ищете профессиональных грузчиков, которые справятся с любыми задачами быстро и качественно? Наши специалисты обеспечат аккуратную погрузку, транспортировку и разгрузку вашего имущества. Мы гарантируем грузчики в самаре недорого, внимательное отношение к каждой детали и доступные цены на все виды работ.
clozaril 100mg oral – glimepiride online order famotidine 20mg cheap
clozapine 50mg us – brand accupril pepcid 40mg usa
pin up casino giris: pin-up online – pin up bet
https://gruzchikibol.ru
http://pinupgiris.fun/# pin-up bonanza
pin up casino guncel giris: aviator pin up – pin-up giris
https://slotsiteleri.guru/# deneme bonusu veren siteler
http://slotsiteleri.guru/# deneme bonusu veren siteler
oyun siteleri slot: canl? slot siteleri – casino slot siteleri
https://slotsiteleri.guru/# 2024 en iyi slot siteleri
Your post was a beacon of knowledge. Thank you for illuminating this subject.
https://gruzchikivagon.ru
aviator oyna slot: aviator oyunu 100 tl – aviator oyunu 50 tl
https://aviatoroyna.bid/# aviator bahis
https://gruzchikistudent.ru
https://pinupgiris.fun/# pin up güncel giris
https://gruzchikietazh.ru
gates of olympus slot: gates of olympus oyna demo – gate of olympus hile
https://gruzchikibaza.ru
2024 en iyi slot siteleri: en guvenilir slot siteleri – slot siteleri 2024
https://gatesofolympus.auction/# gates of olympus demo oyna
quetiapine 50mg us – buy generic quetiapine for sale eskalith without prescription
https://gatesofolympus.auction/# gates of olympus sirlari
sweet bonanza kazanc: sweet bonanza demo turkce – sweet bonanza
http://slotsiteleri.guru/# slot oyunlari siteleri
http://aviatoroyna.bid/# aviator
gate of olympus hile: gates of olympus s?rlar? – gates of olympus oyna
https://o-okkultizme.com
ashwagandha herb
https://aviatoroyna.bid/# aviator
https://catherineasquithgallery.com
celexa starting dose
pin up guncel giris: pin-up giris – pin-up giris
дешево заказать грузчиков
aviator oyunu 50 tl: aviator hilesi ucretsiz – aviator hilesi ucretsiz
no rx pharmacy
http://gatesofolympus.auction/# gates of olympus guncel
https://gruzchikjob.ru
https://gatesofolympus.auction/# gates of olympus slot
http://gatesofolympus.auction/# gates of olympus demo türkçe
sweet bonanza: sweet bonanza guncel – sweet bonanza yasal site
https://gatesofolympus.auction/# gates of olympus demo türkçe oyna
deneme bonusu veren slot siteleri: bonus veren slot siteleri – slot kumar siteleri
sweet bonanza 100 tl: sweet bonanza hilesi – sweet bonanza kazanma saatleri
http://pinupgiris.fun/# pin up
canada pharmacy online: canada pharmacy online legit – canadian pharmacy ltd
reputable mexican pharmacies online: cheapest mexico drugs – medication from mexico pharmacy
canada discount pharmacy Certified Canadian Pharmacy canadian pharmacy 365
http://mexicanpharmacy.shop/# buying prescription drugs in mexico
buy anafranil 50mg for sale – imipramine 75mg usa doxepin 25mg sale
order clomipramine 25mg pill – asendin 50 mg pills doxepin order
order seroquel for sale – buy sertraline 50mg pill eskalith medication
canadian pharmacy no scripts Large Selection of Medications canadian 24 hour pharmacy
Предлагаем слуги: https://lit9.ru, демонтаж фундамента, слом домов.
precription drugs from canada: canadian discount pharmacy – online canadian pharmacy
www canadianonlinepharmacy Licensed Canadian Pharmacy canada pharmacy online
online shopping pharmacy india: Cheapest online pharmacy – indian pharmacy
hydroxyzine 10mg price – buy pamelor 25 mg generic amitriptyline for sale online
https://mexicanpharmacy.shop/# purple pharmacy mexico price list
pharmacies in mexico that ship to usa: mexico pharmacy – buying prescription drugs in mexico
pharmacy website india Healthcare and medicines from India cheapest online pharmacy india
mexican rx online: mexican pharmacy – reputable mexican pharmacies online
reputable indian pharmacies: indian pharmacy – india pharmacy
https://mhpereezd.ru
mail order pharmacy india indian pharmacy delivery india online pharmacy
order synthroid
best canadian pharmacy: canadian pharmacy 24 – online canadian pharmacy
top 10 online pharmacy in india: Cheapest online pharmacy – legitimate online pharmacies india
ed drugs online from canada: safe canadian pharmacy – canadian pharmacy online
mexican border pharmacies shipping to usa: Mexican Pharmacy Online – medication from mexico pharmacy
world pharmacy india: Cheapest online pharmacy – online pharmacy india
online pharmacy india Cheapest online pharmacy indian pharmacy paypal
https://canadianpharmacy24.store/# canadian world pharmacy
canadianpharmacymeds com: canadian pharmacy 24 – canadian pharmacy price checker
canadian pharmacy no scripts: Large Selection of Medications – canadian pharmacy checker
п»їbest mexican online pharmacies: reputable mexican pharmacies online – mexico pharmacy
legal canadian pharmacy online pills now even cheaper safe canadian pharmacy
mexican pharmacy: Mexican Pharmacy Online – buying prescription drugs in mexico online
buying prescription drugs in mexico online: Mexican Pharmacy Online – best mexican online pharmacies
hydroxyzine online – endep 10mg generic generic endep
india pharmacy mail order Generic Medicine India to USA top 10 pharmacies in india
india online pharmacy: Healthcare and medicines from India – indian pharmacy online
cheapest online pharmacy india: Healthcare and medicines from India – buy medicines online in india
My spouse and I stumbled over here coming from a different
page and thought I might check things out. I like what I see so i
am just following you. Look forward to looking over your web page repeatedly.
canadian drugs online: Licensed Canadian Pharmacy – pharmacy in canada
http://mexicanpharmacy.shop/# medicine in mexico pharmacies
india pharmacy mail order Cheapest online pharmacy top 10 pharmacies in india
I’m not sure exactly why but this site is loading very slow for me.
Is anyone else having this problem or is it a issue on my
end? I’ll check back later on and see if the problem still exists.
best online pharmacies in mexico cheapest mexico drugs purple pharmacy mexico price list
reputable indian pharmacies: Healthcare and medicines from India – india online pharmacy
cheapest online pharmacy india: Healthcare and medicines from India – india pharmacy
canada drugs online: canadian family pharmacy – best canadian pharmacy
canadian pharmacy online ship to usa: prescription drugs canada buy online – canadianpharmacymeds
buy medicines online in india indian pharmacy delivery online shopping pharmacy india
canadian discount pharmacy: Prescription Drugs from Canada – canadapharmacyonline legit
ordering prednisone: buy prednisone online no script – no prescription online prednisone
http://prednisoneall.com/# prednisone online pharmacy
https://zithromaxall.shop/# zithromax online paypal
Incredible points. Sound arguments. Keep up the amazing work.
amoxicillin 875 mg tablet amoxicillin 500 mg without a prescription amoxicillin pharmacy price
I am really impressed with your writing skills as well as with the layout on your blog.
Is this a paid theme or did you modify it yourself?
Either way keep up the excellent quality writing,
it’s rare to see a nice blog like this one today.
I have read so many articles about the blogger lovers but
this post is in fact a fastidious post, keep it up.
https://zithromaxall.com/# zithromax pill
https://gruzchikivrn.ru
zithromax 500mg over the counter zithromax cost australia zithromax 600 mg tablets
http://zithromaxall.shop/# buy zithromax 1000mg online
I loved as much as you will receive carried out right here.
The sketch is tasteful, your authored subject matter stylish.
nonetheless, you command get bought an edginess over that you wish be delivering the following.
unwell unquestionably come more formerly again as exactly the same
nearly very often inside case you shield this hike.
https://prednisoneall.shop/# how much is prednisone 10mg
amoxicillin canada price: amoxicillin from canada – amoxicillin 500 mg cost
http://clomidall.shop/# can you get generic clomid for sale
where to get cheap clomid without a prescription cost of generic clomid pills can i get clomid pill
amoxicillin 775 mg: amoxicillin 500mg capsules price – where to buy amoxicillin over the counter
http://zithromaxall.com/# zithromax drug
amoxicillin over the counter – buy keflex 250mg without prescription ciprofloxacin online
clavulanate us – where can i buy linezolid order ciprofloxacin 500mg pill
can you buy generic clomid online order cheap clomid now how can i get cheap clomid no prescription
https://zithromaxall.shop/# where can i buy zithromax medicine
augmentin 625mg cost – order generic ciprofloxacin 500mg order ciprofloxacin online
Good site you’ve got here.. It’s difficult to find quality writing
like yours nowadays. I seriously appreciate people like you!
Take care!!
After checking out a few of the articles on your site, I honestly like your
technique of blogging. I book marked it to my bookmark site list and will be checking
back in the near future. Please check out my website as well and let me know what you think.
Hey! This is kind of off topic but I need some help
from an established blog. Is it tough to set up your own blog?
I’m not very techincal but I can figure things out pretty quick.
I’m thinking about creating my own but I’m not sure where to start.
Do you have any points or suggestions? Many thanks
http://amoxilall.shop/# amoxicillin from canada
http://amoxilall.com/# amoxicillin 825 mg
order cheap clomid for sale buy clomid without prescription get generic clomid tablets
https://gruzchikivrn.ru/
https://prednisoneall.shop/# can i buy prednisone online without a prescription
I’m truly enjoying the design and layout of your website.
It’s a very easy on the eyes which makes it much more pleasant for me
to come here and visit more often. Did you hire out a designer to create your
theme? Great work!
amoxicillin without a prescription: price for amoxicillin 875 mg – where can i buy amoxicillin online
http://prednisoneall.shop/# prednisone nz
prednisone 2.5 mg tab how to get prednisone without a prescription prednisone 10mg tablets
https://amoxilall.com/# amoxicillin for sale online
https://amoxilall.shop/# canadian pharmacy amoxicillin
lamictal vs abilify
where can i purchase zithromax online: purchase zithromax z-pak – zithromax generic price
prednisone 10mg tablets prednisone for sale no prescription cost of prednisone 5mg tablets
Thanks for thr great article!
http://amoxilall.shop/# amoxicillin pharmacy price
This was a thoroughly insightful enjoy reading. Thank you for sharing your expertise!
http://prednisoneall.com/# medicine prednisone 5mg
Hi there i am kavin, its my first time to commenting anyplace,
when i read this post i thought i could also create comment due to this
brilliant paragraph.
http://prednisoneall.com/# prednisone 12 tablets price
Paragraph writing is also a excitement, if you be familiar with
afterward you can write otherwise it is complicated to write.
can i buy prednisone over the counter in usa prednisone tablets canada can you buy prednisone in canada
Keep on writing, great job!
This article is a perfect blend of informative and entertaining. Well done!
Your thoughtful analysis has really made me think. Thanks for the great enjoy reading!
http://zithromaxall.com/# where to get zithromax over the counter
prednisone 1 mg tablet prednisone 20 mg pill online prednisone 5mg
order amoxicillin generic – buy ceftin 500mg for sale buy baycip online
https://zithromaxall.shop/# zithromax over the counter canada
cialis for sale: Buy Cialis online – Tadalafil price
https://kamagraiq.shop/# Kamagra 100mg price
cheap kamagra Sildenafil Oral Jelly Kamagra 100mg
buy Kamagra: Kamagra Oral Jelly Price – Kamagra tablets
Tadalafil Tablet: Generic Tadalafil 20mg price – Cialis 20mg price
acarbose interactions
tadalafil 5mg
http://kamagraiq.shop/# sildenafil oral jelly 100mg kamagra
buy Kamagra: Kamagra Iq – buy kamagra online usa
semaglutide not working
Cialis 20mg price Generic Tadalafil 20mg price Buy Cialis online
buy kamagra online usa: buy Kamagra – buy kamagra online usa
cialis for sale: cialis without a doctor prescription – Generic Cialis without a doctor prescription
https://sildenafiliq.xyz/# cheapest viagra
http://kamagraiq.shop/# Kamagra Oral Jelly
cheap kamagra: Kamagra gel – buy Kamagra
generic sildenafil generic sildenafil Viagra tablet online
buy cialis pill: Buy Cialis online – buy cialis pill
Cialis 20mg price in USA Generic Cialis without a doctor prescription Cialis 20mg price in USA
super kamagra: kamagra best price – Kamagra 100mg price
tadalafil 20 mg online india
Viagra tablet online: buy viagra here – Cheap Viagra 100mg
https://diplom-sdan.ru/
http://kamagraiq.com/# Kamagra tablets
qiyezp.com
그는 차가운 표정으로 앞에 있는 빈 책상을 가리켰다.
Cheap Sildenafil 100mg cheapest viagra Viagra generic over the counter
Kamagra tablets: Kamagra Oral Jelly Price – sildenafil oral jelly 100mg kamagra
https://tadalafiliq.com/# Cialis 20mg price in USA
http://kamagraiq.com/# buy kamagra online usa
cheapest viagra: buy viagra online – Sildenafil 100mg price
best price for viagra 100mg best price on viagra order viagra
https://diplomnash.ru/
Viagra online price: sildenafil iq – Viagra Tablet price
https://kamagraiq.com/# п»їkamagra
worldwide pharmacy online
buy cialis pill: Cialis 20mg price in USA – Cialis 20mg price
Viagra generic over the counter buy viagra here cheapest viagra
https://kursovaya-student.ru/
https://kamagraiq.shop/# Kamagra Oral Jelly
https://kamagraiq.com/# buy kamagra online usa
kamagra: Kamagra tablets – kamagra
cheapest viagra: generic ed pills – Viagra online price
https://breaking-bad-serial.online/
Cialis without a doctor prescription Generic Tadalafil 20mg price Generic Cialis without a doctor prescription
Kamagra tablets: Kamagra Oral Jelly Price – kamagra
http://kamagraiq.shop/# Kamagra tablets
buy viagra here: sildenafil iq – sildenafil online
Tadalafil Tablet cialis best price Tadalafil price
https://sildenafiliq.xyz/# order viagra
https://tadalafiliq.com/# Buy Cialis online
sildenafil over the counter: viagra without prescription – Cheapest Sildenafil online
https://kvartiruise.ru/
synthroid coupon
http://sildenafiliq.com/# cheap viagra
п»їkamagra Kamagra Oral Jelly Price Kamagra 100mg
http://kamagraiq.com/# Kamagra 100mg price
canada drugs online: Cheapest drug prices Canada – canadian pharmacy online reviews
Online medicine order indian pharmacy reputable indian online pharmacy
http://indianpharmgrx.com/# indian pharmacy paypal
https://kvartiruless.ru/
repaglinide solid dispersion
remeron side effects in elderly
reputable canadian online pharmacies Pharmacies in Canada that ship to the US canada drugs
http://mexicanpharmgrx.shop/# mexico drug stores pharmacies
прогнозы на сегодня хоккей
http://canadianpharmgrx.com/# canada drugs
mexico drug stores pharmacies mexican pharmacy mexican border pharmacies shipping to usa
cleocin 300mg us – order oxytetracycline for sale purchase chloramphenicol generic
reputable indian online pharmacy: indian pharmacy delivery – Online medicine home delivery
http://indianpharmgrx.shop/# indianpharmacy com
purple pharmacy mexico price list: mexico drug stores pharmacies – buying prescription drugs in mexico
pharmacy website india Generic Medicine India to USA indian pharmacy paypal
http://mexicanpharmgrx.com/# reputable mexican pharmacies online
https://kvartirulyspb.ru/
mexican border pharmacies shipping to usa: Mexico drugstore – mexican border pharmacies shipping to usa
qiyezp.com
“뭐?” Fang Jifan은 Zhu Houzhao의 의도하지 않은 말에 당황했습니다.
https://indianpharmgrx.com/# india pharmacy
cheapest pharmacy canada canadian pharmacy cheap legit canadian online pharmacy
сочи гостиницы
zithromax 500mg sale – ofloxacin 200mg pill order ciplox
protonix side effects
robaxin cost
order azithromycin 500mg for sale – buy tetracycline without prescription ciplox 500mg oral
http://canadianpharmgrx.xyz/# legal to buy prescription drugs from canada
buying prescription drugs in mexico Pills from Mexican Pharmacy medicine in mexico pharmacies
https://kvartiruerspb.ru/
my canadian pharmacy: Certified Canadian pharmacies – canada drugs
https://indianpharmgrx.com/# indianpharmacy com
canadian online pharmacy reviews: canadian pharmacy – legit canadian online pharmacy
mexican mail order pharmacies: mexican pharmacy – mexico pharmacies prescription drugs
canada pharmacy Canada pharmacy online buy canadian drugs
https://indianpharmgrx.com/# india pharmacy
Thank you for making complex topics accessible and engaging.
canadian pharmacy 365 canadian pharmacy best canadian pharmacy
https://canadianpharmgrx.xyz/# best canadian online pharmacy
Thank you for consistently producing such high-quality content.
mexico pharmacies prescription drugs: Pills from Mexican Pharmacy – reputable mexican pharmacies online
http://indianpharmgrx.shop/# Online medicine order
https://zhkstroykaspb.ru/
best online pharmacy india Healthcare and medicines from India indian pharmacies safe
cleocin 150mg generic – order cefpodoxime 100mg online cheap chloramphenicol without prescription
http://canadianpharmgrx.xyz/# my canadian pharmacy review
https://kvartiruekb.ru/
legit canadian pharmacy: online canadian pharmacy – canada drugs reviews
http://mexicanpharmgrx.com/# mexican mail order pharmacies
mexico drug stores pharmacies: online pharmacy in Mexico – best online pharmacies in mexico
best online pharmacies in mexico online pharmacy in Mexico п»їbest mexican online pharmacies
http://indianpharmgrx.com/# indian pharmacy online
generic doxycycline: how to buy doxycycline online – doxycycline hyclate
cytotec buy online usa: buy cytotec in usa – п»їcytotec pills online
cytotec buy online usa cytotec online buy cytotec online
https://zhknoviydom.ru/
Your dedication to quality content is evident. Keep up the great work!
diflucan 150 mg tablets: how to get diflucan – buying diflucan over the counter
https://misoprostol.top/# Cytotec 200mcg price
doxycycline tablets online doxycycline doxycycline online
cipro pharmacy: cipro ciprofloxacin – buy cipro
I’m in awe of the way you handle topics with both grace and authority.
cipro for sale: ciprofloxacin 500mg buy online – cipro
purchase cytotec: Abortion pills online – cytotec abortion pill
common side effects of tamoxifen: does tamoxifen cause menopause – alternatives to tamoxifen
diflucan 150 tab diflucan pills diflucan 50mg capsules
tamoxifen postmenopausal: nolvadex gynecomastia – tamoxifen for breast cancer prevention
buy generic synthroid
generic prednisone tablets
buy doxycycline cheap buy doxycycline 100mg doxy 200
tamoxifen vs clomid: tamoxifen lawsuit – common side effects of tamoxifen
purchase cytotec: buy cytotec online fast delivery – buy misoprostol over the counter
https://diflucan.icu/# generic diflucan 150 mg
https://noviydomstroika.ru/
This post was a breath of fresh air. Thank you for your unique insights!
stromectol for human – purchase doryx online purchase cefaclor generic
how to buy doxycycline online: buy doxycycline 100mg – doxycycline hyc 100mg
ivermectin 3mg online – ivermectin 6mg over counter cefaclor oral
where to buy nolvadex how to lose weight on tamoxifen tamoxifen alternatives
prednisone 20 mg online
Outstanding feature
generic diflucan 150 mg: diflucan capsule 150mg – buy diflucan without a prescription
ventolin pills – allegra pill order theophylline online
best price for synthroid
https://reshaitzadachi.ru/
buy diflucan online usa diflucan 6 tabs diflucan 150 capsule
where can i buy cipro online: cipro for sale – antibiotics cipro
ordering lisinopril without a prescription uk
synthroid 75 mcg tablet price
buy ciprofloxacin: where can i buy cipro online – ciprofloxacin mail online
synthroid 125
compare prednisone prices
levothyroxine ordering online
diflucan 150 mg pill diflucan 100 mg tab diflucan canadian pharmacy
buy cytotec pills online cheap: buy misoprostol over the counter – cytotec online
price of prednisone 50 mg
buy cytotec: cytotec pills online – Cytotec 200mcg price
http://doxycyclinest.pro/# doxycycline generic
prednisone buy cheap
buy generic ciprofloxacin antibiotics cipro buy cipro online canada
pharmacy order online
cytotec pills buy online: buy cytotec pills – cytotec pills buy online
tamoxifen alternatives: tamoxifen and depression – tamoxifen dosage
azithromycin price australia
canadian pharmacy 24h com
synthroid 112 mg
arimidex vs tamoxifen bodybuilding who should take tamoxifen tamoxifen endometriosis
glucophage 500 mg tablet
diflucan 100 mg tab: diflucan 6 tablets – diflucan otc canada
The balance and fairness in The writing make The posts a must-read for me. Great job!
buy generic ciprofloxacin: ciprofloxacin mail online – buy generic ciprofloxacin
purchase generic cialis online
doxycycline without a prescription: doxycycline 100mg price – buy cheap doxycycline
prednisone 10mg
synthroid 112 coupon
cheap valtrex canada
buy azithromycin 500mg uk
buy misoprostol over the counter cytotec abortion pill buy cytotec over the counter
prinivil brand name
buy cytotec: Abortion pills online – buy cytotec
prednisone 8 mg
Cytotec 200mcg price: Misoprostol 200 mg buy online – buy cytotec in usa
4mg prednisone daily
https://misoprostol.top/# order cytotec online
valtrex medication
Misoprostol 200 mg buy online: cytotec abortion pill – Abortion pills online
diflucan discount diflucan 150 otc diflucan online buy
cost of brand name lisinopril
cost of tadalafil in mexico
The words are like a melody, each post a new verse in a song I never want to end.
metformin cost in india
cytotec pills online: buy cytotec online – Cytotec 200mcg price
synthroid 0.05 mg tablets
synthroid 25 mg coupon
http://azithromycina.pro/# zithromax cost canada
clomid without insurance can i order clomid without prescription clomid no prescription
purchase albuterol inhalator for sale – promethazine buy online buy theophylline 400mg generic
best generic tadalafil
synthroid europe
zithromax for sale online: zithromax buy online – how to get zithromax
tadalafil 20mg mexico
https://t.me/SecureIyContactingClAbot
metformin 2
where can you buy prednisone: prednisone 10mg price in india – average cost of prednisone 20 mg
lisinopril 40 mg price in india
can i order cheap clomid how can i get clomid buy clomid tablets
repaglinide method development
amoxicillin generic brand: amoxicillin 500 mg tablets – amoxicillin 500 mg price
remeron tablets
3000mg valtrex
I’m bookmarking this for future reference. Your advice is spot on!
canadian 24 hour pharmacy
Your insights have added a lot of value to my understanding. Thanks for sharing.
synthroid 126
no prescription synthroid
ivermectin generic name: stromectol in canada – ivermectin price usa
metformin hcl 500
can you buy stromectol over the counter: cost of ivermectin 1% cream – stromectol how much it cost
http://stromectola.top/# ivermectin buy
http://womangu.ru
buy stromectol uk ivermectin 8000 mcg ivermectin goodrx
mail order pharmacy india
mexican pharmacy
zithromax for sale online
http://stromectola.top/# ivermectin 12 mg
synthroid drooling
sitagliptin route of administration
clarinex tablet – buy flixotide sale buy albuterol 2mg generic
ivermectin 5 mg: ivermectin ebay – ivermectin price comparison
Услуга по сносу старых домов и вывозу мусора в Москве и Московской области. Мы предоставляем услуги по сносу старых зданий и удалению мусора на территории Москвы и Подмосковья. Услуга разбор дома после пожара выполняется опытными специалистами в течение 24 часов после оформления заказа. Перед началом работ наш эксперт бесплатно приезжает на объект для оценки объёма работ и консультации. Чтобы получить дополнительную информацию и рассчитать стоимость услуг, свяжитесь с нами по телефону или оставьте заявку на сайте компании.
http://azithromycina.pro/# buy zithromax without presc
zithromax online prescription
amoxicillin 750 mg price ampicillin amoxicillin amoxicillin 500mg capsule
generic amoxicillin online: ampicillin amoxicillin – order amoxicillin online uk
can i get cheap clomid no prescription: clomid medication – can i get cheap clomid online
daily use cialis cost
canada drugstore pharmacy rx
This post is packed with useful insights. Thanks for sharing your knowledge!
buy prednisone online canada: prednisone sale – prednisone 20 mg tablets
http://amoxicillina.top/# price of amoxicillin without insurance
Your writing style is captivating! I was engaged from start to finish.
cheap methylprednisolone – singulair online order buy azelastine 10 ml online cheap
medicine prednisone 5mg: prednisone 20mg capsule – generic prednisone cost
canada rx pharmacy
buy depo-medrol canada – cetirizine 10mg oral astelin 10ml oral
how can i get generic clomid cost generic clomid where to get generic clomid pill
tadalafil 10 mg canadian pharmacy
can i buy clomid for sale: where buy generic clomid – how to buy cheap clomid prices
buy tadalafil 20mg uk
losartan lisinopril
https://amoxicillina.top/# amoxicillin 500mg pill
purchase azithromycin 500 mg
cheapest prescription pharmacy
Услуга по сносу старых зданий и утилизации отходов в Москве и Московской области. Мы предоставляем услуги по сносу старых сооружений и удалению мусора на территории Москвы и Московской области. Услуга демонтаж фундамента дома выполняется квалифицированными специалистами в течение 24 часов после оформления заказа. Перед началом работ наш эксперт бесплатно посещает объект для определения объёма работ и предоставления консультаций. Чтобы получить дополнительную информацию и рассчитать стоимость услуг, свяжитесь с нами по телефону или оставьте заявку на сайте компании.
buy synthroid 88 mcg online
prednisone 10
ivermectin purchase: ivermectin 1 topical cream – how much does ivermectin cost
canadian online pharmacy no prescription
https://onlinepharmacyworld.shop/# online pharmacy no prescription
canadian pharmacy no prescription canadian pharmacy no prescription needed buying prescription drugs from canada
https://medicationnoprescription.pro/# buy pills without prescription
no prescription drugs: online pharmacy not requiring prescription – buy meds online without prescription
I appreciate the unique viewpoints you bring to your writing. Very insightful!
where to get valtrex
american online pharmacy
https://kursovuyupishem.ru/
buy pain meds online without prescription: canada drugs without prescription – buy medication online without prescription
https://edpill.top/# cheap ed meds
Your piece was both informative and thought-provoking. Thanks for the great work!
spironolactone 90 day supply
buy metformin 500
cheapest pharmacy for prescriptions without insurance pharmacy coupons canadian pharmacy discount code
494829 metformin
buy azithromycin
best online pharmacy without prescription: how to get prescription drugs from canada – non prescription canadian pharmacy
https://edpill.top/# low cost ed pills
canadian pharmacy 24h com safe
valtrex cheap
https://edpill.top/# online erectile dysfunction medication
buy azithromycin 500mg online us
https://edpill.top/# cheap erection pills
online drugstore no prescription buy medications without a prescription mexican pharmacy no prescription
cheap ed pills: pills for erectile dysfunction online – online ed medication
synthroid nz
mexican online mail order pharmacy
http://medicationnoprescription.pro/# buy medication online no prescription
metformin canada over the counter
https://edpill.top/# ed online meds
list of online pharmacies
tadalafil soft tabs
https://onlinepharmacyworld.shop/# canadian pharmacy world coupons
cheapest pharmacy to fill prescriptions without insurance
drugstore com online pharmacy prescription drugs: rx pharmacy no prescription – online pharmacy non prescription drugs
legitimate online pharmacy no prescription canada online prescription overseas online pharmacy-no prescription
You’ve presented a complex topic in a clear and engaging way. Bravo!
https://onlinepharmacyworld.shop/# uk pharmacy no prescription
order desloratadine 5mg for sale – buy beclamethasone no prescription order albuterol pill
medical mall pharmacy
buying online prescription drugs: canada drugs without prescription – buy prescription drugs on line
order lisinopril online from canada
can you buy prednisone online
cheap erection pills: buy ed medication online – cheap ed medication
https://edpill.top/# ed medicine online
generic for synthroid
what is the cheapest ed medication best online ed medication erectile dysfunction medications online
micronase 2.5mg uk – glyburide 5mg generic dapagliflozin 10mg ca
synthroid cellulite
safe canadian pharmacies
PBN sites
We will create a system of private blog network sites!
Benefits of our self-owned blog network:
We carry out everything so google doesn’t grasp that this A private blog network!!!
1- We acquire web domains from separate registrars
2- The primary site is hosted on a VPS hosting (Virtual Private Server is fast hosting)
3- The rest of the sites are on various hostings
4- We designate a distinct Google ID to each site with verification in Search Console.
5- We design websites on WP, we do not utilize plugins with aided by which malware penetrate and through which pages on your websites are created.
6- We never reproduce templates and utilize only distinct text and pictures
We do not work with website design; the client, if desired, can then edit the websites to suit his wishes
http://onlinepharmacyworld.shop/# promo code for canadian pharmacy meds
lisinopril 12.5 tablet
20 mg cialis
http://edpill.top/# erectile dysfunction meds online
can you buy prescription drugs in canada: no prescription on line pharmacies – cheap drugs no prescription
how to buy zithromax
Каталог салонов эпиляции https://findepil.ru/ Москвы и Московской области. Химки, Люберцы, Красногорск, Зеленоград и т.д. Все виды эпиляции – электроэпиляция, депиляция воском, шугаринг, лазерная эпиляция. Можно выбрать салон по цене, для примера выбраны стандартные процедуры эпиляции – руки воск, ноги шугаринг. Каталог постоянно пополняется.
legal online pharmacy coupon code
https://casinvietnam.com/# web c? b?c online uy tin
game c? b?c online uy tin casino tr?c tuy?n vi?t nam casino tr?c tuy?n vi?t nam
can i buy azithromycin in mexico
dánh bài tr?c tuy?n: choi casino tr?c tuy?n trên di?n tho?i – casino online uy tín
buy tadalafil 10mg
The calculator on a smartphone is very constrained in functions. As an architect, I often require a scientific online calculator, such as this https://calculator-online.info/. It is effective for various tasks like financial calculations, percentage calculations, solving complex equations, finding square and cube roots, and more
zestoretic 20 25mg
cost of lisinopril 40mg
safe online pharmacies in canada
https://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
synthroid canada
casino tr?c tuy?n vi?t nam game c? b?c online uy tin game c? b?c online uy tin
tadalafil 20mg price uk
Журнал для женщин http://womangu.ru/ – актуальные новости о звездах и шоу-бизнесе, модные тенденции, статьи об отношениях, красоте и здоровье, рецепты и каталог диет на женском портале.
https://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
best canadian online pharmacy
game c? b?c online uy tín: casino online uy tín – game c? b?c online uy tín
https://praktikaotchet.ru/
no prescription pharmacy paypal
Cada jogador individual pode atestar sua melhor maneira de jogar roleta, é só escolher a sua aposta e girar a roleta para tentar a sorte. O Betway Casino, big bass splash jogue em dispositivos móveis portanto. Por isso, big Bass Splash opção ante bet para aumentar a aposta Dragons Fire. Além da emoção de jogar e ganhar, o Big Bass Splash também oferece a oportunidade de se conectar com outros entusiastas de jogos de casino. Muitos cassinos online que hospedam o jogo oferecem recursos de bate-papo e fóruns onde os jogadores podem compartilhar dicas, estratégias e experiências de jogo. Essa comunidade vibrante adiciona uma dimensão social ao jogo, tornando-o ainda mais envolvente e divertido para os participantes. No Big Bass Splash, os jogadores são desafiados a formar combinações vencedoras de símbolos nos rolos para ganhar prêmios emocionantes. Com uma estrutura de 5 rolos, 3 linhas e 10 linhas de pagamento fixas, este jogo oferece diversas oportunidades para os jogadores aumentarem seus ganhos.
http://www.okaywan.com/home.php?mod=space&uid=501944
Os bônus também foram criados para incentivar os jogadores a continuar apostando usando seu próprio dinheiro quando os fundos de bônus acabarem. Ambas as partes devem ganhar com um bom bônus de aposta. Por exemplo, os clientes podem receber fundos de bônus para apostar, enquanto os operadores conseguem adquirir clientes pagantes. Os desafios surgem quando alguns usuários começam a usar bônus para atividades mal-intencionadas, como lavagem de dinheiro. Desenvolvedores Edital nº 94 2024 – Processo Seletivo Simplificado de Cursos de Graduação – Campus Januária- Inscrições: até 28 03 2024 (17h) Conheça o Vaidebob, reconhecido como o melhor cassino online para jogar grátis. A plataforma se destaca no mercado por oferecer milhares de opções de jogos de cassino gratuitos, perfeitos para aqueles que desejam testar suas habilidades, divertir-se e conhecer todos os recursos dos jogos antes de apostar com dinheiro real.
game c? b?c online uy tin casino tr?c tuy?n uy tin web c? b?c online uy tin
https://praktikaucheba.ru/
glucophage 250
can you buy synthroid over the counter
efficacy and safety of tamsulosin for the treatment of benign prostatic hyperplasia a meta analysis
prinivil generic
best canadian pharmacy
https://referatnash.ru/
best australian online pharmacy
over the counter prednisone medicine
zithromax canadian pharmacy
pharmacy com canada
Meet to our website, your premier online core to African sports, music, and luminary updates. We provide for everything from overwhelming sports events like the Africa Cup of Nations to the latest trends in Afrobeats and ancestral music. Research chic interviews and features on renowned personalities making waves across the continent and beyond.
At our website, we forearm timely and engaging content that celebrates the disparity and vibrancy of African culture. Whether you’re a sports lover, music lover, or eccentric about Africa’s substantial figures, go our community and stay connected for constantly highlights and in-depth stories showcasing the in the most suitable way of African inclination and creativity https://nouvellesafrique.africa/qui-est-exactement-pepe-munoz-l-individu-dont-la/.
Visit our website today and see the potent the human race of African sports, music, and distinguished personalities. Immerse yourself in the richness of Africa’s cultural scene with us!
lisinopril 2.5
lisinopril 20 mg tablet price
buy valtrex online
online pharmacy indonesia
order prednisone 10 mg tablet
Качественное написание рефератов https://referatnovy.ru/, курсовых и дипломных работ от лучших авторов. Уникальные работы под ключ. Заказать студенческую работу за 2 дня.
azithromycin 500 mg order online
Написание дипломных работ https://diplompishem.ru/, курсовых и рефератов от лучших авторов. Заказать студенческую работу с антиплагиатом и уникализацией.
family rx pharmacy
buy metformin online us
pharmacy online track order
glyburide 5mg usa – brand dapagliflozin dapagliflozin 10mg pill
Заказать seo продвижение сайта https://seodelay.ru/ и услуги по продвижению сайта в поисковых системах. SEO продвижение сайтов в топ выдачи в поисковых системах Яндекс, Google. Проведем профессиональную раскрутку и поисковую оптимизацию вашего сайта по низкой стоимости.
SEO продвижение и раскрутка сайтов с гарантией https://seomayker.ru/. Услуги по продвижению сайта в поисковых системах. Видимость вашего сайта в поисковых системах повысится и вы привлечете больше качественных посетителей без необходимости платить за рекламу.
tizanidine side effects hair loss
buy synthroid
casino tr?c tuy?n: dánh bài tr?c tuy?n – dánh bài tr?c tuy?n
Поисковое SEO продвижение сайтов в Москве https://seosferaya.ru/, стоимость тарифов на быструю и недорогую раскрутку сайта в ТОП-10. Оптимизация сайтов в поисковых системах Яндекс и Google. Быстро раскручиваем сайты за счет опыта. Тарифы и цены, кейсы и результаты наших работ в Москве и других крупных городах РФ
order generic tadalafil
Комплексное продвижение сайтов в Москве https://seosferaya.ru/ под ключ. SEO раскрутка сайта в топ Яндекс и Google от профессионалов, первые результаты уже через месяц. Комплексное продвижение сайтов с гарантией.
dánh bài tr?c tuy?n: dánh bài tr?c tuy?n – dánh bài tr?c tuy?n
Your passion for this subject shines through your words. Inspiring!
http://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
I’m genuinely impressed by the depth of your analysis. Great work!
generic for synthroid
order prandin 1mg for sale – order repaglinide without prescription order jardiance 10mg for sale
web c? b?c online uy tín: web c? b?c online uy tín – choi casino tr?c tuy?n trên di?n tho?i
https://casinvietnam.com/# casino tr?c tuy?n uy tin
best price for synthroid
casino tr?c tuy?n: casino online uy tín – web c? b?c online uy tín
generic cialis tadalafil 20mg
american pharmacy
https://casinvietnam.com/# game c? b?c online uy tin
price of azithromycin tablets
synthroid thyroid
web c? b?c online uy tín: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n vi?t nam
https://casinvietnam.shop/# casino tr?c tuy?n vi?t nam
tadalafil generic from canada
pharmacy discount coupons
casino tr?c tuy?n uy tín: casino tr?c tuy?n – casino tr?c tuy?n vi?t nam
cheapest cialis usa
synthroid 200 mg price
oral metformin 500mg – buy precose pills precose pill
casino online uy tín: web c? b?c online uy tín – casino tr?c tuy?n vi?t nam
http://casinvietnam.shop/# casino tr?c tuy?n uy tin
glycomet canada – hyzaar online pill acarbose 50mg
danh bai tr?c tuy?n choi casino tr?c tuy?n tren di?n tho?i danh bai tr?c tuy?n
buy zithromax no prescription
я уже смотрел обзор здесь https://my-obzor.com/ перед тем, как сделать заказ. Не сказать, что все отзывы были 100% положительные, там уже упоминались основные минусы и плюсы
casino online uy tín: casino tr?c tuy?n vi?t nam – web c? b?c online uy tín
You’ve presented a complex topic in a clear and engaging way. Bravo!
PBN sites
We will establish a web of PBN sites!
Merits of our private blog network:
We perform everything SO THAT GOOGLE does not comprehend that THIS IS A private blog network!!!
1- We purchase web domains from distinct registrars
2- The principal site is hosted on a virtual private server (VPS is fast hosting)
3- Additional sites are on separate hostings
4- We allocate a separate Google account to each site with confirmation in Search Console.
5- We make websites on WordPress, we don’t employ plugins with the help of which Trojans penetrate and through which pages on your websites are established.
6- We never repeat templates and employ only unique text and pictures
We refrain from work with website design; the client, if desired, can then edit the websites to suit his wishes
https://casinvietnam.com/# web c? b?c online uy tin
choi casino tr?c tuy?n tren di?n tho?i game c? b?c online uy tin casino tr?c tuy?n uy tin
canadian discount pharmacy
lisinopril 10 12.55mg
заказать мебель
prednisone purchase
casino tr?c tuy?n vi?t nam: casino tr?c tuy?n vi?t nam – casino tr?c tuy?n vi?t nam
офисная мебель в минске
casino tr?c tuy?n vi?t nam casino tr?c tuy?n choi casino tr?c tuy?n tren di?n tho?i
http://casinvietnam.shop/# web c? b?c online uy tin
tadalafil united states
casino tr?c tuy?n: casino tr?c tuy?n vi?t nam – casino online uy tín
https://petroyalportrait.com/
mexican online mail order pharmacy
where can i purchase valtrex
casino tr?c tuy?n vi?t nam casino tr?c tuy?n web c? b?c online uy tin
http://casinvietnam.shop/# casino tr?c tuy?n
game c? b?c online uy tín: casino tr?c tuy?n vi?t nam – game c? b?c online uy tín
zetia 10mg
patients who are prescribed olanzapine (zyprexa) should be monitored for
https://petroyalportrait.com/
prednisone without prescription 10mg
casino online uy tin casino tr?c tuy?n casino online uy tin
casino tr?c tuy?n vi?t nam: casino tr?c tuy?n vi?t nam – game c? b?c online uy tín
http://casinvietnam.com/# casino tr?c tuy?n
legit mexican pharmacy
canada pharmacy online
tadalafil black
casino online uy tin danh bai tr?c tuy?n danh bai tr?c tuy?n
game c? b?c online uy tín: casino tr?c tuy?n vi?t nam – dánh bài tr?c tuy?n
azithromycin 250 mg price in india
casino tr?c tuy?n vi?t nam game c? b?c online uy tin choi casino tr?c tuy?n tren di?n tho?i
choi casino tr?c tuy?n trên di?n tho?i: casino tr?c tuy?n vi?t nam – dánh bài tr?c tuy?n
я уже смотрел обзор здесь https://my-obzor.com/ перед тем, как сделать заказ. Не сказать, что все отзывы были 100% положительные, там уже упоминались основные минусы и плюсы.
http://casinvietnam.shop/# casino online uy tin
best price for synthroid 75 mcg
zithromax pills online
tadalafil 2.5 mg online india
canadian pharmacy scam Large Selection of Medications from Canada canadian pharmacy world reviews
https://indiaph24.store/# top 10 pharmacies in india
pharmacy wholesalers canada
where can i buy azithromycin over the counter nz
canadian pharmacy meds Prescription Drugs from Canada best canadian online pharmacy reviews
http://indiaph24.store/# cheapest online pharmacy india
buy valtrex generic
synthroid 150 cost
Online medicine home delivery buy medicines from India indian pharmacies safe
lisinopril 5mg prices
http://canadaph24.pro/# reliable canadian pharmacy reviews
azithromycin 2 tablets
https://seostrategia.ru/
wellbutrin menstrual cramps
legit canadian pharmacy canadian pharmacies best canadian pharmacy to buy from
lisinopril tabs 40mg
http://indiaph24.store/# indian pharmacy
zofran m 734
60 mg prednisone daily
best india pharmacy Cheapest online pharmacy п»їlegitimate online pharmacies india
http://mexicoph24.life/# mexican online pharmacies prescription drugs
buy prendesone without a prescription
valtrex medicine cost
trustworthy canadian pharmacy
azithromycin 500 mg cost in australia
canadian drug prices canadian pharmacies ordering drugs from canada
https://indiaph24.store/# buy medicines online in india
synthroid 50 pill
tadalafil order
buy cialis online 5mg
mexico pharmacy mexico drug stores pharmacies purple pharmacy mexico price list
https://canadaph24.pro/# canada drugs reviews
canadian pharmacy meds
cheapest online pharmacy india
mexico drug stores pharmacies cheapest mexico drugs reputable mexican pharmacies online
https://mexicoph24.life/# mexican drugstore online
tadalafil best price india
legitimate mexican pharmacy online
can you buy valtrex over the counter in usa
real canadian pharmacy canadian pharmacies canada pharmacy reviews
https://canadaph24.pro/# canadian neighbor pharmacy
prednisone without a script
valtrex rx where to buy
indian pharmacies safe Generic Medicine India to USA world pharmacy india
https://indiaph24.store/# india online pharmacy
where can i buy tadalafil
cheap viagra online canadian pharmacy
lamisil 250mg without prescription – purchase griseofulvin pill purchase griseofulvin online
medicine in mexico pharmacies buying prescription drugs in mexico online buying prescription drugs in mexico
buy valtrex online no prescription
cheapest on line valtrex without a prescription
https://canadaph24.pro/# canadian drug stores
online otc pharmacy
valtrex for sale cheap
india online pharmacy indian pharmacy fast delivery Online medicine home delivery
synthroid discount
http://canadaph24.pro/# onlinecanadianpharmacy
I’m impressed by your ability to convey such nuanced ideas with clarity.
online pharmacy dubai
valtrex tablet
Online medicine home delivery Cheapest online pharmacy india pharmacy mail order
https://indiaph24.store/# cheapest online pharmacy india
canadian pharmacy
how to get valtrex online
buy 1g azithromycin online
best online pharmacies in mexico mexican pharmacy pharmacies in mexico that ship to usa
http://canadaph24.pro/# reputable canadian online pharmacies
valtrex 250 mg 500 mg
cost less pharmacy
buy synthroid over the counter
buying prescription drugs in mexico Mexican Pharmacy Online medicine in mexico pharmacies
http://indiaph24.store/# buy prescription drugs from india
valtrex prescription price
cost for valtrex
tadalafil united states
vipps canadian pharmacy Certified Canadian Pharmacies legit canadian online pharmacy
trusted canadian pharmacy
http://canadaph24.pro/# canadian pharmacy india
canadian pharmacy online Licensed Canadian Pharmacy canadian pharmacy in canada
https://canadaph24.pro/# canadian pharmacy 1 internet online drugstore
zithromax generic price
rybelsus 14mg for sale – glucovance buy online order desmopressin
rybelsus price – buy rybelsus 14mg generic desmopressin over the counter
0.025 mg synthroid
valtrex over the counter uk
canadian pharmacy no rx needed canadian pharmacies canadian pharmacy victoza
http://canadaph24.pro/# canada drugstore pharmacy rx
synthroid mcg
Your attention to detail is remarkable. I appreciate the thoroughness of your post.
prednisone 5084
best online pharmacies in mexico mexico pharmacy mexican online pharmacies prescription drugs
https://indiaph24.store/# world pharmacy india
This was a thoroughly insightful enjoy reading. Thank you for sharing your expertise!
Закажите SEO продвижение сайта https://seo116.ru/ в Яндекс и Google под ключ в Москве и по всей России от экспертов. Увеличение трафика, рост клиентов, онлайн поддержка. Комплексное продвижение сайтов с гарантией!
buying prescription drugs in mexico online reputable mexican pharmacies online purple pharmacy mexico price list
60 mg prednisone
online pharmacy ordering
https://canadaph24.pro/# canadian pharmacy ratings
valtrex online no prescription
buy azithromycin india
canadian pharmacy 24h com safe Certified Canadian Pharmacies reputable canadian pharmacy
http://mexicoph24.life/# best online pharmacies in mexico
global pharmacy canada Certified Canadian Pharmacies best rated canadian pharmacy
https://mexicoph24.life/# reputable mexican pharmacies online
rx pharmacy online
synthroid 300 mg
how to get tadalafil online
tadalafil no prescription
lisinopril uk
metformin 178
https://indiaph24.store/# best india pharmacy
buy prescription drugs from india indian pharmacy cheapest online pharmacy india
buy prednisone online nz
https://canadaph24.pro/# best canadian online pharmacy reviews
canadian mail order pharmacy Licensed Canadian Pharmacy canadian pharmacies that deliver to the us
buy generic lamisil 250mg – terbinafine price buy grifulvin v paypal
Всё о радиаторах отопления https://heat-komfort.ru/ – выбор радиатора, монтаж, обслуживание.
http://canadaph24.pro/# best canadian online pharmacy
best online pharmacies in mexico cheapest mexico drugs mexico drug stores pharmacies
http://canadaph24.pro/# my canadian pharmacy reviews
Всё о радиаторах отопления https://heat-komfort.ru/ – выбор радиатора, монтаж, обслуживание.
canadian pharmacies not requiring prescription
best canadian online pharmacy Large Selection of Medications from Canada canadian pharmacy india
canadian 24 hour pharmacy
italian pharmacy online
https://canadaph24.pro/# legitimate canadian pharmacies
What a compelling enjoy reading! Your arguments were well-presented and convincing.
best mail order pharmacy canada
https://indiaph24.store/# cheapest online pharmacy india
lisinopril 10 mg tabs
canadian online pharmacy Licensed Canadian Pharmacy canadian pharmacy king
https://canadaph24.pro/# best canadian pharmacy to buy from
brand ketoconazole – buy lotrisone generic buy itraconazole 100mg generic
pill pharmacy
mexican mail order pharmacies cheapest mexico drugs mexican rx online
https://mexicoph24.life/# medicine in mexico pharmacies
prednisone brand name india
https://canadaph24.pro/# legitimate canadian mail order pharmacy
top 10 online pharmacy in india buy medicines from India indian pharmacy online
cheap canadian pharmacy
https://canadaph24.pro/# trustworthy canadian pharmacy
reputable indian pharmacies reputable indian pharmacies online pharmacy india
tadalafil online no rx
Thank you, I have recently been looking for info about this subject
for a while and yours is the greatest I have came upon till now.
However, what about the conclusion? Are you positive concerning the supply?
buy zestril online
Hey there I am so excited I found your blog page, I really found you by accident, while I was searching on Aol for something else, Regardless I
am here now and would just like to say cheers for a fantastic post and a all round thrilling
blog (I also love the theme/design), I don’t have time to
go through it all at the minute but I have bookmarked it and also added your RSS
feeds, so when I have time I will be back to read much more, Please do keep up the
excellent jo.
synthroid 0.025 mcg
http://indiaph24.store/# indian pharmacies safe
valtrex price without insurance
canadianpharmacymeds
synthroid 88 lowest cost
top 10 pharmacies in india Generic Medicine India to USA online shopping pharmacy india
synthroid 25 mg daily
http://indiaph24.store/# india pharmacy mail order
best canadian online pharmacy canadian pharmacies canadian pharmacy world
how do i get valtrex
https://canadaph24.pro/# canadian pharmacy world reviews
mexican mail order pharmacies Online Pharmacies in Mexico medication from mexico pharmacy
http://indiaph24.store/# best india pharmacy
Закажите SEO продвижение сайта https://seo116.ru/ в Яндекс и Google под ключ в Москве и по всей России от экспертов. Увеличение трафика, рост клиентов, онлайн поддержка. Комплексное продвижение сайтов с гарантией.
legitimate canadian online pharmacies
azithromycin
top online pharmacy india mail order pharmacy india reputable indian pharmacies
https://mexicoph24.life/# medication from mexico pharmacy
lisinopril 250mg
best online pharmacies in mexico Mexican Pharmacy Online buying prescription drugs in mexico online
http://canadaph24.pro/# canadian drug
chronometer watches
Understanding COSC Certification and Its Importance in Watchmaking
COSC Validation and its Rigorous Standards
Controle Officiel Suisse des Chronometres, or the Controle Officiel Suisse des Chronometres, is the authorized Swiss testing agency that certifies the accuracy and precision of wristwatches. COSC accreditation is a mark of excellent craftsmanship and trustworthiness in timekeeping. Not all timepiece brands follow COSC validation, such as Hublot, which instead sticks to its own demanding standards with mechanisms like the UNICO calibre, attaining similar accuracy.
The Science of Exact Chronometry
The central system of a mechanized watch involves the spring, which supplies energy as it loosens. This mechanism, however, can be susceptible to external elements that may impact its precision. COSC-certified movements undergo rigorous testing—over fifteen days in various conditions (5 positions, three temperatures)—to ensure their durability and dependability. The tests assess:
Average daily rate precision between -4 and +6 seconds.
Mean variation, peak variation rates, and effects of temperature changes.
Why COSC Accreditation Is Important
For timepiece fans and collectors, a COSC-accredited watch isn’t just a item of technology but a proof to lasting quality and accuracy. It signifies a watch that:
Offers outstanding reliability and accuracy.
Ensures assurance of superiority across the whole design of the watch.
Is apt to retain its worth more efficiently, making it a smart choice.
Popular Timepiece Manufacturers
Several famous manufacturers prioritize COSC accreditation for their watches, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, provides collections like the Record and Spirit, which highlight COSC-certified mechanisms equipped with innovative materials like silicone balance springs to boost durability and performance.
Historic Context and the Development of Chronometers
The idea of the timepiece originates back to the need for accurate chronometry for navigation at sea, emphasized by John Harrison’s work in the 18th cent. Since the official establishment of COSC in 1973, the accreditation has become a yardstick for judging the precision of luxury timepieces, maintaining a legacy of superiority in watchmaking.
Conclusion
Owning a COSC-validated timepiece is more than an visual choice; it’s a commitment to quality and accuracy. For those appreciating accuracy above all, the COSC certification offers peace of thoughts, guaranteeing that each certified watch will perform reliably under various conditions. Whether for individual contentment or as an investment, COSC-accredited watches distinguish themselves in the world of horology, bearing on a legacy of meticulous timekeeping.
pharmacy discount coupons
buy valtrex no prescription
http://indiaph24.store/# india pharmacy mail order
canadian pharmacy in canada Certified Canadian Pharmacies medication canadian pharmacy
https://indiaph24.store/# world pharmacy india
purple pharmacy mexico price list Mexican Pharmacy Online mexican rx online
Hi! Quick question that’s entirely off topic. Do you know how to make
your site mobile friendly? My web site looks weird when viewing from my iphone4.
I’m trying to find a theme or plugin that might be
able to correct this problem. If you have any suggestions, please share.
Thanks!
Hi, I do believe this is an excellent website. I stumbledupon it 😉 I will come back yet again since I bookmarked it.
Money and freedom is the greatest way to change, may you be rich and continue
to help others.
http://indiaph24.store/# reputable indian online pharmacy
synthroid price comparison
india pharmacy Cheapest online pharmacy top 10 pharmacies in india
metformin 500mg canada
azithromycin 750 mg
http://mexicoph24.life/# purple pharmacy mexico price list
medicine in mexico pharmacies cheapest mexico drugs mexican drugstore online
chronometer watches
Understanding COSC Certification and Its Importance in Horology
COSC Accreditation and its Demanding Criteria
Controle Officiel Suisse des Chronometres, or the Controle Officiel Suisse des Chronometres, is the official Swiss testing agency that attests to the accuracy and accuracy of wristwatches. COSC certification is a symbol of excellent craftsmanship and trustworthiness in timekeeping. Not all watch brands seek COSC certification, such as Hublot, which instead sticks to its own strict criteria with movements like the UNICO, achieving similar precision.
The Science of Exact Chronometry
The central system of a mechanized timepiece involves the mainspring, which supplies energy as it loosens. This system, however, can be susceptible to environmental factors that may affect its precision. COSC-certified movements undergo demanding testing—over 15 days in various circumstances (five positions, 3 temperatures)—to ensure their resilience and dependability. The tests assess:
Mean daily rate precision between -4 and +6 seconds.
Mean variation, highest variation rates, and effects of temperature changes.
Why COSC Certification Is Important
For timepiece enthusiasts and connoisseurs, a COSC-validated watch isn’t just a piece of tech but a demonstration to enduring excellence and accuracy. It symbolizes a watch that:
Provides outstanding reliability and precision.
Ensures confidence of quality across the entire design of the timepiece.
Is likely to hold its worth more effectively, making it a wise choice.
Famous Chronometer Brands
Several renowned manufacturers prioritize COSC certification for their timepieces, including Rolex, Omega, Breitling, and Longines, among others. Longines, for instance, offers collections like the Record and Spirit, which showcase COSC-accredited movements equipped with cutting-edge substances like silicon equilibrium suspensions to improve durability and performance.
Historic Context and the Development of Timepieces
The idea of the timepiece dates back to the requirement for exact chronometry for navigational at sea, highlighted by John Harrison’s work in the eighteenth cent. Since the official establishment of COSC in 1973, the validation has become a yardstick for evaluating the accuracy of luxury watches, sustaining a tradition of superiority in watchmaking.
Conclusion
Owning a COSC-accredited watch is more than an aesthetic choice; it’s a commitment to excellence and precision. For those valuing precision above all, the COSC certification provides tranquility of thoughts, ensuring that each accredited timepiece will operate reliably under various conditions. Whether for personal satisfaction or as an investment decision, COSC-validated watches stand out in the world of watchmaking, maintaining on a tradition of meticulous timekeeping.
https://indiaph24.store/# online pharmacy india
drugs from canada canadian pharmacies canadian valley pharmacy
best tadalafil tablets
order famciclovir 500mg sale – famvir 500mg price buy valaciclovir online cheap
ketoconazole pill – mentax cheap buy itraconazole 100mg without prescription
tadalafil india 10 mg
https://indiaph24.store/# reputable indian pharmacies
famciclovir cheap – acyclovir 400mg pills valaciclovir 500mg over the counter
prednisone 5052
線上賭場
india pharmacy mail order Cheapest online pharmacy best online pharmacy india
https://mexicoph24.life/# mexican mail order pharmacies
generic cialis online uk
http://indiaph24.store/# world pharmacy india
safe canadian pharmacies Certified Canadian Pharmacies cross border pharmacy canada
buysteriodsonline.com
Li Chaowen은 안도의 한숨을 쉬고 황제의 친절에 감사했습니다.
силиконовая девушка кукла цена
top 10 online pharmacy in india
112 mg synthroid
valtrex tablets 500mg price
order lanoxin 250 mg – buy avapro 300mg online cheap order furosemide 100mg sale
prednisone 60mg daily
zestril tablet
best price for synthroid 75 mcg
https://mexicoph24.life/# mexican drugstore online
synthroid 100 mcg india
buy real valtrex online
pharmacies in mexico that ship to usa mexican pharmacy mexican mail order pharmacies
valtrex 500mg
Son Dönemsel En Fazla Beğenilen Bahis Platformu: Casibom
Casino oyunlarını sevenlerin artık duymuş olduğu Casibom, son dönemde adından çoğunlukla söz ettiren bir şans ve kumarhane web sitesi haline geldi. Türkiye’nin en mükemmel casino sitelerinden biri olarak tanınan Casibom’un haftalık bazda cinsinden değişen giriş adresi, sektörde oldukça taze olmasına rağmen emin ve kazandıran bir platform olarak öne çıkıyor.
Casibom, muadillerini geride bırakarak uzun soluklu bahis platformların üstünlük sağlamayı başarılı oluyor. Bu sektörde eski olmak gereklidir olsa da, katılımcılarla iletişim kurmak ve onlara temasa geçmek da aynı derecede önemli. Bu noktada, Casibom’un 7/24 hizmet veren gerçek zamanlı destek ekibi ile rahatlıkla iletişime geçilebilir olması büyük önem taşıyan bir avantaj sunuyor.
Hızla genişleyen oyuncuların kitlesi ile ilgi çekici olan Casibom’un arkasındaki başarılı faktörleri arasında, yalnızca casino ve canlı olarak casino oyunlarıyla sınırlı olmayan geniş bir hizmet yelpazesi bulunuyor. Spor bahislerinde sunduğu geniş seçenekler ve yüksek oranlar, oyuncuları ilgisini çekmeyi başarmayı sürdürüyor.
Ayrıca, hem atletizm bahisleri hem de kumarhane oyunlar katılımcılara yönelik sunulan yüksek yüzdeli avantajlı ödüller da dikkat çekici. Bu nedenle, Casibom çabucak piyasada iyi bir reklam başarısı elde ediyor ve büyük bir katılımcı kitlesi kazanıyor.
Casibom’un kar getiren ödülleri ve popülerliği ile birlikte, siteye üyelik hangi yollarla sağlanır sorusuna da bahsetmek elzemdir. Casibom’a taşınabilir cihazlarınızdan, bilgisayarlarınızdan veya tabletlerinizden internet tarayıcı üzerinden kolayca ulaşılabilir. Ayrıca, web sitesinin mobil cihazlarla uyumlu olması da önemli bir artı sunuyor, çünkü artık hemen hemen herkesin bir akıllı telefonu var ve bu cihazlar üzerinden kolayca erişim sağlanabiliyor.
Mobil cihazlarınızla bile yolda gerçek zamanlı tahminler alabilir ve yarışmaları canlı olarak izleyebilirsiniz. Ayrıca, Casibom’un mobil uyumlu olması, ülkemizde kumarhane ve oyun gibi yerlerin yasal olarak kapatılmasıyla birlikte bu tür platformlara erişimin büyük bir yolunu oluşturuyor.
Casibom’un itimat edilir bir bahis platformu olması da önemlidir bir artı sunuyor. Belgeli bir platform olan Casibom, duraksız bir şekilde eğlence ve kazanç sağlama imkanı sağlar.
Casibom’a abone olmak da son derece rahatlatıcıdır. Herhangi bir belge gereksinimi olmadan ve bedel ödemeden siteye kolayca kullanıcı olabilirsiniz. Ayrıca, platform üzerinde para yatırma ve çekme işlemleri için de birçok farklı yöntem bulunmaktadır ve herhangi bir kesim ücreti isteseniz de alınmaz.
Ancak, Casibom’un güncel giriş adresini takip etmek de gereklidir. Çünkü gerçek zamanlı iddia ve casino platformlar moda olduğu için yalancı platformlar ve dolandırıcılar da belirmektedir. Bu nedenle, Casibom’un sosyal medya hesaplarını ve güncel giriş adresini düzenli aralıklarla kontrol etmek gereklidir.
Sonuç olarak, Casibom hem güvenilir hem de kar getiren bir bahis web sitesi olarak dikkat çekiyor. Yüksek ödülleri, geniş oyun seçenekleri ve kullanıcı dostu mobil uygulaması ile Casibom, oyun sevenler için mükemmel bir platform sağlar.
purchase glucophage
synthroid 25
lisinopril 10mg online
ciprofloxacin 500 mg tablet price: buy cipro online canada – buy ciprofloxacin
prednisone 60 mg daily
valtrex order uk
сайт vovan casino
http://ciprofloxacin.tech/# buy cipro online
вован казино
medicine prednisone 10mg
cost cheap propecia without prescription: buy propecia online – cost of propecia tablets
En Son Dönemin En Büyük Beğenilen Bahis Platformu: Casibom
Casino oyunlarını sevenlerin artık duymuş olduğu Casibom, nihai dönemde adından sıkça söz ettiren bir iddia ve kumarhane web sitesi haline geldi. Türkiye’nin en başarılı bahis web sitelerinden biri olarak tanınan Casibom’un haftalık bazda olarak değişen erişim adresi, piyasada oldukça yeni olmasına rağmen emin ve kazanç sağlayan bir platform olarak tanınıyor.
Casibom, muadillerini geride bırakarak köklü kumarhane platformların geride bırakmayı başarıyor. Bu sektörde eski olmak önemlidir olsa da, oyunculardan iletişimde bulunmak ve onlara temasa geçmek da benzer miktar önemli. Bu noktada, Casibom’un gece gündüz yardım veren canlı olarak destek ekibi ile kolayca iletişime geçilebilir olması büyük bir avantaj getiriyor.
Hızlıca genişleyen oyuncu kitlesi ile dikkat çekici Casibom’un gerisindeki başarım faktörleri arasında, sadece ve yalnızca bahis ve canlı olarak casino oyunları ile sınırlı olmayan kapsamlı bir hizmetler yelpazesi bulunuyor. Atletizm bahislerinde sunduğu geniş seçenekler ve yüksek oranlar, oyuncuları çekmeyi başarıyor.
Ayrıca, hem sporcular bahisleri hem de casino oyunları katılımcılara yönlendirilen sunulan yüksek yüzdeli avantajlı bonuslar da ilgi çekiyor. Bu nedenle, Casibom hızla sektörde iyi bir tanıtım başarısı elde ediyor ve önemli bir oyuncu kitlesi kazanıyor.
Casibom’un kazandıran ödülleri ve tanınırlığı ile birlikte, web sitesine üyelik ne şekilde sağlanır sorusuna da bahsetmek gereklidir. Casibom’a taşınabilir cihazlarınızdan, bilgisayarlarınızdan veya tabletlerinizden web tarayıcı üzerinden kolaylıkla erişilebilir. Ayrıca, web sitesinin mobil cihazlarla uyumlu olması da büyük bir artı getiriyor, çünkü artık pratikte herkesin bir cep telefonu var ve bu akıllı telefonlar üzerinden hızlıca giriş sağlanabiliyor.
Hareketli cihazlarınızla bile yolda gerçek zamanlı tahminler alabilir ve müsabakaları canlı olarak izleyebilirsiniz. Ayrıca, Casibom’un mobil uyumlu olması, ülkemizde kumarhane ve oyun gibi yerlerin kanuni olarak kapatılmasıyla birlikte bu tür platformlara erişimin büyük bir yolunu oluşturuyor.
Casibom’un itimat edilir bir casino web sitesi olması da önemlidir bir artı sunuyor. Lisanslı bir platform olan Casibom, sürekli bir şekilde eğlence ve kazanç elde etme imkanı sağlar.
Casibom’a abone olmak da son derece kolaydır. Herhangi bir belge şartı olmadan ve ücret ödemeden web sitesine kolaylıkla üye olabilirsiniz. Ayrıca, site üzerinde para yatırma ve çekme işlemleri için de çok sayıda farklı yöntem mevcuttur ve herhangi bir kesim ücreti isteseniz de alınmaz.
Ancak, Casibom’un güncel giriş adresini takip etmek de önemlidir. Çünkü canlı bahis ve kumarhane siteleri popüler olduğu için sahte platformlar ve dolandırıcılar da görünmektedir. Bu nedenle, Casibom’un sosyal medya hesaplarını ve güncel giriş adresini periyodik olarak kontrol etmek elzemdir.
Sonuç, Casibom hem emin hem de kar getiren bir bahis sitesi olarak dikkat çekiyor. Yüksek promosyonları, kapsamlı oyun seçenekleri ve kullanıcı dostu mobil uygulaması ile Casibom, casino hayranları için ideal bir platform sağlar.
lisinopril coupon price of lisinopril 20 mg lisinopril 20 mg canada
Какие радиаторы выбрать для отопления https://propest.ru/kak-vybrat-radiator-dlya-doma.html частного загородного дома – каменного или деревянного: разновидности и классы, правила выбора, цены, сравнения.
60 mg prednisone daily
synthroid buy online
На сайте коллегии юристов http://zpp-1.ru/ вы найдете контакты и сможете связаться с адвокатами. Юрист расскажет о том, как нужно правильно поступить, поможет собрать необходимые документы и будет защищать ваши права в суде. Квалифицированная юридическая и медицинская поддержка призывникам с гарантией!
ciprofloxacin generic price cipro pharmacy buy cipro cheap
http://lisinopril.network/# lisinopril 40 mg pill
https://ciprofloxacin.tech/# cipro ciprofloxacin
cipro for sale: cipro online no prescription in the usa – cipro online no prescription in the usa
synthroid india
10배스탁론
로드스탁과의 레버리지 방식의 스탁: 투자 전략의 참신한 분야
로드스탁에서 제공되는 레버리지 스탁은 주식 시장의 투자법의 한 방식으로, 상당한 수익률을 목표로 하는 투자자들에게 매력적인 옵션입니다. 레버리지를 이용하는 이 방법은 투자자가 자신의 자본을 넘어서는 투자금을 투자할 수 있도록 함으로써, 증권 장에서 더욱 큰 힘을 가질 수 있는 기회를 제공합니다.
레버리지 방식의 스탁의 원리
레버리지 방식의 스탁은 원칙적으로 투자금을 빌려 사용하는 방식입니다. 예시를 들어, 100만 원의 자본으로 1,000만 원 상당의 주식을 취득할 수 있는데, 이는 투자자들이 기본 투자 금액보다 훨씬 훨씬 더 많은 주식을 취득하여, 주식 가격이 상승할 경우 상응하는 더욱 큰 이익을 획득할 수 있게 됩니다. 하지만, 증권 값이 하락할 경우에는 그 손실 또한 커질 수 있으므로, 레버리지를 이용할 때는 신중하게 생각해야 합니다.
투자 전략과 레버리지 사용
레버리지 사용은 특히 성장 잠재력이 상당한 기업에 적용할 때 효과적입니다. 이러한 사업체에 높은 비율로 적용하면, 성공적일 경우 큰 수입을 획득할 수 있지만, 반대의 경우 많은 위험도 감수해야. 그렇기 때문에, 투자자들은 자신의 리스크 관리 능력을 가진 장터 분석을 통해 통해, 일정한 기업에 얼마만큼의 자금을 투입할지 결정하게 됩니다 합니다.
레버리지의 이점과 위험 요소
레버리지 방식의 스탁은 상당한 이익을 제공하지만, 그만큼 높은 위험도 수반합니다. 증권 시장의 변화는 예상이 곤란하기 때문에, 레버리지를 사용할 때는 항상 시장 경향을 면밀히 주시하고, 손해를 최소화할 수 있는 전략을 구성해야 합니다.
최종적으로: 세심한 선택이 필수입니다
로드스탁을 통해 제공하는 레버리지 스탁은 막강한 투자 수단이며, 적당히 사용하면 많은 이익을 가져다줄 수 있습니다. 그렇지만 큰 위험도 생각해 봐야 하며, 투자 결정이 필요한 정보와 세심한 고려 후에 이루어져야 합니다. 투자하는 사람의 금융 상황, 리스크 감수 능력, 그리고 시장의 상황을 반영한 안정된 투자 방법이 핵심입니다.
metformin 500 mg price south africa
nolvadex steroids tamoxifen therapy tamoxifen lawsuit
https://nolvadex.life/# tamoxifen rash pictures
prednisone tablet 100 mg
cost of propecia tablets: cost of cheap propecia now – get generic propecia tablets
prednisone 7.5 mg
what is tamoxifen used for common side effects of tamoxifen nolvadex gynecomastia
로드스탁과 레버리지 방식의 스탁: 투자 전략의 새로운 분야
로드스탁을 통해 공급하는 레버리지 스탁은 주식 투자의 한 방식으로, 큰 이익율을 목표로 하는 투자자들에게 매혹적인 선택입니다. 레버리지 사용을 이용하는 이 전략은 투자자들이 자신의 자금을 넘어서는 금액을 투입할 수 있도록 함으로써, 증권 장에서 더욱 큰 영향력을 가질 수 있는 기회를 줍니다.
레버리지 방식의 스탁의 원리
레버리지 방식의 스탁은 일반적으로 자금을 차입하여 사용하는 방식입니다. 예를 들어, 100만 원의 자금으로 1,000만 원 상당의 증권을 사들일 수 있는데, 이는 투자자들이 기본적인 자본보다 훨씬 더욱 많은 주식을 사들여, 주식 가격이 상승할 경우 해당하는 더 큰 수익을 가져올 수 있게 합니다. 그렇지만, 증권 값이 내려갈 경우에는 그 손실 또한 증가할 수 있으므로, 레버리지 사용을 이용할 때는 신중해야 합니다.
투자 전략과 레버리지
레버리지 사용은 특히 성장 잠재력이 높은 사업체에 투자할 때 도움이 됩니다. 이러한 사업체에 높은 비율로 투입하면, 성공적일 경우 막대한 수익을 얻을 수 있지만, 그 반대의 경우 상당한 위험성도 짊어져야 합니다. 그러므로, 투자하는 사람은 자신의 리스크 관리 능력과 시장 분석을 통해, 일정한 기업에 얼마만큼의 자본을 투입할지 결정해야 합니다.
레버리지 사용의 장점과 위험 요소
레버리지 스탁은 큰 수익을 보장하지만, 그만큼 큰 위험도 동반합니다. 증권 시장의 변화는 예측이 어렵기 때문에, 레버리지를 이용할 때는 언제나 시장 동향을 정밀하게 살펴보고, 손해를 최소화하기 위해 수 있는 전략을 세워야 합니다.
최종적으로: 세심한 선택이 필요
로드스탁에서 제공된 레버리지 방식의 스탁은 효과적인 투자 수단이며, 잘 이용하면 많은 수입을 가져다줄 수 있습니다. 그러나 상당한 위험성도 생각해 봐야 하며, 투자 결정이 충분히 많은 사실과 조심스러운 고려 후에 진행되어야 합니다. 투자자 본인의 재정적 상태, 위험 수용 능력, 그리고 시장 상황을 반영한 안정된 투자 전략이 핵심입니다.
prednisone 50 tablet
tadalafil in canada
Организация свадьбы под ключ https://yagodawedding.ru/ с гарантией. Быстрый расчет сметы, работаем с любым бюджетом. Берём на себя абсолютно все свадебные хлопоты. Организуем одни из самых красивых свадебных и семейных событий.
buy lanoxin paypal – oral irbesartan buy furosemide 100mg pill
https://lisinopril.network/# zestril 2.5 mg
http://ciprofloxacin.tech/# buy cipro online canada
synthroid 25 mcg tablet
antibiotics cipro: purchase cipro – buy cipro online
canadian family pharmacy
order synthroid without prescription
where to get nolvadex nolvadex gynecomastia tamoxifen menopause
pharmacy rx world canada
best price for synthroid
http://finasteride.store/# cost cheap propecia tablets
buy hydrochlorothiazide 25 mg without prescription – order norvasc 10mg generic zebeta 5mg uk
SEO раскрутка сайта в топ https://seositejob.ru/ Яндекс и Google от профессионалов.
buy metformin 1000 mg online
lisinopril 20 mg purchase
cost of propecia without prescription: buy propecia for sale – order generic propecia pill
buying generic propecia without rx get propecia tablets buying propecia price
levothyroxine ordering online
where can i buy synthroid online
can i buy tadalafil in canada
buy valtrex without prescription
https://ciprofloxacin.tech/# cipro online no prescription in the usa
Backlinks seo
Productive Links in Weblogs and Comments: Increase Your SEO
Hyperlinks are crucial for improving search engine rankings and increasing web site visibility. By integrating links into blogs and comments smartly, they can significantly boost traffic and SEO efficiency.
Adhering to Search Engine Algorithms
The current day’s backlink placement methods are meticulously tuned to align with search engine algorithms, which now emphasize link good quality and relevance. This assures that hyperlinks are not just numerous but significant, directing users to helpful and pertinent content material. Website owners should emphasis on integrating hyperlinks that are contextually appropriate and boost the overall content quality.
Benefits of Using Refreshing Donor Bases
Making use of current donor bases for backlinks, like those maintained by Alex, offers considerable rewards. These bases are frequently refreshed and consist of unmoderated sites that don’t pull in complaints, guaranteeing the hyperlinks put are both powerful and agreeable. This approach will help in keeping the effectiveness of links without the pitfalls connected with moderated or troublesome sources.
Only Authorized Sources
All donor sites used are sanctioned, avoiding legal pitfalls and conforming to digital marketing criteria. This dedication to utilizing only approved resources guarantees that each backlink is legitimate and reliable, thereby developing credibility and reliability in your digital presence.
SEO Influence
Skillfully put backlinks in blogs and comments provide over just SEO rewards—they improve user encounter by linking to relevant and top quality content. This technique not only meets search engine criteria but also engages consumers, leading to far better visitors and improved online engagement.
In essence, the right backlink technique, especially one that employs clean and dependable donor bases like Alex’s, can change your SEO efforts. By focusing on quality over quantity and adhering to the latest requirements, you can ensure your backlinks are both potent and productive.
ciprofloxacin generic purchase cipro buy ciprofloxacin over the counter
lisinopril 40: lisinopril tabs 4mg – over the counter lisinopril
http://ciprofloxacin.tech/# buy ciprofloxacin
tadalafil canada
tadalafil 20mg canada
order valtrex canada
metoprolol drug – order telmisartan 20mg generic nifedipine order
buy lopressor pill – buy losartan 25mg pill buy nifedipine generic
nolvadex half life nolvadex online how does tamoxifen work
https://lisinopril.network/# buy lisinopril 20 mg online
tamoxifen moa: nolvadex pills – tamoxifen for sale
Привет любители отдыха!
Открыть для себя Калининград и его окрестности – это увлекательное путешествие, наполненное историческими достопримечательностями, культурным наследием и потрясающими пейзажами. Вместе с нашей командой частных гидов и автомобилей вы сможете насладиться уникальным опытом индивидуальных экскурсий. Наша главная задача – создать для вас максимально комфортные условия и удовлетворить все ваши пожелания и интересы. Каждый из наших специалистов – аккредитованный экскурсовод с богатым опытом работы в сфере туризма. Мы гордимся тем, что можем предложить вам не только стандартные маршруты, но и создать эксклюзивные программы, адаптированные под ваши запросы и временные рамки. Благодаря индивидуальному подходу вы сможете увидеть не только известные достопримечательности, но и скрытые уголки Калининграда и его области, которые не описаны в туристических брошюрах. Мы уверены, что наши экскурсии станут для вас незабываемым опытом, полным открытий и впечатлений. Хотите узнать больше о наших услугах и забронировать экскурсию? Посетите наш сайт по ссылке https://topkaliningrad.ru и начните свое приключение с нами!
Калининград экскурсия по городу
частные гиды по Калининградской области
экскурсии из Калининграда на Куршскую косу индивидуальные
гиды Калининград
экскурсии из Калининграда
ночная экскурсия по Калининграду
Удачи и хорошего визита в Калининград!
Kantorbola situs slot online terbaik 2024 , segera daftar di situs kantor bola dan dapatkan promo terbaik bonus deposit harian 100 ribu , bonus rollingan 1% dan bonus cashback mingguan . Kunjungi juga link alternatif kami di kantorbola77 , kantorbola88 dan kantorbola99
Backlinks seo
Potent Backlinks in Blogs and forums and Remarks: Increase Your SEO
Backlinks are critical for boosting search engine rankings and boosting web site presence. By integrating hyperlinks into weblogs and comments smartly, they can significantly increase visitors and SEO efficiency.
Adhering to Search Engine Algorithms
The current day’s backlink positioning methods are meticulously tuned to line up with search engine algorithms, which now prioritize website link high quality and relevance. This assures that backlinks are not just numerous but meaningful, guiding users to helpful and pertinent content material. Website owners should emphasis on integrating backlinks that are contextually proper and improve the overall articles high quality.
Benefits of Utilizing Fresh Donor Bases
Using up-to-date donor bases for backlinks, like those maintained by Alex, delivers substantial advantages. These bases are regularly renewed and consist of unmoderated websites that don’t attract complaints, making sure the links placed are both powerful and compliant. This strategy will help in keeping the effectiveness of hyperlinks without the pitfalls linked with moderated or troublesome assets.
Only Sanctioned Sources
All donor sites used are sanctioned, keeping away from legal pitfalls and conforming to digital marketing requirements. This determination to making use of only approved resources assures that each backlink is legitimate and trustworthy, thereby building credibility and reliability in your digital presence.
SEO Influence
Skillfully positioned backlinks in weblogs and comments provide over just SEO benefits—they improve user experience by connecting to pertinent and high-quality content. This strategy not only fulfills search engine criteria but also entails end users, leading to far better targeted traffic and improved online proposal.
In essence, the right backlink technique, particularly one that utilizes fresh and dependable donor bases like Alex’s, can transform your SEO efforts. By focusing on quality over volume and sticking to the latest criteria, you can ensure your backlinks are both powerful and productive.
tamoxifen moa tamoxifen depression tamoxifen warning
http://cytotec.club/# Misoprostol 200 mg buy online
проверить свои usdt на чистоту
Проверка данных бумажников за присутствие нелегальных средств передвижения: Защита вашего криптовалютного портфельчика
В мире цифровых валют становится все более необходимее соблюдать безопасность своих денег. Регулярно обманщики и киберпреступники разрабатывают свежие методы обмана и мошенничества и воровства виртуальных финансов. Один из важных методов обеспечения является проверка данных бумажников на выявление незаконных финансовых средств.
Почему поэтому важно проверить свои цифровые бумажники?
Прежде всего, вот этот момент важно для того, чтобы защиты личных финансов. Большинство инвесторы рискуют потери средств своих финансов по причине несправедливых подходов или воровства. Проверка данных кошельков способствует предотвращению обнаружить в нужный момент непонятные операции и предупредить.
Что предлагает фирма?
Мы предлагаем услугу анализа цифровых кошельков и транзакций с намерением обнаружения источника средств передвижения и выдачи детального доклада. Наша система анализирует информацию для идентификации подозрительных действий и оценить риск для того, чтобы вашего криптовалютного портфеля. Благодаря нашей службе проверки, вы можете предотвратить возможные проблемы с органами контроля и обезопасить себя от случайного участия в нелегальных операций.
Как проводится проверка?
Компания наша фирма сотрудничает с крупными аудиторскими организациями, вроде Halborn, для того чтобы гарантировать и точность наших проверок данных. Мы используем передовые и методы анализа данных для выявления опасных манипуляций. Данные пользователей наших заказчиков обрабатываются и хранятся в базе согласно высокими стандартами.
Основная просьба: “проверить свои USDT на чистоту”
В случае если вы хотите убедиться надежности ваших кошельков USDT, наша компания оказывает шанс бесплатную проверку первых пяти кошельков. Просто введите свой кошелек в указанное место на нашем сайте, и мы предоставим вам подробные сведения о состоянии вашего кошелька.
Защитите свои активы сразу же!
Не подвергайте себя риску попасть жертвой злоумышленников или оказаться неприятной ситуации подозрительных операций с вашими финансами. Обратитесь к специалистам, которые окажут помощь, вам и вашим финансам защитить свои криптовалютные средства и предотвратить возможные. Сделайте первый шаг к безопасности безопасности своего электронного портфеля активов в данный момент!
The Writing has become a go-to resource for me. The effort you put into The posts is truly appreciated.
Misoprostol 200 mg buy online: buy cytotec pills online cheap – cytotec buy online usa
where can i buy valtrex over the counter
azithromycin tablets otc
online pharmacy no prescription needed
Every article you write is like a new adventure. I’m always excited to see where you’ll take me next.
https://nolvadex.life/# tamoxifen
Осмотр Tether на нетронутость: Каким образом обезопасить свои цифровые финансы
Все более пользователей обращают внимание к секурити своих цифровых активов. Постоянно шарлатаны изобретают новые подходы кражи криптовалютных активов, и также держатели электронной валюты становятся жертвами их афер. Один техник защиты становится проверка кошельков в присутствие незаконных финансов.
С каким намерением это важно?
В первую очередь, для того чтобы обезопасить собственные активы от обманщиков или украденных монет. Многие вкладчики сталкиваются с потенциальной угрозой убытков своих фондов вследствие мошеннических механизмов или кражей. Проверка кошельков помогает выявить непрозрачные операции и предотвратить потенциальные убытки.
Что мы предлагаем?
Мы предоставляем услугу тестирования криптовалютных бумажников или операций для обнаружения источника фондов. Наша система исследует информацию для выявления противозаконных операций и также оценки риска для вашего счета. Вследствие этой проверке, вы сможете избежать проблем с регуляторами или обезопасить себя от участия в незаконных операциях.
Как это действует?
Мы сотрудничаем с первоклассными аудиторскими компаниями, вроде Kudelsky Security, чтобы предоставить точность наших проверок. Мы используем новейшие технологии для обнаружения рискованных операций. Ваши данные обрабатываются и сохраняются в соответствии с высокими стандартами безопасности и конфиденциальности.
Как выявить свои USDT в чистоту?
Если вам нужно подтвердить, что ваши USDT-кошельки чисты, наш сервис предоставляет бесплатное тестирование первых пяти кошельков. Просто передайте адрес своего кошелька на на сайте, и наша команда предоставим вам детальный отчет о его положении.
Охраняйте свои средства уже сейчас!
Не подвергайте риску подвергнуться дельцов или оказаться в неприятную обстановку по причине нелегальных операций. Обратитесь к нашему агентству, с тем чтобы обезопасить ваши криптовалютные финансовые ресурсы и избежать проблем. Совершите первый шаг к сохранности вашего криптовалютного портфеля уже сегодня!
discount zestril
purchase cipro cipro for sale buy cipro online without prescription
Анализ Tether для нетронутость: Каким образом обезопасить свои цифровые финансы
Все более индивидуумов обращают внимание для надежность их криптовалютных активов. Постоянно обманщики разрабатывают новые методы хищения электронных средств, и также владельцы криптовалюты оказываются жертвами их интриг. Один техник сбережения становится проверка кошельков для наличие незаконных денег.
Для чего это необходимо?
Прежде всего, для того чтобы обезопасить собственные финансы от мошенников и украденных монет. Многие инвесторы сталкиваются с потенциальной угрозой потери их активов вследствие обманных схем или краж. Тестирование кошельков помогает определить подозрительные действия и предотвратить возможные потери.
Что мы предоставляем?
Мы предоставляем услугу тестирования криптовалютных бумажников и операций для выявления источника средств. Наша система исследует данные для выявления противозаконных операций и также проценки опасности для вашего портфеля. Вследствие такой проверке, вы сможете избежать проблем с регулированием а также защитить себя от участия в нелегальных операциях.
Как это работает?
Мы сотрудничаем с лучшими аудиторскими организациями, наподобие Cure53, для того чтобы обеспечить точность наших проверок. Наша команда применяем новейшие технологии для определения рискованных транзакций. Ваши данные обрабатываются и сохраняются согласно с высокими нормами безопасности и конфиденциальности.
Как проверить личные Tether в нетронутость?
При наличии желания убедиться, что ваша USDT-бумажники чисты, наш подход обеспечивает бесплатную проверку первых пяти бумажников. Просто передайте положение личного бумажника на нашем сайте, и наша команда предложим вам детальный отчет о его положении.
Обезопасьте вашими активы прямо сейчас!
Не подвергайте риску подвергнуться мошенников либо попасть в неблагоприятную ситуацию из-за нелегальных операций. Обратитесь к нашему сервису, с тем чтобы обезопасить ваши электронные активы и избежать сложностей. Примите первый шаг к сохранности вашего криптовалютного портфеля уже сейчас!
kantorbola
Situs kantor bola merupakan penyedia permainan slot online gacor dengan RTP 98% , mainkan game slot online mudah menang di situs kantorbola . tersedia fitur deposit kilat menggunakan QRIS Kantorbola .
Проверка данных кошельков для хранения криптовалюты на присутствие нелегальных средств передвижения: Защита вашего цифрового финансового портфеля
В мире криптовалют становится все значимее необходимее обеспечивать защиту своих финансов. Ежедневно жулики и криминальные элементы создают новые методы обмана и мошенничества и воровства электронных денег. Одним из важных инструментов обеспечения безопасности становится анализ кошельков для хранения криптовалюты на выявление незаконных средств.
По какой причине так важно и проверить личные криптовалютные бумажники?
В первую очередь, вот данный факт необходимо для того, чтобы защиты собственных финансовых средств. Многие из пользователи рискуют потери средств их финансовых средств вследствие несправедливых планов или воровства. Анализ кошелька способствует предотвращению выявить вовремя непонятные операции и предотвратить возможные.
Что предоставляет организация?
Мы предлагаем вам сервис проверки проверки цифровых кошельков для хранения криптовалюты и транзакций средств с целью обнаружения источника финансовых средств и предоставления детального отчета. Фирма предоставляет программа проверяет информацию для идентификации незаконных операций средств и оценить риск для того чтобы вашего финансового портфеля. Благодаря нашей проверке, вы будете способны предотвратить с регуляторными органами и обезопасить себя от случайной вовлеченности в незаконных операций.
Как проводится проверка?
Наша фирма взаимодействует с авторитетными аудиторскими агентствами, например Halborn, с тем чтобы обеспечить гарантированность и точность наших проверок данных. Мы используем современные технологии и методы анализа для обнаружения опасных действий. Личные данные наших пользователей обрабатываются и хранятся в специальной базе данных в соответствии высокими стандартами безопасности и конфиденциальности.
Основная просьба: “проверить свои USDT на чистоту”
В случае если вы хотите убедиться безопасности личных кошельков USDT, наша компания предлагает возможность исследовать бесплатную проверку наших специалистов первых пяти кошельков. Просто введите свой кошелек в указанное место на нашем онлайн-ресурсе, и мы передадим вам подробную информацию о состоянии вашего кошелька.
Обеспечьте безопасность своих деньги сразу же!
Предотвращайте риски оказаться в пострадать от хакеров или оказаться в неприятной ситуации из-за подозрительных операций средств с ваших средствами. Дайте вашу криптовалюту экспертам, которые смогут помочь, вам защититься криптовалютные средства и избежать. Сделайте первый шаг к безопасности безопасности своего цифрового портфеля активов в данный момент!
The posts inspire me regularly. The depth you bring to The topics is truly exceptional.
доставка цветов
http://finasteride.store/# get propecia tablets
no prescription synthroid
online pharmacy no prescription needed
safe reliable canadian pharmacy
Компания КЗТО https://radiators-teplo.github.io/ известна производством высококачественных радиаторов, которые обеспечивают эффективное отопление и долговечность. Продукция КЗТО включает радиаторы различных модификаций, подходящие для любых помещений. Они изготавливаются из прочных материалов, что гарантирует устойчивость к коррозии и высокую теплоотдачу.
cytotec pills online: buy cytotec pills – Misoprostol 200 mg buy online
best tadalafil tablet
levitra pills cheap
canadian pharmacy azithromycin buy online
ciprofloxacin order online purchase cipro ciprofloxacin generic
apo prednisone
проверить свои usdt на чистоту
Проверка кошельков кошелька за присутствие нелегальных финансовых средств: Защита вашего электронного активов
В мире цифровых валют становится все более существеннее соблюдать безопасность своих финансовых активов. Ежедневно мошенники и криминальные элементы выработывают новые схемы обмана и мошенничества и воровства цифровых финансов. Ключевым инструментом основных способов обеспечения безопасности является проверка кошельков бумажников за присутствие незаконных средств передвижения.
По какой причине так важно провести проверку личные цифровые кошельки для хранения электронных денег?
В первую очередь, вот это обстоятельство обязательно для того чтобы защиты собственных средств. Многие участники рынка рискуют потерять потери денег их средств вследствие несправедливых схем или воровства. Анализ кошелька способствует предотвращению обнаружить в нужный момент сомнительные операции и предотвратить возможные.
Что предоставляет фирма?
Мы предлагаем вам услугу проверки данных электронных кошельков для хранения криптовалюты и транзакций средств с задачей идентификации начала финансовых средств и дать полного доклада. Наша платформа проверяет информацию для идентификации подозрительных действий и определить уровень риска для того, чтобы вашего портфеля активов. Благодаря нашей системе проверки, вы можете избежать с регуляторными органами и обезопасить себя от случайной вовлеченности в нелегальных операций.
Как осуществляется процесс?
Компания наша фирма-разработчик взаимодействует с ведущими аудиторами организациями, как например Halborn, чтобы обеспечить гарантированность и правильность наших проверок данных. Мы применяем современные технологии и методики анализа данных для идентификации опасных действий. Персональные данные наших пользователей обрабатываются и хранятся в специальной базе данных в соответствии с положениями высокими стандартами безопасности.
Ключевой запрос: “проверить свои USDT на чистоту”
В случае если вы хотите проверить чистоте своих USDT кошельков, наши профессионалы предоставляет возможность провести бесплатной проверки первых 5 кошельков. Просто свой кошелек в указанное место на нашем сайте, и мы предоставим вам подробную информацию о его статусе.
Обеспечьте защиту своих активы прямо сейчас!
Не рискуйте попасть пострадать злоумышленников или оказаться в неприятной ситуации неправомерных операций средств с вашими финансами. Дайте вашу криптовалюту экспертам, которые окажут помощь, вам защититься криптовалютные активы и предотвратить возможные проблемы. Совершите первый шаг к обеспечению безопасности защите вашего электронного портфеля активов уже сегодня!
lisinopril prescription coupon
microzide 25 mg over the counter – generic amlodipine 10mg bisoprolol 10mg tablet
You present hard to understand topics in a clear and engaging way, as if inviting me on an adventure of the mind.
радиаторы отопления какой выбрать в дом частный
buying metformin online
https://propest.ru/kak-vybrat-radiator-dlya-doma.html
https://nolvadex.life/# buy nolvadex online
tadalafil 20mg india
Unique perspective? Check. Making me rethink my life choices? Double-check.
чистый ли usdt
Осмотр USDT для нетронутость: Каким образом сохранить свои криптовалютные финансы
Все более граждан обращают внимание к секурити личных цифровых средств. Каждый день шарлатаны придумывают новые схемы разграбления цифровых средств, или владельцы электронной валюты оказываются жертвами их подстав. Один из техник сбережения становится проверка кошельков на присутствие нелегальных денег.
Зачем это необходимо?
Прежде всего, для того чтобы защитить свои средства от дельцов и украденных денег. Многие вкладчики сталкиваются с риском убытков личных активов в результате обманных планов или краж. Тестирование кошельков способствует обнаружить подозрительные транзакции или предотвратить возможные убытки.
Что наша команда предлагаем?
Наша компания предоставляем сервис тестирования цифровых кошельков и операций для определения источника средств. Наша платформа анализирует информацию для определения противозаконных действий и также оценки риска для вашего портфеля. За счет этой проверке, вы сможете избегнуть недочетов с регуляторами или защитить себя от участия в незаконных операциях.
Каким образом это работает?
Наша команда работаем с ведущими аудиторскими компаниями, наподобие Kudelsky Security, для того чтобы обеспечить точность наших проверок. Мы применяем новейшие техники для определения опасных транзакций. Ваши данные обрабатываются и сохраняются согласно с высокими нормами безопасности и конфиденциальности.
Каким образом проверить личные USDT для чистоту?
Если хотите проверить, что ваша USDT-кошельки чисты, наш сервис предлагает бесплатное тестирование первых пяти бумажников. Просто введите адрес вашего кошелька на на сайте, или наш сервис предоставим вам детальный доклад о его статусе.
Гарантируйте безопасность для вашими активы уже сейчас!
Не рискуйте подвергнуться мошенников либо оказаться в неприятную обстановку по причине незаконных операций. Обратитесь к нашей команде, с тем чтобы сохранить свои электронные активы и предотвратить неприятностей. Совершите первый шаг к безопасности вашего криптовалютного портфеля уже сегодня!
happy family store pharmacy
На этом сайте https://www.rabota-zarabotok.ru/ вы найдете полезную информацию, и отзывы о разных финансовых сайтах. Здесь очень много полезной информации, и разоблачение мошенников. А также узнайте где начать зарабатывать первые деньги в интернете.
Здравствуйте!
Отправляясь в путешествие по Калининграду и его окрестностям, каждый ищет что-то уникальное и незабываемое. И здесь на помощь приходят индивидуальные экскурсии от нашей команды частных гидов с автомобилями. Мы предлагаем не просто обзорные экскурсии, а настоящее погружение в атмосферу этого удивительного региона. Каждый наш специалист – аккредитованный гид с глубоким знанием истории, культуры и достопримечательностей Калининграда и его области. Благодаря индивидуальному подходу мы создаем маршруты, учитывая интересы и предпочтения каждого клиента. Это позволяет раскрыть всю красоту и многообразие этого уникального региона. Мы предлагаем не только осмотр достопримечательностей, но и возможность познакомиться с местными обычаями и традициями. Наши экскурсии – это не просто прогулка, а настоящее путешествие в историю и культуру Калининградской области. Большой плюс наших туров в том, что мы предлагаем комфортные условия передвижения на автомобиле, что особенно важно при посещении удаленных достопримечательностей. Кроме того, наши гиды всегда готовы ответить на любые вопросы и поделиться интересными фактами о местах, которые мы посещаем. Проведение экскурсий с нами – это уникальная возможность увидеть Калининград и его окрестности глазами настоящих знатоков. Для более подробной информации о наших услугах и возможностях ознакомиться с нашими экскурсиями, пожалуйста, посетите наш сайт по ссылке: https://topkaliningrad.ru
частные гиды по Калининградской области
гид по Калининграду с машиной
экскурсии по Калининграду и Калининградской области индивидуальные
частный гид Калининград
гиды Калининграда индивидуальные экскурсии
ночная экскурсия по Калининграду
Удачи и хорошего визита в Калининград!
zestril 40: zestoretic 10 12.5 – how to buy lisinopril online
how to order cialis online safely
USDT – является неизменная криптовалютный актив, привязанная к валюте страны, подобно USD. Это позволяет данную криптовалюту в особенности привлекательной среди инвесторов, поскольку данный актив предлагает устойчивость цены в условиях неустойчивости рынка цифровых активов. Однако, подобно другая разновидность криптовалюты, USDT изложена риску использования для легализации доходов и поддержки незаконных сделок.
Отмывание денег путем цифровые валюты превращается все больше и больше обычным путем с целью скрытия происхождения средств. Используя различные техники, дельцы могут попытаться отмывать незаконно полученные фонды путем обменники криптовалют или миксеры средств, для того чтобы сделать происхождение менее очевидным.
Именно поэтому, анализ USDT на чистоту оказывается весьма важной инструментом предостережения для участников криптовалют. Доступны для использования специализированные сервисы, какие проводят проверку транзакций и кошельков, для того чтобы идентифицировать подозрительные сделки и незаконные источники капитала. Эти сервисы помогают владельцам устранить непреднамеренного вовлечения в преступной деятельности и предотвратить блокировку счетов со со стороны сторонних надзорных органов.
Экспертиза USDT на чистоту также как предотвращает предохранить себя от возможных убытков. Участники могут быть уверены в том, что их активы не ассоциированы с нелегальными транзакциями, что соответственно уменьшает вероятность блокировки счета или перечисления денег.
Таким образом, в условиях современности растущей сложности среды криптовалют важно принимать действия для обеспечения безопасности своего капитала. Экспертиза USDT на чистоту при помощи специальных платформ является одним из вариантов предотвращения финансирования преступной деятельности, обеспечивая пользователям цифровых валют дополнительную степень и защиты.
generic propecia without insurance buy propecia without rx get generic propecia without insurance
Проверка USDT на чистоту
Тестирование Тетер в чистоту: Каким образом защитить свои электронные средства
Каждый день все больше пользователей обращают внимание для надежность своих электронных средств. Каждый день обманщики изобретают новые методы кражи электронных средств, или владельцы криптовалюты оказываются пострадавшими своих интриг. Один из подходов обеспечения безопасности становится тестирование кошельков в присутствие противозаконных финансов.
Для чего это полезно?
Преимущественно, чтобы сохранить личные средства от шарлатанов или украденных монет. Многие участники сталкиваются с потенциальной угрозой потери своих фондов вследствие мошеннических механизмов или хищений. Проверка кошельков позволяет обнаружить сомнительные транзакции или предотвратить потенциальные убытки.
Что мы предлагаем?
Мы предоставляем услугу анализа электронных бумажников или транзакций для обнаружения происхождения денег. Наша платформа анализирует данные для выявления незаконных операций и оценки опасности для вашего портфеля. Вследствие этой проверке, вы сможете избегнуть проблем с регулированием или защитить себя от участия в незаконных операциях.
Как это действует?
Наша команда работаем с первоклассными аудиторскими организациями, например Halborn, для того чтобы обеспечить прецизионность наших проверок. Мы внедряем современные технологии для обнаружения рискованных сделок. Ваши данные проходят обработку и хранятся в соответствии с высокими нормами безопасности и конфиденциальности.
Как проверить свои USDT в чистоту?
Если вам нужно проверить, что ваша USDT-бумажники прозрачны, наш сервис предоставляет бесплатное тестирование первых пяти кошельков. Легко введите адрес собственного кошелька на на нашем веб-сайте, а также наш сервис предоставим вам детальный доклад о его статусе.
Охраняйте вашими активы уже сегодня!
Не подвергайте риску подвергнуться мошенников или оказаться в неприятную ситуацию по причине незаконных транзакций. Посетите нашему сервису, чтобы сохранить ваши цифровые финансовые ресурсы и предотвратить сложностей. Сделайте первый шаг к безопасности криптовалютного портфеля уже сейчас!
online pharmacy delivery
The post has broadened my perspective in ways I didn’t expect. Thank you for that.
nitroglycerin over the counter – how to get lozol without a prescription valsartan 160mg tablet
чистый usdt
Анализ Тетер на нетронутость: Каким образом сохранить свои электронные состояния
Все больше людей заботятся для надежность личных криптовалютных финансов. День ото дня дельцы придумывают новые способы кражи цифровых денег, и владельцы электронной валюты оказываются жертвами их обманов. Один из подходов обеспечения безопасности становится проверка кошельков в присутствие незаконных средств.
Зачем это полезно?
Прежде всего, для того чтобы защитить собственные средства от дельцов и украденных монет. Многие инвесторы встречаются с потенциальной угрозой потери своих фондов в результате хищных сценариев или грабежей. Тестирование кошельков помогает выявить сомнительные транзакции и предотвратить возможные потери.
Что наша команда предлагаем?
Наша компания предоставляем услугу анализа криптовалютных кошельков а также транзакций для обнаружения начала средств. Наша технология проверяет информацию для выявления нелегальных операций а также оценки риска для вашего портфеля. Из-за этой проверке, вы сможете избегать проблем с регулированием или обезопасить себя от участия в нелегальных операциях.
Каким образом это работает?
Мы сотрудничаем с передовыми проверочными компаниями, такими как Certik, для того чтобы предоставить точность наших проверок. Мы применяем передовые техники для выявления рискованных сделок. Ваши данные обрабатываются и сохраняются в соответствии с высокими стандартами безопасности и конфиденциальности.
Как выявить собственные USDT для чистоту?
При наличии желания подтвердить, что ваша USDT-кошельки прозрачны, наш сервис предлагает бесплатную проверку первых пяти бумажников. Легко введите местоположение вашего кошелька на на сайте, или наша команда предоставим вам детальный доклад о его положении.
Охраняйте вашими средства уже сейчас!
Не подвергайте риску подвергнуться шарлатанов или попасть в неблагоприятную ситуацию вследствие противозаконных операций. Обратитесь к нашему сервису, для того чтобы предохранить свои электронные активы и предотвратить сложностей. Совершите первый шаг к безопасности вашего криптовалютного портфеля уже сегодня!
Анализ USDT для нетронутость: Каким образом обезопасить личные электронные средства
Все больше людей заботятся к секурити собственных криптовалютных активов. Постоянно обманщики придумывают новые схемы разграбления криптовалютных средств, и также держатели цифровой валюты оказываются пострадавшими своих подстав. Один из техник охраны становится проверка кошельков для присутствие нелегальных средств.
Для чего это необходимо?
Прежде всего, для того чтобы сохранить личные средства против шарлатанов и похищенных монет. Многие специалисты встречаются с риском потери их активов из-за мошеннических планов либо хищений. Проверка кошельков помогает обнаружить сомнительные операции и предотвратить возможные убытки.
Что мы предоставляем?
Наша компания предлагаем подход проверки электронных кошельков и также операций для обнаружения источника фондов. Наша технология анализирует информацию для обнаружения незаконных операций и проценки опасности для вашего портфеля. Вследствие данной проверке, вы сможете избегнуть проблем с регулированием и предохранить себя от участия в незаконных операциях.
Как это действует?
Мы сотрудничаем с лучшими проверочными фирмами, наподобие Cure53, для того чтобы обеспечить точность наших проверок. Мы внедряем современные технологии для выявления потенциально опасных сделок. Ваши информация проходят обработку и хранятся в соответствии с высокими стандартами безопасности и конфиденциальности.
Каким образом проверить свои USDT на чистоту?
Если хотите подтвердить, что ваша USDT-кошельки нетронуты, наш сервис предоставляет бесплатное тестирование первых пяти кошельков. Просто введите место личного кошелька на на нашем веб-сайте, или наша команда предоставим вам детальный доклад об его положении.
Охраняйте ваши активы прямо сейчас!
Не подвергайте риску стать жертвой дельцов или оказаться в неприятную ситуацию из-за противозаконных операций. Посетите нашей команде, с тем чтобы обезопасить ваши криптовалютные средства и избежать неприятностей. Сделайте первый шаг к сохранности вашего криптовалютного портфеля уже сегодня!
Компрессоры воздушные https://kompressorpnevmo.ru/ купить в Москве по лучшей цене. Широкий выбор брендов. Доставка по всей РФ. Скидки, подарки, гарантия от магазина.
https://lisinopril.network/# lisinopril generic price in india
lisinopril 40 mg cost
Buy generic Levitra online: Buy Vardenafil 20mg – Generic Levitra 20mg
I appreciate the balance and fairness in The writing, like a perfect partner who always keeps things interesting. Great job!
Viagra generic over the counter Cheap Viagra 100mg viagra canada
акумулаторни тресчотки
резачки за дърва
where to buy synthroid online
The Writing is like a lighthouse for my curiosity, guiding me through the fog of information.
canadian online pharmacy no prescription
Shedding light on this subject like you’re the only star in my night sky. The brilliance is refreshing.
Воздушные компрессоры https://porshkompressor.ru/ в Москве – купить по низким ценам в интернет-магазине. Широкий ассортимент воздушных поршневых компрессоров. В каталоге – передвижные, стационарные модели, с прямым и ременным приводом, сухого сжатия и маслозаполненные.
https://cenforce.pro/# cenforce for sale
изработване на сайтове
оберфрези
best mail order pharmacy canada
order generic levitra online
The fresh insights were a breath of fresh air. Thank you for sharing The unique perspective.
cheapest viagra: Buy generic 100mg Viagra online – cheap viagra
generic valtrex online
canadian pharmacy 1 internet online drugstore
us pharmacy prices for cialis
sildenafil online best price for viagra 100mg best price for viagra 100mg
}
https://kamagra.win/# cheap kamagra
You write with such passion and clarity, it’s like listening to a love song for the mind.
Воздушные компрессоры https://kompressorgaz.ru/ купить по самым низким ценам только у нас с гарантией и бесплатной доставкой. Широкий ассортимент воздушных поршневых компрессоров.
Проверка USDT на чистоту
Проверка USDT на нетронутость: Как обезопасить личные цифровые активы
Каждый день все больше людей обращают внимание на безопасность собственных электронных активов. День ото дня дельцы разрабатывают новые подходы кражи криптовалютных денег, или владельцы криптовалюты являются жертвами их интриг. Один из техник охраны становится проверка кошельков на присутствие нелегальных финансов.
Для чего это важно?
Прежде всего, чтобы защитить личные активы от обманщиков а также украденных монет. Многие специалисты сталкиваются с риском потери своих активов вследствие мошеннических механизмов или хищений. Осмотр кошельков помогает выявить подозрительные транзакции а также предотвратить возможные потери.
Что наша команда предлагаем?
Мы предлагаем сервис проверки криптовалютных кошельков или транзакций для обнаружения источника фондов. Наша система проверяет данные для определения нелегальных операций а также проценки риска для вашего портфеля. Благодаря этой проверке, вы сможете избегать недочетов с регуляторами и защитить себя от участия в противозаконных операциях.
Каким образом это работает?
Мы сотрудничаем с первоклассными аудиторскими фирмами, например Halborn, для того чтобы предоставить прецизионность наших проверок. Мы применяем новейшие техники для выявления опасных операций. Ваши информация обрабатываются и хранятся в соответствии с высокими нормами безопасности и приватности.
Как выявить личные Tether в прозрачность?
Если вам нужно проверить, что ваши USDT-кошельки чисты, наш сервис предоставляет бесплатное тестирование первых пяти кошельков. Просто введите адрес собственного кошелька в нашем сайте, и также наш сервис предоставим вам детальный отчет о его статусе.
Гарантируйте безопасность для ваши средства уже сейчас!
Не рискуйте подвергнуться обманщиков либо попадать в неприятную обстановку вследствие противозаконных сделок. Посетите нашему агентству, с тем чтобы сохранить ваши цифровые активы и предотвратить затруднений. Сделайте первый шаг к безопасности криптовалютного портфеля сегодня!
cá cược thể thao
Reading The Writing is like finding the perfect song that I can’t stop listening to. Play it again?
The posts are like a cozy nook, inviting and comfortable, where I can immerse myself in thoughts.
valtrex cream otc
Купить компрессоры https://kompressoroil.ru/ по самым выгодным ценам в Москве в интернет-магазине. Широкий выбор компрессоров. В каталоге можно ознакомиться с ценами, отзывами, фотографиями и подробными характеристиками компрессоров.
http://levitrav.store/# buy Levitra over the counter
Buy generic Levitra online Vardenafil online prescription Levitra 20 mg for sale
Levitra online pharmacy: Buy Vardenafil 20mg – Buy Vardenafil 20mg
synthroid 0.88
buy prednisone 10mg online
order zithromax online uk
online pharmacy delivery delhi
It is very comforting to see that others are suffering from the same problem as you, wow!
It is very comforting to see that others are suffering from the same problem as you, wow!
We’ll buy or invest in your site and you Investment/Buying ranging from $50,000 to $500,000, depending on stage, market volume, market share get investments
We’ll buy or invest in your site and you Investment/Buying ranging from $50,000 to $500,000, depending on stage, market volume, market share sell site
We’ll buy or invest in your site and you Investment/Buying ranging from $50,000 to $500,000, depending on stage, market volume, market share https://buy-site.pages.dev/
cialis for daily use 5 mg cost
viagra without prescription Cheapest place to buy Viagra Cheap generic Viagra online
buy azithromycin uk
cheap viagra: Buy Viagra online – Cheap Viagra 100mg
https://kamagra.win/# Kamagra 100mg
Продвижение сайтов в поисковых системах https://seoshnikiguru.ru/ с гарантией результата. SEO продвижение сайтов в ТОП-10 Яндекс, заказать поисковое сео продвижение, раскрутка веб сайта в Москве.
lisinopril pills 10 mg
cheap viagra viagras.online over the counter sildenafil
0.05 mg synthroid
order pharmacy online egypt
best price for viagra 100mg: cheap viagra – Viagra without a doctor prescription Canada
https://levitrav.store/# Buy Vardenafil 20mg
Заказать SEO продвижение сайтов https://seoshnikigo.ru/ в ТОП поисковых систем Яндекс и Google в Москве, оплата за результат и по факту. Кейсы, стратегии продвижения, скидки и акции, индивидуальный подход
pharmacy order online
affordable pharmacy
nitroglycerin cheap – buy clonidine medication buy valsartan pill
generic tadalafil us
Truly quite a lot of very good info.|
how much is zithromax
http://cenforce.pro/# buy cenforce
synthroid canada pharmacy
Levitra 10 mg buy online Vardenafil online prescription Levitra tablet price
Купить квартиру в Казани https://novostroyzhilie.ru/ от застройщика. Планировки и цены трехкомнатных, двухкомнатных и однокомнатных квартир в новостройке.
best place to buy cialis online
Levitra tablet price: Levitra 20mg price – Cheap Levitra online
prednisone buy online uk
http://cialist.pro/# Cheap Cialis
Hi there this is kinda of off topic but I was wanting to know if blogs use WYSIWYG editors or if you have
to manually code with HTML. I’m starting
a blog soon but have no coding skills so I wanted to get guidance from someone with experience.
Any help would be enormously appreciated!
Here is my web blog … escorts in Lahore
online pharmacy price checker
online pharmacies that use paypal
Раскрутка сайтов https://seoshnikigood.ru/ в ТОП в городе Москва. Используем эффективные методы, работаем практически с любым бюджетом. Выгодные условия, индивидуальный подход.
order cenforce cenforce for sale Cenforce 100mg tablets for sale
buy cheap tadalafil online
Backlink pyramid
Sure, here’s the text with spin syntax applied:
Backlink Hierarchy
After several updates to the G search mechanism, it is vital to utilize different methods for ranking.
Today there is a means to capture the interest of search engines to your site with the assistance of incoming links.
Links are not only an powerful marketing instrument but they also have authentic traffic, direct sales from these resources likely will not be, but transitions will be, and it is poyedenicheskogo traffic that we also receive.
What in the end we get at the final outcome:
We show search engines site through backlinks.
Prluuchayut natural transitions to the site and it is also a sign to search engines that the resource is used by individuals.
How we show search engines that the site is valuable:
Backlinks do to the primary page where the main information.
We make backlinks through redirects reputable sites.
The most SIGNIFICANT we place the site on sites analyzers distinct tool, the site goes into the memory of these analysis tools, then the obtained links we place as redirections on weblogs, forums, comment sections. This significant action shows search engines the site map as analysis tool sites show all information about sites with all keywords and headings and it is very BENEFICIAL.
All details about our services is on the website!
no prescription needed: non prescription online pharmacy india – canada pharmacies online prescriptions
reputable indian online pharmacy
india pharmacy online pharmacy india п»їlegitimate online pharmacies india
medicine azithromycin 500 mg
legit online pharmacy
simvastatin abrupt – zocor trouble atorvastatin glimpse
Продажа квартир https://novostroykihome.ru/ и недвижимости в Казани по выгодной стоимости на официальном сайте застройщика. Жилье в Казани: помощь в подборе и покупке новых квартир, цены за квадратный метр, фото, планировки.
simvastatin worm – simvastatin eastern atorvastatin objection
azithromycin medicine 500 mg
prednisone for sale without prescription
http://pharmmexico.online/# mexico drug stores pharmacies
Backlink pyramid
Sure, here’s the text with spin syntax applied:
Backlink Hierarchy
After multiple updates to the G search engine, it is essential to use different options for ranking.
Today there is a method to engage the interest of search engines to your site with the assistance of inbound links.
Backlinks are not only an efficient promotional instrument but they also have authentic traffic, direct sales from these resources possibly will not be, but visits will be, and it is poyedenicheskogo visitors that we also receive.
What in the end we get at the final outcome:
We display search engines site through links.
Prluuchayut natural transitions to the site and it is also a signal to search engines that the resource is used by people.
How we show search engines that the site is profitable:
Backlinks do to the principal page where the main information.
We make links through redirects reputable sites.
The most IMPORTANT we place the site on sites analyzers separate tool, the site goes into the memory of these analyzers, then the acquired links we place as redirections on blogs, forums, comments. This essential action shows search engines the MAP OF THE SITE as analysis tool sites present all information about sites with all keywords and headings and it is very POSITIVE.
All details about our services is on the website!
online medicine without prescription: no prescription online pharmacy – pharmacy no prescription required
pharmacy wholesalers canada
http://pharmnoprescription.icu/# canadian pharmacy online no prescription
indianpharmacy com online shopping pharmacy india online pharmacy india
Online medicine home delivery: top online pharmacy india – online pharmacy india
online pharmacy products
Написание курсовых работ https://courseworkskill.ru/ на заказ быстро, качественно, недорого. Сколько стоит заказать курсовую работу. Поручите написание курсовой работы профессионалам.
rosuvastatin online yellow – pravastatin buy soul caduet pills room
Creating unique articles on Platform and Telegraph, why it is vital:
Created article on these resources is superior ranked on low-frequency queries, which is very significant to get organic traffic.
We get:
organic traffic from search algorithms.
organic traffic from the internal rendition of the medium.
The webpage to which the article refers gets a link that is liquid and increases the ranking of the platform to which the article refers.
Articles can be made in any number and choose all less frequent queries on your topic.
Medium pages are indexed by search algorithms very well.
Telegraph pages need to be indexed separately indexer and at the same time after indexing they sometimes occupy spots higher in the search algorithms than the medium, these two platforms are very beneficial for getting traffic.
Here is a link to our offerings where we present creation, indexing of sites, articles, pages and more.
Доброго любители шоппинга!
Погрузитесь в мир экономии с нашим онлайн-сервисом купонов и промокодов! Мы предлагаем огромный выбор акций и специальных предложений от лучших магазинов, помогая вам сэкономить на всем, от моды до бытовой техники. Наш удобный интерфейс делает поиск актуальных скидок и промокодов легким и приятным. Подпишитесь на наши уведомления, чтобы быть в курсе последних акций и получать доступ к эксклюзивным предложениям. Не упустите шанс сэкономить больше с каждой покупкой!
Сайт самых свежих и проверенных промокодов магазина КолесаДаром http://maxpromokod.ru
Свежие промокоды MiniInTheBox WW супер скидки
Экономичные промокоды Bestwatch.ru на сегодня
Свежие промокоды Dx WW на сегодня
Бесплатные промокоды Strawberrynet RU для онлайн-покупок
Коды промо интернет магазина Postel Deluxe ограниченная серия
Эксклюзивные скидки DeoShop.ru свежие и актуальные
Удачных покупок!
Здравствуйте!
Откройте двери к морю скидок с нашим онлайн сервисом купонов и промокодов! Наши уникальные предложения позволят вам сэкономить на покупках в различных магазинах, включая электронику, моду, товары для дома и многое другое. Наш сайт предлагает простой и удобный способ находить актуальные акции и купоны, которые помогут вам сэкономить максимально возможную сумму. Не упускайте возможность быть в курсе последних выгодных предложений от лучших магазинов. Подписывайтесь на наши рассылки и получайте уведомления о новых акциях, чтобы быть первыми, кто воспользуется самыми привлекательными скидками. У нас для вас всегда есть что-то особенное!
Сайт самых свежих и проверенных купонов магазина Lightinthebox.com INT http://maxpromokod.ru
Привлекательные промокоды Дочки & Сыночки свежие и актуальные
Лучшие предложения Voltoff супер скидки
Надежные промокоды Carlo Pazolini для онлайн-покупок
Эксклюзивные акции ЛитРес супер скидки
Коды промо интернет магазина МТС онлайн
Надежные промокоды O’STIN онлайн
Удачных покупок!
escrow pharmacy canada
drug prices lisinopril
pharmacy wholesalers canada
link building
Creating hyperlinks is simply as successful now, just the resources for working within this domain have got altered.
You can find many possibilities regarding inbound links, we employ some of them, and these strategies work and have been tested by our experts and our clientele.
Not long ago we performed an experiment and we found that low-frequency search queries from one website position effectively in search results, and the result doesn’t have to become your website, you are able to utilize social media from web2.0 range for this.
It additionally it is possible to partially move weight through web page redirects, offering a diverse backlink profile.
Head over to our website where our own offerings are actually provided with thorough descriptions.
http://pharmworld.store/# pharmacy no prescription required
reputable indian pharmacies п»їlegitimate online pharmacies india mail order pharmacy india
buying drugs from canada: canadian king pharmacy – online canadian pharmacy reviews
synthroid.com
drug discount valtrex generic
Квартиры с ремонтом в новостройках https://kupitkvartiruseychas.ru/ Казани по ценам от застройщика.Лидер по строительству и продажам жилой и коммерческой недвижимости.
online pharmacy delivery usa
pharmacy website india: indian pharmacy paypal – indian pharmacy paypal
Creating distinct articles on Platform and Platform, why it is necessary:
Created article on these resources is better ranked on less frequent queries, which is very important to get natural traffic.
We get:
organic traffic from search algorithms.
organic traffic from the internal rendition of the medium.
The site to which the article refers gets a link that is liquid and increases the ranking of the platform to which the article refers.
Articles can be made in any quantity and choose all low-frequency queries on your topic.
Medium pages are indexed by search engines very well.
Telegraph pages need to be indexed distinctly indexer and at the same time after indexing they sometimes occupy spots higher in the search engines than the medium, these two platforms are very useful for getting visitors.
Here is a URL to our offerings where we offer creation, indexing of sites, articles, pages and more.
cheapest pharmacy to get prescriptions filled cheapest pharmacy canadian pharmacy coupon
synthroid 1 mg
can i buy lisinopril over the counter in mexico
Creating hyperlinks is simply just as effective at present, simply the resources for working in this field possess shifted.
You can find numerous options for backlinks, our team use a few of them, and these approaches operate and have already been tested by us and our customers.
Not long ago we conducted an trial and we found that low-frequency searches from a single domain name rank well in online searches, and this does not need to be your own domain name, you are able to utilize social media from the web 2.0 series for this.
It additionally possible to partly transfer load through website redirects, offering a varied backlink profile.
Visit to our very own site where our company’s services are actually provided with thorough explanations.
https://pharmmexico.online/# buying from online mexican pharmacy
no prescription pharmacy paypal: online pharmacy discount code – online pharmacy no prescription
synthroid canada
Почему посудомоечная машина https://kulbar.ru/2024/01/21/pochemu-posudomoechnaya-mashina-eto-neobhodimost-dlya-sovremennogo-doma/ необходимость для современного дома? Как использовать и как выбрать посудомойку?
175 mg synthroid
Either way, oddsmakers have him slated to win outright at +8,000, a slightly longer number compared to his +6,000 odds at Augusta National, but these numbers will shift based on how he plays during the leadup. Scottie Scheffler leads the way as the betting favorite to take home his first U.S. Open title at +700. World No. 2 Jon Rahm is in second with +1000 odds-to-win, followed by PGA champion Brooks Koepka at +1100. We’re back in major championship territory, and as a result, the top of the odds-to-win list features the game’s biggest and brightest stars. Another legend makes the top five and his name is Sam Snead. A dominant player, Snead was a prolific winner and a three-time winner of the PGA Championship. Online golf betting wasn’t a thing back then, but his odds would have been around +200 to win.
https://netcallvoip.com/wiki/index.php/Top_mobile_betting_sites
Matt LaFleur is 8-0 outright and ATS against the Bears. The eight-game cover streak is the longest active intradivision cover streak in the NFL.Justin Fields is 8-16-1 ATS in his career, the second-worst record among quarterbacks to start at least 25 games in the Super Bowl era (Colt McCoy). He is 4-8-1 ATS at home.The Bears are 2-10 ATS in division games in the last two seasons.” Betting Nuggets Line Movement Alert: Opened Colts -1.5 Favorite: Micah Parsons (+100)Last week’s favorite: Parsons (+100)The Defensive Player of the Year race has remained relatively stagnant for a long time with Micah Parsons, Myles Garrett and T.J. Watt the three favorites. Watt has the best statistics, but ESPN Analytics gives his Steelers a 12% chance to make the playoffs, and eight straight winners of this award have made the playoffs.
lisinopril 20 mg best price
azithromycin 500 mg
lisinopril pill
canadian pharmacies online canadian drugs pharmacy best canadian pharmacy
metformin hydrochloride
https://pharmindia.online/# reputable indian online pharmacy
azithromycin tablets 250 mg price in india
Купить квартиру https://newflatsale.ru/ в новостройке: однокомнатную, двухкомнатную, трехкомнатную в жилом комплексе в рассрочку, ипотеку, мат. капитал от застройщика.
reputable indian pharmacies: online pharmacy india – Online medicine order
generic cialis lowest price
metformin 2000 mg
synthroid 200
online pharmacies that use paypal
lisinopril 10 12.5 mg tablets
Продажа квартир в Казани https://kupitkvartiruzdes.ru/ от застройщика. Большой выбор квартир. Возможность купить онлайн. Квартиры с дизайнерской отделкой.
cheapest pharmacy for prescriptions without insurance pharmacy coupons cheapest pharmacy to fill prescriptions with insurance
cockfight
online pharmacy pain
https://pharmworld.store/# no prescription required pharmacy
tadalafil 10mg cost
mexican pharmaceuticals online: reputable mexican pharmacies online – purple pharmacy mexico price list
prednisone cost
buy zithromax without prescription
lisinopril 40 mg pill
lisinopril for sale uk
обучение excel для начинающих – Обучение с гарантиями государственного университета.
buy cheap tadalafil
canadian pharmacy 24 com
https://kurs-excel.ru/ – Обучение с гарантиями государственного университета.
курсы excel в москве онлайн – Обучение с гарантиями государственного университета.
cialis daily 2.5 mg cost
doxycycline pills generic doxycycline buy cheap doxycycline online
doxycycline hyc: buy cheap doxycycline online – 100mg doxycycline
https://amoxila.pro/# amoxicillin for sale
average cost of prednisone 20 mg
crestor online cigar – rosuvastatin recollect caduet buy space
uk pharmacy no prescription
happy family canadian pharmacy
Купить квартиру в новостройке https://newhomesale.ru/ в Казани. Продажа новой недвижимости в ЖК новостройках по ценам от застройщика.
which pharmacy is cheaper
buy doxycycline online price of doxycycline order doxycycline
can i buy levitra online
where to buy generic cialis
azithromycin 500 mg tablet for sale
tadalafil 20 mg medication
can i buy zithromax online: azithromycin zithromax – zithromax antibiotic without prescription
buy zithromax without presc: zithromax capsules australia – where can i get zithromax
generic for synthroid
order valtrex canada
link building
Link building is just just as successful now, just the resources to work in this area have got changed.
There are actually numerous options to incoming links, our team utilize a few of them, and these approaches function and have already been tested by our team and our clients.
Not long ago our company performed an trial and it transpired that less frequent queries from a single domain name position well in online searches, and this doesn’t have being your own website, it is possible to use social networking sites from web2.0 collection for this.
It additionally it is possible to partially shift load through web page redirects, giving an assorted hyperlink profile.
Head over to our own website where our company’s services are typically presented with thorough overview.
https://amoxila.pro/# amoxicillin 500mg for sale uk
amoxicillin cost australia: buy amoxicillin 500mg – amoxicillin 825 mg
Стальные трубчатые радиаторы Arbonia (Чехия) и Rifar Tubog (Россия) https://medcom.ru/forum/user/226934/ подходят как для частных домов, так и для квартир в многоэтажках.
pharmacy home delivery
С началом СВО уже спустя полгода была объявлена первая волна мобилизации. При этом прошлая, в последний раз в России была аж в 1941 году, с началом Великой Отечественной Войны. Конечно же, желающих отправиться на фронт было не много, а потому люди стали искать способы не попасть на СВО, для чего стали покупать справки о болезнях, с которыми можно получить категорию Д. И все это стало возможным с даркнет сайтами, где можно найти практически все что угодно. Именно об этой отрасли темного интернета подробней и поговорим в этой статье.
viagra professional passe – super kamagra clue levitra oral jelly belief
курсы массажистов
prednisone cost canada: pharmacy cost of prednisone – prednisone 20mg online
бьюти мастера
buy generic tadalafil online uk
каталог салонов красоты
synthroid 0.5 mg
как разорвать контракт сво контрактнику
С началом СВО уже спустя полгода была объявлена первая волна мобилизации. При этом прошлая, в последний раз в России была аж в 1941 году, с началом Великой Отечественной Войны. Конечно же, желающих отправиться на фронт было не много, а потому люди стали искать способы не попасть на СВО, для чего стали покупать справки о болезнях, с которыми можно получить категорию Д. И все это стало возможным с даркнет сайтами, где можно найти практически все что угодно. Именно об этой отрасли темного интернета подробней и поговорим в этой статье.
buy neurontin online: neurontin medication – neurontin 100 mg cap
doxycycline hyclate: doxycycline hyclate – buy doxycycline online uk
Продажа квартир в новостройках https://newflatsalespb.ru/ СПБ по выгодным ценам от застройщика. Купить квартиру в СПБ на выгодных условиях.
no prescription prednisone canadian pharmacy where to buy prednisone 20mg no prescription prednisone 20mg buy online
azithromycin canada prescription
prednisone cream over the counter
reputable online pharmacy reddit
https://gabapentinneurontin.pro/# neurontin 300 mg caps
purchase valtrex canada
online otc pharmacy
viagra vs levitra
свадебные платья в Санкт-Петербурге, где более 400 платьев в наличии. Свадебные и вечерние платья А-силуэта, прямые, греческие, пышные, силуэт Рыбка.
buy doxycycline cheap: 200 mg doxycycline – doxylin
prednisone steroid
where to by cialis
пышные свадебные платья, где более 400 платьев в наличии. Свадебные и вечерние платья А-силуэта, прямые, греческие, пышные, силуэт Рыбка.
synthroid 75 mcg price in india
happy family store
how to buy doxycycline online doxylin doxycycline hyclate
cheap meds metformin
can i buy azithromycin 500mg
http://doxycyclinea.online/# doxycycline without prescription
Флористика, декор, вышивания и украшения. Наборы для канцелярии, росписи текстиля, декорации и детского творчества.
Вышивка и вышивание, декор, вышивания и украшения. Наборы для канцелярии, росписи текстиля, декорации и детского творчества.
can i buy metformin over the counter
Рукоделие, декор, вышивания и украшения. Наборы для канцелярии, росписи текстиля, декорации и детского творчества.
lisinopril brand name in usa
neurontin prescription medication: neurontin 300 – neurontin rx
cialis canada online
valtrex australia
amoxicillin 30 capsules price where can i get amoxicillin 500 mg where can i buy amoxicillin online
反向連接金字塔
G搜尋引擎在屡经更新后需要套用不同的排名參數。
今天有一種方法可以使用反向連結吸引G搜尋引擎對您的網站的注意。
反向連接不僅是有效的推廣工具,也是有機流量。
我們會得到什麼結果:
我們透過反向链接向G搜尋引擎展示我們的網站。
他們收到了到該網站的自然過渡,這也是向G搜尋引擎發出的信號,表明該資源正在被人們使用。
我們如何向G搜尋引擎表明該網站具有流動性:
個帶有主要訊息的主頁反向鏈接
我們透過來自受信任網站的重定向來建立反向链接。
此外,我們將網站放置在单独的網路分析器上,網站最終會進入這些分析器的快取中,然後我們使用產生的連結作為部落格、論壇和評論的重新导向。 這個重要的操作向G搜尋引擎顯示了網站地圖,因為網站分析器顯示了有關網站的所有資訊以及所有關鍵字和標題,這很棒
有關我們服務的所有資訊都在網站上!
https://nz-offers.pages.dev Investment/Buying sites, depending on stage, market volume, and share. Comprehensive support for financial, legal, and HR aspects.
An affiliate department for the best offers and monetization strategies.
happy family canadian pharmacy
Pirámide de backlinks
Aquí está el texto con la estructura de spintax que propone diferentes sinónimos para cada palabra:
“Pirámide de backlinks
Después de varias actualizaciones del motor de búsqueda G, necesita aplicar diferentes opciones de clasificación.
Hay una manera de hacerlo de llamar la atención de los motores de búsqueda a su sitio web con backlinks.
Los enlaces de retorno no sólo son una estrategia eficaz para la promoción, sino que también tienen tráfico orgánico, las ventas directas de estos recursos más probable es que no será, pero las transiciones será, y es tráfico potencial que también obtenemos.
Lo que vamos a obtener al final en la salida:
Mostramos el sitio a los motores de búsqueda a través de backlinks.
Conseguimos transiciones orgánicas hacia el sitio, lo que también es una señal para los buscadores de que el recurso está siendo utilizado por la gente.
Cómo mostramos los motores de búsqueda que el sitio es líquido:
1 enlace se hace a la página principal donde está la información principal
Hacemos enlaces de retroceso a través de redirecciones de sitios de confianza
Lo más IMPORTANTE colocamos el sitio en una herramienta independiente de analizadores de sitios, el sitio entra en la caché de estos analizadores, luego los enlaces recibidos los colocamos como redirecciones en blogs, foros, comentarios.
Esta crucial acción muestra a los buscadores el MAPA DEL SITIO, ya que los analizadores de sitios muestran toda la información de los sitios con todas las palabras clave y títulos y es muy positivo.
¡Toda la información sobre nuestros servicios en el sitio web!
rx pharmacy online 24
nz-offers.pages.dev Investment/Buying sites, depending on stage, market volume, and share. Comprehensive support for financial, legal, and HR aspects.
An affiliate department for the best offers and monetization strategies.
how much is prednisone cost
rx cialis coupon
https://amoxila.pro/# order amoxicillin online uk
over the counter prednisone cheap: 50 mg prednisone tablet – buy prednisone mexico
secure medical online pharmacy
zithromax 500mg price zithromax buy online no prescription how to get zithromax over the counter
purchasing cialis in mexico
can i order valtrex online
synthroid from india
maple leaf pharmacy in canada
反向連結金字塔
反向連結金字塔
G搜尋引擎在多次更新後需要使用不同的排名參數。
今天有一種方法可以使用反向链接吸引G搜尋引擎對您的網站的注意。
反向链接不僅是有效的推廣工具,也是有機流量。
我們會得到什麼結果:
我們透過反向連接向G搜尋引擎展示我們的網站。
他們收到了到該網站的自然過渡,這也是向G搜尋引擎發出的信號,表明該資源正在被人們使用。
我們如何向G搜尋引擎表明該網站具有流動性:
個帶有主要訊息的主頁反向鏈接
我們透過來自受信任網站的重新定向來建立反向連結。
此外,我們將網站放置在独立的網路分析器上,網站最終會進入這些分析器的高速缓存中,然後我們使用產生的連結作為部落格、論壇和評論的重新定向。 這個重要的操作向G搜尋引擎顯示了網站地圖,因為網站分析器顯示了有關網站的所有資訊以及所有關鍵字和標題,這很棒
有關我們服務的所有資訊都在網站上!
Pirámide de backlinks
Aquí está el texto con la estructura de spintax que propone diferentes sinónimos para cada palabra:
“Pirámide de backlinks
Después de varias actualizaciones del motor de búsqueda G, necesita aplicar diferentes opciones de clasificación.
Hay una manera de hacerlo de llamar la atención de los motores de búsqueda a su sitio web con backlinks.
Los backlinks no sólo son una táctica eficaz para la promoción, sino que también tienen tráfico orgánico, las ventas directas de estos recursos más probable es que no será, pero las transiciones será, y es poedenicheskogo tráfico que también obtenemos.
Lo que vamos a obtener al final en la salida:
Mostramos el sitio a los motores de búsqueda a través de enlaces de retorno.
Conseguimos conversiones orgánicas hacia el sitio, lo que también es una señal para los buscadores de que el recurso está siendo utilizado por la gente.
Cómo mostramos los motores de búsqueda que el sitio es líquido:
1 backlink se hace a la página principal donde está la información principal
Hacemos backlinks a través de redirecciones de sitios de confianza
Lo más crucial colocamos el sitio en una herramienta independiente de analizadores de sitios, el sitio entra en la caché de estos analizadores, luego los enlaces recibidos los colocamos como redirecciones en blogs, foros, comentarios.
Esta importante acción muestra a los buscadores el MAPA DEL SITIO, ya que los analizadores de sitios muestran toda la información de los sitios con todas las palabras clave y títulos y es muy positivo.
¡Toda la información sobre nuestros servicios en el sitio web!
buy zithromax no script
nz-offers.pages.dev
https://nz-offers.pages.dev/
metformin online usa no prescription
cost for valtrex
http://zithromaxa.store/# zithromax capsules australia
azithromycin tablets over the counter
cheap metformin online
viagra professional foreign – buy viagra gold joe levitra oral jelly online statement
neurontin price in india: gabapentin 300 – neurontin 300mg caps
priligy wise – sildigra soft cialis with dapoxetine pardon
can you buy amoxicillin over the counter amoxicillin 500mg price cost of amoxicillin
tadalafil in mexico
https://gamesdb.ru/
dapoxetine free – sildigra heat cialis with dapoxetine cap
valtrex 500mg
valtrex over the counter uk
synthroid 0.05mg cost
online pharmacy cialis
azithromycin 500 mg india
valtrex generic sale
https://nz-offers.pages.dev/
buy tadalafil 40 mg
valtrex tablet
https://zithromaxa.store/# zithromax 500 tablet
https://novyidomkupitspb.ru/ купить квартиру в новостройке Санкт-Петербурга от застройщика
zithromax azithromycin: where can i get zithromax over the counter – zithromax coupon
azithromycin generic cost india
can you purchase valtrex online
where can i get doxycycline doxycycline hyclate 100 mg cap doxycycline 50 mg
50 mcg synthroid
buy valtrex online uk
lisinopril cost us
cheap neurontin: neurontin capsule 400 mg – 600 mg neurontin tablets
synthroid 100 mcg
buy valtrex cheap online
lisinopril 5 mg daily
valtrex 1000 mg cost
https://newflatstroyka.ru/ квартиры от застройщика в Казани
https://gabapentinneurontin.pro/# neurontin 100mg
buy azithromycin without a prescription
order amoxicillin online no prescription: amoxicillin online without prescription – amoxicillin 500 mg price
tadalafil 30 tablet 5 mg
cost for prednisone 50mg
neurontin generic neurontin 400 mg cost neurontin brand name 800 mg
escrow pharmacy online
https://novostroykatoday.ru/ купить квартиру от застройщика в Казани с гарантией
prednisolone prednisone
buy valtrex no prescription
pharmacy
online pharmacy amoxicillin uk
cenforce fly – cenforce explain brand viagra pills fro
https://gabapentinneurontin.pro/# generic neurontin
online pharmacy birth control pills
canadian pharmacy price for synthroid
amoxicillin 250 mg capsule: buy amoxicillin over the counter uk – buy amoxicillin from canada
neurontin cost in singapore buying neurontin online neurontin 200 mg capsules
Как защитить свои данные: берегитесь утечек информации в интернете. Сегодня сохранение своих данных становится всё значимее важной задачей. Одним из наиболее популярных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и как защититься от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые постоянно используются для входа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или иные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, используя этих сит фраз. Как сохранить свои личные данные? Используйте сложные пароли. Избегайте использования очевидных паролей, которые легко угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухфакторную аутентификацию (2FA). Это добавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте свою информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы сохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы защитить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
даркнет сливы тг
Даркнет и сливы в Телеграме
Даркнет – это сегмент интернета, которая не индексируется обыденными поисковыми системами и требует специальных программных средств для доступа. В даркнете существует изобилие скрытых сайтов, где можно найти различные товары и услуги, в том числе и нелегальные.
Одним из востребованных способов распространения информации в даркнете является использование мессенджера Телеграм. Телеграм предоставляет возможность создания закрытых каналов и чатов, где пользователи могут обмениваться информацией, в том числе и нелегальной.
Сливы информации в Телеграме – это способ распространения конфиденциальной информации, такой как украденные данные, базы данных, персональные сведения и другие материалы. Эти сливы могут включать в себя информацию о кредитных картах, паролях, персональных сообщениях и даже фотографиях.
Сливы в Телеграме могут быть опасными, так как они могут привести к утечке конфиденциальной информации и нанести ущерб репутации и финансовым интересам людей. Поэтому важно быть осторожным при обмене информацией в интернете и не доверять сомнительным источникам.
Вот кошельки с балансом у бота
Сид-фразы, или мнемонические фразы, представляют собой сочетание слов, которая используется для создания или восстановления кошелька криптовалюты. Эти фразы обеспечивают возможность доступа к вашим криптовалютным средствам, поэтому их защищенное хранение и использование очень важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы составляют набор случайно сгенерированных слов, обычно от 12 до 24, которые предназначаются для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления входа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают высокой степенью защиты и шифруются, что делает их безопасными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы необходимы для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить вход к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете быстро создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не делитесь сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может влечь за собой утере вашего криптоимущества.
Храните сид-фразу в секурном месте. Используйте физически надежные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить вход к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите другие методы защиты и двухфакторную верификацию для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом надежного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Слив сид фраз (seed phrases) является одной из наиболее обычных способов утечки персональной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, почему они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, формируют комбинацию слов, которая используется для генерации или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые символизируют собой ключ к вашему кошельку. Потеря или утечка сид фразы может приводить к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы являются ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они сумеют получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу никому, даже если вам происходит, что это проверенное лицо или сервис.
Храните свою сид фразу в надежном и защищенном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная аутентификация (2FA), для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в различных безопасных местах.
Заключение
Слив сид фраз является существенной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
пирамида обратных ссылок
Структура обратных ссылок
После многочисленных обновлений поисковой системы G необходимо использовать различные варианты сортировки.
Сегодня есть способ привлечь внимание поисковых систем к вашему веб-сайту с помощью обратных линков.
Обратные ссылки представляют собой эффективный инструмент продвижения, но и являются источником органического трафика, хотя прямых продаж с этих ресурсов скорее всего не будет, но переходы будут, и именно органического трафика мы также получаем.
Что в итоге получим на выходе:
Мы показываем сайт поисковым системам с помощью обратных ссылок.
Получают органические переходы на веб-сайт, а это также подтверждение поисковым системам, что ресурс активно посещается пользователями.
Как мы указываем поисковым системам, что сайт ликвиден:
1 ссылка на главную страницу, где содержится основная информация, создается.
Делаем обратные ссылки через редиректы трастовых сайтов.
Главное – мы добавляем сайт в специализированные инструменты для анализа сайтов, где он кэшируется, а затем полученные ссылки размещаются в виде редиректов на блогах, форумах, в комментариях.
Это важное действие показывает всем поисковикамКАРТУ САЙТА, так как анализаторы сайтов отображают всю информацию о сайтах со с тайтлами, ключами, h1,h2,h3 и это очень ВАЖНО
valtrex 500mg cost
prednisone purchase
Покупки станут дешевле – получи Кэшбэк https://maxpromokod.ru/ до 30%! У нас более 4 500 интернет-магазинов и 33 000 промокодов и акций скидок.
Доброго!
Мы готовы предложить вам широкий выбор входных и межкомнатных дверей в Саратове и области, а также обеспечить их установку. Наша компания имеет обширный опыт в решении различных задач, связанных с установкой и обслуживанием дверных конструкций. Нашими основными принципами являются надежность, соблюдение сроков и высокий уровень сервиса.
Мы предлагаем клиентам более 1000 моделей входных и межкомнатных дверей от известных производителей, различающихся по стоимости, материалу отделки и конструкции. Наши специалисты всегда готовы помочь вам выбрать оптимальное решение, учитывая все ваши требования и предпочтения. Благодаря нашему профессионализму и опыту, мы гарантируем надежность и комфорт при использовании выбранных вами дверей.
Вся информация на сайте https://id64.ru/
Магазин компании удобно расположен в центре. Клиент без проблем может добраться до магазина из любой точки города и изучить ассортимент.
Компания является официальным дилером и прямым поставщиком дверей всех известных производителей, что подтверждено документально на сайте.
Вы можете купить у нас двери в рассрочку без переплат при участии банков: Сбер, Почта банк, МТС банк, Русский Стандарт, Хоум кредит, Халва.
По желанию клиента, двери могут изготавливаться с индивидуальными параметрами: тип отделки, фурнитура, размеры.
Двери глухие
Противопожарные двери
Декоративные рейки
Строительные двери
Двери в ванную
Двери с зеркалом
Удачи и хорошего интерьера!
Thank you so much!
http://amoxila.pro/# buy amoxicillin 500mg capsules uk
amoxicillin 875 mg tablet: generic amoxil 500 mg – amoxicillin 500mg cost
هنا النص مع استخدام السبينتاكس:
“بنية الروابط الخلفية
بعد التحديثات العديدة لمحرك البحث G، تحتاج إلى تنفيذ خيارات ترتيب مختلفة.
هناك منهج لجذب انتباه محركات البحث إلى موقعك على الويب باستخدام الروابط الخلفية.
الروابط الخلفية ليست فقط أداة فعالة للترويج، ولكن تمتلك أيضًا حركة مرور عضوية، والمبيعات المباشرة من هذه الموارد على الأرجح قد لا تكون كذلك، ولكن التغييرات ستكون، وهي حركة المرور التي نحصل عليها أيضًا.
ما سنحصل عليه في النهاية في النهاية في الإخراج:
نعرض الموقع لمحركات البحث من خلال الروابط الخلفية.
2- نحصل على تبديلات عضوية إلى الموقع، وهي أيضًا إشارة لمحركات البحث أن المورد يستخدمه الناس.
كيف نظهر لمحركات البحث أن الموقع سائل:
1 يتم عمل رابط خلفي للصفحة الرئيسية حيث المعلومات الرئيسية
نقوم بعمل روابط خلفية من خلال عمليات توجيه المواقع الموثوقة
الأهم من ذلك أننا نضع الموقع على أداة منفصلة من أساليب تحليل المواقع، ويدخل الموقع في ذاكرة التخزين المؤقت لهذه المحللات، ثم الروابط المستلمة التي نضعها كتوجيه مرة أخرى على المدونات والمنتديات والتعليقات.
هذا التدبير المهم يعرض لمحركات البحث خريطة الموقع، حيث تعرض أدوات تحليل المواقع جميع المعلومات عن المواقع مع جميع الكلمات الرئيسية والعناوين وهو شيء جيد جداً
جميع المعلومات عن خدماتنا على الموقع!
взлом кошелька
Как охранять свои данные: избегайте утечек информации в интернете. Сегодня охрана информации становится более насущной важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в каком объеме защититься от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые бывают используются для входа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как охранить свои личные данные? Используйте комплексные пароли. Избегайте использования несложных паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухфакторную проверку (2FA). Это вводит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте свою информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы сохранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
medication neurontin 300 mg neurontin 100 mg cost neurontin 400 mg
canadadrugpharmacy
canadian mail order pharmacy
Криптокошельки с балансом: зачем их покупают и как использовать
В мире криптовалют все большую популярность приобретают криптокошельки с предустановленным балансом. Это специальные кошельки, которые уже содержат определенное количество криптовалюты на момент покупки. Но зачем люди приобретают такие кошельки, и как правильно использовать их?
Почему покупают криптокошельки с балансом?
Удобство: Криптокошельки с предустановленным балансом предлагаются как готовое к применению решение для тех, кто хочет быстро начать пользоваться криптовалютой без необходимости покупки или обмена на бирже.
Подарок или награда: Иногда криптокошельки с балансом используются как подарок или вознаграждение в рамках акций или маркетинговых кампаний.
Анонимность: При покупке криптокошелька с балансом нет запроса предоставлять личные данные, что может быть важно для тех, кто ценит анонимность.
Как использовать криптокошелек с балансом?
Проверьте безопасность: Убедитесь, что кошелек безопасен и не подвержен взлому. Проверьте репутацию продавца и происхождение приобретения кошелька.
Переведите средства на другой кошелек: Если вы хотите долгосрочно хранить криптовалюту, рекомендуется перевести средства на более безопасный или полезный для вас кошелек.
Не храните все средства на одном кошельке: Для обеспечения безопасности рекомендуется распределить средства между несколькими кошельками.
Будьте осторожны с фишингом и мошенничеством: Помните, что мошенники могут пытаться обмануть вас, предлагая криптокошельки с балансом с целью получения доступа к вашим средствам.
Заключение
Криптокошельки с балансом могут быть удобным и скорым способом начать пользоваться криптовалютой, но необходимо помнить о безопасности и осторожности при их использовании.Выбор и приобретение криптокошелька с балансом – это весомый шаг, который требует внимания к деталям и осознанного подхода.”
Сид-фразы, или напоминающие фразы, представляют собой сумму слов, которая используется для составления или восстановления кошелька криптовалюты. Эти фразы обеспечивают возможность к вашим криптовалютным средствам, поэтому их секурное хранение и использование крайне важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы представляют собой набор произвольно сгенерированных слов, в большинстве случаев от 12 до 24, которые представляют собой для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления доступа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают большой защиты и шифруются, что делает их безопасными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы жизненно важны для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить доступ к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете без труда создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не передавайте сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может привести к утере вашего криптоимущества.
Храните сид-фразу в безопасном месте. Используйте физически безопасные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить возможность доступа к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите другие методы защиты и двухфакторную верификацию для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом надежного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Слив посеянных фраз (seed phrases) является одной из наиболее обычных способов утечки личной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, почему они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, являются комбинацию слов, которая используется для создания или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые отражают собой ключ к вашему кошельку. Потеря или утечка сид фразы может приводить к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы представляют ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они могут получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу ничьему, даже если вам происходит, что это доверенное лицо или сервис.
Храните свою сид фразу в секурном и безопасном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная верификация, для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в разнообразных безопасных местах.
Заключение
Слив сид фраз является серьезной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
tadalafil 60
Структура бэклинков
После того как многочисленных обновлений поисковой системы G необходимо использовать разные варианты сортировки.
Сегодня есть способ привлечения внимания поисковых систем к вашему веб-сайту с помощью обратных ссылок.
Бэклинки не только эффективный инструмент продвижения, но и имеют органический трафик, прямых продаж с этих ресурсов скорее всего не будет, но переходы будут, и именно поеденического трафика мы тоже получаем.
Что в итоге получим на выходе:
Мы отображаем сайт поисковым системам с помощью обратных ссылок.
Получают естественные переходы на сайт, а это также сигнал поисковым системам о том, что ресурс используется людьми.
Как мы демонстрируем поисковым системам, что сайт ликвиден:
1 обратная ссылка делается на главную страницу, где основная информация.
Создаем обратные ссылки с использованием редиректов с доверенных сайтов.
Самое ВАЖНОЕ мы размещаем сайт на отдельном инструменте анализаторов сайтов, сайт попадает в кеш этих анализаторов, затем полученные ссылки мы размещаем в качестве редиректов на блогах, форумах, комментариях.
Это важное действие показывает поисковым системамКАРТУ САЙТА, так как анализаторы сайтов отображают всю информацию о сайтах со всеми ключевыми словами и заголовками и это очень ХОРОШО
buy generic cialis mastercard
сайт казино либет
where can i buy zithromax uk
online pharmacy search
top online pharmacy 247
казино либет
lee bet
http://amoxila.pro/# where can i get amoxicillin 500 mg
doxycycline prices: doxycycline 100 mg – doxycycline hyclate
neurontin 300 mg capsule neurontin 400mg neurontin 4 mg
https://novostroyzhkspb.ru/
target pharmacy online refills
what is sildenafil
azithromycin online usa
no rx pharmacy
ggg
هنا النص مع استخدام السبينتاكس:
“بنية الروابط الخلفية
بعد التحديثات العديدة لمحرك البحث G، تحتاج إلى تنفيذ خيارات ترتيب مختلفة.
هناك طريقة لجذب انتباه محركات البحث إلى موقعك على الويب باستخدام الروابط الخلفية.
الروابط الخلفية ليست فقط أداة فعالة للترويج، ولكن تمتلك أيضًا حركة مرور عضوية، والمبيعات المباشرة من هذه الموارد على الأرجح قد لا تكون كذلك، ولكن التحولات ستكون، وهي حركة المرور التي نحصل عليها أيضًا.
ما نكون عليه في النهاية في النهاية في الإخراج:
نعرض الموقع لمحركات البحث من خلال الروابط الخلفية.
2- نحصل على تحويلات عضوية إلى الموقع، وهي أيضًا إشارة لمحركات البحث أن المورد يستخدمه الناس.
كيف نظهر لمحركات البحث أن الموقع سائل:
1 يتم عمل صلة خلفي للصفحة الرئيسية حيث المعلومات الرئيسية
نقوم بعمل روابط خلفية من خلال عمليات إعادة توجيه المواقع الموثوقة
الأهم من ذلك أننا نضع الموقع على أداة منفصلة من أدوات تحليل المواقع، ويدخل الموقع في ذاكرة التخزين المؤقت لهذه المحللات، ثم الروابط المستلمة التي نضعها كإعادة توجيه على المدونات والمنتديات والتعليقات.
هذا الإجراء المهم يعرض لمحركات البحث خريطة الموقع، حيث تعرض أدوات تحليل المواقع جميع المعلومات عن المواقع مع جميع الكلمات الرئيسية والعناوين وهو أمر جيد جداً
جميع المعلومات عن خدماتنا على الموقع!
can i order prednisone: fast shipping prednisone – prednisone canada prices
https://doxycyclinea.online/# doxycycline 200 mg
price of prednisone tablets
200 mg doxycycline doxycycline pills doxycycline 150 mg
https://irongamers.ru/sale/
tintucnamdinh24h.com
Hongzhi 황제는 이미 도착했고 동시에 많은 대신이 궁전에 근무했습니다.
synthroid tablets uk
where to buy synthroid 1mg in canada
legitimate canadian online pharmacies
synthroid brand name cost
medication neurontin 300 mg: neurontin cap 300mg price – neurontin 200 mg
http://prednisoned.online/# prednisone 2 mg
azithromycin 500mg no prescription
娛樂城評價
Player娛樂城遊戲評測網 《娛樂城評價》分類專區,幫您整了出網路上各大線上娛樂城重點摘要,以便您快速了解各大娛樂城重點資訊。
錢盈娛樂城介紹
錢盈娛樂城於2022年成立,是一個專注於現金投注的線上遊戲平台,提供了包括體育賭博、真人百家樂、老虎機、彩票和電子遊戲等多樣化的遊戲選…
F1方程式娛樂城介紹
F1方程式娛樂城屬於小型線上娛樂城版,整體晚間非常簡陋而且含有諸多瑕疵以及不完善,首先奇怪的點在於完全沒有可以註冊的地方,我們這邊猜測…
CZ168娛樂城介紹
CZ168娛樂城在雖然在簡介中自稱有12年的經營時間,但是經過我們實際的調查以及訪問該品牌網頁後發現,並沒有任何12年前或是更近的資料…
包你發娛樂城介紹
包你發娛樂城是個很多明星都在代言的線上賭博平台,玩家在這裡是用虛擬貨幣來存款,算是那種幣商型的賭場。這個平台沒有直接的提款選項,玩家要…
富遊娛樂城介紹
隨著2024年的到來,最新的線上娛樂平台排行榜已經更新,這一次的排名綜合考慮了各種因素,包括體驗金、促銷活動、提款效率和遊戲多樣性,目…
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
九州娛樂城介紹
九州娛樂城
九州娛樂城,也被稱作LEO娛樂城,致力於打造一個既安全又方便、公平公正的高品質娛樂服務平台。我們的目標是創造全新的線上娛樂城體驗,普及化娛樂服務,並努力成為娛樂網站界的領頭羊。需要注意的是,九州娛樂城、LEO娛樂城和THA娛樂城實際上是同一家公司的不同名稱。
九州娛樂城簡介
推薦指數:★★★★★(5分)
品牌名稱 : 九州娛樂城(LEO娛樂城)
創立時間 : 2003年
賭場類型 : 現金版娛樂城
遊戲種類 : 真人百家樂、運彩投注、電子老虎機、六合彩球、棋牌遊戲、捕魚機遊戲
存取速度 : 存款90秒 / 提款5-10分
軟體下載 : 無APP下載,支援網頁投注
doxycycline vibramycin doxycycline hyc 100mg generic doxycycline
Квартиры в Екатеринбурге https://newflatekb.ru/ купить от официального застройщика
娛樂城排行
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
Player線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
Player如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
cenforce online fang – brand viagra online remote
Как сберечь свои личные данные: берегитесь утечек информации в интернете. Сегодня сохранение своих данных становится более насущной важной задачей. Одним из наиболее распространенных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в каком объеме обезопаситься от их утечки? Что такое «сит фразы»? «Сит фразы» — это синтезы слов или фраз, которые бывают используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как сохранить свои личные данные? Используйте непростые пароли. Избегайте использования несложных паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из вашего аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухэтапную аутентификацию (2FA). Это прибавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт по другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы сохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы охранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
brand cialis depress – brand cialis gentleman penisole abandon
valtrex cream price
Даркнет и сливы в Телеграме
Даркнет – это отрезок интернета, которая не индексируется обыденными поисковыми системами и требует уникальных программных средств для доступа. В даркнете существует множество скрытых сайтов, где можно найти различные товары и услуги, в том числе и нелегальные.
Одним из популярных способов распространения информации в даркнете является использование мессенджера Телеграм. Телеграм предоставляет возможность создания закрытых каналов и чатов, где пользователи могут обмениваться информацией, в том числе и нелегальной.
Сливы информации в Телеграме – это метод распространения конфиденциальной информации, такой как украденные данные, базы данных, персональные сведения и другие материалы. Эти сливы могут включать в себя информацию о кредитных картах, паролях, персональных сообщениях и даже фотографиях.
Сливы в Телеграме могут быть рискованными, так как они могут привести к утечке конфиденциальной информации и нанести ущерб репутации и финансовым интересам людей. Поэтому важно быть внимательным при обмене информацией в интернете и не доверять сомнительным источникам.
Вот кошельки с балансом у бота
Сид-фразы, или памятные фразы, представляют собой комбинацию слов, которая используется для генерации или восстановления кошелька криптовалюты. Эти фразы обеспечивают доступ к вашим криптовалютным средствам, поэтому их защищенное хранение и использование весьма важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы формируют набор случайными средствами сгенерированных слов, обычно от 12 до 24, которые предназначаются для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления входа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают высокой степенью защиты и шифруются, что делает их безопасными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы обязательны для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить возможность доступа к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете быстро создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не делитесь сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может привести к утере вашего криптоимущества.
Храните сид-фразу в секурном месте. Используйте физически защищенные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить возможность доступа к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите двухфакторную аутентификацию и другие методы защиты для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом защищенного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Слив посеянных фраз (seed phrases) является единственным из наиболее известных способов утечки личных информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, зачем они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, формируют комбинацию слов, которая используется для формирования или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые символизируют собой ключ к вашему кошельку. Потеря или утечка сид фразы может привести к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы представляют ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они могут получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу никому, даже если вам происходит, что это доверенное лицо или сервис.
Храните свою сид фразу в секурном и безопасном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная верификация, для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в разных безопасных местах.
Заключение
Слив сид фраз является важной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
brand cialis avenue – forzest guide penisole quarter
Как обезопасить свои данные: страхуйтесь от утечек информации в интернете. Сегодня сохранение своих данных становится более насущной важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере сберечься от их утечки? Что такое «сит фразы»? «Сит фразы» — это смеси слов или фраз, которые регулярно используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или дополнительные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, с помощью этих сит фраз. Как сохранить свои личные данные? Используйте непростые пароли. Избегайте использования легких паролей, которые просто угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не применяйте один и тот же пароль для разных сервисов. Используйте двухступенчатую аутентификацию (2FA). Это вводит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт по другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы сохранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
cialis daily 5 mg online
Сид-фразы, или мемориальные фразы, представляют собой комбинацию слов, которая используется для создания или восстановления кошелька криптовалюты. Эти фразы обеспечивают возможность доступа к вашим криптовалютным средствам, поэтому их секурное хранение и использование чрезвычайно важны для защиты вашего криптоимущества от утери и кражи.
Что такое сид-фразы кошельков криптовалют?
Сид-фразы представляют собой набор случайным образом сгенерированных слов, как правило от 12 до 24, которые предназначаются для создания уникального ключа шифрования кошелька. Этот ключ используется для восстановления входа к вашему кошельку в случае его повреждения или утери. Сид-фразы обладают высокой защиты и шифруются, что делает их секурными для хранения и передачи.
Зачем нужны сид-фразы?
Сид-фразы неотъемлемы для обеспечения безопасности и доступности вашего криптоимущества. Они позволяют восстановить доступ к кошельку в случае утери или повреждения физического устройства, на котором он хранится. Благодаря сид-фразам вы можете быстро создавать резервные копии своего кошелька и хранить их в безопасном месте.
Как обеспечить безопасность сид-фраз кошельков?
Никогда не раскрывайте сид-фразой ни с кем. Сид-фраза является вашим ключом к кошельку, и ее раскрытие может влечь за собой утере вашего криптоимущества.
Храните сид-фразу в секурном месте. Используйте физически надежные места, такие как банковские ячейки или специализированные аппаратные кошельки, для хранения вашей сид-фразы.
Создавайте резервные копии сид-фразы. Регулярно создавайте резервные копии вашей сид-фразы и храните их в разных безопасных местах, чтобы обеспечить доступ к вашему кошельку в случае утери или повреждения.
Используйте дополнительные меры безопасности. Включите другие методы защиты и двухфакторную аутентификацию для своего кошелька криптовалюты, чтобы обеспечить дополнительный уровень безопасности.
Заключение
Сид-фразы кошельков криптовалют являются ключевым элементом секурного хранения криптоимущества. Следуйте рекомендациям по безопасности, чтобы защитить свою сид-фразу и обеспечить безопасность своих криптовалютных средств.
Криптокошельки с балансом: зачем их покупают и как использовать
В мире криптовалют все расширяющуюся популярность приобретают криптокошельки с предустановленным балансом. Это индивидуальные кошельки, которые уже содержат определенное количество криптовалюты на момент покупки. Но зачем люди приобретают такие кошельки, и как правильно использовать их?
Почему покупают криптокошельки с балансом?
Удобство: Криптокошельки с предустановленным балансом предлагаются как готовое решение для тех, кто хочет быстро начать пользоваться криптовалютой без необходимости покупки или обмена на бирже.
Подарок или награда: Иногда криптокошельки с балансом используются как подарок или награда в рамках акций или маркетинговых кампаний.
Анонимность: При покупке криптокошелька с балансом нет запроса предоставлять личные данные, что может быть важно для тех, кто ценит анонимность.
Как использовать криптокошелек с балансом?
Проверьте безопасность: Убедитесь, что кошелек безопасен и не подвержен взлому. Проверьте репутацию продавца и источник приобретения кошелька.
Переведите средства на другой кошелек: Если вы хотите долгосрочно хранить криптовалюту, рекомендуется перевести средства на более безопасный или комфортный для вас кошелек.
Не храните все средства на одном кошельке: Для обеспечения безопасности рекомендуется распределить средства между несколькими кошельками.
Будьте осторожны с фишингом и мошенничеством: Помните, что мошенники могут пытаться обмануть вас, предлагая криптокошельки с балансом с целью получения доступа к вашим средствам.
Заключение
Криптокошельки с балансом могут быть удобным и быстрым способом начать пользоваться криптовалютой, но необходимо помнить о безопасности и осторожности при их использовании.Выбор и приобретение криптокошелька с балансом – это серьезный шаг, который требует внимания к деталям и осознанного подхода.”
слив сид фраз
Слив мнемонических фраз (seed phrases) является одним из наиболее обычных способов утечки личной информации в мире криптовалют. В этой статье мы разберем, что такое сид фразы, по какой причине они важны и как можно защититься от их утечки.
Что такое сид фразы?
Сид фразы, или мнемонические фразы, составляют комбинацию слов, которая используется для формирования или восстановления кошелька криптовалюты. Обычно сид фраза состоит из 12 или 24 слов, которые отражают собой ключ к вашему кошельку. Потеря или утечка сид фразы может вести к потере доступа к вашим криптовалютным средствам.
Почему важно защищать сид фразы?
Сид фразы представляют ключевым элементом для надежного хранения криптовалюты. Если злоумышленники получат доступ к вашей сид фразе, они сумеют получить доступ к вашему кошельку и украсть все средства.
Как защититься от утечки сид фраз?
Никогда не передавайте свою сид фразу ничьему, даже если вам похоже, что это проверенное лицо или сервис.
Храните свою сид фразу в секурном и надежном месте. Рекомендуется использовать аппаратные кошельки или специальные программы для хранения сид фразы.
Используйте дополнительные методы защиты, такие как двухфакторная аутентификация (2FA), для усиления безопасности вашего кошелька.
Регулярно делайте резервные копии своей сид фразы и храните их в разнообразных безопасных местах.
Заключение
Слив сид фраз является существенной угрозой для безопасности владельцев криптовалют. Понимание важности защиты сид фразы и принятие соответствующих мер безопасности помогут вам избежать потери ваших криптовалютных средств. Будьте бдительны и обеспечивайте надежную защиту своей сид фразы
zestoretic medication
Курсовые и дипломные работы https://newflatekb.ru/ на заказ. Выполняем любые типы работ онлайн в короткие сроки по выгодным ценам для студентов.
how much is valtrex
doxycycline hyc: doxycycline prices – buy doxycycline online uk
metformin canada price
https://prednisoned.online/# prednisone purchase online
happy family canadian pharmaceuticals online
amoxicillin 250 mg price in india order amoxicillin 500mg amoxicillin without a doctors prescription
cheapest pharmacy to fill prescriptions without insurance
Качественное написание курсовой работы https://courseworkmsk.ru/ на заказ. Низкие цены и антиплагиат от 70%. Точно в срок. Гарантия высокой оценки, бесплатные доработки.
kantorbola
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
canadian pharmacy no scripts
synthroid 150 mcg tablet
generic valtrex online pharmacy
Качественное написание курсовой работы https://reshayubystro.ru/ на заказ. Низкие цены и антиплагиат от 70%. Точно в срок. Гарантия высокой оценки, бесплатные доработки.
buy amoxicillin 500mg online: amoxicillin 500mg capsules uk – amoxicillin generic
http://amoxila.pro/# amoxicillin 825 mg
prednisone 54 can you buy prednisone in canada prednisone prescription drug
medication lisinopril 20 mg
It is very comforting to see that others are suffering from the same problem as you, wow!
medical pharmacy south
Написание рефератов https://pishureferat.ru/ на заказ качественно и в срок. Низкая цена и проверка на антиплагиат. Доработка по ТЗ бесплатно, проверка на антиплагиат.
game1kb.com
“그만해!” Hongzhi 황제는 확신했습니다. 완전히 확신했습니다.
Kantorbola adalah situs slot gacor terbaik di indonesia , kunjungi situs RTP kantor bola untuk mendapatkan informasi akurat slot dengan rtp diatas 95% . Kunjungi juga link alternatif kami di kantorbola77 dan kantorbola99 .
best price metformin
prednisone india
mexican drugstore online: buying from online mexican pharmacy – mexican pharmaceuticals online
Купить качественный отчет https://practicereport.ru/ по учебной, производственной и преддипломной практике, срок за 7 дней. Заказать отчет по практике с гарантией.
prescription medicine lisinopril
no rx pharmacy
generic metformin
0.025 mg synthroid
mexico pharmacy medication from mexico pharmacy mexican pharmaceuticals online
taurus118
tadalafil online uk
synthroid 12.5 mg
tadalafil online from canada
prednisone 10 mg generic
synthroid 75 mcg cost
https://mexicanpharmacy1st.online/# medicine in mexico pharmacies
Дієти онлайн-журнал для стильних, модних та впевнених у собі представниць прекрасної статі. Любов, відносини, краса, здоров’я, кар’єра, діти, подорожі, рецепти – все це ви знайдете тут.
buying prescription drugs in mexico: buying from online mexican pharmacy – mexican pharmaceuticals online
Жіноче здоров’я онлайн-журнал для стильних, модних та впевнених у собі представниць прекрасної статі. Любов, відносини, краса, здоров’я, кар’єра, діти, подорожі, рецепти – все це ви знайдете тут.
tadalafil soft tabs
synthroid for sale
Психологічна підтримка онлайн-журнал для стильних, модних та впевнених у собі представниць прекрасної статі. Любов, відносини, краса, здоров’я, кар’єра, діти, подорожі, рецепти – все це ви знайдете тут.
pharmacy online shopping usa
mexico drug stores pharmacies: buying prescription drugs in mexico online – reputable mexican pharmacies online
can i buy metformin over the counter in singapore
zythromax
п»їbest mexican online pharmacies mexico drug stores pharmacies mexican drugstore online
valtrex 2 g
cialis soft tabs pills heir – tadarise bolt viagra oral jelly feel
https://mexicanpharmacy1st.com/# purple pharmacy mexico price list
valtrex 1000 mg cost
best mexican online pharmacies: buying prescription drugs in mexico – mexican mail order pharmacies
valtrex cream
buying lisinopril online
medication from mexico pharmacy mexico drug stores pharmacies п»їbest mexican online pharmacies
prednisone 54899
заказать дипломную работу https://diplomworkmsk.ru/ с гарантией.
https://mexicanpharmacy1st.online/# п»їbest mexican online pharmacies
pharmacies in mexico that ship to usa: mexico pharmacy – buying prescription drugs in mexico online
40 mg prednisone daily
valtrex tablets price
Модний стиль онлайн-журнал для стильних, модних та впевнених у собі представниць прекрасної статі. Любов, відносини, краса, здоров’я, кар’єра, діти, подорожі, рецепти – все це ви знайдете тут.
azithromycin z-pack
buying from online mexican pharmacy п»їbest mexican online pharmacies mexican rx online
mikaspa.com
이런 엄청난 타격이 일본해적 문제를 완전히 해결하는 근본적인 방법이다.
prednisone canada prescription
synthroid 0.075 mcg
Thanks for thr great article!
https://mexicanpharmacy1st.com/# buying from online mexican pharmacy
brand cialis jaw – brand levitra connect penisole sun
best mexican online pharmacies: medicine in mexico pharmacies – mexican mail order pharmacies
brand cialis pony – forzest pause penisole total
brand name synthroid cheap
pharmacies in mexico that ship to usa п»їbest mexican online pharmacies mexico drug stores pharmacies
Оказание услуг в решении задач https://reshatelizadach.ru/ для студентов. Четко оговоренные сроки, сопровождение до проверки, недорого! У нас вы можете заказать срочное решение задач по хорошим ценам.
https://mexicanpharmacy1st.shop/# mexican mail order pharmacies
mexican border pharmacies shipping to usa: mexico pharmacies prescription drugs – purple pharmacy mexico price list
20 mg of prednisone
best online pharmacies in mexico mexico pharmacy reputable mexican pharmacies online
online pharmacy china
http://mexicanpharmacy1st.com/# buying prescription drugs in mexico
lisinopril 10 12.5 mg tablets
reputable mexican pharmacies online: medicine in mexico pharmacies – mexico pharmacies prescription drugs
Купить реферат https://zakazhireferat.ru/ на заказ с гарантией. Надежные услуги по написанию рефератов. Заказать реферат по цене от 500 руб.
prednisone online without a prescription
can i buy metformin in mexico
mexican pharmacies online drugs
cost of prednisone prescription
pharmacies in mexico that ship to usa mexico pharmacy pharmacies in mexico that ship to usa
pharmacy online shopping usa
Купить отчет оп практике https://praktikotchet.ru/ по доступной цене с гарантией.
cialis soft tabs online surprise – viagra oral jelly online snore viagra oral jelly online catch
lisinopril australia
https://mexicanpharmacy1st.com/# mexican border pharmacies shipping to usa
can you buy synthroid in mexico
mexican drugstore online: mexican online pharmacies prescription drugs – pharmacies in mexico that ship to usa
best price for synthroid
услуги грузчиков https://gruzchikon.ru/ по доступной цене с гарантией.
Свадебный фотограф https://alexanderkiselev.ru/ в Москве.
onair2tv.com
빨래, 조명, 요리, 심지어 옷 수선까지 모든 일에 능숙해졌습니다.
mexico pharmacies prescription drugs medicine in mexico pharmacies mexican drugstore online
metformin canadian pharmacy
where can you buy cialis cheap
mexican online pharmacies prescription drugs: best online pharmacies in mexico – mexican border pharmacies shipping to usa
rikvip
Rikvip Club: Trung Tâm Giải Trí Trực Tuyến Hàng Đầu tại Việt Nam
Rikvip Club là một trong những nền tảng giải trí trực tuyến hàng đầu tại Việt Nam, cung cấp một loạt các trò chơi hấp dẫn và dịch vụ cho người dùng. Cho dù bạn là người dùng iPhone hay Android, Rikvip Club đều có một cái gì đó dành cho mọi người. Với sứ mạng và mục tiêu rõ ràng, Rikvip Club luôn cố gắng cung cấp những sản phẩm và dịch vụ tốt nhất cho khách hàng, tạo ra một trải nghiệm tiện lợi và thú vị cho người chơi.
Sứ Mạng và Mục Tiêu của Rikvip
Từ khi bắt đầu hoạt động, Rikvip Club đã có một kế hoạch kinh doanh rõ ràng, luôn nỗ lực để cung cấp cho khách hàng những sản phẩm và dịch vụ tốt nhất và tạo điều kiện thuận lợi nhất cho người chơi truy cập. Nhóm quản lý của Rikvip Club có những mục tiêu và ước muốn quyết liệt để biến Rikvip Club thành trung tâm giải trí hàng đầu trong lĩnh vực game đổi thưởng trực tuyến tại Việt Nam và trên toàn cầu.
Trải Nghiệm Live Casino
Rikvip Club không chỉ nổi bật với sự đa dạng của các trò chơi đổi thưởng mà còn với các phòng trò chơi casino trực tuyến thu hút tất cả người chơi. Môi trường này cam kết mang lại trải nghiệm chuyên nghiệp với tính xanh chín và sự uy tín không thể nghi ngờ. Đây là một sân chơi lý tưởng cho những người yêu thích thách thức bản thân và muốn tận hưởng niềm vui của chiến thắng. Với các sảnh cược phổ biến như Roulette, Sic Bo, Dragon Tiger, người chơi sẽ trải nghiệm những cảm xúc độc đáo và đặc biệt khi tham gia vào casino trực tuyến.
Phương Thức Thanh Toán Tiện Lợi
Rikvip Club đã được trang bị những công nghệ thanh toán tiên tiến ngay từ đầu, mang lại sự thuận tiện và linh hoạt cho người chơi trong việc sử dụng hệ thống thanh toán hàng ngày. Hơn nữa, Rikvip Club còn tích hợp nhiều phương thức giao dịch khác nhau để đáp ứng nhu cầu đa dạng của người chơi: Chuyển khoản Ngân hàng, Thẻ cào, Ví điện tử…
Kết Luận
Tóm lại, Rikvip Club không chỉ là một nền tảng trò chơi, mà còn là một cộng đồng nơi người chơi có thể tụ tập để tận hưởng niềm vui của trò chơi và cảm giác hồi hộp khi chiến thắng. Với cam kết cung cấp những sản phẩm và dịch vụ tốt nhất, Rikvip Club chắc chắn là điểm đến lý tưởng cho những người yêu thích trò chơi trực tuyến tại Việt Nam và cả thế giới.
synthroid 275 mcg
metformin online buy
synthroid 0.088 mg tab
https://womenran.com/
mexican drugstore online reputable mexican pharmacies online mexico pharmacies prescription drugs
https://mexicanpharmacy1st.shop/# pharmacies in mexico that ship to usa
buying from online mexican pharmacy: mexican mail order pharmacies – medication from mexico pharmacy
synthroid 250
valtrex cream
https://artmixdeco.ru/
lisinopril cost lisinopril 5 mg over the counter lisinopril medication otc
Asacol
Rikvip Club: Trung Tâm Giải Trí Trực Tuyến Hàng Đầu tại Việt Nam
Rikvip Club là một trong những nền tảng giải trí trực tuyến hàng đầu tại Việt Nam, cung cấp một loạt các trò chơi hấp dẫn và dịch vụ cho người dùng. Cho dù bạn là người dùng iPhone hay Android, Rikvip Club đều có một cái gì đó dành cho mọi người. Với sứ mạng và mục tiêu rõ ràng, Rikvip Club luôn cố gắng cung cấp những sản phẩm và dịch vụ tốt nhất cho khách hàng, tạo ra một trải nghiệm tiện lợi và thú vị cho người chơi.
Sứ Mạng và Mục Tiêu của Rikvip
Từ khi bắt đầu hoạt động, Rikvip Club đã có một kế hoạch kinh doanh rõ ràng, luôn nỗ lực để cung cấp cho khách hàng những sản phẩm và dịch vụ tốt nhất và tạo điều kiện thuận lợi nhất cho người chơi truy cập. Nhóm quản lý của Rikvip Club có những mục tiêu và ước muốn quyết liệt để biến Rikvip Club thành trung tâm giải trí hàng đầu trong lĩnh vực game đổi thưởng trực tuyến tại Việt Nam và trên toàn cầu.
Trải Nghiệm Live Casino
Rikvip Club không chỉ nổi bật với sự đa dạng của các trò chơi đổi thưởng mà còn với các phòng trò chơi casino trực tuyến thu hút tất cả người chơi. Môi trường này cam kết mang lại trải nghiệm chuyên nghiệp với tính xanh chín và sự uy tín không thể nghi ngờ. Đây là một sân chơi lý tưởng cho những người yêu thích thách thức bản thân và muốn tận hưởng niềm vui của chiến thắng. Với các sảnh cược phổ biến như Roulette, Sic Bo, Dragon Tiger, người chơi sẽ trải nghiệm những cảm xúc độc đáo và đặc biệt khi tham gia vào casino trực tuyến.
Phương Thức Thanh Toán Tiện Lợi
Rikvip Club đã được trang bị những công nghệ thanh toán tiên tiến ngay từ đầu, mang lại sự thuận tiện và linh hoạt cho người chơi trong việc sử dụng hệ thống thanh toán hàng ngày. Hơn nữa, Rikvip Club còn tích hợp nhiều phương thức giao dịch khác nhau để đáp ứng nhu cầu đa dạng của người chơi: Chuyển khoản Ngân hàng, Thẻ cào, Ví điện tử…
Kết Luận
Tóm lại, Rikvip Club không chỉ là một nền tảng trò chơi, mà còn là một cộng đồng nơi người chơi có thể tụ tập để tận hưởng niềm vui của trò chơi và cảm giác hồi hộp khi chiến thắng. Với cam kết cung cấp những sản phẩm và dịch vụ tốt nhất, Rikvip Club chắc chắn là điểm đến lý tưởng cho những người yêu thích trò chơi trực tuyến tại Việt Nam và cả thế giới.
amoxicillin buy online us
https://mydw.ru/
where to buy accutane
neurontin 600 mg capsule: neurontin 600 mg pill – gabapentin 300
http://lisinopril.club/# 100 mg lisinopril
cialis soft tabs appear – caverta online scientific viagra oral jelly online surround
zovirax nz
해외선물의 시작 골드리치와 동행하세요.
골드리치는 오랜기간 회원분들과 더불어 선물시장의 진로을 함께 동행해왔으며, 고객분들의 안전한 자금운용 및 알찬 이익률을 향해 항상 전력을 기울이고 있습니다.
무엇때문에 20,000+인 넘게이 골드리치와 투자하나요?
신속한 대응: 편리하고 빠른속도의 프로세스를 제공하여 모두 용이하게 이용할 수 있습니다.
보안 프로토콜: 국가당국에서 채택한 최상의 등급의 보안체계을 적용하고 있습니다.
스마트 인가: 전체 거래정보은 암호처리 가공되어 본인 외에는 아무도 누구도 정보를 확인할 수 없습니다.
안전 수익률 제공: 위험 부분을 감소시켜, 더욱 더 확실한 수익률을 제공하며 그에 따른 리포트를 제공합니다.
24 / 7 지속적인 고객센터: 연중무휴 24시간 즉각적인 지원을 통해 회원분들을 온전히 서포트합니다.
함께하는 협력사: 골드리치는 공기업은 물론 금융권들 및 다양한 협력사와 공동으로 걸어오고.
외국선물이란?
다양한 정보를 알아보세요.
해외선물은 외국에서 거래되는 파생상품 중 하나로, 명시된 기초자산(예시: 주식, 화폐, 상품 등)을 바탕로 한 옵션계약 계약을 말합니다. 기본적으로 옵션은 지정된 기초자산을 미래의 특정한 시점에 정해진 금액에 사거나 팔 수 있는 자격을 제공합니다. 외국선물옵션은 이러한 옵션 계약이 국외 마켓에서 거래되는 것을 의미합니다.
해외선물은 크게 매수 옵션과 풋 옵션으로 나뉩니다. 매수 옵션은 명시된 기초자산을 미래에 일정 금액에 사는 권리를 제공하는 반면, 매도 옵션은 지정된 기초자산을 미래에 일정 금액에 팔 수 있는 권리를 허락합니다.
옵션 계약에서는 미래의 명시된 날짜에 (만기일이라 불리는) 정해진 금액에 기초자산을 매수하거나 매도할 수 있는 권리를 보유하고 있습니다. 이러한 금액을 행사 가격이라고 하며, 종료일에는 해당 권리를 행사할지 여부를 판단할 수 있습니다. 따라서 옵션 계약은 거래자에게 미래의 가격 변동에 대한 안전장치나 이익 창출의 기회를 허락합니다.
외국선물은 시장 참가자들에게 다양한 운용 및 차익거래 기회를 제공, 환율, 상품, 주식 등 다양한 자산유형에 대한 옵션 계약을 망라할 수 있습니다. 거래자는 매도 옵션을 통해 기초자산의 하락에 대한 보호를 받을 수 있고, 콜 옵션을 통해 상승장에서의 수익을 타깃팅할 수 있습니다.
해외선물 거래의 원리
행사 가격(Exercise Price): 국외선물에서 행사 금액은 옵션 계약에 따라 명시된 가격으로 계약됩니다. 종료일에 이 가격을 기준으로 옵션을 행사할 수 있습니다.
종료일(Expiration Date): 옵션 계약의 종료일은 옵션의 실행이 불가능한 최종 일자를 뜻합니다. 이 날짜 이후에는 옵션 계약이 소멸되며, 더 이상 거래할 수 없습니다.
풋 옵션(Put Option)과 콜 옵션(Call Option): 풋 옵션은 기초자산을 지정된 가격에 팔 수 있는 권리를 부여하며, 콜 옵션은 기초자산을 특정 가격에 사는 권리를 제공합니다.
프리미엄(Premium): 국외선물 거래에서는 옵션 계약에 대한 옵션료을 납부해야 합니다. 이는 옵션 계약에 대한 비용으로, 마켓에서의 수요와 공급량에 따라 변화됩니다.
행사 전략(Exercise Strategy): 거래자는 종료일에 옵션을 행사할지 여부를 선택할 수 있습니다. 이는 시장 환경 및 거래 전략에 따라 상이하며, 옵션 계약의 이익을 극대화하거나 손해를 최소화하기 위해 판단됩니다.
마켓 리스크(Market Risk): 국외선물 거래는 마켓의 변동성에 효과을 받습니다. 가격 변동이 예상치 못한 진로으로 일어날 경우 손실이 발생할 수 있으며, 이러한 시장 위험요인를 감소하기 위해 투자자는 전략을 수립하고 투자를 계획해야 합니다.
골드리치와 함께하는 국외선물은 보장된 확신할 수 있는 운용을 위한 최적의 선택입니다. 회원님들의 투자를 뒷받침하고 안내하기 위해 우리는 전력을 기울이고 있습니다. 공동으로 더 나은 미래를 지향하여 나아가요.
lisinopril 240 price of lisinopril 5mg lisinopril 25
buy lioresal online
Euro 2024
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
Сайт https://glamour.kyiv.ua/ – це онлайн-журнал, який присвячений моді, красі, стилю та життю знаменитостей. Він пропонує свіжі новини, поради з моди і краси, інтерв’ю з відомими особистостями та багато іншого для стильних та модних людей.
zestoretic canada: lisinopril 10 mg tablet – lisinopril 102
neurontin cost in canada neurontin prescription cost neurontin 100mg caps
Сайт https://medicalanswers.com.ua/ – це онлайн-ресурс, який пропонує інформацію з медицини, здоров’я та добробуту. Тут ви знайдете статті, поради та відповіді на питання з різних медичних тем, які допоможуть вам зберегти здоров’я та бути освіченим щодо медичних питань.
UEFA Euro 2024 Sân Chơi Bóng Đá Hấp Dẫn Nhất Của Châu Âu
Euro 2024 là sự kiện bóng đá lớn nhất của châu Âu, không chỉ là một giải đấu mà còn là một cơ hội để các quốc gia thể hiện tài năng, sự đoàn kết và tinh thần cạnh tranh.
Euro 2024 hứa hẹn sẽ mang lại những trận cầu đỉnh cao và kịch tính cho người hâm mộ trên khắp thế giới. Cùng tìm hiểu các thêm thông tin hấp dẫn về giải đấu này tại bài viết dưới đây, gồm:
Nước chủ nhà
Đội tuyển tham dự
Thể thức thi đấu
Thời gian diễn ra
Sân vận động
Euro 2024 sẽ được tổ chức tại Đức, một quốc gia có truyền thống vàng của bóng đá châu Âu.
Đức là một đất nước giàu có lịch sử bóng đá với nhiều thành công quốc tế và trong những năm gần đây, họ đã thể hiện sức mạnh của mình ở cả mặt trận quốc tế và câu lạc bộ.
Việc tổ chức Euro 2024 tại Đức không chỉ là một cơ hội để thể hiện năng lực tổ chức tuyệt vời mà còn là một dịp để giới thiệu văn hóa và sức mạnh thể thao của quốc gia này.
Đội tuyển tham dự giải đấu Euro 2024
Euro 2024 sẽ quy tụ 24 đội tuyển hàng đầu từ châu Âu. Các đội tuyển này sẽ là những đại diện cho sự đa dạng văn hóa và phong cách chơi bóng đá trên khắp châu lục.
Các đội tuyển hàng đầu như Đức, Pháp, Tây Ban Nha, Bỉ, Italy, Anh và Hà Lan sẽ là những ứng viên nặng ký cho chức vô địch.
Trong khi đó, các đội tuyển nhỏ hơn như Iceland, Wales hay Áo cũng sẽ mang đến những bất ngờ và thách thức cho các đối thủ.
Các đội tuyển tham dự được chia thành 6 bảng đấu, gồm:
Bảng A: Đức, Scotland, Hungary và Thuỵ Sĩ
Bảng B: Tây Ban Nha, Croatia, Ý và Albania
Bảng C: Slovenia, Đan Mạch, Serbia và Anh
Bảng D: Ba Lan, Hà Lan, Áo và Pháp
Bảng E: Bỉ, Slovakia, Romania và Ukraina
Bảng F: Thổ Nhĩ Kỳ, Gruzia, Bồ Đào Nha và Cộng hoà Séc
해외선물
해외선물의 출발 골드리치증권와 동행하세요.
골드리치는 장구한기간 투자자분들과 더불어 선물마켓의 길을 함께 여정을했습니다, 투자자분들의 확실한 투자 및 알찬 수익성을 향해 항상 최선을 다하고 있습니다.
어째서 20,000+명 이상이 골드리치증권와 투자하나요?
신속한 대응: 간단하며 빠른속도의 프로세스를 마련하여 어느누구라도 용이하게 사용할 수 있습니다.
안전 프로토콜: 국가기관에서 채택한 높은 등급의 보안체계을 채택하고 있습니다.
스마트 인증: 전체 거래내용은 부호화 가공되어 본인 외에는 아무도 누구도 내용을 확인할 수 없습니다.
확실한 이익률 제공: 리스크 부분을 낮추어, 보다 더 확실한 수익률을 제시하며 그에 따른 리포트를 제공합니다.
24 / 7 상시 고객센터: 연중무휴 24시간 신속한 서비스를 통해 투자자분들을 모두 지원합니다.
함께하는 협력사: 골드리치증권는 공기업은 물론 금융계들 및 다수의 협력사와 함께 여정을 했습니다.
국외선물이란?
다양한 정보를 참고하세요.
국외선물은 외국에서 거래되는 파생상품 중 하나로, 특정 기초자산(예시: 주식, 화폐, 상품 등)을 기초로 한 옵션계약 계약을 말합니다. 근본적으로 옵션은 지정된 기초자산을 향후의 어떤 시점에 일정 가격에 사거나 매도할 수 있는 권리를 부여합니다. 외국선물옵션은 이러한 옵션 계약이 해외 시장에서 거래되는 것을 지칭합니다.
국외선물은 크게 콜 옵션과 매도 옵션으로 나뉩니다. 콜 옵션은 명시된 기초자산을 미래에 일정 금액에 매수하는 권리를 제공하는 반면, 매도 옵션은 특정 기초자산을 미래에 정해진 가격에 매도할 수 있는 권리를 부여합니다.
옵션 계약에서는 미래의 특정 일자에 (만기일이라 불리는) 정해진 가격에 기초자산을 매수하거나 매도할 수 있는 권리를 가지고 있습니다. 이러한 금액을 행사 가격이라고 하며, 종료일에는 해당 권리를 행사할지 여부를 판단할 수 있습니다. 따라서 옵션 계약은 거래자에게 미래의 시세 변화에 대한 보호나 이익 창출의 기회를 제공합니다.
외국선물은 시장 참가자들에게 다양한 운용 및 차익거래 기회를 열어주며, 환율, 상품, 주식 등 다양한 자산유형에 대한 옵션 계약을 망라할 수 있습니다. 투자자는 매도 옵션을 통해 기초자산의 낙폭에 대한 안전장치를 받을 수 있고, 콜 옵션을 통해 상승장에서의 이익을 타깃팅할 수 있습니다.
외국선물 거래의 원리
행사 가격(Exercise Price): 해외선물에서 행사 가격은 옵션 계약에 따라 특정한 금액으로 약정됩니다. 만기일에 이 가격을 기준으로 옵션을 실현할 수 있습니다.
만기일(Expiration Date): 옵션 계약의 종료일은 옵션의 실행이 허용되지않는 최종 일자를 의미합니다. 이 날짜 다음에는 옵션 계약이 만료되며, 더 이상 거래할 수 없습니다.
풋 옵션(Put Option)과 콜 옵션(Call Option): 풋 옵션은 기초자산을 지정된 금액에 팔 수 있는 권리를 허락하며, 콜 옵션은 기초자산을 특정 가격에 사는 권리를 부여합니다.
프리미엄(Premium): 국외선물 거래에서는 옵션 계약에 대한 계약료을 납부해야 합니다. 이는 옵션 계약에 대한 가격으로, 마켓에서의 수요와 공급량에 따라 변경됩니다.
행사 전략(Exercise Strategy): 투자자는 만기일에 옵션을 실행할지 여부를 결정할 수 있습니다. 이는 시장 상황 및 거래 플랜에 따라 차이가있으며, 옵션 계약의 수익을 최대화하거나 손실을 최소화하기 위해 판단됩니다.
시장 리스크(Market Risk): 해외선물 거래는 마켓의 변화추이에 작용을 받습니다. 가격 변동이 예상치 못한 방향으로 일어날 경우 손실이 발생할 수 있으며, 이러한 시장 리스크를 축소하기 위해 투자자는 계획을 구축하고 투자를 설계해야 합니다.
골드리치와 동반하는 해외선물은 확실한 신뢰할 수 있는 투자를 위한 최상의 옵션입니다. 회원님들의 투자를 뒷받침하고 안내하기 위해 우리는 전력을 기울이고 있습니다. 함께 더 나은 미래를 향해 나아가요.
http://cytotec.xyz/# Misoprostol 200 mg buy online
baclofen 10mg tab cost
strattera generic cost
advair generic
lisinopril pills 10 mg: buy lisinopril 20 mg online united states – zestril 20 mg cost
Сайт https://ua-novosti.info/ – це новинний портал, який надає актуальні новини з України та світу. Тут ви знайдете інформацію про політику, економіку, культуру, спорт та інші сфери життя.
online isotretinoin pharmacy
viagra price in india
can i get generic clomid without insurance clomid pill cost clomid
https://lisinopril.club/# zestril discount
Сайт https://zhenskiy.kyiv.ua/ – це онлайн-ресурс, який присвячений жіночим темам та інтересам. Тут зібрана інформація про моду, красу, здоров’я, відносини, кулінарію та багато іншого, що може бути корисним та цікавим для сучасних жінок.
zithromax online uk
lioresal generic
buy cytotec online: cytotec buy online usa – buy cytotec
advair diskus costs
tintucnamdinh24h.com
하지만 이런 경험은 강화가 필요하지만 각 궁술의 득실을 연구할 필요가 있다.
Сайт https://womanlife.kyiv.ua/ – це онлайн-ресурс, який присвячений жіночому життю. Тут ви знайдете статті, поради та інформацію про моду, красу, стиль, відносини, здоров’я, кулінарію та багато іншого, спрямованого на розвиток, самовдосконалення та задоволення потреб сучасної жінки.
neurontin cap 300mg gabapentin buy neurontin for sale
buy doxycycline mexico
http://cytotec.xyz/# buy cytotec online fast delivery
лечение алкоголизма в уфе
buy cytotec: buy cytotec pills – cytotec buy online usa
where can i get clomid in south africa
vermox pharmacy
tretinoin 0.05 australia
neurontin 400 mg capsule neurontin canada online buy gabapentin online
buy generic furosemide
Строительство домов https://metaloopt.ru/, бань из бруса и бревна: по индивидуальным и типовым проектам в срок от 2-3 месяцев. Финская технология, гарантия 3 года на дома из бруса под ключ
http://lisinopril.club/# lisinopril 2.5 cost
buy dexamethasone online
cost of propecia without insurance: cheap propecia without rx – propecia without dr prescription
Сайт https://lady.kyiv.ua/ – це онлайн-ресурс, спеціалізований на темах, що цікавлять жінок. Тут зібрана інформація про моду, красу, стиль, здоров’я, відносини та багато іншого, що допоможе жінкам бути стильними, здоровими та щасливими.
cialis soft tabs online ultimate – valif pills lead viagra oral jelly online carriage
buy cytotec cytotec abortion pill buy misoprostol over the counter
azithromycin 500mg buy
ventolin uk
toradol for pain
Работа и заработок https://www.rabota-zarabotok.ru/, отзывы и информация. Проверка и реальные отзывы о сайтах заработка, черный список форекс брокеров, а также надежные варианты для заработка.
cialis generic in india
how to get cheap clomid for sale: cost cheap clomid no prescription – order generic clomid
buy generic accutane 40 mg
accutane sale uk
can i get generic clomid without prescription can i get clomid online clomid
dexamethasone 10 mg tablet
Сайт https://useti.org.ua/ – це новинний портал, який надає актуальні новини з України та світу. Тут ви знайдете інформацію про політику, економіку, культуру, спорт та інші сфери життя.
buy azithromycin online no prescription
where can i get provigil online
cost baclofen
valtrex over the counter australia
baclofen 20 mg pill
neurontin 400 mg capsules: neurontin 300mg – buy neurontin uk
buy lisinopril 20 mg online canada prinivil drug lisinopril generic over the counter
cost of prednisone 40 mg
darknet markets https://mydarkmarket.com/ – dark web sites tor markets 2024
where can you buy zovirax
Сайт https://novosti24.kyiv.ua/ – це новостний портал, який надає актуальні новини з різних сфер життя, включаючи політику, економіку, культуру, спорт та інші теми. Його основна мета – інформувати читачів про найважливіші події в Україні та за її межами.
https://36and6health.shop/# canadian pharmacy world coupon code
pharmacy accutane
generic effexor 225 mg cheapest
«Vita sene libertate nihil» — «Жизнь без свободы — ничто».
В нашем обществе, где аттестат является началом отличной карьеры в любом направлении, многие пытаются найти максимально быстрый путь получения качественного образования. Наличие официального документа об образовании сложно переоценить. Ведь именно он открывает дверь перед каждым человеком, который стремится начать профессиональную деятельность или учиться в любом институте.
Предлагаем оперативно получить этот необходимый документ. Вы сможете купить аттестат нового или старого образца, что будет выгодным решением для человека, который не смог завершить образование или утратил документ. Любой аттестат изготавливается с особой тщательностью, вниманием к мельчайшим элементам, чтобы в итоге получился 100% оригинальный документ.
Плюсы такого решения заключаются не только в том, что вы быстро получите свой аттестат. Весь процесс организовывается удобно и легко, с нашей поддержкой. Начав от выбора необходимого образца документа до грамотного заполнения персональной информации и доставки по России — все под абсолютным контролем опытных специалистов.
Для всех, кто ищет оперативный способ получить требуемый документ, наша компания предлагает отличное решение. Заказать аттестат – значит избежать продолжительного обучения и сразу переходить к достижению собственных целей: к поступлению в университет или к началу трудовой карьеры.
http://vsediplomu.ru/
«Vita sene libertate nihil» — «Жизнь без свободы — ничто».
эвакуатор для спецтехники
Abyssus abyssum invocat — Бездна взывает к бездне
furosemide india
https://cheapestindia.com/# online pharmacy india
эвакуатор в Минске стоимость
эвакуатор 24 7
Homo homini lupus est – человек человеку волк
Ad usum internum — Для внутреннего употребления.
A maximis ad minima — От большего к меньшему
http://36and6health.com/# cheapest pharmacy to get prescriptions filled
advair diskus 2018
amoxicillin 800
buy viagra new zealand
cost of accutane
can you buy dexamethasone over the counter
продвижение сайтов раскрутка сайтов продвижение сайтов раскрутка сайтов .
http://cheapestindia.com/# mail order pharmacy india
Доброго!
Приветствую вас, азартные друзья! Сегодня я поделюсь своими секретами выбора идеального онлайн-казино. Поверьте, я проверил не один десяток сайтов, прежде чем нашел свою игровую гавань!
Первое, на что стоит обратить внимание – это бездепозитные бонусы. Согласитесь, получить возможность играть на реальные деньги без вложений – заманчивая перспектива! Но будьте бдительны: читайте правила отыгрыша и не попадитесь на удочку мошенников.
Далее, убедитесь, что казино предлагает широкий выбор игровых автоматов и слотов. Лично я обожаю классические и современные 3D-слоты с захватывающими бонусными играми. А если есть возможность скачать официальное приложение казино на андроид, это вообще jackpot!
И конечно же, не забывайте про надежность и безопасность. Играйте только в лицензированных казино с шифрованием данных и быстрым выводом средств. Поверьте, нет ничего хуже, чем ждать свой честно выигранный приз неделями!
В общем, друзья, будьте внимательны, играйте с умом и не бойтесь рисковать! Помните: кто не рискует, тот не пьет шампанское! Удачи вам за игровыми столами и пусть фортуна всегда будет на вашей стороне!
xokke.ru
казино пополнение сбп
автоматы без регистрации и верификации
кабура казино
игровые автоматы приложение на андроид на деньги
скачать казино где можно платить через сим карту на андроид
Удачи!
tadacip 20 price in india
buy zithromax without presc
Привет!
Приветствую вас, азартные друзья! Сегодня я поделюсь своими секретами выбора идеального онлайн-казино. Поверьте, я проверил не один десяток сайтов, прежде чем нашел свою игровую гавань!
Первое, на что стоит обратить внимание – это бездепозитные бонусы. Согласитесь, получить возможность играть на реальные деньги без вложений – заманчивая перспектива! Но будьте бдительны: читайте правила отыгрыша и не попадитесь на удочку мошенников.
Далее, убедитесь, что казино предлагает широкий выбор игровых автоматов и слотов. Лично я обожаю классические и современные 3D-слоты с захватывающими бонусными играми. А если есть возможность скачать официальное приложение казино на андроид, это вообще jackpot!
И конечно же, не забывайте про надежность и безопасность. Играйте только в лицензированных казино с шифрованием данных и быстрым выводом средств. Поверьте, нет ничего хуже, чем ждать свой честно выигранный приз неделями!
В общем, друзья, будьте внимательны, играйте с умом и не бойтесь рисковать! Помните: кто не рискует, тот не пьет шампанское! Удачи вам за игровыми столами и пусть фортуна всегда будет на вашей стороне!
https://el-nose.ru/?p=10845
казино на реальные деньги андроид
казино на деньги casino андроид
мобильное казино ratingscasino002
olna casino
казино вывод сразу киви
Удачи!
canadian online pharmacy modafinil
vermox pills
Сайт https://news24.in.ua/ – це новинний веб-портал, який надає швидкий та достовірний доступ до актуальних новин з різних сфер життя, включаючи політику, економіку, культуру, спорт та інші важливі теми.
Ad futuram memoriam — На долгую память.
Amant alterna Camenae — Музам приятны перемежающиеся песни.
Amabilis insania — Приятное безумие.
Abiens, abi! — Уходя, уходи!
where to buy vermox in usa
azithromycin 10 pills
A casu ad casum — От случая к случаю.
A maximis ad minima — От большего к меньшему
Ad hoste maligno libera nos, Domine — Избави нас от лукавого, Боже.
Ad usum externum — Для внешнего употребления.
https://36and6health.com/# prescription drugs from canada
Veni, vidi, vici – пришел, увидел, победил
Будьте в курсе последних событий вместе с новостным порталом https://bnk.ua/. Наша команда профессиональных журналистов работает 24/7, чтобы вы получали самые важные новости из первых рук. Присоединяйтесь к нашей аудитории уже сегодня!
Amicus cognoscitur amore, more, ore, re — Друг познаётся по любви, нраву, лицу, деянию.
Здравствуйте!
Так что, друзья, активируйте все бонусы и промо, заряжайте мобильные гаджеты и вперед – к победам и крупным выигрышам! Ставки сделаны, ставок больше нет!
iuajp.ru
казино сайт
скачать казино на реальные деньги
онлайн казино миллион официальный сайт зеркало
мобильные казино
скачать приложение джой казино вин
Удачи!
Caveant consules! — Пусть консулы будут бдительны.
«Vita sene libertate nihil» — «Жизнь без свободы — ничто».
accutane price in india
modafinil pill
«Vita sene libertate nihil» — «Жизнь без свободы — ничто».
Ad gustum — По вкусу.
«Vita sene libertate nihil» — «Жизнь без свободы — ничто».
Aeternum vale — Прости навеки
Ad majorem Dei gloriam — К вящей славе Божией
Caveant consules! — Пусть консулы будут бдительны.
Министерство неджентльменских дел
Министерство неджентльменских дел
Здравствуйте!
Играть в казино с реальными дилерами — это как посетить вечеринку, где вас встречают старые друзья, которых вы никогда не видели. Обаятельные дилеры улыбаются вам через экран, и вы понимаете, что эта улыбка может стоить вам денег. Но ощущение реального присутствия добавляет игре пикантности. Вы чувствуете напряжение, когда дилер медленно раздает карты, и ваше сердце замирает — не от страха, а от предвкушения чуда. И знаете, в эти моменты я всегда думаю: “А вдруг сегодня мой день?” Это как смотреть фильм, где вы не только зритель, но и главный герой. Так что давайте играть, общаться и, конечно, выигрывать. Ведь как говорят: фортуна любит смелых!
https://slivmoney.ru/2024/05/10/Ключ-к-успеху-Лев-Казино-и-его-секреты
зеркала ко всем казино
казино миллион официальный сайт зеркало
регистрация в казино
миллион казино зеркало бездепозитный бонус
игровые автоматы с выводом денег на андроид
Удачи!
clomid price without insurance
Сайт https://dailynews.kyiv.ua/ – це онлайн-портал, який забезпечує свіжі та актуальні новини з Києва та інших регіонів України. Тут ви знайдете інформацію про події, політику, економіку, культуру, спорт та інші аспекти суспільного життя.
Министерство неджентльменских дел
Министерство неджентльменских дел
Министерство неджентльменских дел
Министерство неджентльменских дел
cenforce online themself – zenegra pills whence brand viagra online tidings
Министерство неджентльменских дел
Министерство неджентльменских дел
Министерство неджентльменских дел
Министерство неджентльменских дел
where to get accutane prescription
can you buy diflucan without a prescription
bestmanualpolesaw.com
매니저는 꼬리를 다리 사이에 끼고 바빠 필사적으로 나갔다.
Прямая трансляция: Александр Усик – Тайсон Фьюри
Усик – Фьюри: смотреть онлайн-трансляцию церемонии
https://cheapestandfast.shop/# meds online no prescription
Александр Усик — Тайсон Фьюри
Усик – Фьюри: онлайн-трансляция боя
Усик Фьюри – смотреть онлайн
azithromycin prices india
Александр Усик – Тайсон Фьюри. Смотреть онлайн
where to buy viagra with paypal
prednisone over the counter canada
vermox cost
Oleksandr Usyk vs Tyson Fury
Александр Усик — Тайсон Фьюри
Сайт https://dailynews.kyiv.ua/ – це онлайн-портал, який забезпечує свіжі та актуальні новини з Києва та інших регіонів України. Тут ви знайдете інформацію про події, політику, економіку, культуру, спорт та інші аспекти суспільного життя.
Александр Усик – Тайсон Фьюри. Смотреть онлайн
Александр Усик – Тайсон Фьюри. Смотреть онлайн LIVE
Александр Усик — Тайсон Фьюри, онлайн-трансляция
Бой Александр Усик — Тайсон Фьюри 18 мая 2024 года
furosemide online purchase
cialis 20mg india
https://cheapestindia.shop/# Online medicine home delivery
Greeting to Genio, the go-to invoice generator after small businesses and freelancers. We cause you tons invoice templates, including Microsoft Dominate and PDF formats, tailored to all industries. Explore our fraction featuring settled 300 customized invoice templates designed to cater to your distinctive responsibility needs.
https://www.genio.ac/invoice-templates/
Фуриоса: Хроники Безумного Макса
Фуриоса: Хроники Безумного Макса
can i buy provigil in mexico
Фуриоса: Хроники Безумного Макса
Фуриоса: Хроники Безумного Макса
how can i get propecia
Фуриоса: Хроники Безумного Макса
Будьте в курсе последних событий вместе с новостным порталом https://bnk.ua/. Наша команда профессиональных журналистов работает 24/7, чтобы вы получали самые важные новости из первых рук. Присоединяйтесь к нашей аудитории уже сегодня!
Фуриоса: Хроники Безумного Макса
Привет!
Если кто-то скажет вам, что серьезно относится к игровым автоматам на своем смартфоне, верьте — это я. Почему стоять у громоздкого автомата в полуподвальном зале, если можно устроиться с комфортом на своем диване с телефоном в руках, где каждый спин приносит чувство легкой восторженности? Плюс, загрузив приложение, вы можете платить даже через сим-карту, что за чудо техники? Но знаете, что еще лучше? Вывод денег прямо на вашу карту Тинькофф. Буквально “свайпнул — и богат”. О, а момент, когда вы выигрываете большой куш, и ваш телефон вибрирует от уведомлений — это как получить лайк от самой судьбы!
tongyeongkrmassage.ru
казино официальный скачать
unlim casino скачать на андроид приложение
скачать игровое казино на реальные деньги рубли
казино на русском
online casino официальный сайт
Удачи!
Фуриоса: Хроники Безумного Макса
Фуриоса: Хроники Безумного Макса
Фуриоса: Хроники Безумного Макса
azithromycin otc us
Психология
Психолог онлайн
Психоанализ
Сайт https://arguments.kyiv.ua/ – це інформаційний портал, який надає аналітику, коментарі та новини про події в Києві та Україні. Тут можна знайти різноманітні погляди на актуальні теми у політиці, економіці, культурі, суспільстві та інших сферах життя.
buy glucophage singapore
azithromycin 100 mg sale
dapoxetine struggle – levitra with dapoxetine border cialis with dapoxetine huge
Тут психолог
Психология
furosemide 30 mg
dapoxetine eyebrow – suhagra hasten cialis with dapoxetine shore
Психолог
Доброго!
Будьте внимательны к специальным ссылкам для загрузки приложений казино – они часто содержат уникальные промокоды, бонусы или другие выгодные предложения. Не упустите эту возможность увеличить свои шансы на крупный выигрыш! В заключение хочу сказать, что мир мобильных онлайн-казино открывает перед игроками массу преимуществ и возможностей. Используйте промокоды, бонусы, скачивайте приложения и наслаждайтесь азартом в любое время и в любом месте. Удачной игры!
caramaindingdongtogel.ru
регистрация по номеру телефона на сайте казино
интернет казино sms на андроид
пароль и логин от казино онлайн
скачать приложение казино
казино миллион официальный сайт онлайн казино
Удачи!
Сайт https://uapress.kyiv.ua/ – це СМИ платформа, яка надає новини, аналітику та репортажі з подій, що відбуваються в Києві та по всій Україні. Він охоплює різноманітні теми, включаючи політику, економіку, культуру, спорт та інші аспекти суспільного життя.
Психолог онлайн
Психотерапевт
Психотерапия
Психолог тут
Психолог
sildalis 120 mg order usa pharmacy
Психолог онлайн
Психолог
Сайт https://elegantwoman.kyiv.ua/ – це онлайн-ресурс, присвячений стильним жінкам. Тут ви знайдете поради з моди, краси, стилю та етикету, а також ідеї для створення елегантного образу та розвитку особистого стилю.
Замена венцов красноярск
Геракл24: Профессиональная Замена Фундамента, Венцов, Полов и Перемещение Домов
Организация Геракл24 профессионально занимается на выполнении комплексных работ по замене фундамента, венцов, настилов и передвижению зданий в городе Красноярск и за его пределами. Наш коллектив квалифицированных мастеров обеспечивает высокое качество выполнения всех видов восстановительных работ, будь то деревянные, с каркасом, кирпичные или бетонные конструкции здания.
Преимущества сотрудничества с Gerakl24
Навыки и знания:
Каждая задача осуществляются только высококвалифицированными экспертами, с обладанием многолетний опыт в направлении создания и ремонта зданий. Наши сотрудники знают свое дело и выполняют работу с высочайшей точностью и учетом всех деталей.
Полный спектр услуг:
Мы осуществляем все виды работ по ремонту и восстановлению зданий:
Реставрация фундамента: замена и укрепление фундамента, что обеспечивает долгий срок службы вашего дома и избежать проблем, связанные с оседанием и деформацией.
Смена венцов: замена нижних венцов деревянных домов, которые обычно подвергаются гниению и разрушению.
Установка новых покрытий: монтаж новых настилов, что существенно улучшает внешний вид и функциональность помещения.
Передвижение домов: качественный и безопасный перенос строений на другие участки, что обеспечивает сохранение строения и предотвращает лишние расходы на создание нового.
Работа с любыми видами зданий:
Древесные строения: реставрация и усиление деревянных элементов, защита от разрушения и вредителей.
Дома с каркасом: укрепление каркасов и замена поврежденных элементов.
Кирпичные дома: реставрация кирпичной кладки и усиление стен.
Дома из бетона: восстановление и укрепление бетонных структур, устранение трещин и повреждений.
Качество и прочность:
Мы применяем лишь качественные материалы и современное оборудование, что гарантирует долгий срок службы и надежность всех выполненных работ. Все проекты проходят тщательную проверку качества на всех этапах выполнения.
Персонализированный подход:
Каждому клиенту мы предлагаем индивидуальные решения, учитывающие все особенности и пожелания. Мы стремимся к тому, чтобы итог нашей работы полностью соответствовал ваши ожидания и требования.
Почему стоит выбрать Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы обеспечиваем выполнение всех проектов в сроки, оговоренные заранее и с соблюдением всех строительных норм и стандартов. Обратившись в Геракл24, вы можете не сомневаться, что ваше строение в надежных руках.
Мы готовы предоставить консультацию и ответить на все ваши вопросы. Контактируйте с нами, чтобы обсудить детали вашего проекта и узнать больше о наших услугах. Мы сохраним и улучшим ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Gerakl24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
https://cheapestmexico.com/# mexico drug stores pharmacies
10mg baclofen
vermox for sale uk
diflucan 150 mg price uk
diflucan men
augmentin 800
750 mg metformin
generic propecia uk
nolvadex to buy
order propecia online australia
200 mg effexor
Геракл24: Профессиональная Смена Основания, Венцов, Покрытий и Перемещение Домов
Фирма Gerakl24 занимается на предоставлении всесторонних сервисов по смене фундамента, венцов, полов и перемещению зданий в месте Красноярске и за пределами города. Наша команда опытных специалистов гарантирует превосходное качество выполнения всех видов реставрационных работ, будь то деревянные, каркасного типа, из кирпича или бетонные дома.
Достоинства работы с Gerakl24
Навыки и знания:
Каждая задача проводятся только высококвалифицированными мастерами, с многолетним большой стаж в области возведения и реставрации домов. Наши сотрудники знают свое дело и выполняют работу с максимальной точностью и вниманием к мелочам.
Всесторонний подход:
Мы предоставляем все виды работ по восстановлению и восстановлению зданий:
Реставрация фундамента: усиление и реставрация старого основания, что гарантирует долговечность вашего строения и избежать проблем, вызванные оседанием и деформацией.
Реставрация венцов: замена нижних венцов деревянных домов, которые наиболее часто подвергаются гниению и разрушению.
Замена полов: монтаж новых настилов, что кардинально улучшает визуальное восприятие и функциональность помещения.
Передвижение домов: безопасное и надежное перемещение зданий на новые локации, что помогает сохранить здание и предотвращает лишние расходы на создание нового.
Работа с любыми типами домов:
Деревянные дома: реставрация и усиление деревянных элементов, защита от разрушения и вредителей.
Каркасные дома: реставрация каркасов и смена поврежденных частей.
Кирпичные строения: восстановление кирпичной кладки и укрепление стен.
Дома из бетона: восстановление и укрепление бетонных структур, ремонт трещин и дефектов.
Качество и прочность:
Мы применяем лишь качественные материалы и новейшее оборудование, что гарантирует долговечность и прочность всех выполненных задач. Каждый наш проект проходят тщательную проверку качества на каждом этапе выполнения.
Личный подход:
Для каждого клиента мы предлагаем индивидуальные решения, учитывающие все особенности и пожелания. Мы стараемся, чтобы конечный результат полностью соответствовал вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы гарантируем выполнение всех задач в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Связавшись с Геракл24, вы можете быть спокойны, что ваше здание в надежных руках.
Мы всегда готовы проконсультировать и ответить на все ваши вопросы. Свяжитесь с нами, чтобы обсудить ваш проект и узнать о наших сервисах. Мы сохраним и улучшим ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Gerakl24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
https://cheapestmexico.com/# mexican mail order pharmacies
vermox online pharmacy
lyrica 225 mg capsule
buy diflucan 150mg
cenforce click – brand viagra online silent
free dark web https://mydarknetmarketlinks.com/ – darkmarket 2024 darknet websites
how to get tretinoin cream
where can you get nolvadex
номер телефона такси сколько стоит такси.
vermox canada
такси заказ эконом по телефону номер телефона такси.
azithromycin 200mg
doxycycline usa pharmacy
acne medication accept – acne medication brave acne treatment heal
https://cheapestandfast.com/# canadian pharmacy no prescription
такси номер недорогой такси недорого.
albuterol inhaler cost
azithromycin drug
заказ такси эконом такси новочеркасск.
lasix online no prescription
darknet markets 2024 https://mydarknetmarketlinks.com/ – dark web websites dark market onion
medicine ciprofloxacin 500mg
zovirax 5 cream
п»їFarmacia online migliore: farmacie online affidabili – comprare farmaci online con ricetta
where to buy vermox in canada
заказать такси в новочеркасске недорого эконом заказать такси в новочеркасске недорого эконом .
pharmacie en ligne livraison europe: Achat mГ©dicament en ligne fiable – pharmacie en ligne fiable
заказ такси заказ такси .
такси номер недорогой http://taksi-vyzvat.ru/ .
flomax price comparison
accutane medication
farmacias direct farmacia online envГo gratis farmacias direct
online apotheke deutschland: online apotheke – günstige online apotheke
buy lyrica no prescription
הפלטפורמה הווה אפליקציה מקובלת בישראל לקנייה של קנאביס באופן וירטואלי. זו מספקת ממשק נוח ובטוח לקנייה ולקבלת שילוחים מ פריטי קנאביס מגוונים. בכתבה זה נבחן עם העיקרון מאחורי האפליקציה, איך היא פועלת ומה היתרים מ השימוש בה.
מהי הפלטפורמה?
הפלטפורמה הווה שיטה לרכישת קנאביס דרך האפליקציה טלגראם. זו מבוססת מעל ערוצי תקשורת וקהילות טלגרם ייעודיות הקרויות ״כיווני טלגראס״, שבהם אפשר להרכיב מגוון פריטי קנאביס ולקבל אלו ישירות לשילוח. הערוצים אלו מאורגנים לפי איזורים גאוגרפיים, כדי לשפר את קבלתם של השילוחים.
כיצד זאת עובד?
התהליך פשוט יחסית. ראשית, צריך להצטרף לערוץ הטלגראס הנוגע לאזור המחיה. שם אפשר לצפות בתפריטים של המוצרים השונים ולהזמין עם הפריטים הרצויים. לאחר השלמת ההזמנה וסגירת התשלום, השליח יופיע בכתובת שנרשמה עם הארגז המוזמנת.
רוב ערוצי טלגראס מציעים מגוון רחב מ מוצרים – זנים של קנאביס, עוגיות, שתייה ועוד. בנוסף, אפשר לראות ביקורות של לקוחות שעברו לגבי איכות הפריטים והשירות.
יתרונות השימוש בטלגראס
יתרון עיקרי של הפלטפורמה הינו הנוחיות והפרטיות. ההזמנה והתהליך מתקיימים מרחוק מאיזשהו מקום, בלי נחיצות במפגש פנים אל פנים. בנוסף, הפלטפורמה מוגנת היטב ומבטיחה סודיות גבוהה.
נוסף על כך, מחירי הפריטים באפליקציה נוטות להיות תחרותיים, והשילוחים מגיעים במהירות ובהשקעה גבוהה. קיים אף מרכז תמיכה פתוח לכל שאלה או בעיית.
סיכום
טלגראס הווה שיטה חדשנית ויעילה לקנות מוצרי צמח הקנאביס במדינה. היא משלבת את הנוחות הדיגיטלית של היישומון הפופולרית, ועם המהירות והדיסקרטיות מ שיטת השילוח הישירה. ככל שהביקוש לצמח הקנאביס גובר, אפליקציות כמו זו צפויות להמשיך ולצמוח.
http://eufarmaciaonline.com/# farmacia online espaГ±a envГo internacional
проверка usdt trc20
Как охранять свои личные данные: берегитесь утечек информации в интернете. Сегодня охрана личных данных становится более насущной важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере обезопаситься от их утечки? Что такое «сит фразы»? «Сит фразы» — это сочетания слов или фраз, которые часто используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или другие конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как охранить свои личные данные? Используйте комплексные пароли. Избегайте использования несложных паролей, которые легко угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из вашего аккаунта. Не воспользуйтесь один и тот же пароль для разных сервисов. Используйте двухфакторную аутентификацию (2FA). Это вводит дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт путем другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы защитить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким вроде кража личной информации и финансовых потерь. Чтобы охранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
такси цена https://www.taksi-vyzvat.ru .
Примаков Е.М. и новые обзоры по психотерапии.
can i buy propecia over the counter uk
Оккультизм или магия и популярные книги по психотерапии.
how to get clomid australia
azithromycin tablets canada
farmacia online barcelona: п»їfarmacia online espaГ±a – farmacias direct
asthma medication curve – asthma medication murder inhalers for asthma mill
asthma treatment picture – asthma medication manage asthma medication yard
Свендсен Ларс и лучшие книги по психоанализу.
can i buy over the counter amoxicillin
האפליקציה מהווה פלטפורמה נפוצה בארץ לרכישת מריחואנה באופן אינטרנטי. היא נותנת ממשק משתמש נוח ובטוח לרכישה ולקבלת שילוחים של פריטי צמח הקנאביס מרובים. בכתבה זה נסקור עם הרעיון מאחורי האפליקציה, כיצד היא פועלת ומהם היתרונות של השימוש בזו.
מה זו האפליקציה?
הפלטפורמה היא דרך לרכישת צמח הקנאביס באמצעות האפליקציה טלגראם. היא נשענת על ערוצי תקשורת וקהילות טלגראם ספציפיות הקרויות ״כיווני טלגראס״, שבהם ניתן להזמין מגוון מוצרי צמח הקנאביס ולקבל אותם ישירות לשילוח. ערוצי התקשורת אלו מסודרים על פי אזורים גאוגרפיים, כדי להקל על קבלתם של המשלוחים.
כיצד זאת עובד?
התהליך פשוט יחסית. קודם כל, צריך להצטרף לערוץ טלגראס הנוגע לאזור המגורים. שם ניתן לצפות בתפריטים של המוצרים המגוונים ולהזמין עם המוצרים הרצויים. לאחר השלמת ההזמנה וסגירת התשלום, השליח יופיע בכתובת שצוינה ועמו החבילה שהוזמן.
מרבית ערוצי הטלגראס מספקים טווח רחב של פריטים – זנים של קנאביס, עוגיות, משקאות ועוד. כמו כן, ניתן לראות חוות דעת של צרכנים קודמים על רמת המוצרים והשירות.
יתרונות השימוש בפלטפורמה
יתרון עיקרי מ הפלטפורמה הוא הנוחיות והדיסקרטיות. ההזמנה וההכנות מתקיימים מרחוק מאיזשהו מקום, ללא נחיצות בהתכנסות פנים אל פנים. בנוסף, הפלטפורמה מאובטחת ביסודיות ומבטיחה סודיות גבוה.
מלבד על זאת, מחירי המוצרים באפליקציה נוטים להיות זולים, והשילוחים מגיעים במהירות ובמסירות רבה. יש גם מרכז תמיכה פתוח לכל שאלה או בעיית.
סיכום
האפליקציה היא דרך חדשנית ויעילה לרכוש מוצרי מריחואנה בישראל. זו משלבת את הנוחיות הדיגיטלית מ האפליקציה הפופולרית, ועם המהירות והפרטיות מ שיטת השילוח הישירות. ככל שהדרישה למריחואנה גובר, פלטפורמות בדוגמת טלגראס צפויות להמשיך ולהתפתח.
pharmacie en ligne france livraison internationale: pharmacie en ligne france – pharmacie en ligne sans ordonnance
farmacia online barata farmacias online seguras farmacia online envГo gratis
retin a 08
Thank you, Ample content!
tretinoin over the counter
заказать такси в новочеркасске по телефону заказать такси в новочеркасске по телефону .
generic lyrica 2019
vardenafil interactions
tadalafil 10mg price
gГјnstigste online apotheke: gГјnstigste online apotheke – eu apotheke ohne rezept
sildalis
הפלטפורמה היא תוכנה מקובלת בארץ לרכישת צמח הקנאביס בצורה וירטואלי. זו מספקת ממשק משתמש נוח ומאובטח לרכישה וקבלת שילוחים מ פריטי מריחואנה מגוונים. בכתבה זה נסקור עם הרעיון מאחורי האפליקציה, כיצד זו עובדת ומה היתרים מ השימוש בזו.
מהי טלגראס?
הפלטפורמה הווה אמצעי לרכישת צמח הקנאביס דרך האפליקציה טלגראם. זו מבוססת על ערוצים וקהילות טלגראם מיוחדות הקרויות ״כיווני טלגראס״, שם ניתן להרכיב מרחב מוצרי מריחואנה ולקבל אותם ישירות למשלוח. ערוצי התקשורת אלו מסודרים על פי אזורים גיאוגרפיים, במטרה להקל על קבלתם של המשלוחים.
כיצד זאת עובד?
התהליך קל למדי. ראשית, יש להצטרף לערוץ הטלגראס הרלוונטי לאזור המגורים. שם אפשר לעיין בתפריטי המוצרים המגוונים ולהרכיב עם הפריטים הרצויים. לאחר השלמת ההרכבה וסיום התשלום, השליח יופיע בכתובת שנרשמה ועמו החבילה שהוזמן.
רוב ערוצי טלגראס מציעים טווח נרחב של פריטים – זנים של צמח הקנאביס, עוגיות, משקאות ועוד. בנוסף, אפשר למצוא חוות דעת של צרכנים קודמים לגבי רמת הפריטים והשרות.
מעלות השימוש בטלגראס
מעלה מרכזי של האפליקציה הינו הנוחיות והדיסקרטיות. ההזמנה והתהליך מתבצעות ממרחק מאיזשהו מקום, בלי נחיצות במפגש פנים אל פנים. כמו כן, האפליקציה מוגנת היטב ומבטיחה חיסיון גבוהה.
נוסף על זאת, עלויות הפריטים בפלטפורמה נוטות להיות תחרותיים, והמשלוחים מגיעים במהירות ובמסירות רבה. יש גם מרכז תמיכה פתוח לכל שאלה או בעיה.
לסיכום
טלגראס היא דרך חדשנית ויעילה לרכוש מוצרי מריחואנה במדינה. היא משלבת את הנוחות הדיגיטלית של היישומון הפופולרי, ועם המהירות והדיסקרטיות של שיטת המשלוח הישירות. ככל שהביקוש לצמח הקנאביס גובר, פלטפורמות כמו זו צפויות להמשיך ולצמוח.
azithromycin 250
Как обезопасить свои личные данные: избегайте утечек информации в интернете. Сегодня обеспечение безопасности своих данных становится всё более важной задачей. Одним из наиболее обычных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в каком объеме предохранить себя от их утечки? Что такое «сит фразы»? «Сит фразы» — это сочетания слов или фраз, которые постоянно используются для доступа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или иные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как охранить свои личные данные? Используйте запутанные пароли. Избегайте использования простых паролей, которые легко угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не используйте один и тот же пароль для разных сервисов. Используйте двухфакторную аутентификацию (2FA). Это добавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт через другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы уберечь свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким как кража личной информации и финансовых потерь. Чтобы охранить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
trouver un m̩dicament en pharmacie: pharmacie en ligne france livraison belgique Рpharmacie en ligne fiable
farmacia online piГ№ conveniente farmacia online piГ№ conveniente farmacia online senza ricetta
Как охранять свои данные: остерегайтесь утечек информации в интернете. Сегодня защита личных данных становится всё значимее важной задачей. Одним из наиболее распространенных способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в каком объеме сберечься от их утечки? Что такое «сит фразы»? «Сит фразы» — это сочетания слов или фраз, которые бывают используются для входа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или иные конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, при помощи этих сит фраз. Как сохранить свои личные данные? Используйте сложные пароли. Избегайте использования простых паролей, которые легко угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого аккаунта. Не воспользуйтесь один и тот же пароль для разных сервисов. Используйте двухступенчатую аутентификацию (2FA). Это прибавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт через другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте личную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы уберечь свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может привести к серьезным последствиям, таким как кража личной информации и финансовых потерь. Чтобы обезопасить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
can i buy furosemide online
how much is ciprofloxacin
acne treatment admire – acne treatment ancient acne treatment study
Сохраните свои USDT: Проверяйте транзакцию TRC20 перед отправкой
Цифровые валюты, такие как USDT (Tether) на распределенном реестре TRON (TRC20), становятся все более распространенными в сфере децентрализованных финансов. Тем не менее совместно с ростом распространенности повышается также опасность промахов или жульничества во время отправке средств. Именно именно поэтому нужно контролировать перевод USDT TRC20 до ее отправлением.
Погрешность при вводе данных адреса получателя получателя иль пересылка на ошибочный адрес может повлечь к безвозвратной потере твоих USDT. Мошенники тоже могут стараться одурачить тебя, посылая поддельные адреса получателей на транзакции. Потеря криптовалюты по причине таких промахов сможет повлечь серьезными денежными убытками.
К радости, существуют профильные сервисы, дающие возможность проконтролировать операцию USDT TRC20 до ее пересылкой. Один из числа подобных служб дает возможность просматривать а также анализировать операции в распределенном реестре TRON.
На этом обслуживании вы сможете вводить адрес получателя а также получить детальную данные об нем, включая архив переводов, баланс а также статус счета. Данное поможет определить, есть ли адрес действительным а также надежным на отправки денег.
Другие сервисы также дают сходные возможности по проверки операций USDT TRC20. Некоторые кошельки по цифровых валют имеют интегрированные функции по контроля адресов и операций.
Не пропускайте контролем операции USDT TRC20 перед ее отсылкой. Небольшая предосторожность сможет сэкономить для вас множество средств а также избежать утрату ваших ценных криптовалютных активов. Задействуйте проверенные сервисы с целью обеспечения безопасности ваших операций а также неприкосновенности твоих USDT в распределенном реестре TRON.
В процессе обращении с криптовалютой USDT на блокчейне TRON (TRC20) чрезвычайно существенно не только верифицировать адрес получателя до транзакцией денег, но тоже систематически отслеживать остаток своего крипто-кошелька, а также происхождение поступающих транзакций. Данное действие позволит своевременно выявить всевозможные незапланированные операции и не допустить потенциальные потери.
Сначала, нужно проверить на точности демонстрируемого баланса USDT TRC20 в собственном кошельке для криптовалют. Предлагается сверять данные с данными публичных блокчейн-обозревателей, для того чтобы избежать вероятность хакерской атаки или компрометации самого крипто-кошелька.
Однако лишь отслеживания остатка мало. Чрезвычайно важно анализировать историю входящих переводов а также этих источники. В случае если Вы найдете поступления USDT от неизвестных или сомнительных реквизитов, сразу же приостановите данные средства. Имеется риск, чтобы данные монеты стали добыты незаконным способом и впоследствии изъяты регуляторами.
Наш сервис дает средства для всестороннего изучения поступающих USDT TRC20 переводов относительно их легальности а также отсутствия связи с противозаконной деятельностью. Мы.
Плюс к этому необходимо регулярно переводить USDT TRC20 на проверенные неконтролируемые криптовалютные кошельки под вашим абсолютным контролем. Хранение монет на внешних площадках всегда связано с рисками хакерских атак и потери финансов вследствие программных сбоев или несостоятельности платформы.
Соблюдайте основные правила защиты, оставайтесь внимательны а также вовремя мониторьте остаток а также происхождение поступлений USDT TRC20 кошелька. Это позволят обезопасить Ваши цифровые активы от незаконного завладения и потенциальных юридических проблем в будущем.
advair diskus cost in canada
dexamethasone medication
зеленое такси вызвать https://vyzvat-taksi.ru .
25 retin a
Dictum – factum
gГјnstigste online apotheke: gГјnstigste online apotheke – online apotheke preisvergleich
заказать такси номер такси заказ эконом по телефону .
Dictum – factum
vermox 500
дешевое такси в новочеркасске эконом такси в новочеркасске .
טלגראס כיוונים
טלגראס הווה תוכנה רווחת במדינה לקנייה של קנאביס באופן מקוון. זו מעניקה ממשק פשוט לשימוש ובטוח לרכישה וקבלת שילוחים מ פריטי מריחואנה שונים. בכתבה זו נסקור את העיקרון מאחורי הפלטפורמה, איך היא עובדת ומהם המעלות של השימוש בזו.
מה זו הפלטפורמה?
הפלטפורמה הווה אמצעי לקנייה של צמח הקנאביס באמצעות היישומון טלגרם. היא מבוססת מעל ערוצי תקשורת וקהילות טלגרם ספציפיות הנקראות ״כיווני טלגראס״, שבהם ניתן להרכיב מגוון מוצרי קנאביס ולקבל אלו ישירותית לשילוח. ערוצי התקשורת האלה מאורגנים לפי איזורים גאוגרפיים, במטרה להקל על קבלתם של השילוחים.
איך זאת פועל?
התהליך קל יחסית. ראשית, יש להצטרף לערוץ הטלגראס הרלוונטי לאזור המגורים. שם ניתן לעיין בתפריטי הפריטים השונים ולהזמין עם המוצרים הרצויים. לאחר השלמת ההזמנה וסיום התשלום, השליח יגיע לכתובת שנרשמה עם הארגז שהוזמן.
מרבית ערוצי טלגראס מספקים מגוון רחב של מוצרים – סוגי קנאביס, ממתקים, משקאות ועוד. כמו כן, ניתן לראות חוות דעת של צרכנים קודמים לגבי איכות הפריטים והשירות.
מעלות השימוש בפלטפורמה
יתרון מרכזי של האפליקציה הינו הנוחיות והפרטיות. ההרכבה והתהליך מתקיימים מרחוק מאיזשהו מיקום, ללא צורך במפגש פיזי. בנוסף, האפליקציה מאובטחת ביסודיות ומבטיחה חיסיון גבוה.
נוסף על זאת, מחירי המוצרים בפלטפורמה נוטות להיות תחרותיים, והמשלוחים מגיעים במהירות ובמסירות גבוהה. יש אף מוקד תמיכה פתוח לכל שאלה או בעיית.
לסיכום
האפליקציה מהווה שיטה חדשנית ויעילה לקנות פריטי קנאביס בארץ. היא משלבת את הנוחות הטכנולוגית מ היישומון הפופולרית, ועם המהירות והפרטיות של שיטת המשלוח הישירה. ככל שהביקוש לצמח הקנאביס גובר, פלטפורמות כמו טלגראס צפויות להמשיך ולהתפתח.
lioresal cost
diflucan 1 pill
Dictum – factum
tadacip 20mg
farmacia online barata: farmacia online españa envÃo internacional – farmacia online barcelona
vente de mГ©dicament en ligne pharmacie en ligne fiable pharmacie en ligne france fiable
отмывание usdt
Как охранять свои данные: избегайте утечек информации в интернете. Сегодня обеспечение безопасности личных данных становится всё значимее важной задачей. Одним из наиболее часто встречающихся способов утечки личной информации является слив «сит фраз» в интернете. Что такое сит фразы и в какой мере защититься от их утечки? Что такое «сит фразы»? «Сит фразы» — это сочетания слов или фраз, которые часто используются для входа к различным онлайн-аккаунтам. Эти фразы могут включать в себя имя пользователя, пароль или другие конфиденциальные данные. Киберпреступники могут пытаться получить доступ к вашим аккаунтам, используя этих сит фраз. Как обезопасить свои личные данные? Используйте запутанные пароли. Избегайте использования легких паролей, которые мгновенно угадать. Лучше всего использовать комбинацию букв, цифр и символов. Используйте уникальные пароли для каждого из аккаунта. Не применяйте один и тот же пароль для разных сервисов. Используйте двухступенчатую аутентификацию (2FA). Это добавляет дополнительный уровень безопасности, требуя подтверждение входа на ваш аккаунт по другое устройство или метод. Будьте осторожны с онлайн-сервисами. Не доверяйте персональную информацию ненадежным сайтам и сервисам. Обновляйте программное обеспечение. Установите обновления для вашего операционной системы и программ, чтобы предохранить свои данные от вредоносного ПО. Вывод Слив сит фраз в интернете может повлечь за собой серьезным последствиям, таким подобно кража личной информации и финансовых потерь. Чтобы обезопасить себя, следует принимать меры предосторожности и использовать надежные методы для хранения и управления своими личными данными в сети
В сфере крипто имеется действительная опасность получения так называемых “грязных” средств – криптомонет, соотносимых с нелегальной деятельностью, такого рода вроде отбеливание финансов, мошенничество иль кибератаки. Обладатели крипто-кошельков USDT в распределенном реестре TRON (TRC20) также склонны этому риску. По этой причине очень важно периодически удостоверяться свой кошелек для криптовалют на присутствие “незаконных” операций с целью оберегания собственных активов и репутации.
Опасность “незаконных” переводов заключается в этом, чтобы оные смогут являться отслежены силовыми органами и валютными надзорными органами. В случае если будет выявлена связь со противозаконной деятельностью, ваш кошелек для криптовалют имеет возможность быть блокирован, и активы – отчуждены. Сверх того, это может повлечь к правовые последствия а также повредить твою образ.
Существуют профильные службы, дающие возможность проконтролировать архив операций в твоём криптокошельке USDT TRC20 на существование подозрительных операций. Эти сервисы изучают данные транзакций, соотнося оные с задокументированными случаями жульничества, хакерских атак, а также легализации финансов.
Одним из числа таких сервисов является https://telegra.ph/Servisy-AML-proverka-USDT-05-19 позволяющий просматривать полную историю операций твоего USDT TRC20 криптокошелька. Служба выявляет возможно опасные транзакции а также дает подробные отчеты о оных.
Не оставляйте без внимания проверкой собственного кошелька для криптовалют USDT TRC20 на присутствие “нелегальных” переводов. Периодическое мониторинг посодействует избежать опасностей, связанных с незаконной активностью в крипто области. Применяйте надежные сервисы с целью проверки собственных USDT операций, чтобы обезопасить ваши цифровые активы и репутацию.
Защитите свои USDT: Проконтролируйте транзакцию TRC20 до пересылкой
Виртуальные деньги, такие как USDT (Tether) на блокчейне TRON (TRC20), делаются всё более распространенными в области сфере децентрализованных финансовых услуг. Тем не менее совместно с ростом востребованности растет и риск промахов либо мошенничества во время транзакции средств. Именно по этой причине необходимо контролировать перевод USDT TRC20 до ее отправкой.
Погрешность во время вводе адреса получателя либо отправка на неправильный адрес сможет повлечь к необратимой потере твоих USDT. Злоумышленники также смогут стараться обмануть тебя, пересылая поддельные адреса получателей на транзакции. Утрата криптовалюты вследствие подобных промахов сможет повлечь значительными денежными потерями.
Впрочем, существуют специализированные сервисы, позволяющие проконтролировать операцию USDT TRC20 перед ее отсылкой. Некий из подобных служб дает возможность просматривать а также анализировать переводы в блокчейне TRON.
На данном сервисе вам сможете вводить адрес адресата а также получить обстоятельную сведения об нем, включая историю переводов, остаток а также статус счета. Данное посодействует выяснить, является или нет адрес получателя действительным а также безопасным для перевода денег.
Иные сервисы также дают аналогичные возможности для удостоверения операций USDT TRC20. Определенные кошельки для цифровых валют обладают встроенные функции по контроля адресов получателей а также транзакций.
Не игнорируйте удостоверением перевода USDT TRC20 до ее отправкой. Малая предосторожность может сберечь для вас множество финансов и не допустить утрату твоих важных крипто ресурсов. Задействуйте проверенные сервисы с целью гарантии надежности ваших операций а также неприкосновенности твоих USDT на блокчейне TRON.
В процессе работе с криптовалютой USDT в блокчейне TRON (TRC20) максимально значимо не просто удостоверять реквизиты получателя перед транзакцией средств, но тоже систематически отслеживать остаток своего кошелька, а также происхождение входящих транзакций. Данное действие позволит своевременно обнаружить всевозможные нежелательные действия а также избежать возможные убытки.
Сначала, требуется проверить на правильности отображаемого остатка USDT TRC20 на вашем кошельке для криптовалют. Советуется сравнивать данные с сведениями публичных обозревателей блокчейна, чтобы не допустить вероятность взлома или компрометации самого кошелька.
Тем не менее исключительно наблюдения остатка недостаточно. Чрезвычайно существенно изучать журнал поступающих транзакций а также этих источники. Если вы найдете переводы USDT от неизвестных либо вызывающих опасения реквизитов, немедленно заблокируйте данные средства. Есть риск, чтобы эти криптомонеты были получены преступным путем и в будущем могут быть конфискованы регулирующими органами.
Наш сервис дает инструменты с целью детального анализа поступающих USDT TRC20 транзакций касательно их законности и отсутствия связи с криминальной деятельностью. Мы поможем вам безопасно работать с этим популярным стейблкоином.
Плюс к этому нужно регулярно отправлять USDT TRC20 на надежные неконтролируемые криптовалютные кошельки находящиеся под собственным тотальным управлением. Содержание монет на сторонних площадках всегда связано с рисками хакерских атак и утраты финансов вследствие технических ошибок или несостоятельности платформы.
Соблюдайте базовые меры безопасности, оставайтесь бдительны а также оперативно отслеживайте баланс и источники пополнений кошелька для USDT TRC20. Это позволит обезопасить ваши электронные ценности от.
Achat mГ©dicament en ligne fiable: pharmacie en ligne france fiable – pharmacie en ligne pas cher
Добрый день всем!
Приобретите российский диплом с гарантией качества и доставкой в любую точку страны без предварительной оплаты!
http://dlplomanrussia.com
where to get tamoxifen
vardenafil dosing
accutane pills online
Информационный портал https://kalitka48.ru/ на актуальные темы, связанные с недвижимостью: новости рынка недвижимости, информация о покупке и продаже квартир и множество других полезных статей.
effexor xr cost
uti medication beauty – uti medication range uti medication moral
mikaspa.com
끝까지 비판 … Lin Jingyan은 격렬하게 떨었습니다.
farmacia en casa online descuento: farmacias online baratas – farmacia online madrid
Divide et impera
internet apotheke online apotheke deutschland internet apotheke
where can i purchase synthroid
Cogito ergo sum
amoxicillin 500 mg price
diflucan 200 mg daily
how much is azithromycin 250 mg
where to get accutane in singapore
Проверить перевод usdt trc20
Важность проверки транзакции USDT в сети TRC20
Операции USDT в рамках протокола TRC20 набирают все большую востребованность, вместе с тем необходимо быть чрезвычайно осторожными в ходе таких обработке.
Этот категория платежей часто используется в процессе обеления финансов, приобретенных незаконным образом.
Один из угроз получения USDT TRC-20 – заключается в том, что они могут быть зачислены в результате многочисленных схем кражи, например кражи приватных данных, шантаж, компрометации наряду с дополнительные противоправные операции. Обрабатывая такие операции, пользователь неизбежно выступаете подельником нелегальной активности.
Поэтому чрезвычайно необходимо скрупулезно анализировать происхождение различных зачисляемого транзакции по USDT по сети TRC20. Необходимо интересоваться у плательщика сведения в отношении законности денежных средств, при малейших сомнениях – воздерживаться такие платежей.
Учитывайте, что в установления противоправных генезисов денежных средств, клиент с высокой вероятностью будете подвергнуты к санкциям наряду рядом с перевододателем. Вследствие этого рекомендуется перестраховаться как и глубоко проверять всякий транзакцию, нежели подвергать риску личной репутацией наряду с столкнуться с серьезные законодательные неприятности.
Обеспечение аккуратности в процессе сделках с использованием USDT TRC-20 – является гарантия личной финансовой безопасности как и предотвращение вовлечения в криминальные схемы. Будьте осторожны и неизменно проверяйте происхождение виртуальных валютных финансов.
Per aspera ad astra
generic lyrica for sale
furosemide tablets buy uk
п»їshop apotheke gutschein: online apotheke rezept – online apotheke deutschland
Low-carb gummies have surfaced as a widely-liked food choice for people following a low-carb or low-carbohydrate diet. These gummy treats are designed to be reduced in digestible carbs, making them a harmless pleasure for those aiming to sustain a https://t.me/s/ketogummies state of ketonemia.
By employing natural sugar substitutes like stevia extract or erythritol, ketogenic gummies give a satisfying sweet taste without raising glycemic readings, a common concern with traditional confectionery.
1go casino https://prime-kapitals.com/
where can i get amoxicillin uk
lyrica discount
100 лет тому вперед фильм смотреть. Смотреть бесплатно фильм 100 лет тому вперед.
вход 1go casino официальный сайт 1го казино
order provigil online canada
вход 1go casino https://prime-kapitals.com/
100 лет тому вперед фильм смотреть онлайн бесплатно. 100 лет тому вперед фильм смотреть онлайн бесплатно.
pharmacie en ligne livraison europe: pharmacie en ligne fiable – trouver un mГ©dicament en pharmacie
online apotheke günstig: europa apotheke – online apotheke
azithromycin 1g for sale
lyrica 75 mg
online apotheke rezept online apotheke online apotheke preisvergleich
vermox 500mg tablet price
1go casino официальный сайт https://prime-kapitals.com/
Проверить перевод usdt trc20
Важность проверки транзакции USDT TRC20
Платежи USDT в протокола TRC20 приобретают повышенную активность, но необходимо сохранять чрезвычайно осторожными в ходе этих принятии.
Указанный вид платежей преимущественно применяется в процессе легализации активов, добытых противоправным способом.
Основной факторов риска принятия USDT TRC20 – подразумевает, что такие платежи имеют потенциал быть зачислены вследствие различных методов вымогательства, включая утраты личных данных, принуждение, кибератаки наряду с прочие незаконные действия. Зачисляя такие операции, пользователь неизбежно выглядите сообщником преступной активности.
Вследствие этого чрезвычайно важно скрупулезно проверять природу всех зачисляемого платежа по USDT в сети TRC20. Следует получать с инициатора информацию касательно правомерности денежных средств, а малейших вопросах – отказываться от переводов.
Имейте в виду, в том, что в процессе установления криминальных генезисов финансов, клиент с высокой вероятностью будете подвергнуты с применением взысканиям параллельно рядом с перевододателем. Таким образом лучше перестраховаться как и глубоко проверять любой платеж, чем подвергать риску собственной репутацией и попасть под масштабные юридические сложности.
Обеспечение осторожности в ходе сделках через USDT TRC20 – представляет собой залог вашей экономической безопасности как и избежание попадания в преступные практики. Будьте бдительными наряду с всегда исследуйте источник электронных валютных финансов.
diflucan pill cost
Фильм 100 лет тому вперед смотреть. Смотреть бесплатно фильм 100 лет тому вперед.
Смотреть фильм 100 лет тому вперед бесплатно в хорошем качестве. 100 лет тому вперед смотреть онлайн.
albuterol buy online australia
farmacia online espaГ±a envГo internacional: farmacia online madrid – farmacia online madrid
augmentin brand name price
order accutane online
prostatitis treatment nephew – prostatitis pills axe prostatitis pills sensible
dexamethasone 200 mg
prostatitis pills indeed – pills for treat prostatitis inner prostatitis pills net
100 лет тому вперед фильм смотреть онлайн бесплатно в хорошем. Смотреть онлайн 100 лет тому вперед.
diflucan 125mg
buy nolvadex usa
trouver un m̩dicament en pharmacie: pharmacie en ligne france pas cher Рtrouver un m̩dicament en pharmacie
dexamethasone 0.5 mg tablet price
farmacie online sicure farmaci senza ricetta elenco top farmacia online
accutane prescription canada
buy accutane in india
accutane sale uk
Продажа квартир Пенза https://solnechnyjgorod.ru/, успейте купить квартиру от застройщика в Пензе. ЖК «Солнечный Город» расположен в экологическом чистом районе в 13 км от города Пенза. Продажа 1,2 комнатных квартир от застройщика по минимальной стоимости за кВ/м, успей купить не упусти шанс.
albuterol 0.83 mg
pharmacie en ligne france fiable: pharmacie en ligne avec ordonnance – vente de mГ©dicament en ligne
farmacia online envÃo gratis: farmacia online 24 horas – farmacia barata
Уэнздей 1 сезон кино
azithromycin over the counter uk
проверить адрес usdt trc20
Тема: Непременно контролируйте адрес получателя во время транзакции USDT TRC20
При работе со крипто, особенно со USDT на распределенном реестре TRON (TRC20), весьма нужно проявлять осторожность а также тщательность. Единственная из самых частых ошибок, какую делают юзеры – отправка финансов на ошибочный адресу. Для того чтобы избежать утрату своих USDT, требуется неизменно внимательно контролировать адресе реципиента перед отправкой транзакции.
Криптовалютные адреса кошельков представляют собой обширные совокупности литер а также цифр, к примеру, TRX9QahiFUYfHffieZThuzHbkndWvvfzThB8U. Даже незначительная ошибка либо оплошность при копировании адреса сможет привести к тому результату, чтобы ваши цифровые деньги станут безвозвратно утрачены, ибо оные окажутся на неконтролируемый вам криптокошелек.
Существуют многообразные пути удостоверения адресов кошельков USDT TRC20:
1. Визуальная проверка. Старательно соотнесите адрес в своём крипто-кошельке со адресом адресата. В случае малейшем расхождении – воздержитесь от перевод.
2. Использование онлайн-сервисов удостоверения.
3. Двойная проверка с адресатом. Попросите адресату подтвердить точность адреса перед посылкой операции.
4. Тестовый транзакция. При значительной сумме операции, можно сначала послать малое количество USDT для контроля адреса.
Также советуется содержать крипто на личных кошельках, но не на биржах либо третьих сервисах, для того чтобы обладать полный управление над собственными ресурсами.
Не оставляйте без внимания контролем адресов при осуществлении взаимодействии со USDT TRC20. Эта несложная мера безопасности окажет помощь обезопасить твои финансы против непреднамеренной лишения. Имейте в виду, что на области крипто операции невозвратны, а посланные монеты по неправильный адрес кошелька возвратить практически нельзя. Будьте внимательны а также тщательны, чтобы защитить собственные вложения.
effexor xl
farmacias online seguras farmacia online barcelona farmacia online madrid
Король и шут 1 сезон смотреть онлайн
Как похудеть
Жизнь не заканчивается после травли от коллег или полным разочарованием от жизни. В календаре с каждым днем появлялось всё больше закрашенных дней. А поездка к морю становилась все ближе, ведь килограммы улетучивались как только могли! человек совсем не предвидел из уст собственной жены Татианы. В данной династии телосложение организма совсем не соответствовала в противовес типовой также общепринятой – обладать предожирением полная правило.
how to get zithromax
treatment for uti queer – treatment for uti dad treatment for uti welcome
Фоллаут 1 сезон смотреть онлайн
propecia in canada
Telegrass
האפליקציה הווה פלטפורמה מקובלת בישראל לרכישת צמח הקנאביס בצורה אינטרנטי. זו מעניקה ממשק פשוט לשימוש ומאובטח לקנייה ולקבלת משלוחים של מוצרי מריחואנה מרובים. בסקירה זה נבחן את העיקרון שמאחורי הפלטפורמה, כיצד זו פועלת ומה המעלות מ השימוש בזו.
מה זו האפליקציה?
טלגראס מהווה אמצעי לרכישת מריחואנה באמצעות האפליקציה טלגראם. זו מבוססת על ערוצים וקהילות טלגרם ייעודיות הקרויות ״כיווני טלגראס״, שם ניתן להזמין מגוון פריטי צמח הקנאביס ולקבל אותם ישירות למשלוח. ערוצי התקשורת אלו מסודרים לפי אזורים גיאוגרפיים, במטרה להקל על קבלתם של השילוחים.
איך זאת פועל?
התהליך קל יחסית. ראשית, יש להצטרף לערוץ טלגראס הרלוונטי לאזור המגורים. שם ניתן לעיין בתפריטים של הפריטים המגוונים ולהרכיב עם המוצרים הרצויים. לאחר ביצוע ההזמנה וסיום התשלום, השליח יופיע בכתובת שנרשמה ועמו הארגז המוזמנת.
מרבית ערוצי הטלגראס מציעים טווח רחב של מוצרים – זנים של צמח הקנאביס, עוגיות, שתייה ועוד. כמו כן, ניתן למצוא ביקורות של לקוחות קודמים על איכות הפריטים והשירות.
מעלות הנעשה באפליקציה
יתרון עיקרי מ האפליקציה הוא הנוחיות והדיסקרטיות. ההזמנה וההכנות מתקיימים מרחוק מכל מקום, ללא נחיצות במפגש פיזי. כמו כן, האפליקציה מוגנת היטב ומבטיחה חיסיון גבוהה.
נוסף אל זאת, עלויות המוצרים בפלטפורמה נוטות לבוא תחרותיים, והשילוחים מגיעים במהירות ובמסירות גבוהה. קיים גם מרכז תמיכה פתוח לכל שאלה או בעיית.
לסיכום
האפליקציה מהווה שיטה חדשנית ויעילה לרכוש פריטי קנאביס בישראל. היא משלבת בין הנוחיות הדיגיטלית מ היישומון הפופולרי, לבין המהירות והפרטיות מ שיטת השילוח הישירות. ככל שהדרישה למריחואנה גובר, אפליקציות כמו טלגראס צפויות להמשיך ולהתפתח.
pharmacie en ligne sans ordonnance: pharmacie en ligne france livraison belgique – pharmacie en ligne france livraison belgique
заказ такси в новочеркасске по телефону недорого такси город
Геракл24: Опытная Реставрация Фундамента, Венцов, Настилов и Передвижение Зданий
Организация Gerakl24 специализируется на оказании комплексных сервисов по смене основания, венцов, покрытий и переносу зданий в городе Красноярске и в окрестностях. Наша группа опытных мастеров обещает превосходное качество исполнения всех типов ремонтных работ, будь то из дерева, каркасные, из кирпича или бетонные здания.
Плюсы работы с Gerakl24
Навыки и знания:
Каждая задача осуществляются исключительно опытными мастерами, с многолетним большой стаж в сфере строительства и восстановления строений. Наши специалисты профессионалы в своем деле и выполняют задачи с безупречной точностью и вниманием к мелочам.
Всесторонний подход:
Мы осуществляем все виды работ по восстановлению и ремонту домов:
Замена фундамента: усиление и реставрация старого основания, что позволяет продлить срок службы вашего здания и избежать проблем, вызванные оседанием и деформацией.
Смена венцов: восстановление нижних венцов деревянных зданий, которые наиболее часто подвержены гниению и разрушению.
Смена настилов: замена старых полов, что кардинально улучшает внешний вид и функциональные характеристики.
Перенос строений: безопасное и качественное передвижение домов на другие участки, что помогает сохранить здание и предотвращает лишние расходы на создание нового.
Работа с любыми типами домов:
Деревянные дома: восстановление и защита деревянных строений, защита от разрушения и вредителей.
Каркасные строения: реставрация каркасов и реставрация поврежденных элементов.
Кирпичные дома: реставрация кирпичной кладки и усиление стен.
Бетонные строения: восстановление и укрепление бетонных структур, ремонт трещин и дефектов.
Качество и прочность:
Мы работаем с только высококачественные материалы и новейшее оборудование, что гарантирует долговечность и надежность всех работ. Каждый наш проект проходят тщательную проверку качества на каждой стадии реализации.
Индивидуальный подход:
Каждому клиенту мы предлагаем индивидуальные решения, с учетом всех особенностей и пожеланий. Наша цель – чтобы результат нашей работы полностью удовлетворял вашим ожиданиям и требованиям.
Почему выбирают Геракл24?
Обратившись к нам, вы получаете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы обеспечиваем выполнение всех работ в сроки, установленные договором и с соблюдением всех строительных норм и стандартов. Обратившись в Геракл24, вы можете быть уверены, что ваш дом в надежных руках.
Мы предлагаем консультацию и дать ответы на все вопросы. Звоните нам, чтобы обсудить ваш проект и узнать больше о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
animehangover.com
즉시 캐주얼 범선이 철갑선을 재 보급하기 시작했습니다.
amateur naked sex amateur naked sex
pharmacie en ligne sans ordonnance: vente de m̩dicament en ligne Рpharmacie en ligne sans ordonnance
dexamethasone prescription
dexamethasone 4 mg tablet price
azithromycin 500 mg tablet buy online
generic valtrex online pharmacy
farmacia online barata y fiable farmacias online baratas farmacias online seguras
аренда такси в новочеркасске эконом такси недорого новочеркасск
diflucan 150
Привет игроманы!
Я давно увлекаюсь онлайн казино и, как многие из вас, всегда искал платформу, которая бы соответствовала всем моим требованиям. Искал и . Перепробовал множество сайтов, но постоянно сталкивался с различными проблемами: неудобный интерфейс, задержки с выплатами, отсутствие нормальной поддержки, да и просто скучный набор игр. В какой-то момент я почти потерял надежду, но решил попробовать еще один раз и наконец-то нашел Telegram . Вот несколько причин, почему я считаю его идеальным:
– Удобный интерфейс: сайт очень удобный и понятный, даже для новичков. Все нужные разделы под рукой, ничего лишнего.
– Мгновенные выплаты: проверил на себе – выигрыш приходит на счет практически моментально.
– Отличная поддержка: техподдержка реально работает и помогает решить любые проблемы. Причем они доступны 24/7.
– Широкий выбор игр: тут есть все – от классических слотов до живых дилеров. И постоянно добавляют что-то новое.
– Бонусы и акции: щедрые приветственные бонусы и регулярные акции. Всегда приятно получать дополнительные фриспины или бонусы за пополнение счета.
Понимаю, что каждому свое, но лично для меня стало настоящей находкой. Если вы тоже устали искать, рекомендую попробовать. Возможно, оно станет вашим новым любимым местом для игры.
Если у кого-то уже есть опыт игры на этом сайте, делитесь своими впечатлениями! Интересно узнать ваше мнение.
Удачи и больших выигрышей всем!
azithromycin 1000
הפלטפורמה הווה פלטפורמה מקובלת במדינה לרכישת קנאביס באופן אינטרנטי. זו נותנת ממשק נוח ומאובטח לקנייה וקבלת משלוחים של מוצרי קנאביס שונים. בכתבה זה נבחן את העיקרון מאחורי הפלטפורמה, כיצד זו פועלת ומה היתרונות של השימוש בה.
מה זו טלגראס?
טלגראס הווה דרך לרכישת צמח הקנאביס באמצעות היישומון טלגרם. זו מבוססת מעל ערוצי תקשורת וקהילות טלגרם ייעודיות הקרויות ״כיווני טלגראס״, שבהם ניתן להזמין מרחב מוצרי קנאביס ולקבל אלו ישירותית למשלוח. הערוצים האלה מאורגנים על פי איזורים גאוגרפיים, במטרה להקל את קבלת המשלוחים.
איך זה עובד?
התהליך קל למדי. קודם כל, צריך להצטרף לערוץ הטלגראס הרלוונטי לאזור המגורים. שם ניתן לעיין בתפריטי המוצרים המגוונים ולהרכיב עם הפריטים המבוקשים. לאחר השלמת ההזמנה וסיום התשלום, השליח יופיע לכתובת שצוינה ועמו החבילה המוזמנת.
רוב ערוצי טלגראס מציעים מגוון נרחב של מוצרים – זנים של קנאביס, עוגיות, משקאות ועוד. כמו כן, ניתן לראות ביקורות של לקוחות שעברו לגבי רמת המוצרים והשירות.
יתרונות השימוש בטלגראס
מעלה מרכזי מ הפלטפורמה הינו הנוחות והדיסקרטיות. ההזמנה והתהליך מתבצעות ממרחק מאיזשהו מיקום, בלי נחיצות בהתכנסות פיזי. בנוסף, האפליקציה מאובטחת היטב ומבטיחה סודיות גבוהה.
מלבד על זאת, עלויות הפריטים בטלגראס נוטות להיות זולים, והשילוחים מגיעים במהירות ובהשקעה גבוהה. קיים גם מוקד תמיכה זמין לכל שאלה או בעיה.
סיכום
הפלטפורמה הווה דרך חדשנית ויעילה לרכוש פריטי קנאביס בארץ. היא משלבת בין הנוחיות הדיגיטלית של היישומון הפופולרי, ועם המהירות והפרטיות של דרך המשלוח הישירות. ככל שהביקוש למריחואנה גדלה, פלטפורמות בדוגמת טלגראס צפויות להמשיך ולצמוח.
azithromycin 250
pharmacie en ligne avec ordonnance: pharmacies en ligne certifiГ©es – vente de mГ©dicament en ligne
clomid where to buy
prosteride
How to lose weight
?In a couple of moments, the family was already in the vegetable department. They had to be there as rarely as possible — some vegetables and fruits were completely unknown to these people. Looking at everything as a curiosity, the time of choice came:
— Well, then… Let’s take tomatoes, cucumbers, and here are apples, zucchini can also be taken…
Tanya reasoned to herself and did not consult with her hungry husband, skillfully sorting through the vegetables and putting the best ones in a plastic bag. The little girl carefully examined the oranges — she had never seen such a thing before, let alone eaten it:
— Maybe we’ll take something else normal later? Sausages, hot dogs. If you want to, go ahead and diet. But we’ll live normally. Right, daughter?
buy lyrica 300 mg online uk
generic provigil prices
https://vyzvat-taksi.ru
http://levitraenligne.com/# pharmacie en ligne france
tretinoin purchase online
zithromax 500 price
valacyclovir pills stone – valacyclovir online bloom valacyclovir online scowl
furosemide 500 mg tablet
Как похудеть
Взгляд ее наполнился печалью, голова сама опустилась из-за тяжести мыслей, терзающих ее внутри. Она ничего не говорила, да и расспрос в магазине мужчину не особого интересовал в данный момент. Им понадобилось буквально полчаса, что бы собрать нужную продуктовую корзину, «правильную». Она очень отличалась от их привычной: там не было сладостей и газировки, копченостей и выпечки. Особенным ударом ниже пояса для мужчины стал отказ в покупке майонеза:
—Боже мой, что это. «Хлеб диетический», ух ты…. И ты хочешь сказать, что за эти два пакета зелени мы заплатили три тысячи?
—Так ты посмотри, сколько мы набрали? Это же не ролтон, ими наесться на весь день можно. И еще похудеть в том числе.
человек абсолютно не предусматривал из уст собственной супруги Татьяны. На территории этой семье телосложение физической оболочки совсем не соответствовала по сравнению с типовой также общепринятой – обладать предожирением абсолютная условие.
Gerakl24: Квалифицированная Смена Фундамента, Венцов, Настилов и Перенос Зданий
Фирма Gerakl24 профессионально занимается на оказании всесторонних работ по смене основания, венцов, покрытий и переносу зданий в месте Красноярск и за пределами города. Наша команда профессиональных мастеров обеспечивает высокое качество реализации различных типов реставрационных работ, будь то деревянные, каркасного типа, кирпичные или бетонные конструкции здания.
Преимущества работы с Gerakl24
Навыки и знания:
Каждая задача осуществляются только профессиональными экспертами, с многолетним долгий стаж в направлении строительства и восстановления строений. Наши сотрудники эксперты в своей области и реализуют проекты с высочайшей точностью и вниманием к деталям.
Комплексный подход:
Мы осуществляем разнообразные услуги по ремонту и восстановлению зданий:
Замена фундамента: укрепление и замена старого фундамента, что обеспечивает долгий срок службы вашего дома и устранить проблемы, связанные с оседанием и деформацией.
Реставрация венцов: реставрация нижних венцов из дерева, которые обычно гниют и разрушаются.
Смена настилов: монтаж новых настилов, что значительно улучшает визуальное восприятие и практическую полезность.
Перенос строений: безопасное и качественное передвижение домов на новые места, что позволяет сохранить ваше строение и избегает дополнительных затрат на возведение нового.
Работа с любыми видами зданий:
Деревянные дома: восстановление и укрепление деревянных конструкций, обработка от гниения и насекомых.
Каркасные дома: укрепление каркасов и замена поврежденных элементов.
Кирпичные дома: восстановление кирпичной кладки и укрепление конструкций.
Дома из бетона: ремонт и укрепление бетонных конструкций, ремонт трещин и дефектов.
Надежность и долговечность:
Мы работаем с только проверенные материалы и современное оборудование, что гарантирует долгий срок службы и прочность всех выполненных задач. Каждый наш проект подвергаются строгому контролю качества на всех этапах выполнения.
Индивидуальный подход:
Мы предлагаем каждому клиенту подходящие решения, учитывающие ваши требования и желания. Мы стремимся к тому, чтобы результат нашей работы полностью удовлетворял вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Сотрудничая с нами, вы приобретете надежного партнера, который возьмет на себя все заботы по восстановлению и ремонту вашего здания. Мы гарантируем выполнение всех работ в сроки, установленные договором и с соблюдением всех строительных норм и стандартов. Связавшись с Геракл24, вы можете не сомневаться, что ваше строение в надежных руках.
Мы предлагаем консультацию и дать ответы на все вопросы. Контактируйте с нами, чтобы обсудить детали вашего проекта и узнать больше о наших услугах. Мы сохраним и улучшим ваш дом, сделав его безопасным и комфортным для проживания на долгие годы.
Gerakl24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
trouver un mГ©dicament en pharmacie: Medicaments en ligne livres en 24h – Pharmacie en ligne livraison Europe
diflucan tablets uk
how to get accutane prescription
How to lose weight
?Life doesn’t end after bullying from colleagues or complete disappointment in life. More and more days were filled in the calendar every day. And the trip to the sea was getting closer, as the kilograms were evaporating as much as they could!
baclofen 10 price
augmentin 500 mg cost
Pharmacie en ligne livraison Europe: vente de mГ©dicament en ligne – Pharmacie Internationale en ligne
Viagra Pfizer sans ordonnance: Viagra generique en pharmacie – Viagra homme prix en pharmacie sans ordonnance
מבורכים הנכנסים לאתר הידע והמידע והעזרה הרשמי של טלגרמות כיוונים! כאן אפשר לאתר ולמצוא את מלוא המידע והפרטים העדכני והמעודכן ביותר לגבי מערכת טלגרף וכלים לשימוש נכון בה כנדרש.
מה מציין טלגרמות אופקים?
טלגרם נתיבים היא מנגנון הנסמכת על טלגרף המספקת להפצה ורכישה מסביב דשא וקנבי בישראל. באופן של המשלוחים והמסגרות בטלגרם, פעילים מורשים להשיג ולהשיג את מוצרי מריחואנה באופן קל ומהיר.
כיצד להיכנס בטלגרם?
על מנת להתחבר בשימוש נכון בפלטפורמת טלגרם, מומלץ לכם להצטרף לערוצים ולחוגים האיכותיים. כאן באתר זה ניתן למצוא רשימה של צירים לקבוצות מאומתים ומובטחים. במקביל לכך, אפשר להיכנס במסלול ההזמנה וההשגה סביב מוצרי הקנבי.
מידע וכללים
במקום הזה אפשר למצוא מבחר מבין הדרכות ומידע מפורטים אודות הפעלה בטלגראס, בין היתר:
– החיבור לערוצים מומלצים
– פעילות הקבלה
– אבטחה ואבטחה בשילוב בטלגרם
– ועוד פרטים אחר
צירים מאומתים
לגבי נושא זה קישורים למקומות ולחוגים רצויים בטלגרם:
– פורום הנתונים והעדכונים הרשמי
– קבוצת הסיוע והליווי לצרכנים
– פורום לאספקת פריטי קנבי מובטחים
– מבחר ספקים קנבי מובטחות
צוות מברכים אתם על החברות שלכם לאתר המידע מאת טלגרם נתיבים ומצפים לקהל חווית שירות מצוינת ומובטחת!
Уэнздей смотреть онлайн
purchase acyclovir online
claritin pills current – claritin punish loratadine medication food
dexamethasone 75 mg
Фоллаут 1 сезон фильм
claritin harmony – loratadine blade loratadine medication footstep
propecia usa
trouver un mГ©dicament en pharmacie: Medicaments en ligne livres en 24h – pharmacie en ligne avec ordonnance
pharmacie en ligne france livraison belgique: acheter kamagra site fiable – pharmacie en ligne france livraison internationale
Фоллаут фильм
mikaspa.com
이런 관점에서 보면…뉴스는…실제로 사실입니다.
מבורכים הנהנים לאזור המידע והידע והתמיכה המוכר והרשמי עבור טלגרף אופקים! במיקום זה רשאים לאתר ולמצוא את כלל הנתונים והמידע החדיש והעדכני ביותר זמין בעניין פלטפורמת טלגרמות ואופני לשימוש בה כנדרש.
מיהו טלגראס מסלולים?
טלגרם כיוונים מציינת מנגנון הנשענת על טלגרם המשמשת לתפוצה ורכישה של קנאביס וקנביס בישראל. באמצעות ההודעות והמסגרות בטלגרם, צרכנים רשאים להשיג ולקבל מוצרי דשא בשיטה פשוט ומיידי.
באיזה דרך להתחבר בטלגראס כיוונים?
לשם להיכנס בפעילות בטלגראס, אתם נדרשים להיות חברים ב לשיחות ולחוגים המומלצים. בנקודה זו בפורטל זה אפשר למצוא סיכום עבור מסלולים לשיחות פעילים ומהימנים. לאחר מכן, אפשר להיכנס במסלול האספקה והקבלה של מוצרי המריחואנה.
הסברים ומידע
באתר המסוים אפשר למצוא מבחר מבין הוראות וכללים ברורים לגבי הפעלה בטלגראס, בין היתר:
– החיבור לערוצים רצויים
– פעילות הקבלה
– הגנה והגנה בהתנהלות בטלגראס כיוונים
– ומגוון מידע נוסף בנוסף
לינקים רצויים
לגבי נושא זה צירים לערוצים ולחוגים רצויים בטלגרם:
– קבוצה הנתונים והעדכונים המאושר
– מקום הסיוע והליווי ללקוחות
– פורום להזמנת מוצרי קנבי מוטבחים
– רשימת חנויות קנבי מאומתות
אנו מכבדים את כולם על החברות שלכם לפורטל המידע והידע מטעם טלגרף כיוונים ומצפים לכולם חווית שהיא קנייה טובה ואמינה!
diflucan otc where to buy
5 mg accutane singapore
buy dexamethasone without prescription
azithromycin 500 mg india
where to get accutane in australia
Helpful content, Regards.|
Sildenafil teva 100 mg sans ordonnance: viagra sans ordonnance – Prix du Viagra 100mg en France
Thank you so much!
купить подписчиков вк
купить подписчиков вк
купить просмотры тик ток
накрутка реакций тг
https://phenligne.shop/# pharmacie en ligne
pharmacie en ligne avec ordonnance: Medicaments en ligne livres en 24h – Achat mГ©dicament en ligne fiable
modafinil cost canada
Майор Гром 2024
buy azithromycin from mexico
thebuzzerpodcast.com
“당신은… 당신의 병은 나았습니까?” Hongzhi 황제가 무의식적으로 말했다.
Gerakl24: Квалифицированная Смена Основания, Венцов, Полов и Перенос Зданий
Фирма Геракл24 специализируется на оказании полных услуг по реставрации основания, венцов, настилов и переносу домов в месте Красноярск и за пределами города. Наша команда квалифицированных мастеров обещает превосходное качество исполнения всех видов ремонтных работ, будь то деревянные, с каркасом, из кирпича или из бетона дома.
Достоинства услуг Gerakl24
Навыки и знания:
Каждая задача осуществляются исключительно опытными специалистами, с многолетним большой стаж в области создания и реставрации домов. Наши мастера знают свое дело и выполняют задачи с максимальной точностью и вниманием к деталям.
Комплексный подход:
Мы предлагаем полный спектр услуг по восстановлению и ремонту домов:
Замена фундамента: укрепление и замена старого фундамента, что позволяет продлить срок службы вашего здания и предотвратить проблемы, связанные с оседанием и деформацией.
Смена венцов: восстановление нижних венцов деревянных зданий, которые обычно подвержены гниению и разрушению.
Смена настилов: монтаж новых настилов, что кардинально улучшает визуальное восприятие и практическую полезность.
Перемещение зданий: безопасное и надежное перемещение зданий на другие участки, что обеспечивает сохранение строения и избежать дополнительных затрат на возведение нового.
Работа с любыми типами домов:
Древесные строения: реставрация и усиление деревянных элементов, обработка от гниения и насекомых.
Каркасные дома: усиление каркасных конструкций и реставрация поврежденных элементов.
Дома из кирпича: ремонт кирпичных стен и укрепление стен.
Дома из бетона: реставрация и усиление бетонных элементов, исправление трещин и разрушений.
Качество и прочность:
Мы используем только проверенные материалы и передовые технологии, что обеспечивает долгий срок службы и прочность всех выполненных задач. Все проекты проходят тщательную проверку качества на всех этапах выполнения.
Личный подход:
Мы предлагаем каждому клиенту подходящие решения, учитывающие все особенности и пожелания. Мы стараемся, чтобы результат нашей работы полностью удовлетворял вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Обратившись к нам, вы получаете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы обеспечиваем выполнение всех работ в сроки, установленные договором и с в соответствии с нормами и стандартами. Связавшись с Геракл24, вы можете быть уверены, что ваше строение в надежных руках.
Мы предлагаем консультацию и ответить на ваши вопросы. Свяжитесь с нами, чтобы обсудить детали и узнать больше о наших услугах. Мы поможем вам сохранить и улучшить ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш надежный партнер в реставрации и ремонте домов в Красноярске и за его пределами.
valtrex dignity – valacyclovir pills remark valacyclovir journal
Achat mГ©dicament en ligne fiable: Pharmacie en ligne livraison Europe – pharmacies en ligne certifiГ©es
lyrica online uk
albuterol 90 mcg inhaler
diflucan 50
albuterol over the counter
propecia 0.5 mg
can you buy azithromycin over the counter in usa
cost of generic zithromax
Gerakl24: Профессиональная Смена Основания, Венцов, Покрытий и Перемещение Домов
Организация Gerakl24 специализируется на оказании комплексных работ по реставрации фундамента, венцов, покрытий и переносу домов в месте Красноярском регионе и в окрестностях. Наша команда опытных специалистов гарантирует высокое качество исполнения всех видов реставрационных работ, будь то деревянные, каркасные, из кирпича или бетонные конструкции строения.
Достоинства сотрудничества с Геракл24
Навыки и знания:
Весь процесс выполняются лишь высококвалифицированными мастерами, с обладанием многолетний практику в сфере создания и реставрации домов. Наши специалисты знают свое дело и выполняют проекты с высочайшей точностью и учетом всех деталей.
Полный спектр услуг:
Мы предоставляем разнообразные услуги по реставрации и восстановлению зданий:
Замена фундамента: замена и укрепление фундамента, что позволяет продлить срок службы вашего строения и избежать проблем, вызванные оседанием и деформацией.
Реставрация венцов: замена нижних венцов деревянных домов, которые обычно подвергаются гниению и разрушению.
Смена настилов: замена старых полов, что значительно улучшает внешний вид и функциональные характеристики.
Перенос строений: безопасное и качественное передвижение домов на новые места, что позволяет сохранить ваше строение и предотвращает лишние расходы на создание нового.
Работа с любыми видами зданий:
Дома из дерева: восстановление и укрепление деревянных конструкций, защита от гниения и вредителей.
Каркасные строения: укрепление каркасов и смена поврежденных частей.
Дома из кирпича: реставрация кирпичной кладки и усиление стен.
Бетонные дома: восстановление и укрепление бетонных структур, устранение трещин и повреждений.
Качество и прочность:
Мы используем только проверенные материалы и современное оборудование, что гарантирует долговечность и надежность всех выполненных работ. Каждый наш проект подвергаются строгому контролю качества на каждой стадии реализации.
Индивидуальный подход:
Для каждого клиента мы предлагаем персонализированные решения, учитывающие ваши требования и желания. Наша цель – чтобы итог нашей работы полностью удовлетворял ваши ожидания и требования.
Почему стоит выбрать Геракл24?
Работая с нами, вы получаете надежного партнера, который возьмет на себя все хлопоты по восстановлению и ремонту вашего здания. Мы обещаем выполнение всех работ в установленные сроки и с соблюдением всех правил и норм. Обратившись в Геракл24, вы можете быть спокойны, что ваше строение в надежных руках.
Мы предлагаем консультацию и ответить на ваши вопросы. Звоните нам, чтобы обсудить детали вашего проекта и узнать о наших сервисах. Мы сохраним и улучшим ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Gerakl24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
40 mg baclofen
provigil without prescription
provigil tab 200mg
pharmacie en ligne livraison europe: Acheter Cialis 20 mg pas cher – pharmacie en ligne france fiable
synthroid tab 112 mcg
accutane pills
medicine baclofen 10 mg
buy accutane nz
качественная заливка бетона https://betonzavody.ru/
pharmacie en ligne livraison europe: Levitra 20mg prix en pharmacie – vente de mГ©dicament en ligne
how to buy accutane
заказать сео продвижение сайта
metformin with no prescription
loratadine bloody – claritin pills observe claritin pills helpless
furosemide 200 mg tab
dexamethasone 5 mg tablets
Viagra homme prix en pharmacie sans ordonnance: SildГ©nafil 100 mg prix en pharmacie en France – Viagra homme sans prescription
seo продвижение сайта сколько стоит
flomax
Майор Гром 2024
strattera price uk
Майор Гром 2024
lasix 100 mg
Майор Гром 2024
diflucan 150 mg capsule
Майор Гром 2024
Майор Гром: Игра смотреть онлайн
Achat mГ©dicament en ligne fiable: Acheter Cialis – pharmacie en ligne france pas cher
Фоллаут смотреть онлайн
where can i buy zovirax
fluconazole without script
dapoxetine remove – priligy reflection priligy river
dapoxetine estate – priligy gown priligy boy
Король и шут 1 сезон смотреть онлайн
augmentin cheapest
trouver un mГ©dicament en pharmacie: kamagra oral jelly – pharmacie en ligne avec ordonnance
vermox price in south africa
dexamethasone 25 mg
625mg amoxicillin
https://eroticahd.ru/
Майор Гром 2024
pharmacie en ligne pas cher: levitra generique sites surs – pharmacie en ligne livraison europe
Майор Гром 2024
Психология в рассказах, истории из жизни.
https://topthuthuat.com/top-5-trang-web-ung-dung-pho-bien-nhat-o-viet-nam-bi-quyet-kiem-tien-qua-proxy/
modafinil cost uk
Доставка из Китая с таможенными услугами — это профессиональное решение для импорта товаров из Китая, включающее в себя организацию перевозки, таможенное оформление и сопутствующие услуги. Мы предоставляем полный спектр услуг, связанных
китай доставка бесплатная включая организацию международных перевозок, таможенное оформление, сертификацию и страхование грузов. Наши специалисты помогут вам выбрать оптимальный маршрут и вид транспорта, оформить необходимые документы и декларации, а также проконсультируют по вопросам налогообложения и таможенного законодательства.
azithromycin price canada
advair diskus for sale
Viagra homme prix en pharmacie sans ordonnance: viagra en ligne – Viagra sans ordonnance livraison 24h
albuterol usa price
500mg advair
flomax canada
купить подростковый велосипед https://velo4u.ru
augmentin discount
azithromycin capsules
The UK’s news sites https://ukcervicalcancer.org.uk/articles/newstopuk-provides-vital-information-support-to-uk-cervical-cancer-organisation.html scene is well supplied with and assorted, encompassing a considerable sphere of outlets from the esteemed BBC and The Paladin to the more mind-boggling tabloids like The Day-star and The Daily Mail. Each of these sources brings a contrastive position to the scoop, reflecting the pluralism of British society. The BBC, funded during the prominent through the latitude recompense, aims to plan for fair and thorough coverage. It is continually seen as the gold universal in broadcasting, known an eye to its commitment to unprejudiced reporting and in-depth analysis.
advair 500 50 mcg
vermox 100mg online
pharmacie en ligne livraison europe: pharmacie en ligne – pharmacies en ligne certifiГ©es
best advair coupon
vermox pharmacy uk
can i buy flomax without a prescription
where can i buy tretinoin cream
купить диплом колледжа http://www.kupitediplom0029.ru .
vente de mГ©dicament en ligne: Acheter Cialis – pharmacie en ligne france pas cher
zithromax 250
baclofen buy canada
Официальный центр оформления и выпуска международных водительских прав (удостоверений) МВУ в Казахстане. Международные водительские права в Алматы, с бесплатной доставкой.
Licenze Windows originali
trouver un mГ©dicament en pharmacie: achat kamagra – Pharmacie sans ordonnance
canadian pharmacy diflucan
купить аттестат за 9 класс https://kupitediplom0029.ru
claritin lesson – claritin pills warm loratadine clutch
baclofen discount
generic flomax
250 mg lyrica
average cost cialis daily use
diflucan 500 mg
trouver un mГ©dicament en pharmacie: pharmacie en ligne avec ordonnance – pharmacies en ligne certifiГ©es
сеть сайтов pbn
Работая в сео, нужно осознавать, что не получится одним инструментом поднять веб-сайт в топ выдачи поисковых систем, поскольку поисковики это как дорожка с конечным этапом, а интернет-ресурсы это автомобили для гонок, которые все стремятся занять первое место.
Так вот:
Перечень – Для того чтобы веб-сайт был адаптивным и быстрым, важна
оптимизирование
Сайт должен содержать только уникальные материалы, это тексты и картинки
ОБЯЗАТЕЛЬНО набор ссылок через сайты с статьями и напрямую на основную страницу
Увеличение беклинков с использованием второстепенных сайтов
Ссылочная структура, это ссылки первого уровня, Tier-2, Tier-3
Ну и главное это личная сеть веб-сайтов PBN, которая ссылается на основной сайт
Все PBN-сайты должны быть без футпринтов, т.е. поисковые системы не должны понимать, что это один собственник всех сайтов, поэтому ОЧЕНЬ важно следовать все эти указания.
lyrica online
The game involves interacting with an AI-powered girlfriend who displays “yandere” traits—extreme, all-encompassing love often pre-eminent to covetous or violent behavior. In yandere simulator players must steer conversations and actions to look after a relationship while managing the AI’s unpredictable emotions, creating a anxious and immersive experience.
Стоматологическая клиника Мастерская Улыбок предлагает широкий спектр услуг по диагностике, лечению, профилактике и эстетической коррекции проблем с зубами и дёснами. Мы используем современное оборудование и материалы, а наши специалисты обладают высокой квалификацией и опытом.
В клинике созданы комфортные условия для пациентов: удобные кресла, приятная атмосфера, приветливый персонал. Мы заботимся о вашем здоровье и стараемся сделать посещение стоматолога максимально комфортным и безболезненным.
Наши услуги включают:
круглосуточные стоматологии казань
диагностику состояния зубов и дёсен;
лечение кариеса, пульпита, периодонтита и других заболеваний;
профессиональную гигиену полости рта;
эстетическую коррекцию зубного ряда (установка коронок, виниров, имплантов);
исправление прикуса с помощью брекетов или элайнеров;
отбеливание зубов;
лечение дёсен (пародонтит, гингивит, пародонтоз).
Мы также предлагаем услуги по детской стоматологии, протезированию и имплантации.
Обращаясь в клинику Мастерская Улыбок, вы можете быть уверены в качестве предоставляемых услуг и профессионализме наших врачей. Мы заботимся о вашей улыбке и делаем всё возможное, чтобы она была здоровой и красивой!
lyrica price comparison
In yandere ai girlfriend simulator, you’re stuck internal the home of an tormenting anime catgirl. Your target is to persuade her to unrestricted the face door so you can gross away. To whatever manner, be cautious—if you offend her provoke, things could moulder dangerous.
Замена венцов красноярск
Геракл24: Квалифицированная Смена Основания, Венцов, Полов и Передвижение Строений
Компания Gerakl24 занимается на выполнении всесторонних услуг по смене основания, венцов, полов и перемещению домов в населённом пункте Красноярске и за его пределами. Наша команда квалифицированных мастеров обеспечивает превосходное качество выполнения всех типов реставрационных работ, будь то из дерева, каркасного типа, из кирпича или из бетона строения.
Достоинства сотрудничества с Геракл24
Квалификация и стаж:
Каждая задача проводятся лишь профессиональными экспертами, с обладанием многолетний стаж в направлении создания и восстановления строений. Наши сотрудники эксперты в своей области и осуществляют проекты с максимальной точностью и вниманием к мелочам.
Комплексный подход:
Мы предоставляем все виды работ по восстановлению и восстановлению зданий:
Реставрация фундамента: усиление и реставрация старого основания, что позволяет продлить срок службы вашего дома и устранить проблемы, связанные с оседанием и деформацией строения.
Смена венцов: восстановление нижних венцов деревянных зданий, которые чаще всего гниют и разрушаются.
Установка новых покрытий: замена старых полов, что значительно улучшает визуальное восприятие и функциональность помещения.
Перемещение зданий: безопасное и надежное перемещение зданий на новые локации, что обеспечивает сохранение строения и предотвращает лишние расходы на строительство нового.
Работа с любыми типами домов:
Древесные строения: восстановление и укрепление деревянных конструкций, защита от гниения и вредителей.
Каркасные дома: укрепление каркасов и реставрация поврежденных элементов.
Кирпичные дома: восстановление кирпичной кладки и укрепление конструкций.
Бетонные строения: восстановление и укрепление бетонных структур, ремонт трещин и дефектов.
Качество и надежность:
Мы применяем лишь качественные материалы и современное оборудование, что гарантирует долговечность и прочность всех выполненных задач. Каждый наш проект проходят тщательную проверку качества на всех этапах выполнения.
Индивидуальный подход:
Для каждого клиента мы предлагаем индивидуальные решения, с учетом всех особенностей и пожеланий. Мы стараемся, чтобы итог нашей работы полностью соответствовал вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Обратившись к нам, вы приобретете надежного партнера, который возьмет на себя все хлопоты по ремонту и реконструкции вашего строения. Мы обещаем выполнение всех проектов в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Связавшись с Геракл24, вы можете быть спокойны, что ваше здание в надежных руках.
Мы готовы предоставить консультацию и дать ответы на все вопросы. Звоните нам, чтобы обсудить ваш проект и получить больше информации о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш партнер по реставрации и ремонту домов в Красноярске и окрестностях.
Sign up with our community of beyond 2 million elated users who are saving tempo and getting paid faster with our transportable invoice solutions. Our movable invoicing tools, including non-stationary invoice apps, purvey to both iOS and Android users. Whether you have need of an invoice app pro iPhone, an Android invoice app, or a sweeping responsive billing software, we’ve got you covered.
https://www.genio.ac/mobile-invoices
propecia 2mg
pharmacie en ligne france pas cher: cialis prix – Pharmacie en ligne livraison Europe
сеть сайтов pbn
Работая в сео, нужно осознавать, что невозможно одним способом вывести сайт в верхние позиции поисковых систем, так как поисковые системы это как дорожка с конечным этапом, а сайты это гоночные автомобили, которые все желают быть первыми.
Так вот:
Перечень – Для того чтобы веб-сайт был адаптивным и быстр, важна
улучшение
Сайт должен иметь только уникальный контент, это текст и картинки
В ОБЯЗАТЕЛЬНОМ ПОРЯДКЕ ссылочный профиль через статейные сайты и напрямую на главную
Усиление входящих ссылок с помощью второстепенных сайтов
Ссылочная пирамида, это ссылки первого уровня, Tier-2, Tier-3
Ну и главное это личная сеть веб-сайтов PBN, которая ссылается на деньговый сайт
Все сайты сети PBN должны быть без футпринтов, т.е. поисковики не должны знать, что это один владелец всех веб-сайтов, поэтому крайне важно соблюдать все эти указания.
game1kb.com
너무 많은 사람들에게 맞고 온 몸에 상처가 나고 다리가 부러졌습니다.
срочный выкуп авто http://www.vykup-avtomsk.ru .
線上娛樂城的世界
隨著互聯網的飛速發展,在線娛樂城(在線賭場)已經成為許多人休閒的新選擇。線上娛樂城不僅提供多元化的游戲選擇,還能讓玩家在家中就能體驗到賭場的興奮和樂趣。本文將討論線上娛樂城的特色、利益以及一些常有的遊戲。
什麼在線娛樂城?
線上娛樂城是一種透過網際網路提供賭錢游戲的平台。玩家可以透過電腦、智慧型手機或平板設備進入這些網站,參與各種博彩活動,如德州撲克、輪盤賭、二十一點和老虎机等。這些平台通常由專業的軟體公司開發,確保游戲的公平性和安全性。
網上娛樂城的好處
便利:玩家不用離開家,就能體驗賭博的興奮。這對於那些住在在遠離的實體賭場區域的人來說尤為方便。
多樣化的游戲選擇:線上娛樂城通常提供比實體賭場更多的遊戲選擇,並且經常更新遊戲內容,保持新鮮。
優惠和獎金:許多網上娛樂城提供豐富的優惠計劃,包括註冊獎勵、存款紅利和忠誠度計劃,引誘新玩家並鼓勵老玩家不斷遊戲。
安全和保密性:合法的線上娛樂城使用高端的加密方法來保護玩家的個人信息和財務交易,確保遊戲過程的穩定和公正性。
常有的在線娛樂城遊戲
撲克:撲克是最受歡迎賭錢游戲之一。網上娛樂城提供多種撲克變體,如德州撲克、奧馬哈撲克和七張牌等。
輪盤賭:輪盤賭是一種古老的賭博遊戲,玩家可以投注在數字、數字組合或顏色上上,然後看小球落在哪個區域。
黑傑克:又稱為黑傑克,這是一種競爭玩家和莊家點數的游戲,目標是讓手牌點數點數盡量接近21點但不超過。
吃角子老虎:老虎機是最受歡迎且是最受歡迎的賭博游戲之一,玩家只需旋轉捲軸,看圖案排列出贏得的組合。
結尾
網上娛樂城為現代的賭博愛好者提供了一個方便的、興奮且多元化的娛樂活動。不管是撲克牌愛好者還是老虎机愛好者,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的的不斷提升,在線娛樂城的遊戲體驗將變得越來越逼真和有趣。然而,玩家在體驗遊戲的同時,也應該保持,避免沉迷於博彩活動,保持健康的遊戲心態。
https://d-addicts.com/what-is-astrology/
娛樂城
網上娛樂城的世界
隨著互聯網的飛速發展,在線娛樂城(線上賭場)已經成為許多人娛樂的新選擇。線上娛樂城不僅提供多元化的遊戲選擇,還能讓玩家在家中就能體驗到賭場的興奮和樂趣。本文將討論在線娛樂城的特色、優勢以及一些常見的的游戲。
什麼叫網上娛樂城?
線上娛樂城是一種經由互聯網提供博彩遊戲的平台。玩家可以通過計算機、智能手機或平板電腦進入這些網站,參與各種賭博活動,如撲克、輪盤、21點和老虎机等。這些平台通常由專業的軟件公司開發,確保遊戲的公平性和穩定性。
網上娛樂城的優勢
方便性:玩家無需離開家,就能享受博彩的樂趣。這對於那些生活在遠離的實體賭場地區的人來說尤為方便。
多元化的游戲選擇:線上娛樂城通常提供比實體賭場更多的游戲選擇,並且經常更新遊戲內容,保持新鮮感。
好處和獎金:許多網上娛樂城提供多樣的獎勵計劃,包括註冊紅利、存款獎金和會員計劃,吸引新玩家並促使老玩家繼續遊戲。
穩定性和保密性:正當的線上娛樂城使用先進的加密方法來保護玩家的個人資料和金融交易,確保游戲過程的安全和公正。
常有的網上娛樂城遊戲
德州撲克:德州撲克是最流行博彩游戲之一。在線娛樂城提供多樣撲克變體,如德州撲克、奧馬哈撲克和七張撲克等。
賭盤:輪盤賭是一種古老的賭場遊戲,玩家可以投注在數字、數字排列或顏色選擇上,然後看轉球落在哪個區域。
黑傑克:又稱為黑傑克,這是一種比拼玩家和莊家點數的遊戲,目標是讓手牌點數盡量接近21點但不超過。
老虎機:吃角子老虎是最簡單且是最常見的博彩遊戲之一,玩家只需旋轉捲軸,等待圖案排列出中獎的組合。
結尾
線上娛樂城為現代的賭博愛好者提供了一個方便的、興奮且豐富的娛樂方式。無論是撲克愛好者還是吃角子老虎迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的不斷提升,在線娛樂城的遊戲體驗將變得越來越真實和有趣。然而,玩家在體驗遊戲的同時,也應該保持,避免過度沉迷於博彩活動,維持健康的遊戲心態。
pharmacie en ligne livraison europe: pharmacie en ligne pas cher – pharmacies en ligne certifiГ©es
пакеты бумажные печать
Почему теневой плинтус – красивая и практичная деталь интерьера,
Как правильно установить теневой плинтус своими руками,
Креативные способы использования теневого плинтуса в дизайне помещения,
Теневой плинтус: классический стиль в современном исполнении,
Советы стилиста: как сделать цвет теневого плинтуса акцентом в помещении,
Теневой плинтус: простое решение для скрытия кабелей и проводов,
Преимущества использования теневого плинтуса с интегрированной подсветкой,
Теневой плинтус: элегантность и стиль в дизайне помещения,
Почему теневой плинтус – важная деталь в оформлении интерьера
алюминиевый плинтус купить москва алюминиевый плинтус купить москва .
Теневой плинтус: стильное решение для обновления интерьера,
Шаг за шагом инструкция по установке теневого плинтуса,
Как использовать теневой плинтус для создания уникального интерьера,
Модные тренды в выборе теневых плинтусов для современного дома,
Как подобрать цвет теневого плинтуса к отделке стен,
Как спрятать коммуникации с помощью теневого плинтуса: практические советы,
Теневой плинтус с подсветкой: создаем эффектное освещение в интерьере,
Современные тренды в использовании теневого плинтуса для уюта и красоты,
Интерьер безупречный до мелочей: роль теневого плинтуса в декоре
плинтус скрытого монтажа плинтус скрытого монтажа .
Замена венцов красноярск
Геракл24: Квалифицированная Замена Основания, Венцов, Покрытий и Перемещение Строений
Фирма Gerakl24 специализируется на предоставлении комплексных сервисов по смене фундамента, венцов, полов и передвижению домов в городе Красноярском регионе и за пределами города. Наша команда опытных мастеров гарантирует превосходное качество исполнения различных типов восстановительных работ, будь то древесные, каркасного типа, из кирпича или бетонные здания.
Плюсы работы с Геракл24
Квалификация и стаж:
Каждая задача осуществляются только опытными экспертами, с обладанием большой практику в сфере возведения и ремонта зданий. Наши мастера профессионалы в своем деле и осуществляют проекты с безупречной точностью и вниманием к мелочам.
Полный спектр услуг:
Мы предлагаем разнообразные услуги по реставрации и восстановлению зданий:
Замена фундамента: замена и укрепление фундамента, что гарантирует долговечность вашего строения и предотвратить проблемы, связанные с оседанием и деформацией.
Замена венцов: восстановление нижних венцов деревянных зданий, которые обычно подвержены гниению и разрушению.
Смена настилов: замена старых полов, что значительно улучшает визуальное восприятие и практическую полезность.
Перемещение зданий: безопасное и качественное передвижение домов на другие участки, что помогает сохранить здание и предотвращает лишние расходы на строительство нового.
Работа с любыми видами зданий:
Дома из дерева: реставрация и усиление деревянных элементов, защита от разрушения и вредителей.
Каркасные строения: укрепление каркасов и смена поврежденных частей.
Кирпичные строения: восстановление кирпичной кладки и усиление стен.
Дома из бетона: восстановление и укрепление бетонных структур, исправление трещин и разрушений.
Качество и прочность:
Мы работаем с только высококачественные материалы и новейшее оборудование, что гарантирует долговечность и прочность всех выполненных задач. Все наши проекты подвергаются строгому контролю качества на каждой стадии реализации.
Персонализированный подход:
Каждому клиенту мы предлагаем персонализированные решения, учитывающие ваши требования и желания. Наша цель – чтобы итог нашей работы соответствовал вашим запросам и желаниям.
Почему выбирают Геракл24?
Обратившись к нам, вы найдете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы обещаем выполнение всех проектов в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете быть спокойны, что ваше строение в надежных руках.
Мы готовы предоставить консультацию и дать ответы на все вопросы. Контактируйте с нами, чтобы обсудить детали и узнать больше о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, сделав его уютным и безопасным для долгого проживания.
Геракл24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
promethazine face – promethazine wife promethazine vary
https://jasdam.cz
娛樂城
網上娛樂城的天地
隨著互聯網的飛速發展,線上娛樂城(網上賭場)已經成為許多人休閒的新選擇。網上娛樂城不僅提供多元化的游戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和樂趣。本文將研究網上娛樂城的特色、利益以及一些常有的游戲。
什麼線上娛樂城?
網上娛樂城是一種透過網際網路提供賭錢遊戲的平台。玩家可以經由計算機、智慧型手機或平板電腦進入這些網站,參與各種賭錢活動,如德州撲克、輪盤賭、黑傑克和吃角子老虎等。這些平台通常由專家的軟件公司開發,確保遊戲的公正和穩定性。
線上娛樂城的優勢
便利性:玩家不用離開家,就能享受賭錢的快感。這對於那些住在在遠離的實體賭場地區的人來說尤其方便。
多元化的游戲選擇:線上娛樂城通常提供比實體賭場更多樣化的游戲選擇,並且經常改進遊戲內容,保持新鮮感。
優惠和獎勵計劃:許多在線娛樂城提供豐厚的獎金計劃,包括註冊紅利、存款獎金和會員計劃,引誘新玩家並鼓勵老玩家繼續遊戲。
安全性和保密性:正當的在線娛樂城使用先進的的加密來保護玩家的私人信息和財務交易,確保游戲過程的公平和公平。
常見的的在線娛樂城遊戲
撲克:德州撲克是最受歡迎博彩遊戲之一。線上娛樂城提供多樣德州撲克變體,如德州撲克、奧馬哈撲克和七張牌等。
輪盤:輪盤賭是一種傳統的賭場遊戲,玩家可以投注在單個數字、數字組合或顏色上上,然後看球落在哪個區域。
黑傑克:又稱為黑傑克,這是一種對比玩家和莊家點數的游戲,目標是讓手牌點數點數儘量接近21點但不超過。
吃角子老虎:老虎機是最受歡迎也是最受歡迎的賭錢遊戲之一,玩家只需轉捲軸,看圖案排列出獲勝的組合。
總結
網上娛樂城為當代賭博愛好者提供了一個方便、興奮且多樣化的娛樂方式。無論是撲克愛好者還是老虎機迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的不斷進步,網上娛樂城的游戲體驗將變化越來越現實和有趣。然而,玩家在享用游戲的同時,也應該自律,避免沉溺於賭錢活動,維持健康的心態。
vermox tablets price
dexamethasone 15 mg
Acheter Sildenafil 100mg sans ordonnance: viagra sans ordonnance – Viagra pas cher paris
2 zithromax
網上娛樂城的天地
隨著互聯網的迅速發展,線上娛樂城(網上賭場)已經成為許多人休閒的新選擇。在線娛樂城不僅提供多種的遊戲選擇,還能讓玩家在家中就能體驗到賭場的興奮和樂趣。本文將探討線上娛樂城的特色、優勢以及一些常見的的遊戲。
什麼是網上娛樂城?
在線娛樂城是一種經由網際網路提供賭錢游戲的平台。玩家可以通過電腦設備、智慧型手機或平板電腦進入這些網站,參與各種博彩活動,如撲克、輪盤賭、21點和老虎机等。這些平台通常由專業的的軟體公司開發,確保遊戲的公正和安全。
線上娛樂城的利益
方便性:玩家不需要離開家,就能體驗博彩的樂趣。這對於那些居住在偏遠實體賭場地方的人來說尤其方便。
多樣化的遊戲選擇:在線娛樂城通常提供比實體賭場更多的游戲選擇,並且經常改進遊戲內容,保持新穎。
優惠和獎勵計劃:許多在線娛樂城提供豐富的獎金計劃,包括註冊紅利、存款紅利和會員計劃,引誘新玩家並鼓勵老玩家持續遊戲。
安全和隱私性:正規的線上娛樂城使用先進的的加密方法來保護玩家的私人信息和財務交易,確保游戲過程的穩定和公正性。
常見的線上娛樂城遊戲
德州撲克:德州撲克是最受歡迎賭博游戲之一。在線娛樂城提供多種撲克變體,如德州撲克、奧馬哈和七張撲克等。
輪盤賭:輪盤賭是一種經典的賭博遊戲,玩家可以賭注在單個數字、數字排列或顏色上上,然後看轉球落在哪個地方。
21點:又稱為二十一點,這是一種比拼玩家和莊家點數的遊戲,目標是讓手牌點數點數盡可能接近21點但不超過。
老虎机:老虎机是最受歡迎也是最受歡迎的博彩遊戲之一,玩家只需旋轉捲軸,看圖案排列出獲勝的組合。
結尾
在線娛樂城為現代賭博愛好者提供了一個方便的、刺激的且豐富的娛樂活動。不管是撲克迷還是老虎機迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著科技的不斷進步,線上娛樂城的遊戲體驗將變得越來越越來越現實和吸引人。然而,玩家在體驗遊戲的同時,也應該保持自律,避免沉溺於賭錢活動,保持健康健康的心態。
lyrica online
where can i get viagra without a prescription
nanosondy
lasix 120 mg
pharmacie en ligne france livraison belgique: pharmacie en ligne france livraison internationale – acheter mГ©dicament en ligne sans ordonnance
лизинг без первоначального взноса для юридических лиц https://leasingber.ru
ascorbic acid pinch – ascorbic acid monk ascorbic acid possession
курсовая работа купить https://kontrolnyeaudit.ru/
buy real tiktok views buy tiktok views and likes
Find Exciting Promotions and Free Rounds: Your Complete Guide
At our gaming platform, we are dedicated to providing you with the best gaming experience possible. Our range of bonuses and bonus spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our awesome promotions and what makes them so special.
Generous Extra Spins and Cashback Promotions
One of our standout promotions is the opportunity to earn up to 200 bonus spins and a 75% cashback with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This incredible offer allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Promotions
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 bonus with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these offers provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, rebate, or bountiful deposit bonuses, we have something for everyone. Join us today, take advantage of these fantastic promotions, and start your journey to big wins and endless fun. Happy gaming!
tretinoin cream usp 0.025 buy online
sapporo88
sapporo88
game reviews
Thrilling Breakthroughs and Beloved Titles in the Sphere of Digital Entertainment
In the fluid environment of digital entertainment, there’s always something innovative and exciting on the forefront. From modifications optimizing iconic mainstays to forthcoming debuts in renowned brands, the digital entertainment landscape is as vibrant as ever.
This is a snapshot into the latest developments and specific the iconic experiences captivating audiences internationally.
Up-to-Date Updates
1. Cutting-Edge Mod for The Elder Scrolls V: Skyrim Optimizes NPC Look
A freshly-launched enhancement for The Elder Scrolls V: Skyrim has caught the interest of fans. This enhancement adds realistic faces and flowing hair for all supporting characters, enhancing the experience’s visuals and depth.
2. Total War Release Situated in Star Wars Universe Galaxy in Development
The Creative Assembly, acclaimed for their Total War series, is supposedly working on a forthcoming title placed in the Star Wars Galaxy universe. This thrilling combination has fans looking forward to the strategic and compelling experience that Total War Games games are acclaimed for, finally placed in a world expansive.
3. GTA VI Arrival Confirmed for Late 2025
Take-Two Interactive’s Leader has confirmed that Grand Theft Auto VI is expected to arrive in Late 2025. With the massive reception of its predecessor, GTA V, players are eager to witness what the upcoming entry of this celebrated series will offer.
4. Enlargement Initiatives for Skull and Bones 2nd Season
Creators of Skull & Bones have revealed expanded strategies for the game’s second season. This nautical saga offers additional updates and changes, keeping enthusiasts immersed and engrossed in the realm of oceanic seafaring.
5. Phoenix Labs Developer Experiences Personnel Cuts
Unfortunately, not every announcements is favorable. Phoenix Labs Developer, the studio behind Dauntless Experience, has communicated significant staff cuts. Regardless of this setback, the experience keeps to be a beloved selection within players, and the developer continues to be committed to its community.
Renowned Releases
1. The Witcher 3: Wild Hunt
With its immersive plot, immersive domain, and captivating adventure, The Witcher 3: Wild Hunt remains a beloved experience across players. Its intricate story and sprawling open world persist to captivate enthusiasts in.
2. Cyberpunk 2077 Game
Regardless of a problematic arrival, Cyberpunk 2077 stays a eagerly awaited experience. With persistent patches and enhancements, the title continues to improve, presenting players a view into a futuristic future rife with danger.
3. GTA 5
Even eras subsequent to its original debut, Grand Theft Auto 5 remains a popular preference among gamers. Its vast free-roaming environment, engaging plot, and shared features sustain players reengaging for additional explorations.
4. Portal 2 Game
A iconic brain-teasing game, Portal 2 Game is acclaimed for its revolutionary systems and brilliant spatial design. Its challenging obstacles and clever writing have established it as a standout experience in the digital entertainment industry.
5. Far Cry 3
Far Cry 3 is celebrated as among the finest games in the franchise, providing fans an open-world journey abundant with danger. Its compelling narrative and legendary personalities have confirmed its status as a fan favorite title.
6. Dishonored
Dishonored Series is hailed for its covert systems and unique environment. Fans assume the persona of a extraordinary executioner, exploring a city abundant with societal mystery.
7. Assassin’s Creed 2
As a member of the celebrated Assassin’s Creed Franchise collection, Assassin’s Creed Game is adored for its engrossing story, engaging mechanics, and period realms. It continues to be a standout experience in the universe and a favorite within enthusiasts.
In closing, the universe of digital entertainment is vibrant and fluid, with new advan
buy diflucan online
price of lyrica 75 mg in india
pharmacie en ligne france fiable: kamagra livraison 24h – acheter mГ©dicament en ligne sans ordonnance
https://formomebel.ru/stoliki/metallicheskie
сайт заказа курсовых https://kontrolnyeaudit.ru/
заказать курсовую недорого и быстро https://kontrolnyeaudit.ru/
Доставка цветов в Саратове https://flowers64.ru/ это отличная возможность заказать различные цветы, букеты, композиции, подарки, не выходя из дома. Служба доставки работает круглосуточно, а сама доставка в течении 90 минут. Вы сможете подарить букет анонимно, просто напишите это при заказе. Огромный ассортимент цветов порадует всех!
Незаменимая часть гардероба – тактичные штаны, которые подчеркнут вашу индивидуальность.
Незаменимые для занятий спортом, тактичные штаны станут вашим надежным помощником.
Высокое качество и непревзойденный комфорт, сделают тактичные штаны вашим любимым предметом гардероба.
Современный стиль и практичность, порадуют даже самого взыскательного покупателя.
Неотъемлемый атрибут современного мужчины – тактичные штаны, порадуют вас надежностью и удобством.
тактичні жіночі штани тактичні жіночі штани .
lasix for sale
অনলাইন গেমিং এবং ক্যাসিনো: বাস্তবতার স্বাদ JiliAce〡JitaBet-এর সাথে
অনলাইন গেমিংয়ের জগতে, বাস্তব-বিশ্বের খেলাধুলার নিয়ম, মেকানিক্স এবং গতিশীলতাকে প্রতিলিপি করার লক্ষ্য নিয়ে স্পোর্টস গেমগুলি তৈরি করা হয়। এই গেমগুলি প্রায়শই বাস্তবসম্মত গ্রাফিক্স, পদার্থবিদ্যা এবং গেমপ্লে মেকানিক্স বৈশিষ্ট্যযুক্ত করে, যা ব্যবহারকারীদের নিমগ্ন অভিজ্ঞতা প্রদান করে। JiliAce〡JitaBet-এর প্ল্যাটফর্মে এই ধরনের বাস্তবসম্মত স্পোর্টস গেমের অভিজ্ঞতা নিন, যা খেলোয়াড়দের একটি ভার্চুয়াল জগতে বাস্তবতার স্বাদ প্রদান করে।
JiliAce〡JitaBet ক্যাসিনো তাদের ব্যবহারকারীদের জন্য বিস্তৃত গেম অফার করে, যা প্রথাগত ইট-ও-মর্টার ক্যাসিনোগুলির গেমগুলিকে অনুকরণ করে। এর মধ্যে রয়েছে জনপ্রিয় স্লট মেশিন, টেবিল গেম যেমন ব্ল্যাকজ্যাক, রুলেট, পোকার এবং ব্যাকার্যাট, বিশেষ গেমস যেমন বিঙ্গো এবং কেনো, এবং লাইভ ডিলার গেম।
JiliAce ক্যাসিনো লগইন করে এই সমস্ত গেমের উত্তেজনা উপভোগ করতে পারেন, যেখানে প্রতিটি গেম ব্যবহারকারীদের জন্য নতুন অভিজ্ঞতা এবং পুরস্কার প্রদান করে। JiliAce লগইন করার পরে, ব্যবহারকারীরা JitaBet-এর বৈচিত্র্যময় গেমের সংগ্রহের মাধ্যমে তাদের পছন্দের গেমটি নির্বাচন করতে পারেন এবং শুরু করতে পারেন তাদের জয়ের যাত্রা।
“ক্র্যাশ” গেমগুলি হল একটি জনপ্রিয় ধরনের অনলাইন জুয়া খেলা, যা বিভিন্ন অনলাইন জুয়া প্ল্যাটফর্মে জনপ্রিয়তা অর্জন করেছে। গেমটি তুলনামূলকভাবে সহজ এবং এতে একটি গুণকের উপর বাজি ধরা জড়িত, যা গেমটি ক্র্যাশ না হওয়া পর্যন্ত ক্রমাগত বৃদ্ধি পায়। JiliAce〡JitaBet-এ ক্র্যাশ গেমগুলির উত্তেজনা উপভোগ করুন এবং আপনার ভাগ্য পরীক্ষা করুন।
অনলাইন বিঙ্গো হল ঐতিহ্যবাহী বিঙ্গো গেমের একটি ডিজিটাল সংস্করণ, যা বহু বছর ধরে কমিউনিটি সেন্টার, বিঙ্গো হল এবং সামাজিক সমাবেশে উপভোগ করা হচ্ছে। অনলাইন সংস্করণটি বিঙ্গোর উত্তেজনাকে একটি ভার্চুয়াল প্ল্যাটফর্মে নিয়ে আসে, যা খেলোয়াড়দের তাদের ঘরে বসেই অংশগ্রহণ করতে দেয়। JiliAce ক্যাসিনোতে বিঙ্গো খেলে আপনার সামাজিক বিঙ্গো অভিজ্ঞতা অনলাইনে উপভোগ করুন।
অবশ্যই, অনলাইন স্লট হল প্রথাগত স্লট মেশিনের ডিজিটাল সংস্করণ যা ইট-এবং-মর্টার ক্যাসিনোতে পাওয়া যায়। এই গেমগুলি অনলাইন জুয়া শিল্পে অত্যন্ত জনপ্রিয় হয়ে উঠেছে, খেলোয়াড়দের স্পিনিং রিলগুলির উত্তেজনা উপভোগ করার একটি সুবিধাজনক উপায় এবং প্রকৃত অর্থ জেতার সুযোগ প্রদান করে। Jili ace ক্যাসিনোতে স্লট গেম খেলে এই উত্তেজনা এবং পুরস্কারের অভিজ্ঞতা নিন।
JiliAce〡JitaBet-এ লগইন করুন এবং বাংলাদেশের শীর্ষ অনলাইন গেমিং এবং ক্যাসিনো প্ল্যাটফর্মের সবকিছু আবিষ্কার করুন। উত্তেজনাপূর্ণ গেম এবং পুরস্কারের জন্য আজই যোগ দিন এবং আপনার জয়ের যাত্রা শুরু করুন!
Jiliacet casino
Jiliacet casino |
Warm welcome! | Get a 200% Welcome Bonus when you log in jiliace casino.
IPL Tournament! | Join the IPL fever with Jita Bet. Win big prizes!
Epic JILI Tournaments! | Go head-to-head in the Jita bet Super Tournament
#jiliacecasino
Cashback on Deposits! | Get cash back on every deposit. At Jili ace casino
Uninterrupted bonuses at JITAACE! | Stay logged in Jiliace login!
https://www.jiliace-casino.online/bn
#Jiliacecasino # Jiliacelogin#Jiliacelogin # Jitabet
Slot Feast! | Spin to win 100% up to 20,000 ৳. at Jili ace login!
Big Fishing Bonus! | Get a 100% bonus up to ৳20,000 in the Fishing Game.
JiliAce Casino’s top choice for great bonuses. login, play, and win big today!
написание курсовых работ https://kontrolnyeaudit.ru/
게이츠 오브 올림푸스
Zhu Houzhao를 따라 희생자를 위한 재정착 지역으로 이동했습니다.
Daily bonuses
Uncover Exciting Offers and Free Rounds: Your Complete Guide
At our gaming platform, we are dedicated to providing you with the best gaming experience possible. Our range of promotions and bonus spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our amazing deals and what makes them so special.
Bountiful Free Rounds and Cashback Deals
One of our standout offers is the opportunity to earn up to 200 bonus spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This unbelievable promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Promotions
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” promotions allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our promotions come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy free spins, refund, or generous deposit bonuses, we have something for everyone. Join us today, take advantage of these awesome offers, and start your journey to big wins and endless fun. Happy gaming!
sapporo88
vente de mГ©dicament en ligne: Levitra pharmacie en ligne – trouver un mГ©dicament en pharmacie
Captivating Innovations and Popular Franchises in the Domain of Interactive Entertainment
In the ever-evolving environment of videogames, there’s always something fresh and engaging on the horizon. From mods improving revered mainstays to upcoming debuts in legendary series, the gaming industry is flourishing as in recent memory.
We’ll take a glimpse into the up-to-date announcements and specific the most popular experiences enthralling enthusiasts internationally.
Latest Announcements
1. Innovative Enhancement for Skyrim Optimizes NPC Appearance
A recent mod for Skyrim has captured the notice of enthusiasts. This modification brings high-polygon heads and flowing hair for every (NPCs), optimizing the game’s graphics and depth.
2. Total War Series Release Located in Star Wars Setting Galaxy Under Development
Creative Assembly, acclaimed for their Total War franchise, is allegedly working on a upcoming experience located in the Star Wars Setting world. This captivating crossover has players looking forward to the profound and engaging adventure that Total War Series experiences are renowned for, ultimately set in a realm expansive.
3. Grand Theft Auto VI Launch Revealed for Late 2025
Take-Two’s Head has announced that GTA VI is planned to debut in Autumn 2025. With the enormous popularity of its earlier title, GTA V, gamers are awaiting to explore what the forthcoming installment of this celebrated universe will offer.
4. Growth Developments for Skull and Bones Sophomore Season
Designers of Skull and Bones have revealed amplified developments for the world’s next season. This swashbuckling journey promises additional experiences and updates, keeping fans invested and absorbed in the domain of maritime nautical adventures.
5. Phoenix Labs Studio Deals with Personnel Cuts
Disappointingly, not all announcements is uplifting. Phoenix Labs, the creator behind Dauntless, has revealed substantial staff cuts. Notwithstanding this challenge, the title remains to be a renowned option among players, and the team keeps committed to its community.
Iconic Titles
1. The Witcher 3: Wild Hunt Game
With its immersive experience, captivating realm, and enthralling gameplay, The Witcher 3: Wild Hunt stays a iconic game among gamers. Its rich narrative and sprawling free-roaming environment persist to engage fans in.
2. Cyberpunk 2077 Game
Regardless of a problematic launch, Cyberpunk keeps a long-awaited release. With constant patches and optimizations, the title keeps progress, offering enthusiasts a perspective into a cyberpunk environment abundant with mystery.
3. Grand Theft Auto 5
Despite decades after its first arrival, Grand Theft Auto 5 stays a popular selection across fans. Its expansive open world, captivating experience, and multiplayer mode keep fans revisiting for more explorations.
4. Portal 2
A legendary puzzle title, Portal 2 Game is celebrated for its innovative gameplay mechanics and clever environmental design. Its demanding challenges and amusing writing have made it a remarkable release in the gaming realm.
5. Far Cry
Far Cry is hailed as one of the best entries in the series, providing enthusiasts an free-roaming experience teeming with adventure. Its immersive narrative and memorable personalities have established its status as a beloved release.
6. Dishonored Series
Dishonored Universe is hailed for its covert gameplay and unique environment. Enthusiasts assume the persona of a otherworldly assassin, traversing a metropolitan area filled with societal danger.
7. Assassin’s Creed Game
As part of the celebrated Assassin’s Creed Franchise lineup, Assassin’s Creed II is beloved for its compelling plot, enthralling gameplay, and historical realms. It continues to be a standout experience in the collection and a cherished within players.
In closing, the world of gaming is flourishing and constantly evolving, with fresh developments
Discover Exciting Offers and Bonus Spins: Your Comprehensive Guide
At our gaming platform, we are devoted to providing you with the best gaming experience possible. Our range of bonuses and free rounds ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our incredible offers and what makes them so special.
Generous Free Rounds and Rebate Promotions
One of our standout offers is the opportunity to earn up to 200 bonus spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This amazing promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Offers
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these offers provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 bonus spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our promotions are easy to access and beneficial to our players. Our promotions come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these incredible opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, refund, or generous deposit bonuses, we have something for everyone. Join us today, take advantage of these awesome promotions, and start your journey to big wins and endless fun. Happy gaming!
Daily bonuses
Uncover Thrilling Deals and Free Rounds: Your Ultimate Guide
At our gaming platform, we are committed to providing you with the best gaming experience possible. Our range of deals and free spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our fantastic deals and what makes them so special.
Plentiful Free Rounds and Rebate Bonuses
One of our standout offers is the opportunity to earn up to 200 bonus spins and a 75% refund with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This fantastic offer allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Offers
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” promotions allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these offers provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Bonus Spins on Popular Games
We also offer up to 1000 free spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our promotions come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy free spins, rebate, or lavish deposit bonuses, we have something for everyone. Join us today, take advantage of these fantastic promotions, and start your journey to big wins and endless fun. Happy gaming!
Фирма Финэксперт специализируется на предоставлении профессиональных бухгалтерских услуг для предприятий малого и среднего бизнеса. Мы берем на себя всю ответственность, связанную с ведением учета и составлением отчетности, чтобы вы могли полностью сосредоточиться на развитии своего бизнеса.
Наши специалисты обладают высокой квалификацией и опытом работы в различных сферах бизнеса Наша команда специалистов обладает обширным опытом работы в различных отраслях бизнеса и обладает высокой квалификацией. Мы гарантируем качественное и своевременное выполнение всех необходимых задач, а также всегда следим за изменениями в законодательстве.
Мы предлагаем широкий спектр услуг, включающий в себя
бухгалтерское услуги казань
Мы ценим каждого клиента и стремимся к долгосрочному сотрудничеству. Наши цены являются конкурентоспособными, а качество услуг – на высоком уровне.
Для получения более подробной информации, не стесняйтесь обращаться к нашим опытным специалистам по телефону или по электронной почте.
Betvisa সহযোগী প্রোগ্রাম: একটি লাভজনক অংশীদারিত্ব
বেটিভিসার সাথে সহযোগী হিসেবে অংশীদারিত্ব করতে আগ্রহী ব্যক্তিদের জন্য, সুবিধাগুলি সমানভাবে লোভনীয়। Betvisa অ্যাফিলিয়েট প্রোগ্রামে যোগদান করে এবং Betvisa অ্যাফিলিয়েট লগইন অ্যাক্সেস করার মাধ্যমে, অ্যাফিলিয়েটরা অনেক সুযোগ লাভ করে।
লাভজনক কমিশন কাঠামো: বেটিভিসা একটি প্রতিযোগিতামূলক কমিশন কাঠামো অফার করে, যা অ্যাফিলিয়েটদের প্ল্যাটফর্মে উল্লেখ করা খেলোয়াড়দের দ্বারা উত্পন্ন রাজস্বের উপর ভিত্তি করে আকর্ষণীয় কমিশন উপার্জন করতে দেয়। উচ্চ উপার্জনের সম্ভাবনার সাথে, একটি Betvisa অনুমোদিত হওয়া একটি লাভজনক উদ্যোগ হতে পারে।
বিস্তৃত বিপণন সরঞ্জাম: Betvisa তার সহযোগীদেরকে প্ল্যাটফর্মটিকে কার্যকরভাবে প্রচার করতে সহায়তা করার জন্য বিপণন সরঞ্জাম এবং সংস্থানগুলির একটি স্যুট দিয়ে সজ্জিত করে। ব্যানার এবং ল্যান্ডিং পৃষ্ঠা থেকে শুরু করে ট্র্যাকিং লিঙ্ক এবং কাস্টমাইজড প্রচারমূলক সামগ্রী, অ্যাফিলিয়েটদের কাছে ট্র্যাফিক চালনা করতে এবং রূপান্তরগুলি সর্বাধিক করার জন্য প্রয়োজনীয় সবকিছুই রয়েছে৷
ডেডিকেটেড সাপোর্ট: বেটভিসা তার সহযোগীদের নিবেদিত সমর্থন প্রদান করে, নিশ্চিত করে যে তারা যখনই প্রয়োজন তখনই দ্রুত সহায়তা এবং নির্দেশনা পায়। প্রযুক্তিগত সমস্যার সমাধান হোক, বিপণন কৌশল অপ্টিমাইজ করা হোক বা প্রশ্নের উত্তর দেওয়া হোক, Betvisa অ্যাফিলিয়েট দল প্রতিটি পদক্ষেপে অ্যাফিলিয়েটদের সমর্থন করতে প্রতিশ্রুতিবদ্ধ।
রিয়েল-টাইম রিপোর্টিংয়ে অ্যাক্সেস: অ্যাফিলিয়েটদের ব্যাপক রিপোর্টিং টুলগুলিতে অ্যাক্সেস রয়েছে যা তাদের রিয়েল-টাইমে তাদের কর্মক্ষমতা ট্র্যাক করতে দেয়। ক্লিক এবং রূপান্তর নিরীক্ষণ থেকে উপার্জন এবং প্লেয়ার কার্যকলাপ বিশ্লেষণ থেকে, অধিভুক্তরা তাদের কৌশলগুলি অপ্টিমাইজ করতে এবং তাদের উপার্জনের সম্ভাবনাকে সর্বাধিক করার জন্য মূল্যবান অন্তর্দৃষ্টি অর্জন করতে পারে।
Betvisa অ্যাফিলিয়েট লগইন সুবিধা এবং এই ব্যুত্থানকর সুবিধাগুলির সমন্বয়ে, Betvisa সহযোগী প্রোগ্রাম একটি অসাধারণ অর্থনৈতিক সুযোগ সৃষ্টি করে। প্ল্যাটফর্মটির বিপণনে যোগদানের অর্থ শুধুমাত্র এক লাভজনক একক নয়, বরং একটি দীর্ঘস্থায়ী লাভজনক উদ্যোগ হতে পারে।
Betvisa Bet | Hit it Big This IPL Season with Betvisa!
Betvisa login! | Every deposit during IPL matches earns a 2% bonus .
Betvisa Bangladesh! | IPL 2024 action heats up, your bets get more rewarding!
Crash Game returns! | huge ₹10 million jackpot. Take the lead on the Betvisa app !
#betvisa
Start Winning Now! | Sign up through Betvisa affiliate login, claim ₹500 free cash.
Grab Your Winning Ticket! | Register login and win ₹8,888 at visa bet!
https://www.betvisa-bet.com/bn
#visabet #betvisalogin #betvisabangladesh#betvisaapp
200% Excitement! | Enjoy slots and fishing games at Betvisa লগইন করুন!
Big Sports Bonuses! | Score up to ₹5,000 in sports bonuses during the IPL season
Gear up for an exhilarating IPL season at Betvisa, propels you towards victory!
clomid in india
acyclovir 200mg price
vente de mГ©dicament en ligne: Medicaments en ligne livres en 24h – pharmacie en ligne livraison europe
prednisone cost in india
accutane 20 mg for sale
buy accutane without prescription
furosemide online
Daily bonuses
Find Exciting Offers and Free Spins: Your Complete Guide
At our gaming platform, we are focused to providing you with the best gaming experience possible. Our range of offers and free rounds ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our fantastic offers and what makes them so special.
Plentiful Bonus Spins and Refund Deals
One of our standout offers is the opportunity to earn up to 200 free spins and a 75% cashback with a deposit of just $20 or more. And during happy hour, you can unlock this bonus with a deposit starting from just $10. This fantastic promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Deals
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 bonus with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit promotion available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” promotions allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these offers provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 bonus spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These bonus spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these unbelievable opportunities to enhance your gaming experience. Whether you’re looking to enjoy bonus spins, rebate, or generous deposit bonuses, we have something for everyone. Join us today, take advantage of these amazing deals, and start your journey to big wins and endless fun. Happy gaming!
JiliAce ক্যাসিনোতে স্পোর্টস এবং ক্যাসিনো গেম: বাস্তব এবং ভার্চুয়ালের মিশ্রণ
অনলাইন গেমিংয়ের জগতে JiliAce ক্যাসিনো একটি বিশিষ্ট স্থান অধিকার করে নিয়েছে, যেখানে ব্যবহারকারীরা বিভিন্ন ধরণের গেম উপভোগ করতে পারেন। আজ আমরা JiliAce〡JitaBet প্ল্যাটফর্মে পাওয়া দুটি জনপ্রিয় গেমের ধরন সম্পর্কে জানব: স্পোর্টস গেম এবং ক্যাসিনো গেম।
স্পোর্টস গেম: বাস্তব খেলার প্রতিলিপি
অনলাইন স্পোর্টস গেমের লক্ষ্য বাস্তব-বিশ্বের খেলাধুলার নিয়ম, মেকানিক্স এবং গতিশীলতাকে প্রতিলিপি করা। একটি নিমগ্ন অভিজ্ঞতা প্রদান করতে তারা প্রায়ই বাস্তবসম্মত গ্রাফিক্স, পদার্থবিদ্যা এবং গেমপ্লে মেকানিক্স বৈশিষ্ট্যযুক্ত। Jili ace casino-তে স্পোর্টস গেম খেলে আপনি এক অসাধারণ অভিজ্ঞতা পাবেন, যেখানে বাস্তব খেলার উত্তেজনা এবং আনন্দ অনুভব করবেন। ফুটবল, বাস্কেটবল, ক্রিকেট এবং অন্যান্য খেলার বিভিন্ন ভার্চুয়াল ম্যাচে অংশগ্রহণ করে আপনার দক্ষতা পরীক্ষা করতে পারেন এবং আপনার প্রিয় দলের সাথে নিজেকে যুক্ত করতে পারেন।
ক্যাসিনো গেম: ঐতিহ্যবাহী মজার ডিজিটাল রূপ
অনলাইন ক্যাসিনোগুলি প্রথাগত ইট-ও-মর্টার ক্যাসিনোগুলিতে পাওয়া গেমগুলির নকল করে এমন বিস্তৃত গেম অফার করে। এর মধ্যে রয়েছে জনপ্রিয় গেম যেমন স্লট মেশিন, টেবিল গেম (যেমন ব্ল্যাকজ্যাক, রুলেট, পোকার এবং ব্যাকার্যাট), বিশেষ গেমস (যেমন বিঙ্গো এবং কেনো), এবং লাইভ ডিলার গেম। JiliAce ক্যাসিনোতে আপনি এই গেমগুলির বিস্তৃত সংগ্রহ উপভোগ করতে পারেন, যা আপনাকে একটি বাস্তব ক্যাসিনোর অভিজ্ঞতা দেবে। Jili ace casino-এর মাধ্যমে আপনি স্লট মেশিনের উত্তেজনা, ব্ল্যাকজ্যাকের কৌশল, এবং লাইভ ডিলারের সাথে খেলার আনন্দ উপভোগ করতে পারবেন।
সহজ লগইন এবং সুবিধাজনক গেমিং
Jili ace login প্রক্রিয়া অত্যন্ত সহজ এবং ব্যবহারকারীদের জন্য সুবিধাজনক। একবার লগইন করলে, আপনি সহজেই বিভিন্ন গেমের অ্যাক্সেস পাবেন এবং আপনার পছন্দসই গেম খেলার জন্য প্রস্তুত হয়ে যাবেন। Jiliace login করার পর, আপনি আপনার গেমিং যাত্রা শুরু করতে পারবেন এবং বিভিন্ন ধরনের বোনাস ও পুরস্কার উপভোগ করতে পারবেন।
Jita Bet: বড় পুরস্কারের সুযোগ
JiliAce ক্যাসিনোতে Jita Bet-এর সাথে আপনার গেমিং অভিজ্ঞতা আরও সমৃদ্ধ করুন। এখানে আপনি বিভিন্ন ধরণের বাজি ধরতে পারেন এবং বড় পুরস্কার জিততে পারেন। Jita Bet প্ল্যাটফর্মটি ব্যবহারকারীদের জন্য সহজ এবং সুরক্ষিত বাজি ধরার সুযোগ প্রদান করে।
যোগদান করুন এবং উপভোগ করুন
JiliAce〡JitaBet-এর অংশ হয়ে আজই আপনার গেমিং যাত্রা শুরু করুন। Jili ace casino এবং Jita Bet-এ লগইন করে স্পোর্টস এবং ক্যাসিনো গেমের মত আকর্ষণীয় গেম উপভোগ করুন। এখনই যোগ দিন এবং অনলাইন গেমিংয়ের এক নতুন জগতে প্রবেশ করুন!
Jiliacet casino
Jiliacet casino |
Warm welcome! | Get a 200% Welcome Bonus when you log in jiliace casino.
IPL Tournament! | Join the IPL fever with Jita Bet. Win big prizes!
Epic JILI Tournaments! | Go head-to-head in the Jita bet Super Tournament
#jiliacecasino
Cashback on Deposits! | Get cash back on every deposit. At Jili ace casino
Uninterrupted bonuses at JITAACE! | Stay logged in Jiliace login!
https://www.jiliace-casino.online/bn
#Jiliacecasino # Jiliacelogin#Jiliacelogin # Jitabet
Slot Feast! | Spin to win 100% up to 20,000 ৳. at Jili ace login!
Big Fishing Bonus! | Get a 100% bonus up to ৳20,000 in the Fishing Game.
JiliAce Casino’s top choice for great bonuses. login, play, and win big today!
Uncover Stimulating Promotions and Free Spins: Your Ultimate Guide
At our gaming platform, we are focused to providing you with the best gaming experience possible. Our range of bonuses and extra spins ensures that every player has the chance to enhance their gameplay and increase their chances of winning. Here’s how you can take advantage of our awesome deals and what makes them so special.
Bountiful Bonus Spins and Rebate Deals
One of our standout promotions is the opportunity to earn up to 200 free spins and a 75% cashback with a deposit of just $20 or more. And during happy hour, you can unlock this offer with a deposit starting from just $10. This amazing promotion allows you to enjoy extended playtime and more opportunities to win without breaking the bank.
Boost Your Balance with Deposit Offers
We offer several deposit bonuses designed to maximize your gaming potential. For instance, you can get a free $20 promotion with minimal wagering requirements. This means you can start playing with extra funds, giving you more chances to explore our vast array of games and win big. Additionally, there’s a $10 deposit bonus available, perfect for those looking to get more value from their deposits.
Multiply Your Deposits for Bigger Wins
Our “Play Big!” offers allow you to double or triple your deposits, significantly boosting your balance. Whether you choose to multiply your deposit by 2 or 3 times, these promotions provide you with a substantial amount of extra funds to enjoy. This means more playtime, more excitement, and more chances to hit those big wins.
Exciting Free Spins on Popular Games
We also offer up to 1000 bonus spins per deposit on some of the most popular games in the industry. Games like Starburst, Twin Spin, Space Wars 2, Koi Princess, and Dead or Alive 2 come with their own unique features and thrilling gameplay. These free spins not only extend your playtime but also give you the opportunity to explore different games and find your favorites without any additional cost.
Why Choose Our Platform?
Our platform stands out due to its user-friendly interface, secure transactions, and a wide variety of games. We prioritize your gaming experience by ensuring that all our offers are easy to access and beneficial to our players. Our bonuses come with minimal wagering requirements, making it easier for you to cash out your winnings. Moreover, the variety of games we offer ensures that there’s something for every type of player, from classic slot enthusiasts to those who enjoy more modern, feature-packed games.
Conclusion
Don’t miss out on these fantastic opportunities to enhance your gaming experience. Whether you’re looking to enjoy free spins, cashback, or bountiful deposit bonuses, we have something for everyone. Join us today, take advantage of these fantastic deals, and start your journey to big wins and endless fun. Happy gaming!
Understanding the Online Gambling Landscape in the Philippines
The world of online gambling has been rapidly evolving, with the Philippines emerging as a dynamic hub for players seeking thrilling gaming experiences. As the industry continues to grow, it’s essential to have a comprehensive understanding of the landscape and the key factors that can elevate your online gambling journey.
The Rise of Betvisa Login in the Philippines
The Philippine online gambling market has witnessed a surge in popularity, with platforms like Betvisa Login leading the charge. These well-established and licensed entities offer a secure and trustworthy environment for players to indulge in a diverse range of games, from sports betting to casino offerings. By prioritizing platforms with a strong track record and positive user feedback, players can rest assured that their gaming activities are protected and regulated.
Mastering the Intricacies of Games
Each game in the online gambling realm has its unique intricacies and strategies. Whether you’re exploring the thrilling world of Visa Bet or immersing yourself in the captivating Betvisa Casino, it’s crucial to take the time to learn the rules and nuances of the games you play. Familiarize yourself with the game mechanics, payouts, and winning strategies by practicing on free demo versions before wagering real money. This approach not only enhances your chances of success but also ensures a more enjoyable and informed gaming experience.
Prioritizing Responsible Gambling
In the pursuit of thrilling gaming adventures, it’s essential to maintain a balanced and responsible approach. Betvisa PH, as a leading platform in the Philippines, emphasizes the importance of responsible gambling. Establish clear limits on your time and budget to prevent overspending and ensure that your online gambling activities remain a source of entertainment rather than a burden. By striking the right balance, you can maximize the excitement and enjoyment of your gaming journey.
Staying Informed and Connected
The online gambling landscape is dynamic, with new games, promotions, and industry trends constantly emerging. To stay ahead of the curve, it’s advisable to stay updated on the latest developments. Subscribing to newsletters or following the social media accounts of platforms like Betvisa Login can keep you informed about the latest offerings, bonuses, and events. Additionally, joining online forums or chat rooms dedicated to the Philippine online gambling community can provide valuable insights and tips from fellow players, further enriching your overall experience.
Embracing the Future of Online Gambling
As the online gambling industry in the Philippines continues to evolve, players must adapt and embrace the changing landscape. By selecting reputable platforms, mastering game strategies, practicing responsible gambling, and staying informed, you can navigate the exciting world of online gambling with confidence and success. With Betvisa Login leading the charge, the future of online gambling in the Philippines is filled with thrilling opportunities waiting to be explored.
Betvisa Bet | Step into the Arena with Betvisa!
Spin to Win Daily at Betvisa PH! | Take a whirl and bag ₱8,888 in big rewards.
Valentine’s 143% Love Boost at Visa Bet! | Celebrate romance and rewards !
Deposit Bonus Magic! | Deposit 50 and get an 88 bonus instantly at Betvisa Casino.
#betvisa
Free Cash & More Spins! | Sign up betvisa login,grab 500 free cash plus 5 free spins.
Sign-Up Fortune | Join through betvisa app for a free ₹500 and fabulous ₹8,888.
https://www.betvisa-bet.com/tl
#visabet #betvisalogin #betvisacasino # betvisaph
Double Your Play at betvisa com! | Deposit 1,000 and get a whopping 2,000 free
100% Cock Fight Welcome at Visa Bet! | Plunge into the exciting world .Bet and win!
Jump into Betvisa for exciting games, stunning bonuses, and endless winnings!
https://rybalka-v-rossii.ru/ – сайт о рыбалке в России, способах ловли рыб, и выборе правильных снастей.
भारत में ऑनलाइन क्रिकेट सट्टेबाजी की बढ़ती लोकप्रियता: कारण और प्रभाव
भारत में इंटरनेट और स्मार्टफोन की बढ़ती पहुंच ने ऑनलाइन सट्टेबाजी को बड़े पैमाने पर लोकप्रिय बना दिया है। देश के कोने-कोने में इंटरनेट की उपलब्धता और किफायती डेटा प्लान्स ने लोगों को ऑनलाइन प्लेटफॉर्म्स पर क्रिकेट सट्टेबाजी में भाग लेने की सुविधा दी है।
साथ ही, सस्ते और प्रभावी स्मार्टफोन्स की उपलब्धता ने इसे और भी सरल बना दिया है। अब लोग अपने मोबाइल फोन के जरिए कहीं भी और कभी भी बेटवीसा जैसे ऑनलाइन कैसीनो और खेल प्लेटफॉर्मों पर सट्टेबाजी कर सकते हैं।
क्रिकेट लीग और टूर्नामेंट्स की बढ़ती संख्या ने भी सट्टेबाजी के अवसरों में वृद्धि की है। आईपीएल (Indian Premier League) ने भारतीय क्रिकेट को एक नया आयाम दिया है, और इसका ग्लैमर तथा वैश्विक अपील सट्टेबाजों के लिए अत्यधिक आकर्षक है।
इसके अतिरिक्त, बीबीएल (Big Bash League), सीपीएल (Caribbean Premier League), और पीएसएल (Pakistan Super League) जैसे अंतरराष्ट्रीय लीग्स ने भी भारतीय सट्टेबाजों को लुभाया है।
इन कारकों के साथ-साथ, बेटवीसा जैसे प्रमुख ऑनलाइन कैसीनो और खेल प्लेटफॉर्मों ने भी भारत में ऑनलाइन क्रिकेट सट्टेबाजी की बढ़ती लोकप्रियता में महत्वपूर्ण भूमिका निभाई है। बेटवीसा की बेहतरीन सुविधाएं और सुरक्षा उपाय उपयोगकर्ताओं को एक विश्वसनीय और आरामदायक गेमिंग अनुभव प्रदान करते हैं।
समग्र रूप से, इंटरनेट और स्मार्टफोन की बढ़ती पहुंच, क्रिकेट लीग/टूर्नामेंट्स की संख्या में वृद्धि, और प्रमुख ऑनलाइन प्लेटफॉर्मों की आगमन ने भारत में ऑनलाइन क्रिकेट सट्टेबाजी को बढ़ावा दिया है।
Betvisa Bet
Betvisa Bet | Catch the BPL Excitement with Betvisa!
Hunt for ₹10million! | Enter the BPL at Betvisa and chase a staggering Bounty.
Valentine’s Boost at Visa Bet! | Feel the rush of a 143% Love Mania Bonus .
predict BPL T20 outcomes | score big rewards through Betvisa login!
#betvisa
Betvisa bonus Win! | Leverage your 10 free spins to possibly win $8,888.
Share and Earn! | win ₹500 via the Betvisa app download!
https://www.betvisa-bet.com/hi
#visabet #betvisalogin #betvisaapp #betvisaIndia
Sign-Up Jackpot! | Register at Betvisa India and win ₹8,888.
Double your play! | with a ₹1,000 deposit and get ₹2,000 free at Betvisa online!
Download the Betvisa download today and don’t miss out on the action!
baclofen price
leebet casino официальный сайт lee bet
Viagra Pfizer sans ordonnance: Viagra generique en pharmacie – Prix du Viagra 100mg en France
promethazine shelter – promethazine lantern promethazine root
Наш сайт эротических рассказов https://shoptop.org/ поможет тебе отвлечься от повседневной суеты и погрузиться в мир страсти и эмоций. Богатая библиотека секс историй для взрослых пробудит твое воображение и позволит насладиться каждой строкой.
Thrilling Developments and Renowned Franchises in the Sphere of Digital Entertainment
In the fluid domain of interactive entertainment, there’s always something new and thrilling on the brink. From modifications enhancing cherished mainstays to forthcoming launches in legendary series, the interactive entertainment realm is prospering as before.
Let’s take a snapshot into the newest developments and some of the beloved games engrossing players worldwide.
Latest Developments
1. Cutting-Edge Enhancement for Skyrim Enhances Non-Player Character Visuals
A latest mod for Skyrim has grabbed the focus of fans. This enhancement adds detailed faces and hair physics for every (NPCs), enhancing the title’s aesthetics and depth.
2. Total War Games Title Placed in Star Wars Universe Under Development
Creative Assembly, known for their Total War series, is reportedly developing a upcoming game set in the Star Wars Universe galaxy. This captivating integration has gamers awaiting the tactical and compelling adventure that Total War Series releases are known for, at last located in a galaxy far, far away.
3. GTA VI Release Communicated for Fall 2025
Take-Two’s Chief Executive Officer has communicated that GTA VI is scheduled to launch in Late 2025. With the colossal reception of its prior release, Grand Theft Auto V, enthusiasts are awaiting to experience what the next installment of this celebrated brand will deliver.
4. Extension Plans for Skull and Bones Second Season
Studios of Skull and Bones have disclosed broader developments for the experience’s sophomore season. This nautical saga promises upcoming updates and enhancements, sustaining enthusiasts immersed and absorbed in the realm of maritime nautical adventures.
5. Phoenix Labs Studio Faces Workforce Reductions
Disappointingly, not everything news is good. Phoenix Labs Studio, the creator developing Dauntless, has revealed large-scale personnel cuts. Despite this challenge, the game continues to be a renowned preference across players, and the studio stays focused on its fanbase.
Popular Releases
1. The Witcher 3: Wild Hunt
With its captivating plot, engrossing realm, and captivating journey, The Witcher 3: Wild Hunt remains a cherished release across players. Its rich plot and wide-ranging sandbox persist to draw enthusiasts in.
2. Cyberpunk 2077
Notwithstanding a rocky release, Cyberpunk continues to be a eagerly awaited game. With persistent enhancements and adjustments, the experience keeps evolve, providing players a perspective into a dystopian world teeming with mystery.
3. GTA 5
Despite time following its initial debut, Grand Theft Auto 5 remains a renowned preference across players. Its expansive sandbox, captivating narrative, and shared components sustain enthusiasts reengaging for more experiences.
4. Portal 2 Game
A iconic problem-solving release, Portal 2 is renowned for its groundbreaking gameplay mechanics and brilliant environmental design. Its challenging obstacles and amusing storytelling have solidified it as a exceptional title in the videogame industry.
5. Far Cry
Far Cry 3 is hailed as a standout entries in the universe, presenting fans an open-world experience filled with excitement. Its compelling narrative and legendary personalities have cemented its position as a cherished release.
6. Dishonored Game
Dishonored is hailed for its sneaky gameplay and exceptional environment. Gamers take on the persona of a otherworldly executioner, navigating a city filled with political mystery.
7. Assassin’s Creed Game
As a component of the acclaimed Assassin’s Creed Universe collection, Assassin’s Creed Game is beloved for its compelling narrative, captivating mechanics, and historical settings. It keeps a noteworthy title in the universe and a iconic within players.
In closing, the realm of gaming is prospering and ever-changing, with groundbreaking advan
tretinoin cream retin a
amoxicillin 250mg cost
частный выкуп авто выкуп авто оценка
выкуп авто москва быстро выкуп авто без взноса
where can i buy acyclovir pills
how to get advair cheap
baclofen over the counter usa
pharmacie en ligne pas cher: Cialis sans ordonnance 24h – Pharmacie sans ordonnance
video games guide
Thrilling Developments and Iconic Titles in the Realm of Gaming
In the fluid domain of digital entertainment, there’s constantly something innovative and thrilling on the forefront. From modifications enhancing iconic classics to forthcoming debuts in celebrated series, the gaming ecosystem is as vibrant as in current times.
We’ll take a overview into the latest developments and some of the most popular titles captivating fans internationally.
Most Recent News
1. Groundbreaking Enhancement for Skyrim Elevates Non-Player Character Look
A newly-released customization for Skyrim has grabbed the attention of fans. This customization introduces realistic heads and dynamic hair for every supporting characters, elevating the world’s visual appeal and depth.
2. Total War Release Placed in Star Wars Galaxy World in Development
The Creative Assembly, renowned for their Total War Games lineup, is reportedly crafting a new game located in the Star Wars Setting galaxy. This exciting integration has players anticipating with excitement the tactical and captivating experience that Total War Series releases are acclaimed for, at last situated in a world far, far away.
3. GTA VI Launch Announced for Late 2025
Take-Two Interactive’s CEO’s Leader has announced that Grand Theft Auto VI is expected to arrive in Q4 2025. With the colossal reception of its previous installment, Grand Theft Auto V, players are excited to explore what the upcoming installment of this iconic universe will bring.
4. Growth Initiatives for Skull & Bones Second Season
Creators of Skull and Bones have communicated amplified strategies for the game’s Season Two. This high-seas journey promises additional features and improvements, sustaining players captivated and absorbed in the realm of high-seas nautical adventures.
5. Phoenix Labs Developer Faces Workforce Reductions
Sadly, not all news is uplifting. Phoenix Labs Developer, the studio behind Dauntless Game, has disclosed massive personnel cuts. Notwithstanding this challenge, the experience continues to be a renowned preference among gamers, and the team stays dedicated to its community.
Iconic Experiences
1. The Witcher 3: Wild Hunt Game
With its compelling experience, absorbing domain, and captivating journey, The Witcher 3: Wild Hunt keeps a cherished experience within enthusiasts. Its expansive experience and vast open world continue to engage fans in.
2. Cyberpunk 2077 Game
Regardless of a rocky arrival, Cyberpunk stays a much-anticipated experience. With constant improvements and fixes, the experience continues to advance, offering gamers a perspective into a high-tech future rife with intrigue.
3. Grand Theft Auto 5
Even time after its original debut, GTA V keeps a iconic option among players. Its sprawling nonlinear world, engaging plot, and co-op components keep players returning for further journeys.
4. Portal 2
A classic analytical release, Portal Game is acclaimed for its groundbreaking mechanics and ingenious level design. Its challenging challenges and clever narrative have cemented it as a exceptional experience in the interactive entertainment industry.
5. Far Cry 3 Game
Far Cry is hailed as a standout installments in the universe, providing players an nonlinear exploration filled with excitement. Its immersive plot and legendary characters have solidified its status as a iconic title.
6. Dishonored Series
Dishonored is hailed for its sneaky mechanics and unique realm. Players adopt the identity of a extraordinary assassin, exploring a urban environment teeming with governmental intrigue.
7. Assassin’s Creed 2
As a segment of the acclaimed Assassin’s Creed series, Assassin’s Creed II is beloved for its immersive story, engaging features, and historical worlds. It remains a remarkable game in the franchise and a iconic among fans.
In summary, the universe of gaming is prospering and dynamic, with groundbreaking developments
স্বাগত বোনাস প্রথম আমানত 200% পান – একটি অসাধারণ সুযোগ
আপনার জন্য একটি অসাধারণ সুযোগ! এই সময়ে, আমরা নতুন সদস্যদের জন্য বিশেষ প্রচার অফার এনেছি – স্বাগত বোনাসে প্রথম আমানতের 200% পান! এই অফারটি পেতে আপনার প্রথম আমানতটি করতে হবে এবং পরে আপনি এই অফারের উপভোগ করতে পারবেন।
খেলার ধরন:
এই সুযোগের আওতায় আমরা আপনাকে স্লট, ফিশার, বিঙ্গো, মেগা বল এবং মানি হুইলে খেলার সুবিধা দিচ্ছি। আপনি যেকোনো খেলায় অংশ নিতে পারেন এবং আপনার আগ্রহ অনুযায়ী খেলাটি চয়ন করতে পারেন।
অফারের বিবরণ:
আপনি ১০০ বিডিটি ডিপোজিট করলে আপনি ২০০% বোনাস পাবেন, অর্থাৎ ৩০০ বিডিটি।
আপনাকে এই বোনাস উত্তোলন করতে হবে x20 বার, অর্থাৎ আপনাকে মোট ৬০০০ বিডিটির জন্য খেলতে হবে।
সর্বোচ্চ উত্তোলন ৩৫০ বিডিটি।
আবেদনের মাত্রা:
এই অফার এপ্রিলের পরে নিবন্ধন করা গ্রাহকদের জন্য প্রযোজ্য।
এই অফারটি সীমিত সময়ের জন্য মাত্র, সুতরাং তা অবিলম্বে পেতে আজই আমাদের সাথে যোগাযোগ করুন। ক্রিকেট অ্যাফিলিয়েট হিসেবে আমাদের প্ল্যাটফর্মে যোগ দিন এবং এই অসাধারণ সুযোগ উপভোগ করুন!
Welcome to Cricket Affiliate | Kick off with a smashing Welcome Bonus !
First Deposit Fiesta! | Make your debut at Cricket Exchange with a 200% bonus.
Daily Doubles! | Keep the scoreboard ticking with a 100% daily bonus at 9wicket!
#cricketaffiliate
IPL 2024 Jackpot! | Stand to win ₹50,000 in the mega IPL draw at cricket world!
Social Sharer Rewards! | Post and earn 100 tk weekly through Crickex affiliate login.
https://www.cricket-affiliate.com/
#cricketexchange #9wicket #crickexaffiliatelogin #crickexlogin
crickex login VIP! | Step up as a VIP and enjoy weekly bonuses!
Join the Action! | Log in through crickex bet exciting betting experience at Live Affiliate.
Dive into the game with crickex live—where every play brings spectacular wins !
https://formomebel.ru/stoliki/na-osnovanii-iz-metalla
https://formomebel.ru/stoliki/metallicheskie
mikrosluchatko https://mikrocz.cz/
nanosluchatka mikrosluchatko
generic propecia available in us
where to purchase zithromax
provigil 200 mg
купить микронаушники https://jasdam.cz/
크립토 골드
이때 왕서인은 천천히 눈을 들어 문제를 제기한 사람을 보았다.
toradol pill cost
acheter mГ©dicament en ligne sans ordonnance: kamagra livraison 24h – Achat mГ©dicament en ligne fiable
buy vermox online
buy amoxil online
Viagra homme prix en pharmacie sans ordonnance: Viagra homme sans prescription – Viagra pas cher paris
video games guide
Captivating Developments and Iconic Releases in the Sphere of Gaming
In the ever-evolving landscape of interactive entertainment, there’s always something fresh and engaging on the cusp. From mods improving beloved staples to forthcoming launches in celebrated universes, the digital entertainment landscape is prospering as ever.
We’ll take a look into the up-to-date updates and a few of the most popular games enthralling audiences across the globe.
Latest Announcements
1. Innovative Customization for The Elder Scrolls V: Skyrim Optimizes NPC Visuals
A latest mod for The Elder Scrolls V: Skyrim has captured the focus of players. This modification introduces lifelike heads and dynamic hair for every supporting characters, optimizing the title’s graphics and engagement.
2. Total War Game Set in Star Wars Galaxy Being Developed
The Creative Assembly, famous for their Total War series, is reportedly working on a new game located in the Star Wars world. This exciting crossover has fans anticipating with excitement the profound and immersive adventure that Total War Series experiences are acclaimed for, now placed in a world distant.
3. Grand Theft Auto VI Arrival Announced for Fall 2025
Take-Two’s Head has revealed that GTA VI is expected to arrive in Fall 2025. With the overwhelming reception of its previous installment, Grand Theft Auto V, enthusiasts are awaiting to see what the upcoming entry of this iconic series will deliver.
4. Extension Strategies for Skull & Bones Second Season
Designers of Skull & Bones have communicated broader plans for the title’s next season. This swashbuckling saga delivers additional content and updates, sustaining players immersed and absorbed in the domain of oceanic nautical adventures.
5. Phoenix Labs Studio Faces Workforce Reductions
Disappointingly, not every news is positive. Phoenix Labs Studio, the developer developing Dauntless Experience, has communicated massive layoffs. In spite of this setback, the game keeps to be a renowned choice amidst fans, and the company continues to be committed to its playerbase.
Renowned Experiences
1. Wild Hunt
With its engaging plot, immersive realm, and captivating journey, The Witcher 3: Wild Hunt remains a beloved release across players. Its rich experience and vast free-roaming environment persist to draw players in.
2. Cyberpunk
Despite a tumultuous release, Cyberpunk Game keeps a highly anticipated game. With persistent updates and adjustments, the experience keeps advance, providing players a view into a futuristic setting teeming with intrigue.
3. GTA V
Yet years following its first debut, Grand Theft Auto 5 stays a iconic preference amidst fans. Its expansive open world, compelling experience, and multiplayer features keep players revisiting for ongoing journeys.
4. Portal Game
A classic brain-teasing title, Portal 2 is renowned for its groundbreaking features and ingenious spatial design. Its intricate conundrums and amusing storytelling have made it a remarkable experience in the videogame landscape.
5. Far Cry 3 Game
Far Cry 3 is celebrated as exceptional entries in the franchise, delivering fans an nonlinear adventure rife with intrigue. Its immersive story and memorable entities have solidified its standing as a fan favorite release.
6. Dishonored Universe
Dishonored Game is celebrated for its sneaky gameplay and distinctive setting. Gamers embrace the role of a otherworldly executioner, traversing a metropolis rife with governmental danger.
7. Assassin’s Creed 2
As a component of the iconic Assassin’s Creed Series collection, Assassin’s Creed Game is cherished for its compelling experience, compelling systems, and era-based settings. It stays a noteworthy experience in the universe and a cherished amidst fans.
In conclusion, the world of gaming is flourishing and constantly evolving, with groundbreaking developments
biaxin barnacle – clarithromycin september cytotec pills sink
https://rybalka-v-rossii.ru – сайт о рыбалке в России, способах ловли рыб, и выборе правильных снастей.к
ভারতের একটি জনপ্রিয় কাৰ্যকলাপ হলো ক্রিকেট। এই ক্রিকেটের অংশ হিসাবে, ক্রিকেক্স (CrickEx) একটি জনপ্রিয় প্ল্যাটফর্ম যা ক্রিকেটের বিভিন্ন কৌশল ও বিষয়বস্তু নিয়ে কাজ করে। ক্রিকেক্স-এর একটি বিশেষ প্রচার ছিল যা প্রতি এপ্রিল মাসে ঘোষণা করা হয়।
এই প্রচারে, ক্রিকেটের প্রিয়দর্শী ভক্তরা বিনামূল্যে ক্রিকেক্স তালিকায় নিবন্ধিত হয়ে 200 বাজি পেতে পারেন। যেসকল ব্যবহারকারী এপ্রিল মাসের পর নিবন্ধিত হবেন, তারাই এই প্রচারে অংশ নিতে পারবেন।
ব্যবহারকারীদের এই প্রচারটিতে অংশ নিতে হলে তাদের প্রথমে “মেম্বার সেন্টার” -এ যেতে হবে এবং তারপর “অ্যাপ্লাই প্রমোশন” বিকল্পটি ক্লিক করতে হবে। এরপর তাদেরকে নিজের পছন্দের প্রমোশন টি চয়ন করতে হবে।
প্রচারটি বন্ধ করার জন্য, ব্যবহারকারীদের প্রথমে “মেম্বার সেন্টার” -এ যেতে হবে, তারপর “প্রমোশন লিস্ট” অপশনে যেতে হবে এবং “স্টপ প্রমোশন” বিকল্পটি ক্লিক করতে হবে।
একজন ব্যবহারকারী শুধুমাত্র একবার এই বিনামূল্য বাজি প্রচারে অংশ নিতে পারেন। এই প্রচারের নিয়ম অনুযায়ী, একটি অ্যাকাউন্ট, আইপি, ফোন নম্বর, ইমেল এবং ব্যাঙ্ক অ্যাকাউন্টের মাধ্যমে শুধুমাত্র একবার এই প্রচারটি ব্যবহার করা যাবে। বাউন্সিংবল8 সংস্থা এই প্রচারটি সংশোধন, স্থগিত বা বন্ধ করার অধিকার সংরক্ষণ করে।
এই প্রচারটি ক্রিকেটে আগ্রহী ভক্তদের মধ্যে জনপ্রিয় হয়ে উঠেছে। এটি ক্রিকেটের প্রতি ভক্তিকে প্রকাশ করার এবং ক্রিকেক্স (CrickEx) প্ল্যাটফর্মে অংশ নেওয়ার একটি উপায়।
Welcome to Cricket Affiliate | Kick off with a smashing Welcome Bonus !
First Deposit Fiesta! | Make your debut at Cricket Exchange with a 200% bonus.
Daily Doubles! | Keep the scoreboard ticking with a 100% daily bonus at 9wicket!
#cricketaffiliate
IPL 2024 Jackpot! | Stand to win ₹50,000 in the mega IPL draw at cricket world!
Social Sharer Rewards! | Post and earn 100 tk weekly through Crickex affiliate login.
https://www.cricket-affiliate.com/
#cricketexchange #9wicket #crickexaffiliatelogin #crickexlogin
crickex login VIP! | Step up as a VIP and enjoy weekly bonuses!
Join the Action! | Log in through crickex bet exciting betting experience at Live Affiliate.
Dive into the game with crickex live—where every play brings spectacular wins !
biaxin pills face – clarithromycin pills principal cytotec observe
leebet либет казино
lee bet casino lee bet регистрация
retin a coupon discount
azithromycin cost india
флешки оптом https://meflash.ru/
купить флешки оптом https://meflash.ru/
fludrocortisone glory – esomeprazole pills surround lansoprazole own
SildГ©nafil 100mg pharmacie en ligne: Viagra generique en pharmacie – Viagra gГ©nГ©rique sans ordonnance en pharmacie
Thrilling Breakthroughs and Beloved Games in the Domain of Interactive Entertainment
In the ever-evolving realm of videogames, there’s always something fresh and thrilling on the forefront. From enhancements optimizing iconic staples to new arrivals in celebrated universes, the digital entertainment ecosystem is as vibrant as ever.
Here’s a snapshot into the most recent updates and specific the most popular games engrossing enthusiasts worldwide.
Up-to-Date Updates
1. New Modification for Skyrim Enhances Non-Player Character Aesthetics
A recent enhancement for Skyrim has captured the interest of fans. This enhancement adds high-polygon faces and hair physics for all supporting characters, elevating the experience’s aesthetics and depth.
2. Total War Games Experience Located in Star Wars World Being Developed
The Creative Assembly, acclaimed for their Total War Games franchise, is supposedly crafting a upcoming release placed in the Star Wars Universe realm. This exciting collaboration has gamers looking forward to the profound and compelling journey that Total War Games experiences are known for, ultimately placed in a galaxy remote.
3. Grand Theft Auto VI Arrival Confirmed for Fall 2025
Take-Two Interactive’s CEO’s Head has confirmed that Grand Theft Auto VI is expected to arrive in Q4 2025. With the overwhelming acclaim of its earlier title, Grand Theft Auto V, players are excited to experience what the upcoming iteration of this celebrated brand will provide.
4. Extension Developments for Skull & Bones 2nd Season
Developers of Skull & Bones have announced enhanced plans for the world’s next season. This high-seas journey provides additional features and enhancements, sustaining fans immersed and immersed in the universe of oceanic seafaring.
5. Phoenix Labs Developer Experiences Layoffs
Disappointingly, not every updates is uplifting. Phoenix Labs, the team in charge of Dauntless Game, has communicated massive workforce reductions. Notwithstanding this obstacle, the release remains to be a iconic selection within fans, and the company continues to be focused on its playerbase.
Beloved Games
1. Wild Hunt
With its immersive narrative, engrossing universe, and enthralling adventure, The Witcher 3 Game stays a cherished release among gamers. Its deep experience and wide-ranging sandbox remain to attract enthusiasts in.
2. Cyberpunk
In spite of a problematic launch, Cyberpunk 2077 Game stays a eagerly awaited title. With constant improvements and adjustments, the game maintains progress, offering players a view into a cyberpunk future abundant with peril.
3. GTA V
Despite time following its debut release, Grand Theft Auto V keeps a iconic selection across fans. Its wide-ranging nonlinear world, engaging narrative, and online mode keep enthusiasts reengaging for further experiences.
4. Portal 2 Game
A legendary analytical game, Portal 2 is acclaimed for its pioneering features and ingenious environmental design. Its complex conundrums and witty dialogue have solidified it as a standout game in the interactive entertainment industry.
5. Far Cry
Far Cry 3 is hailed as a standout titles in the universe, presenting gamers an nonlinear adventure filled with adventure. Its engrossing experience and renowned figures have solidified its status as a beloved release.
6. Dishonored
Dishonored Game is celebrated for its stealthy systems and one-of-a-kind environment. Enthusiasts assume the role of a mystical eliminator, traversing a metropolis abundant with political danger.
7. Assassin’s Creed Game
As part of the renowned Assassin’s Creed Series series, Assassin’s Creed II is revered for its immersive narrative, engaging features, and historical environments. It stays a exceptional experience in the franchise and a iconic within gamers.
In final remarks, the universe of digital entertainment is flourishing and fluid, with groundbreaking advan
purchase advair
tadacip 20mg
advair diskus 250 mg
supermoney88
clomid prescription canada
sunmory33
order lasix 40 mg
SildГ©nafil Teva 100 mg acheter: Viagra sans ordonnance 24h – Prix du Viagra en pharmacie en France
ANGKOT88: Situs Game Deposit Pulsa Terbaik di Indonesia
ANGKOT88 adalah situs game deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai jenis game online terlengkap yang dapat Anda mainkan hanya dengan mendaftar satu ID. Dengan satu ID tersebut, Anda dapat mengakses seluruh permainan yang tersedia di situs kami.
Sebagai situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), ANGKOT88 menjamin keamanan dan kenyamanan Anda. Situs kami didukung oleh server hosting yang cepat dan sistem keamanan dengan metode enkripsi terbaru di dunia, sehingga data Anda akan selalu terjaga keamanannya. Tampilan situs yang modern juga membuat Anda merasa nyaman saat mengakses situs kami.
Keunggulan ANGKOT88
Selain menjadi situs game online terbaik, ANGKOT88 juga menawarkan layanan praktis untuk melakukan deposit menggunakan pulsa XL ataupun Telkomsel dengan potongan terendah dibandingkan situs lainnya. Ini menjadikan kami salah satu situs game online pulsa terbesar di Indonesia. Anda juga dapat melakukan deposit pulsa melalui E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kepercayaan dan Layanan
Kami di ANGKOT88 sangat menjaga kepercayaan Anda sebagai prioritas utama kami. Oleh karena itu, kami selalu berusaha menjadi agen online terpercaya dan terbaik sepanjang masa. Permainan game online yang kami tawarkan sangat praktis, sehingga Anda dapat memainkannya kapan saja dan di mana saja tanpa perlu repot bepergian. Kami menyediakan berbagai jenis game, termasuk yang disiarkan secara LIVE (langsung) dengan host cantik dan kamera yang merekam secara real-time, menjadikan ANGKOT88 situs game online terlengkap dan terbesar di Indonesia.
Promo Menarik dan Menguntungkan
ANGKOT88 juga menawarkan banyak sekali promo menarik dan menguntungkan. Anda bisa menikmati berbagai macam promo yang sesuai dengan kebutuhan Anda, seperti welcome bonus 20%, bonus deposit harian, dan cashback. Semua promo ini tersedia di situs ANGKOT88. Selain itu, kami juga memiliki layanan Customer Service yang siap membantu Anda kapan saja.
Jadi, tunggu apa lagi? Bergabunglah dengan ANGKOT88 dan nikmati pengalaman bermain game online terbaik dan teraman di Indonesia. Daftarkan diri Anda sekarang dan mulai mainkan game favorit Anda dengan nyaman dan aman di situs kami!
doxycycline 150 mg price
https://proauto.kyiv.ua здесь вы найдете обзоры и тест-драйвы автомобилей, свежие новости автопрома, обширный автокаталог с характеристиками и ценами, полезные советы по уходу и ремонту, а также активное сообщество автолюбителей. Присоединяйтесь к нам и оставайтесь в курсе всех событий в мире автомобилей!
Are you looking for reliable and fast proxies? https://fineproxy.org/account/aff.php?aff=29 It offers a wide range of proxy servers with excellent speed and reliability. Perfect for surfing, scraping and more. Start right now with this link: FineProxy.org . Excellent customer service and a variety of tariff plans!
pharmacie en ligne france livraison belgique: achat kamagra – pharmacie en ligne avec ordonnance
furosemide 40 mg tablet cost
noroxin drug
Betvisa Casino: Unlocking Unparalleled Bonuses for Philippine Gamblers
The world of online gambling has witnessed a remarkable surge in popularity, and Betvisa Casino has emerged as a premier destination for players in the Philippines. With its user-friendly platform and a diverse selection of games, Betvisa Casino has become the go-to choice for both seasoned gamblers and newcomers alike.
One of the standout features of Betvisa Casino is its generous bonus offerings, which can significantly enhance the overall gaming experience for players in the Philippines. These bonuses not only provide additional value but also increase the chances of winning big.
For first-time players, Betvisa Casino offers a tempting welcome bonus that can give a substantial boost to their initial bankroll. This bonus allows players to explore the platform’s vast array of games, from thrilling slot titles to immersive live casino experiences, with the added security of a financial cushion.
Existing players, on the other hand, can take advantage of a range of ongoing promotions and bonuses that cater to their specific gaming preferences. These may include reload bonuses, free spins, and even exclusive VIP programs that offer personalized rewards and privileges.
One of the key advantages of Betvisa Casino’s bonus offerings is their versatility. Players can utilize these bonuses across a variety of games, from the Visa Bet sports betting platform to the captivating Betvisa Casino. This flexibility allows players to diversify their gaming portfolios and experience the full breadth of what Betvisa has to offer.
Moreover, Betvisa Casino’s bonus terms and conditions are transparent and player-friendly, ensuring a seamless and enjoyable gaming experience. Whether you’re looking to maximize your winnings or simply enhance your overall enjoyment, these bonuses can provide the extra edge you need.
As the online gambling landscape in the Philippines continues to evolve, Betvisa Casino remains at the forefront, offering an unparalleled combination of games, user-friendliness, and unbeatable bonuses. So, why not take a step into the world of Betvisa Casino and unlock a world of exciting possibilities?
Betvisa Bet | Step into the Arena with Betvisa!
Spin to Win Daily at Betvisa PH! | Take a whirl and bag ?8,888 in big rewards.
Valentine’s 143% Love Boost at Visa Bet! | Celebrate romance and rewards !
Deposit Bonus Magic! | Deposit 50 and get an 88 bonus instantly at Betvisa Casino.
#betvisa
Free Cash & More Spins! | Sign up betvisa login,grab 500 free cash plus 5 free spins.
Sign-Up Fortune | Join through betvisa app for a free ?500 and fabulous ?8,888.
https://www.betvisa-bet.com/tl
#visabet #betvisalogin #betvisacasino # betvisaph
Double Your Play at betvisa com! | Deposit 1,000 and get a whopping 2,000 free
100% Cock Fight Welcome at Visa Bet! | Plunge into the exciting world .Bet and win!
Jump into Betvisa for exciting games, stunning bonuses, and endless winnings!
prednisone 8 pills
https://autoblog.kyiv.ua путеводитель в мире автомобилей. Обзоры и тест-драйвы, актуальные новости, автокаталог, советы по уходу и ремонту, а также общение с автолюбителями. Всё, что нужно для выбора и эксплуатации авто, вы найдете у нас.
https://autoclub.kyiv.ua узнайте все о новых моделях, читайте обзоры и тест-драйвы, получайте советы по уходу за авто и ремонтам. Наш автокаталог и активное сообщество автолюбителей помогут вам быть в курсе последних тенденций.
Achat mГ©dicament en ligne fiable: kamagra gel – pharmacie en ligne france pas cher
angkot88
ANGKOT88: Situs Game Deposit Pulsa Terbaik di Indonesia
ANGKOT88 adalah situs game deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai jenis game online terlengkap yang dapat Anda mainkan hanya dengan mendaftar satu ID. Dengan satu ID tersebut, Anda dapat mengakses seluruh permainan yang tersedia di situs kami.
Sebagai situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), ANGKOT88 menjamin keamanan dan kenyamanan Anda. Situs kami didukung oleh server hosting yang cepat dan sistem keamanan dengan metode enkripsi terbaru di dunia, sehingga data Anda akan selalu terjaga keamanannya. Tampilan situs yang modern juga membuat Anda merasa nyaman saat mengakses situs kami.
Keunggulan ANGKOT88
Selain menjadi situs game online terbaik, ANGKOT88 juga menawarkan layanan praktis untuk melakukan deposit menggunakan pulsa XL ataupun Telkomsel dengan potongan terendah dibandingkan situs lainnya. Ini menjadikan kami salah satu situs game online pulsa terbesar di Indonesia. Anda juga dapat melakukan deposit pulsa melalui E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kepercayaan dan Layanan
Kami di ANGKOT88 sangat menjaga kepercayaan Anda sebagai prioritas utama kami. Oleh karena itu, kami selalu berusaha menjadi agen online terpercaya dan terbaik sepanjang masa. Permainan game online yang kami tawarkan sangat praktis, sehingga Anda dapat memainkannya kapan saja dan di mana saja tanpa perlu repot bepergian. Kami menyediakan berbagai jenis game, termasuk yang disiarkan secara LIVE (langsung) dengan host cantik dan kamera yang merekam secara real-time, menjadikan ANGKOT88 situs game online terlengkap dan terbesar di Indonesia.
Promo Menarik dan Menguntungkan
ANGKOT88 juga menawarkan banyak sekali promo menarik dan menguntungkan. Anda bisa menikmati berbagai macam promo yang sesuai dengan kebutuhan Anda, seperti welcome bonus 20%, bonus deposit harian, dan cashback. Semua promo ini tersedia di situs ANGKOT88. Selain itu, kami juga memiliki layanan Customer Service yang siap membantu Anda kapan saja.
Jadi, tunggu apa lagi? Bergabunglah dengan ANGKOT88 dan nikmati pengalaman bermain game online terbaik dan teraman di Indonesia. Daftarkan diri Anda sekarang dan mulai mainkan game favorit Anda dengan nyaman dan aman di situs kami!
https://sunmory33jitu.com
buy tadalafil 20mg price
provigil cost
аренда юридических адресов от собственника
supermoney88
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
https://levitraenligne.com/# Pharmacie sans ordonnance
https://ktm.org.ua/ у нас вы найдете свежие новости, аналитические статьи, эксклюзивные интервью и мнения экспертов. Будьте в курсе событий и тенденций, следите за развитием ситуации в реальном времени. Присоединяйтесь к нашему сообществу читателей!
https://mostmedia.com.ua мы источник актуальных новостей, аналитики и мнений. Получайте самую свежую информацию, читайте эксклюзивные интервью и экспертные статьи. Оставайтесь в курсе мировых событий и тенденций вместе с нами. Присоединяйтесь к нашему информационному сообществу!
럭키 네코
그럼에도 불구하고 이 Qianhu는 여전히 창백하고 쇠약했습니다.
1600 mg bactrim
strattera sale
average cost of clomid
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
pharmacie en ligne france pas cher: Acheter Cialis 20 mg pas cher – pharmacies en ligne certifiГ©es
sunmory33
sunmory33
PRO88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
PRO88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di PRO88.
Keunggulan PRO88
PRO88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Berbagai Macam Game Online
Kami menyediakan berbagai macam game online terbaik yang bisa Anda mainkan kapan saja dan di mana saja. Dengan satu ID, Anda bisa menikmati semua permainan yang tersedia, mulai dari permainan kartu, slot, hingga taruhan olahraga. PRO88 memastikan semua game yang kami sediakan adalah yang terbaik dan terlengkap di Indonesia.
Keamanan dan Kenyamanan
Kami memahami betapa pentingnya keamanan dan kenyamanan bagi para pemain. Oleh karena itu, PRO88 menggunakan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia. Ini memastikan bahwa data pribadi dan transaksi Anda selalu aman bersama kami. Tampilan situs yang modern juga dirancang untuk memberikan pengalaman bermain yang nyaman dan menyenangkan.
Kesimpulan
PRO88 adalah pilihan terbaik untuk Anda yang mencari situs game online deposit pulsa yang aman dan terpercaya. Dengan berbagai macam game online terbaik dan terlengkap, serta dukungan keamanan yang canggih, PRO88 siap memberikan pengalaman bermain game yang tak terlupakan. Daftar sekarang juga di PRO88 dan nikmati semua permainan yang tersedia hanya dengan satu ID.
Kunjungi kami di PRO88 dan mulailah petualangan game online Anda bersama kami!
Founded in Texas in 2002, https://southeast.newschannelnebraska.com/story/50826769/del-mar-energy-from-humble-beginnings-to-an-energy-market-leader quickly transformed into one of the leading players in the energy market, oil and gas extraction, road construction
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
generic cialis 2018
lasix 40 mg price
how to buy accutane online
azithromycin buy online no prescription
BetVisa: মোবাইল গেমিংয়ের নতুন রূপ
ডিজিটাল যুগে, খেলোয়াড়রা আর ডেস্কটপ গেমিংয়ের সীমিততা সহ্য করতে চান না। তাদের চাহিদা হল, যেকোন সময় যেকোন জায়গায় তাদের প্রিয় স্লট গেমগুলি খেলতে পারা। এই চাহিদা লক্ষ্য করে, BetVisa মোবাইল গেমিংয়ের নতুন মাত্রা উন্মোচন করেছে।
বেটভিসা ডাউনলোড: খেলোয়াড়রা বাড়িতে বসে থাক বা চলার পথে থাকুক না কেন, তাদের স্মার্টফোন বা ট্যাবলেট বের করে BetVisa অ্যাপ চালু করতে পারে এবং সেকেন্ডের মধ্যে স্লটের জগতে ডুব দিতে পারে। এই সুবিধার মাধ্যমে, খেলোয়াড়রা ডেস্কটপ গেমিংয়ের সীমাবদ্ধতা থেকে বিদায় নিতে পারেন।
রিচ গেমিং বৈচিত্র্য: Betvisa তাদের সৃজনশীলতা এবং উদ্ভাবনের জন্য বিখ্যাত গেম ডেভেলপারদের কাছ থেকে শিরোনাম সমন্বিত স্লট গেমগুলির একটি বিস্তৃত লাইব্রেরি নিয়ে গর্বিত। ক্লাসিক ফ্রুট মেশিন থেকে শুরু করে অত্যাধুনিক গ্রাফিক্স এবং অ্যানিমেশন গর্বিত নিমজ্জিত ভিডিও স্লট পর্যন্ত, প্রত্যেক খেলোয়াড়ের পছন্দ ও স্বাদ মেটাতে কিছু না কিছু রয়েছে।
সুচারু গেমপ্লে: বেটিভিসা ডাউনলোড মোবাইল ডিভাইসের জন্য তৈরি অপ্টিমাইজড পারফরম্যান্স এবং স্বজ্ঞাত নিয়ন্ত্রণ সহ একটি নিরবচ্ছিন্ন গেমিং অভিজ্ঞতা নিশ্চিত করে৷ প্লেয়াররা অ্যাপের মাধ্যমে অনায়াসে নেভিগেট করতে পারে, বিভিন্ন গেম অন্বেষণ করতে পারে, এবং কোনো প্রকার ল্যাগ বা গ্লিচ ছাড়াই নিরবচ্ছিন্ন গেমপ্লে উপভোগ করতে পারে।
বিশেষ প্রচার সুযোগ: BetVisa প্রায়শই Betvisa ডাউনলোড অ্যাপের মাধ্যমে প্ল্যাটফর্মে প্রবেশকারী খেলোয়াড়দের জন্য একচেটিয়া প্রচার এবং বোনাস রোল আউট করে। স্বাগত বোনাস থেকে শুরু করে ফ্রি স্পিন এবং লয়্যালটি পুরষ্কার পর্যন্ত, একজনের ব্যাঙ্করোল বাড়ানো এবং গেমিং অভিজ্ঞতা বাড়ানোর প্রচুর সুযোগ রয়েছে।
BetVisa বাংলাদেশ ব্যবহারকারীদের জন্য বিশেষ সুবিধা প্রদান করে। BetVisa বাংলাদেশ লগইন করে খেলোয়াড়রা সহজে তাদের প্রিয় স্লট গেমগুলি খেলতে পারেন।
মোবাইল ডিভাইসের উন্নত অ্যাক্সেসের সুযোগ, রিচ গেমিং বৈচিত্র্য এবং বিশেষ প্রচার সুবিধার মাধ্যমে, BetVisa মোবাইল গেমিংয়ের নতুন বিস্ময় সৃষ্টি করেছে।
Betvisa Bet | Hit it Big This IPL Season with Betvisa!
Betvisa login! | Every deposit during IPL matches earns a 2% bonus .
Betvisa Bangladesh! | IPL 2024 action heats up, your bets get more rewarding!
Crash Game returns! | huge ₹10 million jackpot. Take the lead on the Betvisa app !
#betvisa
Start Winning Now! | Sign up through Betvisa affiliate login, claim ₹500 free cash.
Grab Your Winning Ticket! | Register login and win ₹8,888 at visa bet!
https://www.betvisa-bet.com/bn
#visabet #betvisalogin #betvisabangladesh#betvisaapp
200% Excitement! | Enjoy slots and fishing games at Betvisa লগইন করুন!
Big Sports Bonuses! | Score up to ₹5,000 in sports bonuses during the IPL season
Gear up for an exhilarating IPL season at Betvisa, propels you towards victory!
how to buy modafinil online uk
Viagra pas cher livraison rapide france: Acheter du Viagra sans ordonnance – Meilleur Viagra sans ordonnance 24h
В сети интернет огромное мера анализаторов сайтика, качество опуса которых напрямую молит через тарифных планов.
https://be1.ru/ – лысый
sapporo88
SUPERMONEY88: Situs Game Online Deposit Pulsa Terbaik di Indonesia
SUPERMONEY88 adalah situs game online deposit pulsa terbaik tahun 2020 di Indonesia. Kami menyediakan berbagai macam game online terbaik dan terlengkap yang bisa Anda mainkan di situs game online kami. Hanya dengan mendaftar satu ID, Anda bisa memainkan seluruh permainan yang tersedia di SUPERMONEY88.
Keunggulan SUPERMONEY88
SUPERMONEY88 juga merupakan situs agen game online berlisensi resmi dari PAGCOR (Philippine Amusement Gaming Corporation), yang berarti situs ini sangat aman. Kami didukung dengan server hosting yang cepat dan sistem keamanan dengan metode enkripsi termutakhir di dunia untuk menjaga keamanan database Anda. Selain itu, tampilan situs kami yang sangat modern membuat Anda nyaman mengakses situs kami.
Layanan Praktis dan Terpercaya
Selain menjadi game online terbaik, ada alasan mengapa situs SUPERMONEY88 ini sangat spesial. Kami memberikan layanan praktis untuk melakukan deposit yaitu dengan melakukan deposit pulsa XL ataupun Telkomsel dengan potongan terendah dari situs game online lainnya. Ini membuat situs kami menjadi salah satu situs game online pulsa terbesar di Indonesia. Anda bisa melakukan deposit pulsa menggunakan E-commerce resmi seperti OVO, Gopay, Dana, atau melalui minimarket seperti Indomaret dan Alfamart.
Kami juga terkenal sebagai agen game online terpercaya. Kepercayaan Anda adalah prioritas kami, dan itulah yang membuat kami menjadi agen game online terbaik sepanjang masa.
Kemudahan Bermain Game Online
Permainan game online di SUPERMONEY88 memudahkan Anda untuk memainkannya dari mana saja dan kapan saja. Anda tidak perlu repot bepergian lagi, karena SUPERMONEY88 menyediakan beragam jenis game online. Kami juga memiliki jenis game online yang dipandu oleh host cantik, sehingga Anda tidak akan merasa bosan.
cheap lasix 40 mg
pharmacie en ligne france pas cher: pharmacie en ligne france pas cher – Pharmacie Internationale en ligne
юр адрес москва купить для ооо недорого
amoxil 875
buy azithromycin online usa
buy doxycycline capsules
сео консультация
Советы по сео продвижению.
Информация о том как взаимодействовать с низкочастотными запросами ключевыми словами и как их выбирать
Тактика по деятельности в конкурентной нише.
Обладаю постоянных клиентов взаимодействую с тремя фирмами, есть что рассказать.
Изучите мой аккаунт, на 31 мая 2024г
общий объём выполненных работ 2181 только в этом профиле.
Консультация только в устной форме, никаких скриншотов и отчётов.
Длительность консультации указано 2 часа, но по сути всегда на доступен без строгой привязки к графику.
Как работать с ПО это уже другая история, консультация по работе с программами обсуждаем отдельно в другом разделе, выясняем что требуется при разговоре.
Всё без суеты на без напряжения не спеша
To get started, the seller needs:
Мне нужны контакты от телеграм каналов для связи.
общение только устно, переписываться недостаточно времени.
Суббота и Вс выходной
https://kursovyemetrologiya.ru
online modafinil pharmacy
buy 1 retin a cream
lasix 40 mg daily
https://formomebel.ru/krovati
acyclovir 400 mg daily
pharmacie en ligne sans ordonnance: Acheter Cialis – pharmacie en ligne france livraison internationale
doxycycline 100 mg buy online
выкуп авто выгодно https://vykup-avtomsk.ru
florinef remember – omeprazole pills emerge prevacid pills reluctant
diflucan 50 mg price
секс шоп каталог https://24sex-shop.ru/
интим товары секс шопа https://24sex-shop.ru/
sunmory33
sunmory33
order zithromax online
интернет секс шоп https://24sex-shop.ru/
lyrica price comparison
купить реальную секс куклу https://24sexy-dolls.ru
купить силиконовую секс куклу https://24sexy-dolls.ru
https://fraza.kyiv.ua/ вы найдете последние новости, глубокие аналитические материалы, интервью с влиятельными личностями и экспертные мнения. Следите за важными событиями и трендами в реальном времени. Присоединяйтесь к нашему сообществу и будьте информированы!
как продвинуть сайт
Советы по SEO продвижению.
Информация о том как взаимодействовать с низкочастотными запросами и как их определять
Подход по действиям в соперничающей нише.
У меня есть регулярных взаимодействую с 3 фирмами, есть что поделиться.
Посмотрите мой профиль, на 31 мая 2024г
число выполненных работ 2181 только в этом профиле.
Консультация только в устной форме, никаких скринов и документов.
Продолжительность консультации указано 2 часа, но по реально всегда на связи без жёсткой привязки к графику.
Как взаимодействовать с софтом это уже другая история, консультация по работе с софтом договариваемся отдельно в другом кворке, выясняем что нужно при коммуникации.
Всё без суеты на расслабленно не торопясь
To get started, the seller needs:
Мне нужны данные от телеграм канала для связи.
коммуникация только вербально, переписываться недостаточно времени.
Суббота и воскресенья нерабочие дни
pharmacie en ligne france pas cher: kamagra 100mg prix – Pharmacie sans ordonnance
purchase azithromycin 1g
flomax medicine price
cipro drug
bocor88
купить секс куклу в интернет магазине https://24sexy-dolls.ru
https://7krasotok.com здесь вы найдете статьи о моде, красоте, здоровье, отношениях и карьере. Читайте советы экспертов, участвуйте в обсуждениях и вдохновляйтесь новыми идеями. Присоединяйтесь к нашему сообществу женщин, стремящихся к совершенству!
https://bestwoman.kyiv.ua узнайте всё о моде, красоте, здоровье и личностном росте. Читайте вдохновляющие истории, экспертные советы и актуальные новости. Присоединяйтесь к нашему сообществу женщин, живущих яркой и насыщенной жизнью!
canada generic strattera
문 프린세스 100
“행복 그룹.” Hongzhi 황제는 약간 눈살을 찌푸 렸습니다. 그 이름은 매우 드물고 이상했습니다.
Viagra pas cher paris: viagra sans ordonnance – Viagra prix pharmacie paris
Viagra femme sans ordonnance 24h: Acheter viagra en ligne livraison 24h – Viagra homme prix en pharmacie
diflucan online cheap without a prescription
https://prowoman.kyiv.ua на нашем сайте вы найдете полезные советы по моде, красоте, здоровью и отношениям. Читайте вдохновляющие статьи, участвуйте в обсуждениях и обменивайтесь идеями. Присоединяйтесь к нашему сообществу современных женщин!
azithromycin 500mg tablets for sale
https://superwoman.kyiv.ua вы на нашем надежном гиде в мире женской красоты и стиля жизни! У нас вы найдете актуальные статьи о моде, красоте, здоровье, а также советы по саморазвитию и карьерному росту. Присоединяйтесь к нам и обретайте новые знания и вдохновение каждый день!
buy live tiktok views Buy TikTok Live Views
bocor88
bocor88
how to buy tiktok live views Buy TikTok Live Views
pharmacie en ligne avec ordonnance: acheter kamagra site fiable – Pharmacie Internationale en ligne
how to buy views on tiktok live Buy TikTok Live Views
секс куклы купить 18 https://24sexy-dolls.ru
решения задач на заказ https://resheniezadachmatematika.ru/
Pharmacie en ligne livraison Europe: Levitra 20mg prix en pharmacie – pharmacie en ligne sans ordonnance
курсовые на заказ https://kursovyematematika.ru
Viagra sans ordonnance 24h: viagra en ligne – SildГ©nafil 100 mg sans ordonnance
vermox 500mg tablet price
娛樂城
線上娛樂城的世界
隨著互聯網的快速發展,網上娛樂城(網上賭場)已經成為許多人休閒的新選擇。網上娛樂城不僅提供多樣化的游戲選擇,還能讓玩家在家中就能體驗到賭場的刺激和快感。本文將探討網上娛樂城的特色、利益以及一些常見的的遊戲。
什麼線上娛樂城?
在線娛樂城是一種透過互聯網提供博彩遊戲的平台。玩家可以透過計算機、智慧型手機或平板設備進入這些網站,參與各種賭錢活動,如撲克、賭盤、黑傑克和老虎机等。這些平台通常由專業的的程序公司開發,確保游戲的公平性和安全性。
線上娛樂城的優勢
便利性:玩家不用離開家,就能體驗博彩的樂趣。這對於那些居住在偏遠實體賭場地區的人來說尤為方便。
多種的遊戲選擇:在線娛樂城通常提供比實體賭場更多樣化的遊戲選擇,並且經常更新遊戲內容,保持新穎。
優惠和獎勵計劃:許多網上娛樂城提供豐厚的獎金計劃,包括註冊獎金、存款獎勵和忠誠計劃,吸引新新玩家並促使老玩家繼續遊戲。
安全和保密性:正規的網上娛樂城使用先進的加密方法來保護玩家的個人信息和交易,確保遊戲過程的安全和公平。
常見的線上娛樂城遊戲
德州撲克:德州撲克是最流行賭錢遊戲之一。在線娛樂城提供各種撲克變體,如德州撲克、奧馬哈和七張牌等。
賭盤:賭盤是一種傳統的賭場遊戲遊戲,玩家可以賭注在數字、數字組合或顏色選擇上,然後看球落在哪個位置。
黑傑克:又稱為二十一點,這是一種競爭玩家和莊家點數點數的遊戲,目標是讓手牌點數點數盡可能接近21點但不超過。
老虎機:老虎机是最容易也是最常見的博彩遊戲之一,玩家只需旋轉捲軸,看圖案排列出中獎的組合。
結論
網上娛樂城為現代的賭博愛好者提供了一個方便、刺激且豐富的娛樂選擇。不管是撲克牌愛好者還是老虎机愛好者,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的的不斷發展,網上娛樂城的遊戲體驗將變得越來越越來越真實和吸引人。然而,玩家在享用游戲的同時,也應該保持自律,避免沉迷於賭錢活動,維持健康的心態。
娛樂城
在線娛樂城的天地
隨著網際網路的飛速發展,網上娛樂城(線上賭場)已經成為許多人休閒的新選擇。網上娛樂城不僅提供多種的游戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和樂趣。本文將研究網上娛樂城的特徵、利益以及一些常見的的游戲。
什麼是線上娛樂城?
在線娛樂城是一種經由互聯網提供賭錢遊戲的平台。玩家可以通過電腦設備、手機或平板設備進入這些網站,參與各種博彩活動,如撲克牌、賭盤、二十一點和老虎機等。這些平台通常由專家的程序公司開發,確保遊戲的公平性和穩定性。
在線娛樂城的優勢
方便性:玩家不用離開家,就能體驗賭博的興奮。這對於那些生活在偏遠實體賭場地方的人來說尤為方便。
多樣化的游戲選擇:線上娛樂城通常提供比實體賭場更多的遊戲選擇,並且經常更新遊戲內容,保持新鮮。
優惠和獎勵計劃:許多在線娛樂城提供豐富的獎金計劃,包括註冊獎勵、存款獎勵和忠誠計劃,吸引新玩家並促使老玩家不斷遊戲。
安全和隱私:合法的在線娛樂城使用先進的加密來保護玩家的個人資料和財務交易,確保游戲過程的公平和公正性。
常見的的在線娛樂城游戲
撲克:撲克是最受歡迎賭錢游戲之一。線上娛樂城提供多種德州撲克變體,如德州扑克、奧馬哈撲克和七張撲克等。
賭盤:輪盤是一種經典的賭博遊戲,玩家可以投注在數字、數字組合上或顏色上,然後看球落在哪個區域。
二十一點:又稱為21點,這是一種競爭玩家和莊家點數的遊戲,目標是讓手牌點數儘量接近21點但不超過。
老虎机:吃角子老虎是最容易且是最常見的賭博游戲之一,玩家只需轉動捲軸,等待圖案圖案排列出中獎的組合。
結尾
網上娛樂城為當代賭博愛好者提供了一個便捷、興奮且多樣化的娛樂選擇。不管是撲克愛好者還是老虎機迷,大家都能在這些平台上找到適合自己的遊戲。同時,隨著技術的的不斷提升,網上娛樂城的遊戲體驗將變得越來越越來越真實和引人入勝。然而,玩家在享受遊戲的同時,也應該保持,避免沉迷於賭錢活動,保持健康的娛樂心態。
заказать курсовую онлайн https://kursovyebankovskoe.ru/
Сайт https://zhenskiy.kyiv.ua – це онлайн-ресурс, який присвячений жіночим темам та інтересам. Тут зібрана інформація про моду, красу, здоров’я, відносини, кулінарію та багато іншого, що може бути корисним та цікавим для сучасних жінок.
Доставка цветов в Саратове https://flowers64.ru/ это отличная возможность заказать различные цветы, букеты, композиции, подарки, не выходя из дома.
신속한 환충 서비스와 더불어 주요업체의 안전성
베팅사이트 접속 시 매우 중요한 요소 중 하나는 빠른 입출금 프로세스입니다. 일반적으로 세 분 이내에 입금, 십 분 이내에 환전이 처리되어야 합니다. 메이저 메이저업체들은 필요한 직원 채용으로 이 같은 신속한 입출금 처리를 보장하며, 이를 통해 회원들에게 안도감을 드립니다. 주요사이트를 접속하면서 스피드 있는 경험을 해보세요. 저희는 여러분들이 안심하고 사이트를 이용할 수 있도록 도와드리는 먹튀 해결 팀입니다.
보증금을 걸고 광고 배너 운영
먹튀해결사는 최소 삼천만 원부터 1억 원의 보증금을 예탁한 업체들의 광고 배너를 운영합니다. 만일 먹튀 사고가 발생할 경우, 배팅 룰에 어긋나지 않은 배팅 기록을 캡처하여 먹튀해결사에 문의 주시면, 사실 확인 뒤 보증금으로 신속하게 손해 보상을 처리해드립니다. 피해 발생 시 신속하게 캡처하여 피해 상황을 저장해 두시고 보내주시기 바랍니다.
장기 운영 안전업체 확인
먹튀해결사는 적어도 4년 이상 먹튀 문제 없이 안정적으로 운영하고 있는 사이트만을 검증하여 배너 등록을 허가합니다. 이를 통해 누구나 알만한 대형사이트를 안심하고 접속할 수 있는 기회를 제공합니다. 엄격한 검증 절차를 통해 검증된 사이트를 놓치지 마시고, 보안된 배팅을 경험해보세요.
투명하고 공정한 먹튀 검토
먹튀 해결 팀의 먹튀 검증은 투명함과 공평성을 근거로 실시합니다. 늘 고객들의 의견을 최우선으로 생각하며, 기업의 회유나 이득에 흔들리지 않으며 한 건의 삭제 없이 진실만을 기반으로 검증해왔습니다. 먹튀 사고를 당하고 후회하지 않도록, 바로 지금 시작해보세요.
먹튀검증사이트 목록
먹튀 해결 전문가가 엄선한 안전한 베팅사이트 검증업체 목록 입니다. 지금 등록된 검증업체들은 먹튀 문제가 발생 시 100% 보장을 도와드립니다. 하지만, 제휴 기간이 끝난 업체에서 발생한 사고에 대해서는 책임이 없습니다.
독보적인 먹튀 검증 알고리즘
먹튀 해결 팀은 깨끗한 베팅 환경을 만들기 위해 늘 애쓰고 있습니다. 저희가 권장하는 스포츠토토사이트에서 안전하게 배팅하세요. 고객님의 먹튀 신고 내용은 먹튀 리스트에 등록 노출되어 그 해당 토토사이트에 치명적인 영향을 끼칩니다. 먹튀 리스트 작성 시 먹튀블러드 만의 검증 지식을 최대한 활용하여 공평한 심사를 할 수 있게 하겠습니다.
안전한 도박 환경을 조성하기 위해 항상 애쓰는 먹튀 해결 전문가와 함께 안심하고 즐겨보세요.
pharmacie en ligne france livraison belgique: Cialis sans ordonnance 24h – vente de mГ©dicament en ligne
pharmacies en ligne certifiГ©es: achat kamagra – pharmacie en ligne fiable
buy vermox over the counter uk
在線娛樂城的世界
隨著互聯網的迅速發展,在線娛樂城(線上賭場)已經成為許多人娛樂的新選擇。線上娛樂城不僅提供多元化的遊戲選擇,還能讓玩家在家中就能體驗到賭場的刺激和樂趣。本文將討論線上娛樂城的特點、好處以及一些常見的遊戲。
什麼網上娛樂城?
線上娛樂城是一種通過互聯網提供博彩游戲的平台。玩家可以通過計算機、智慧型手機或平板設備進入這些網站,參與各種賭錢活動,如撲克、輪盤、黑傑克和吃角子老虎等。這些平台通常由專業的程序公司開發,確保游戲的公平性和安全性。
網上娛樂城的好處
便利性:玩家不需要離開家,就能享受博彩的樂趣。這對於那些住在在遠離實體賭場地區的人來說尤其方便。
多種的遊戲選擇:在線娛樂城通常提供比實體賭場更多的游戲選擇,並且經常升級遊戲內容,保持新穎。
優惠和獎勵計劃:許多在線娛樂城提供豐厚的獎勵計劃,包括註冊獎金、存款紅利和忠誠計劃,吸引新新玩家並促使老玩家繼續遊戲。
安全和保密性:合法的在線娛樂城使用高端的加密方法來保護玩家的私人信息和財務交易,確保遊戲過程的安全和公正。
常有的在線娛樂城游戲
撲克牌:撲克是最流行博彩游戲之一。線上娛樂城提供各種德州撲克變體,如德州撲克、奧馬哈撲克和七張撲克等。
賭盤:輪盤賭是一種經典的賭博遊戲,玩家可以投注在單個數字、數字組合或顏色上,然後看小球落在哪個區域。
21點:又稱為二十一點,這是一種對比玩家和莊家點數的游戲,目標是讓手牌點數盡量接近21點但不超過。
老虎机:老虎机是最受歡迎並且是最流行的博彩游戲之一,玩家只需轉捲軸,等待圖案圖案排列出中獎的組合。
結尾
線上娛樂城為現代賭博愛好者提供了一個方便的、興奮且豐富的娛樂方式。不管是撲克愛好者還是吃角子老虎迷,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的的不斷提升,線上娛樂城的游戲體驗將變得越來越現實和吸引人。然而,玩家在享用遊戲的同時,也應該保持,避免過度沉迷於博彩活動,保持健康的遊戲心態。
在線娛樂城的天地
隨著網際網路的飛速發展,在線娛樂城(線上賭場)已經成為許多人消遣的新選擇。線上娛樂城不僅提供多種的遊戲選擇,還能讓玩家在家中就能體驗到賭場的樂趣和快感。本文將討論網上娛樂城的特色、利益以及一些常見的的遊戲。
什麼叫網上娛樂城?
在線娛樂城是一種經由互聯網提供賭博游戲的平台。玩家可以透過電腦、手機或平板進入這些網站,參與各種賭博活動,如德州撲克、輪盤賭、21點和老虎机等。這些平台通常由專家的程序公司開發,確保游戲的公正和穩定性。
在線娛樂城的利益
便利:玩家不用離開家,就能體驗賭錢的興奮。這對於那些住在在偏遠實體賭場地方的人來說尤其方便。
多元化的遊戲選擇:網上娛樂城通常提供比實體賭場更豐富的游戲選擇,並且經常改進游戲內容,保持新鮮。
優惠和獎勵計劃:許多線上娛樂城提供豐厚的優惠計劃,包括註冊紅利、存款紅利和會員計劃,吸引新新玩家並鼓勵老玩家持續遊戲。
安全和保密性:正規的線上娛樂城使用先進的的加密技術來保護玩家的個人信息和財務交易,確保遊戲過程的穩定和公正性。
常見的網上娛樂城遊戲
撲克牌:撲克牌是最流行賭博游戲之一。線上娛樂城提供多樣德州撲克變體,如德州撲克、奧馬哈撲克和七張牌撲克等。
輪盤賭:輪盤是一種古老的賭場遊戲,玩家可以投注在數字、數字排列或顏色上上,然後看轉球落在哪個位置。
二十一點:又稱為二十一點,這是一種對比玩家和莊家點數點數的遊戲,目標是讓手牌點數點數儘量接近21點但不超過。
老虎機:老虎機是最容易並且是最受歡迎的賭錢遊戲之一,玩家只需轉動捲軸,等待圖案圖案排列出贏得的組合。
結論
在線娛樂城為現代的賭博愛好者提供了一個便捷、興奮且多樣化的娛樂方式。不管是撲克牌愛好者還是吃角子老虎迷,大家都能在這些平台上找到適合自己的游戲。同時,隨著技術的的不斷提升,在線娛樂城的遊戲體驗將變得越來越越來越真實和引人入勝。然而,玩家在體驗游戲的同時,也應該保持自律,避免沉溺於博彩活動,保持健康健康的遊戲心態。
Советы по SEO продвижению.
Информация о том как управлять с низкочастотными ключевыми словами и как их выбирать
Тактика по действиям в соперничающей нише.
Обладаю постоянных сотрудничаю с 3 фирмами, есть что рассказать.
Изучите мой аккаунт, на 31 мая 2024г
число успешных проектов 2181 только здесь.
Консультация проходит устно, никаких скриншотов и отчетов.
Время консультации указано 2 часа, но по реально всегда на доступен без строгой привязки к графику.
Как управлять с ПО это уже отдельная история, консультация по работе с программами обсуждаем отдельно в специальном услуге, выясняем что необходимо при коммуникации.
Всё без суеты на без напряжения не торопясь
To get started, the seller needs:
Мне нужны сведения от Telegram чата для коммуникации.
общение только в устной форме, вести переписку нету времени.
Суббота и Вс нерабочие дни
Консультация по сео стратегии продвижению.
Информация о том как работать с низкочастотными запросами и как их определять
Стратегия по деятельности в соперничающей нише.
У меня есть регулярных сотрудничаю с 3 компаниями, есть что поделиться.
Посмотрите мой аккаунт, на 31 мая 2024г
количество выполненных работ 2181 только в этом профиле.
Консультация проходит устно, без снимков с экрана и отчетов.
Продолжительность консультации указано 2 ч, и факту всегда на контакте без твердой привязки к графику.
Как взаимодействовать с ПО это уже отдельная история, консультация по работе с программами обсуждаем отдельно в другом услуге, выясняем что нужно при общении.
Всё без суеты на расслабленно не торопясь
To get started, the seller needs:
Мне нужны контакты от телеграм канала для коммуникации.
разговор только устно, переписываться нету времени.
субботы и воскресенья выходной
заказать курсовую работу https://kupit-kursovuyu-rabotu.ru/ с гарантией и антиплагиатом
order acyclovir
빠릿한 입출금 서비스와 주요업체의 안전성
베팅사이트 접속 시 핵심적인 요소는 빠릿한 환충 처리입니다. 대개 세 분 안에 충전하고, 열 분 이내에 환충이 처리되어야 합니다. 대형 메이저업체들은 넉넉한 인력 고용을 통해 이 같은 빠른 환충 절차를 보증하며, 이를 통해 회원들에게 안전감을 드립니다. 주요사이트를 사용하면서 신속한 체감을 해보세요. 우리는 여러분이 안심하고 웹사이트를 이용할 수 있도록 돕는 먹튀해결 전문가입니다.
보증금을 내고 배너를 운영
먹튀해결사는 최대한 3000만 원에서 일억 원의 보증 자금을 예치한 사이트들의 배너 광고를 운영합니다. 혹시 먹튀 문제가 생길 경우, 배팅 룰에 반하지 않은 배팅 내역을 캡처해서 먹튀 해결 팀에 문의하시면, 확인 후 보증금으로 즉시 피해 보상을 처리합니다. 피해가 생기면 신속하게 캡처하여 피해 상황을 기록해두시고 제출해 주세요.
장기 운영 안전업체 확인
먹튀 해결 팀은 최소 4년간 먹튀 이력 없이 안정적으로 운영한 사이트들을 인증하여 배너 등록을 허용합니다. 이를 통해 어느 누구나 알고 있는 메이저사이트를 안심하고 사용할 수 있는 기회를 제공합니다. 엄격한 검사 작업을 통해 인증된 사이트를 놓치지 마시고, 안전한 배팅을 체험해보세요.
투명하고 공정한 먹튀 검토
먹튀해결사의 먹튀 검증은 투명함과 공정을 근거로 실시합니다. 늘 사용자들의 입장을 최우선으로 생각하며, 업체의 유혹이나 이득에 흔들리지 않으며 하나의 삭제 없이 사실만을 기반으로 검토해왔습니다. 먹튀 문제를 겪고 후회하지 않도록, 지금 바로 시작해보세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 골라낸 안전 토토사이트 인증된 업체 목록 입니다. 현재 등록된 인증된 업체들은 먹튀 사고 발생 시 100% 보증을 해드립니다. 그러나, 제휴 기간이 끝난 업체에서 발생한 사고에 대해서는 책임을 지지 않습니다.
유일무이한 먹튀 검증 알고리즘
먹튀해결사는 깨끗한 베팅 문화를 만들기 위해 계속해서 노력하고 있습니다. 저희는 추천하는 스포츠토토사이트에서 안전하게 베팅하시기 바랍니다. 사용자의 먹튀 신고 내용은 먹튀 리스트에 기재되어 해당 베팅 사이트에 중대한 영향을 줄 수 있습니다. 먹튀 목록 작성 시 먹튀블러드 만의 검토 경험을 충분히 활용하여 공정한 심사를 할 수 있게 하겠습니다.
안전한 베팅 문화를 제공하기 위해 끊임없이 애쓰는 먹튀해결사와 함께 안전하게 즐기시기 바랍니다.
Добро пожаловать на наш ресурс о недвижимости!
Здесь вы найдете актуальные статьи и новости о рынке недвижимости, правовых аспектах продажи жилья, аренде жилых помещений, инвестициях в недвижимость и многом другом.
Мы стремимся поделиться с вами полезной информацией и помочь вам принимать осознанные решения в сфере покупки недвижимости.
Больше интересной информации о строительстве и ремонте можно прочитать на сайте https://stroyka-gid.ru. Только самые популярные статьи и обзоры процесса ремонта помещений и строительства зданий.
lioresal
Больше интересной информации о строительстве и ремонте можно прочитать на сайте https://stroyka-gid.ru. Только самые популярные статьи и обзоры процесса ремонта помещений и строительства зданий.
modafinil india pharmacy
методы продвижения сайта
Советы по оптимизации продвижению.
Информация о том как взаимодействовать с низкочастотными ключевыми словами и как их определять
Тактика по действиям в конкурентной нише.
Обладаю постоянных клиентов работаю с 3 компаниями, есть что рассказать.
Изучите мой аккаунт, на 31 мая 2024г
число завершённых задач 2181 только в этом профиле.
Консультация только устно, без скриншотов и отчетов.
Продолжительность консультации указано 2 ч, но по сути всегда на контакте без твердой привязки ко времени.
Как взаимодействовать с программным обеспечением это уже другая история, консультация по работе с софтом обсуждаем отдельно в отдельном услуге, определяем что необходимо при общении.
Всё спокойно на расслабленно не торопясь
To get started, the seller needs:
Мне нужны сведения от телеграм канала для коммуникации.
общение только устно, переписываться не хватает времени.
Сб и воскресенья выходные
Откройте двери в мир недвижимости с нашим ресурсом!
Получайте экспертные статьи от специалистов в области недвижимости. Узнавайте о налогах на недвижимость, осуществляйте успешные сделки купли-продажи квартир, и всегда оставайтесь в курсе последних тенденций рынка.
http://ufficioporta.ru
best smm panel https://promospanel.com
spotify plays smm panel cheap smm panel
5 래빗스 메가웨이즈
“이 문제는 듣기 쉽습니다.” Li Zheng은 Suleiman이 이것에 관심이 있음을보고 그의 얼굴이 붉어졌습니다.
best paypal smm panel paypal smm panel
jnetoto
Inspirasi dari Kutipan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Taylor Swift, seorang musisi dan penulis lagu terkenal, tidak hanya diakui karena melodi yang indah dan nyanyian yang nyaring, tetapi juga oleh karena kata-kata karyanya yang penuh makna. Dalam lirik-liriknya, Swift sering menggambarkan berbagai unsur kehidupan, berawal dari cinta sampai dengan tantangan hidup. Berikut adalah sejumlah petikan inspiratif dari lagu-lagunya, beserta maknanya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Makna: Bahkan di masa-masa sulit, selalu ada sedikit harapan dan peluang akan masa depan yang lebih baik.
Lirik ini dari lagu “All Too Well” mengingatkan kita kalau biarpun kita barangkali mengalami masa-masa sulit pada saat ini, tetap ada peluang bahwa waktu yang akan datang akan memberikan hal yang lebih baik. Hal ini adalah pesan harapan yang mengukuhkan, mendorong kita untuk tetap bertahan dan tidak menyerah, karena yang terbaik mungkin belum datang.
“Aku akan bertahan karena aku tak bisa mengerjakan apapun tanpamu.” – “You Belong with Me”
Penjelasan: Menemukan asmara dan dukungan dari orang lain dapat memberi kita kekuatan dan kemauan keras untuk terus berjuang melalui rintangan.
best music promotion services https://banger-music.com
miototo
Ashley JKT48: Bintang yang Bersinar Gemilang di Langit Idol
Siapakah Ashley JKT48?
Siapakah sosok muda berbakat yang menyita perhatian banyak penggemar musik di Indonesia dan Asia Tenggara? Itulah Ashley Courtney Shintia, atau yang terkenal dengan pseudonimnya, Ashley JKT48. Masuk dengan grup idola JKT48 pada masa 2018, Ashley dengan segera berubah menjadi salah satu anggota paling populer.
Profil
Terlahir di Jakarta pada tanggal 13 Maret 2000, Ashley berketurunan darah Tionghoa-Indonesia. Beliau memulai karier di dunia hiburan sebagai peraga dan pemeran, hingga akhirnya kemudian menjadi anggota dengan JKT48. Personanya yang ceria, vokal yang mantap, dan keterampilan menari yang mengesankan membentuknya sebagai idola yang sangat dicintai.
Award dan Pengakuan
Popularitas Ashley telah dikenal melalui banyak penghargaan dan pencalonan. Pada tahun 2021, ia memenangkan pengakuan “Member Terpopuler JKT48” di ajang JKT48 Music Awards. Ashley juga dianugerahi sebagai “Idol Tercantik di Asia” oleh sebuah media online pada tahun 2020.
Peran dalam JKT48
Ashley memainkan peran krusial dalam grup JKT48. Ia adalah anggota Tim KIII dan berperan sebagai penari utama dan vokalis. Ashley juga merupakan bagian dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Perjalanan Mandiri
Selain kegiatan dengan JKT48, Ashley juga mengembangkan perjalanan mandiri. Ia telah mengeluarkan beberapa single, diantaranya “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi bersama penyanyi lain, seperti Afgan dan Rossa.
Hidup Pribadi
Di luar kancah pertunjukan, Ashley dikenal sebagai pribadi yang rendah hati dan ramah. Ashley menikmati menghabiskan waktu dengan sanak famili dan teman-temannya. Ashley juga memiliki kesukaan melukis dan memotret.
get votes for online contest how to buy instagram followers with paypal
get soundcloud plays https://promobanger.com/
music marketing agencies https://banger-music.com
Проверка счета USDT
Верификация токенов на сети TRC20 и различных блокчейн платежей
На представленном веб-сайте вы найдете подробные ревью многочисленных инструментов для анализа операций и аккаунтов, содержащие антиотмывочного закона верификации для токенов и других блокчейн-активов. Вот ключевые особенности, которые в наших ревью:
Верификация криптовалюты TRC20
Известные ресурсы обеспечивают всестороннюю проверку платежей USDT на платформе TRC20 блокчейна. Это дает возможность фиксировать необычную действия и удовлетворять регуляторным стандартам.
Контроль переводов USDT
В подробных ревью указаны ресурсы для всестороннего проверки и наблюдения платежей монет, что гарантирует гарантировать ясность и надежность переводов.
антиотмывочная анализ токенов
Определенные инструменты поддерживают антиотмывочную проверку монет, обеспечивая выявлять и предотвращать случаи незаконных операций и финансовых незаконных действий.
Верификация счета токенов
Наши оценки содержат сервисы, которые позволяют контролировать кошельки USDT на выявление блокировок и подозрительных платежей, предоставляя дополнительный уровень уровень защищенности.
Контроль переводов криптовалюты TRC20
Вы описаны ресурсы, предоставляющие проверку переводов токенов в блокчейн-сети TRC20 сети, что позволяет поддерживает соблюдение всем стандартам правилам.
Проверка адреса счета монет
В обзорах доступны инструменты для верификации адресов адресов токенов на предмет опасностей рисков.
Контроль аккаунта USDT на сети TRC20
Наши ревью включают сервисы, предлагающие анализ счетов монет в блокчейн-сети TRC20 платформы, что предотвращает гарантирует предотвратить мошенничества и экономических мошенничеств.
Анализ монет на легитимность
Представленные инструменты предусматривают контролировать переводы и аккаунты на легитимность, фиксируя сомнительную активность.
anti-money laundering контроль USDT на блокчейне TRC20
В описаниях представлены платформы, обеспечивающие AML верификацию для криптовалюты в сети TRC20 блокчейна, обеспечивая вашему делу выполнять глобальным положениям.
Анализ криптовалюты ERC20
Наши ревью охватывают ресурсы, поддерживающие контроль монет в сети ERC20 платформы, что гарантирует обеспечивает детальный анализ переводов и кошельков.
Проверка цифрового кошелька
Мы описываем сервисы, предлагающие услуги по верификации криптокошельков, охватывая наблюдение переводов и определение подозреваемой деятельности.
Проверка счета виртуального кошелька
Наши оценки охватывают платформы, дающие возможность проверять счета виртуальных кошельков для повышения повышенной защиты.
Анализ криптокошелька на операции
Вы найдете ресурсы для контроля криптовалютных кошельков на переводы, что обеспечивает обеспечивает сохранять открытость переводов.
Проверка цифрового кошелька на легитимность
Наши обзоры включают решения, дающие возможность контролировать цифровые кошельки на прозрачность, выявляя возможные подозреваемые платежи.
Ознакомившись с наши описания, вы сможете подходящие ресурсы для проверки и наблюдения виртуальных переводов, чтобы поддерживать поддерживать дополнительный степень защиты и выполнять всех законодательным стандартам.
bisacodyl pills – buy liv52 without prescription purchase liv52 generic
get votes for online contest https://promobanger.com/
congtogel
Inspirasi dari Ucapan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Penyanyi Terkenal, seorang penyanyi dan pengarang lagu terkemuka, tidak hanya dikenal oleh karena melodi yang indah dan suara yang merdu, tetapi juga oleh karena lirik-lirik lagunya yang bermakna. Pada lirik-liriknya, Swift sering menggambarkan berbagai aspek kehidupan, mulai dari asmara sampai rintangan hidup. Berikut ini adalah beberapa petikan menginspirasi dari lagu-lagunya, bersama artinya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Penjelasan: Bahkan di saat-saat sulit, selalu ada seberkas harapan dan kemungkinan akan masa depan yang lebih baik.
Lirik ini dari lagu “All Too Well” menyadarkan kita bahwa meskipun kita barangkali menghadapi masa-masa sulit saat ini, tetap ada potensi kalau hari esok akan membawa perubahan yang lebih baik. Hal ini adalah pesan asa yang menguatkan, mendorong kita untuk bertahan dan tidak mengalah, lantaran yang terbaik bisa jadi belum tiba.
“Aku akan terus bertahan lantaran aku tak mampu melakukan apapun tanpa kamu.” – “You Belong with Me”
Penjelasan: Menemukan kasih dan bantuan dari orang lain dapat memberi kita kekuatan dan kemauan keras untuk bertahan melalui kesulitan.
Online Gambling Sites: Innovation and Advantages for Modern Community
Introduction
Online casinos are virtual platforms that offer players the chance to engage in betting activities such as card games, spin games, blackjack, and slots. Over the past few decades, they have become an essential part of online entertainment, providing numerous benefits and opportunities for players around the world.
Availability and Convenience
One of the main benefits of digital casinos is their availability. Players can enjoy their favorite activities from anywhere in the globe using a computer, iPad, or mobile device. This conserves time and funds that would otherwise be used going to traditional casinos. Additionally, round-the-clock availability to games makes online casinos a easy choice for people with hectic lifestyles.
Range of Activities and Entertainment
Online casinos provide a vast variety of games, allowing all users to discover something they enjoy. From classic card activities and table games to slot machines with diverse themes and increasing jackpots, the diversity of activities ensures there is an option for every preference. The option to engage at various skill levels also makes digital gambling sites an perfect location for both novices and seasoned gamblers.
Economic Benefits
The online casino sector contributes greatly to the economy by generating employment and generating revenue. It supports a diverse range of professions, including software developers, client assistance agents, and marketing professionals. The income generated by online gambling sites also contributes to tax revenues, which can be used to support public services and development projects.
Advancements in Technology
Digital casinos are at the forefront of technological innovation, constantly integrating new innovations to improve the gaming entertainment. High-quality visuals, live dealer games, and virtual reality (VR) gambling sites offer immersive and realistic gaming experiences. These innovations not only improve user satisfaction but also push the limits of what is achievable in online leisure.
Responsible Gambling and Assistance
Many digital casinos encourage responsible gambling by providing resources and resources to assist players manage their betting habits. Options such as deposit limits, self-exclusion choices, and access to assistance programs guarantee that players can engage in gaming in a safe and monitored environment. These measures show the sector’s dedication to promoting safe gaming habits.
Community Engagement and Networking
Online casinos often provide interactive options that allow players to connect with each other, creating a sense of belonging. Multiplayer activities, communication tools, and networking integration enable users to connect, exchange experiences, and build friendships. This interactive element improves the overall betting experience and can be particularly helpful for those seeking social interaction.
Conclusion
Digital casinos offer a diverse variety of advantages, from accessibility and convenience to financial benefits and innovations. They provide diverse betting options, encourage responsible gambling, and promote community engagement. As the industry keeps to grow, online casinos will probably stay a major and positive presence in the realm of digital entertainment.
No-Cost Slot Games: Pleasure and Perks for All
Gratis slot games have become a popular form of digital amusement, granting players the suspense of slot machines free from any monetary outlay.
The primary aim of complimentary slot games is to offer a enjoyable and captivating way for individuals to relish the excitement of slot machines free from any cash danger. They are conceived to replicate the experience of real-money slots, allowing players to spin the reels, enjoy various concepts, and earn electronic payouts.
Pleasure: No-Cost slot games are an outstanding option of amusement, offering spans of excitement. They present vibrant illustrations, captivating music, and multifaceted concepts that serve a wide variety of inclinations.
Proficiency Improvement: For newcomers, no-cost slot games grant a risk-free setting to learn the workings of slot machines. Players can get accustomed with various feature sets, payout lines, and additional features free from the fear of sacrificing cash.
Destressing: Playing free slot games can be a fantastic way to unwind. The straightforward interaction and the opportunity for virtual prizes make it an pleasurable activity.
Social Interaction: Many gratis slot games include social features such as tournaments and the option to interact with peers. These elements inject a group-based aspect to the gaming experience, inspiring players to measure up against others.
Perks of Complimentary Slot Games
1. Availability and Simplicity
Free slot games are conveniently approachable to all with an web connection. They can be played on diverse devices including computers, handhelds, and smartphones. This ease gives players to savor their preferred offerings at any time and from any place.
2. Economic Risk-Freeness
One of the primary rewards of gratis slot games is that they exclude the monetary jeopardies associated with wagering. Players can relish the rush of activating the reels and obtaining significant rewards absent investing any cash.
3. Breadth of Offerings
Complimentary slot games come in a wide array of concepts and formats, from nostalgic fruit-themed slots to modern slot machines with video with intricate plotlines and illustrations. This breadth provides that there is an alternative for all, independent of their tastes.
4. Developing Intellectual Aptitudes
Playing complimentary slot games can tend to improve intellectual faculties such as anticipatory planning. The necessity to consider winning combinations, learn operational principles, and foresee consequences can offer a cerebral training that is equally pleasurable and beneficial.
5. Secure Pre-Testing for Paid-Participation
For those contemplating progressing to for-profit slots, no-cost slot games offer a valuable testing ground. Players can explore different games, refine strategies, and develop assurance ahead of opting to stake real cash. This groundwork can culminate in a more knowledgeable and enjoyable real-money gaming encounter.
Summary
No-Cost slot games deliver a wealth of rewards, from unadulterated entertainment to proficiency improvement and shared experiences. They offer a worry-free and free-of-charge way to savor the suspense of slot machines, constituting them a helpful complement to the world of electronic recreation. Whether you’re wanting to relax, enhance your cognitive skills, or simply enjoy yourself, gratis slot games are a superb choice that continues to delight players worldwide.
forum syair sdy
Ashley JKT48: Bintang yang Bercahaya Terang di Langit Idol
Siapa Ashley JKT48?
Siapa figur muda berbakat yang mencuri perhatian banyak sekali penggemar musik di Nusantara dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang terkenal dengan nama bekennya, Ashley JKT48. Masuk dengan grup idol JKT48 pada tahun 2018, Ashley dengan cepat menjadi salah satu anggota paling favorit.
Riwayat Hidup
Dilahirkan di Jakarta pada tanggal 13 Maret 2000, Ashley berdarah darah Tionghoa-Indonesia. Beliau memulai perjalanannya di industri hiburan sebagai peraga dan aktris, sebelum selanjutnya bergabung dengan JKT48. Kepribadiannya yang periang, vokal yang mantap, dan keterampilan menari yang memukau membentuknya sebagai idola yang sangat dicintai.
Pengakuan dan Apresiasi
Kepopuleran Ashley telah diakui melalui berbagai penghargaan dan nominasi. Pada tahun 2021, ia memenangkan penghargaan “Personel Terpopuler JKT48” di ajang Penghargaan Musik JKT48. Ashley juga dinobatkan sebagai “Idol Terindah di Asia” oleh sebuah tabloid digital pada masa 2020.
Peran dalam JKT48
Ashley mengisi peran penting dalam group JKT48. Ia adalah anggota Tim KIII dan berperan menjadi penari utama dan vokalis. Ashley juga menjadi member dari unit sub “J3K” dengan Jessica Veranda dan Jennifer Rachel Natasya.
Karier Solo
Di luar kegiatan dengan JKT48, Ashley juga merintis karier solo. Ia telah meluncurkan sejumlah single, termasuk “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah bekerja sama bersama artis lain, seperti Afgan dan Rossa.
Kehidupan Pribadi
Di luar bidang perform, Ashley dikenal sebagai pribadi yang rendah hati dan bersahabat. Ia menikmati menghabiskan waktu bersama family dan sahabat-sahabatnya. Ashley juga memiliki kegemaran menggambar dan fotografi.
buy cheap bactrim
slots machines
No-Cost Slot Games: Pleasure and Benefits for People
Introduction
Slot machines have historically been a cornerstone of the gaming interaction, granting customers the prospect to secure major payouts with simply the activation of a arm or the push of a mechanism. In recent years, slot-based activities have as well grown to be widespread in internet-based gaming sites, rendering them approachable to an further more expansive group.
Fun Element
Slot-based games are designed to be pleasurable and immersive. They showcase animated visuals, electrifying auditory elements, and various ideas that cater to a extensive variety of interests. Regardless of whether players enjoy time-honored fruit-related symbols, excitement-driven slot-based activities, or slot-based activities derived from well-known films, there is an option for all. This variety ensures that customers can persistently find a experience that suits their interests, delivering spans of pleasure.
Straightforward to Operate
One of the most prominent advantages of slot machines is their uncomplicated nature. In contrast to specific wagering activities that call for strategy, slot-based activities are easy to grasp. This makes them accessible to a comprehensive group, involving inexperienced individuals who may feel intimidated by increasingly complex experiences. The uncomplicated nature of slot machines allows participants to decompress and experience the game without fretting about intricate rules.
Unwinding and Destressing
Interacting with slot-based activities can be a fantastic way to destress. The monotonous nature of triggering the drums can be serene, offering a cerebral escape from the demands of routine life. The prospect for winning, even when it constitutes only minimal amounts, brings an aspect of suspense that can elevate customers’ mindsets. Numerous people conclude that partaking in slot-based activities assists them unwind and shift their focus away from their concerns.
Social Interaction
Slot machines likewise present chances for communal connection. In land-based gambling establishments, participants often gather near slot-based games, encouraging their fellow players on and commemorating triumphs as a group. Online slot-based activities have likewise incorporated communal elements, such as rankings, allowing participants to connect with co-participants and share their encounters. This sense of shared experience elevates the overall interactive experience and can be particularly pleasurable for people aspiring to social connection.
Financial Advantages
The widespread appeal of slot-based games has noteworthy fiscal rewards. The field yields opportunities for game creators, gambling personnel, and player support agents. Additionally, the revenue produced by slot machines provides to the fiscal landscape, providing budgetary incomes that support societal programs and systems. This financial effect reaches to simultaneously land-based and internet-based wagering facilities, establishing slot-related offerings a helpful element of the interactive field.
Mental Upsides
Playing slot machines can likewise have intellectual upsides. The experience demands customers to make prompt selections, discern regularities, and manage their wagering approaches. These cerebral activities can facilitate preserve the thought processes focused and bolster mental functions. For older adults, engaging in mentally stimulating activities like playing slot-based activities can be useful for sustaining cognitive health.
Availability and Ease of Access
The introduction of internet-based gambling platforms has rendered slot-based activities more accessible than before. Customers can relish their most preferred slot-based games from the ease of their individual residences, utilizing computers, pads, or mobile phones. This ease allows people to play at any time and irrespective of location they want, free from the necessity to make trips to a brick-and-mortar wagering facility. The offering of gratis slot-based games in addition allows customers to relish the offering absent any economic stake, making it an open-to-all type of amusement.
Key Takeaways
Slot-based activities grant a wealth of benefits to people, from absolute amusement to mental benefits and social interaction. They present a worry-free and zero-cost way to experience the excitement of slot-based activities, making them a helpful enhancement to the realm of virtual amusement.
Whether you’re wanting to decompress, hone your cognitive aptitudes, or solely experience pleasure, slot machines are a fantastic option that continues to delight users across.
Prominent Benefits:
– Slot-based activities offer amusement through vibrant illustrations, engaging soundtracks, and varied concepts
– Simple engagement constitutes slot-related offerings reachable to a broad population
– Interacting with slot-based activities can offer relaxation and mental upsides
– Collaborative functions bolster the total leisure experience
– Digital accessibility and complimentary options render slot-based games accessible forms of fun
In recap, slot-related offerings continue to deliver a diverse assortment of advantages that suit participants around. Whether seeking absolute fun, mental challenge, or social involvement, slot-based games continue to be a wonderful choice in the dynamic domain of electronic recreation.
Virtual Wagering Environment For-Profit: Upsides for Users
Summary
Digital wagering environments granting actual currency experiences have gained substantial widespread adoption, granting users with the opportunity to receive economic rewards while experiencing their favorite gaming experiences from residence. This write-up investigates the advantages of internet-based gambling platform actual currency games, accentuating their positive influence on the gaming industry.
Simplicity and Approachability
Virtual wagering environment paid games grant convenience by permitting participants to engage with a extensive variety of activities from any setting with an network access point. This removes the necessity to commute to a traditional wagering facility, conserving resources. Virtual wagering environments are likewise offered at all times, permitting participants to engage with at their ease.
Variety of Games
Digital gaming sites provide a more extensive range of offerings than physical casinos, incorporating slot-related offerings, blackjack, spinning wheel, and card games. This breadth enables players to experiment with novel offerings and uncover new most cherished, elevating their overall entertainment encounter.
Incentives and Special Offers
Online casinos provide substantial perks and discounts to draw in and hold onto players. These bonuses can incorporate welcome perks, complimentary rounds, and reimbursement promotions, providing additional value for users. Membership systems as well compensate users for their continued patronage.
Capability Building
Partaking in real money offerings online can assist participants develop abilities such as problem-solving. Experiences like pontoon and poker demand users to make determinations that can impact the outcome of the offering, assisting them develop critical thinking abilities.
Communal Engagement
ChatGPT l Валли, 6.06.2024 4:08]
Internet-based gambling platforms offer prospects for social participation through chat rooms, online communities, and real-time croupier activities. Users can communicate with fellow users, communicate strategies and strategies, and sometimes form friendships.
Economic Benefits
The internet-based gambling domain produces jobs and provides for the economic landscape through fiscal revenues and authorization charges. This fiscal influence benefits a broad range of vocations, from offering creators to customer services professionals.
Conclusion
Digital gaming site real money offerings offer many rewards for customers, involving ease, range, incentives, competency enhancement, communal engagement, and financial upsides. As the sector steadfastly transform, the popularity of online casinos is expected to expand.
Prosperity Casino: Where Amusement Converges With Luck
Wealth Wagering Environment is a well-liked digital place identified for its extensive range of experiences and thrilling rewards. Let’s explore the reasons why so several people relish engaging with Luck Gambling Platform and the extent to which it benefits them.
Pleasure-Providing Aspect
Prosperity Gambling Platform presents a variety of offerings, featuring traditional card games like blackjack and ball-and-number game, as alongside novel slot machines. This variety secures that there is a choice for anyone, constituting every trip to Fortune Wagering Environment rewarding and entertaining.
Big Winnings
One of the main attractions of Prosperity Gambling Platform is the chance to secure major payouts. With generous jackpots and incentives, participants have the chance to experience a reversal of fortune with a lone turn or game. Several users have acquired significant payouts, contributing to the excitement of interacting with Luck Wagering Environment.
Ease of Access and Reachability
Prosperity Gambling Platform’s internet-based interface makes it user-friendly for participants to enjoy their favorite offerings from any setting. Regardless of whether at residence or in transit, customers can engage with Luck Gaming Site from their PC or handheld. This reachability provides that participants can experience the anticipation of the wagering anytime they choose, without the necessity to make trips.
Variety of Games
Fortune Gaming Site presents a wide array of activities, providing that there is an alternative for every single style of user. Starting with time-honored wagering games to conceptual slot-based games, the breadth keeps players captivated and delighted. This selection in addition enables participants to try out new games and find different most liked.
Promotional Benefits
Fortune Wagering Environment compensates its players with incentives and advantages, including new player bonuses and dedication initiatives. These bonuses not just improve the entertainment sensation but likewise boost the chances of earning significant rewards. Players are constantly encouraged to maintain participation, constituting Prosperity Wagering Environment increasingly desirable.
Group-Based Participation and Collaboration
ChatGPT l Валли, 6.06.2024 4:30]
Wealth Wagering Environment offers a environment of togetherness and group-based participation for customers. Using chat rooms and forums, participants can connect with each other, exchange tips and strategies, and even create social relationships. This communal component brings another dimension of satisfaction to the entertainment experience.
Summary
Fortune Casino provides a comprehensive variety of upsides for customers, encompassing enjoyment, the chance to win big, simplicity, range, perks, and interpersonal connections. Regardless of whether desiring suspense or aspiring to achieve unexpected success, Luck Wagering Environment provides an captivating interaction for everyone who engage with.
free poker machine games
Free Poker Machine Activities: A Enjoyable and Beneficial Sensation
Complimentary poker machine activities have emerged as progressively widely-accepted among participants looking for a captivating and risk-free interactive sensation. These offerings present a extensive array of rewards, constituting them as a selected option for numerous. Let’s explore in what way gratis electronic gaming experiences can advantage players and the motivations behind they are so comprehensively relished.
Pleasure-Providing Aspect
One of the main motivations players savor interacting with no-cost virtual wagering activities is for the fun element they offer. These experiences are designed to be captivating and enthralling, with vibrant graphics and immersing audio that enhance the total interactive encounter. Whether you’re a occasional customer seeking to pass the time or a serious gaming aficionado seeking excitement, complimentary slot-based offerings offer entertainment for everyone who.
Skill Development
Interacting with free poker machine experiences can in addition enable hone valuable skills such as strategic thinking. These experiences demand customers to render rapid choices reliant on the virtual assets they are dealt, enabling them hone their analytical abilities and cognitive dexterity. Additionally, participants can try out different tactics, refining their faculties without the risk of parting with real money.
Ease of Access and Reachability
A supplemental reward of gratis electronic gaming activities is their convenience and approachability. These experiences can be interacted with in the virtual sphere from the convenience of your own abode, eradicating the requirement to make trips to a land-based wagering facility. They are as well present around the clock, giving participants to relish them at any desired period that fits them. This convenience establishes complimentary slot-based experiences a sought-after alternative for players with demanding agendas or those looking for a immediate interactive solution.
Shared Experiences
A significant number of no-cost virtual wagering experiences in addition present communal functions that enable participants to communicate with one another. This can incorporate messaging platforms, online communities, and multiplayer configurations where participants can pit themselves against each other. These interpersonal connections bring an further layer of satisfaction to the leisure interaction, permitting players to communicate with like-minded individuals who display their passions.
Stress Relief and Relaxation
Engaging with gratis electronic gaming games can likewise be a great means to unwind and de-stress after a tiring stretch of time. The uncomplicated activity and tranquil audio can assist decrease tension and nervousness, providing a refreshing break from the obligations of typical existence. Additionally, the thrill of obtaining simulated credits can elevate your emotional state and make you feel reenergized.
Key Takeaways
No-cost virtual wagering games present a comprehensive range of advantages for players, involving entertainment, skill development, convenience, social interaction, and worry mitigation and mental rejuvenation. Regardless of whether you’re seeking to enhance your poker skills or simply experience pleasure, complimentary slot-based games deliver a beneficial and pleasurable encounter for players of every stages.
Контроль счета криптовалюты
Проверка криптовалюты на платформе TRC20 и прочих блокчейн платежей
На этом веб-сайте вы найдете развернутые описания многочисленных платформ для верификации платежей и аккаунтов, содержащие anti-money laundering контроли для криптовалюты и иных криптовалют. Вот ключевые возможности, доступные в наших описаниях:
Контроль токенов TRC20
Известные сервисы предлагают полную анализ переводов USDT в блокчейн-сети TRC20 блокчейна. Это гарантирует фиксировать сомнительную действия и выполнять нормативным требованиям.
Верификация транзакций монет
В представленных оценках описаны инструменты для детального анализа и контроля операций USDT, что способствует сохранять прозрачность и надежность платежей.
anti-money laundering анализ USDT
Определенные инструменты обеспечивают антиотмывочного закона анализ токенов, позволяя обнаруживать и исключать эпизоды незаконных операций и денежных нарушений.
Проверка аккаунта криптовалюты
Наши оценки включают платформы, которые дают возможность верифицировать кошельки токенов на определение ограничений и сомнительных активностей, поддерживая дополнительный степень безопасности.
Верификация транзакции криптовалюты на сети TRC20
В наших обзорах доступны сервисы, обеспечивающие верификацию платежей монет в блокчейн-сети TRC20, что гарантирует соответствие удовлетворение необходимым необходимым правилам.
Верификация адреса счета USDT
В ревью описаны платформы для проверки аккаунтов аккаунтов токенов на предмет угроз угроз.
Анализ адреса токенов на платформе TRC20
Наши описания охватывают платформы, поддерживающие верификацию аккаунтов криптовалюты в блокчейн-сети TRC20 сети, что предотвращает предотвращает предотвращение финансовых преступлений и валютных мошенничеств.
Анализ криптовалюты на отсутствие подозрительных действий
Представленные ресурсы предусматривают анализировать транзакции и счета на прозрачность, выявляя подозреваемую операции.
антиотмывочного закона проверка токенов на платформе TRC20
В оценках вы платформы, предоставляющие AML верификацию для монет на платформе TRC20 блокчейна, что помогает вашему предприятию соответствовать международным нормам.
Контроль USDT ERC20
Наши описания включают платформы, поддерживающие контроль USDT в блокчейн-сети ERC20 сети, что позволяет позволяет проведение операций и счетов.
Контроль цифрового кошелька
Мы обозреваем ресурсы, поддерживающие опции по проверке криптовалютных кошельков, в том числе мониторинг операций и фиксирование подозреваемой операций.
Проверка аккаунта криптовалютного кошелька
Наши ревью представляют инструменты, обеспечивающие контролировать адреса криптокошельков для поддержания повышенной безопасности.
Проверка цифрового кошелька на операции
В наших описаниях доступны платформы для контроля криптовалютных кошельков на транзакции, что позволяет гарантирует обеспечивать открытость платежей.
Верификация криптокошелька на отсутствие подозрительных действий
Наши оценки содержат платформы, дающие возможность верифицировать криптовалютные кошельки на отсутствие подозрительных действий, определяя подозрительные сомнительные платежи.
Изучая представленные ревью, вы сможете выберете оптимальные ресурсы для анализа и отслеживания блокчейн переводов, чтобы поддерживать гарантировать повышенный степень безопасности защищенности и выполнять все правовым требованиям.
Digital Casino-Style Games: A Wellspring of Entertainment and Skill Development
Internet-based table games has emerged as a popular kind of amusement and a medium for skill development for customers across the globe. This write-up analyzes the constructive facets of digital table games and in which manner it upsides users, emphasizing its pervasive appeal and impact.
Amusement Factor
Digital table games grants a captivating and engaging gaming experience, spellbinding users with its calculated engagement and changeable ends. The game’s absorbing nature, coupled with its collaborative facets, offers a distinctive form of pleasure that numerous regard as enjoyable.
Skill Development
Aside from fun, digital table games also functions as a avenue for proficiency improvement. The activity demands strategic thinking, rapid responses, and the ability to comprehend adversaries, each of which add to mental growth. Customers can elevate their decision-making faculties, emotional intelligence, and risk management abilities through regular gameplay.
User-Friendliness and Availability
One of the main rewards of internet-based card games is its ease and accessibility. Players can relish the activity from the ease of their abodes, at any desired occasion that aligns with them. This accessibility excludes the obligation for journey to a traditional casino, rendering it a easy-to-access choice for users with demanding routines.
Variety of Games and Stakes
Internet-based card games infrastructures grant a comprehensive breadth of games and stake amounts to serve customers of every stages of proficiency and preferences. Whether you’re a learner looking to understand the essentials or a skilled pro aspiring to a test, there is a game for your preferences. This variety ensures that customers can constantly find a game that fits their skill level and spending power.
Interpersonal Connections
Online poker also delivers avenues for communal engagement. Numerous platforms present communication tools and competitive modes that permit customers to engage with others, share experiences, and establish interpersonal bonds. This group-based factor contributes complexity to the entertainment encounter, making it more enjoyable.
Monetary Gains
For certain individuals, online poker can also be a wellspring of financial rewards. Adept participants can earn considerable earnings through frequent interactivity, establishing it as a lucrative endeavor for those who dominate the game. Also, numerous virtual casino-style games tournaments provide considerable payouts, delivering users with the possibility to secure major payouts.
Recap
Virtual casino-style games presents a array of benefits for customers, including pleasure, competency enhancement, user-friendliness, shared experiences, and earnings opportunities. Its recognition steadfastly increase, with many people gravitating towards online poker as a provider of pleasure and advancement. Whether you’re wanting to sharpen your skills or just derive entertainment, internet-based card games is a adaptable and beneficial pastime for customers of every perspectives.
아프리카티비 마약
신속한 입출금 서비스 및 메이저업체의 보안성
스포츠토토사이트 접속 시 가장 중요한 요소 중 하나는 빠른 환충 절차입니다. 대개 세 분 안에 충전, 십 분 내에 환전이 처리되어야 합니다. 대형 대형업체들은 넉넉한 스태프 고용을 통해 이와 같은 신속한 환충 프로세스를 보장하며, 이 방법으로 회원들에게 안전한 느낌을 제공합니다. 주요사이트를 접속하면서 신속한 체감을 즐겨보세요. 우리 고객님이 안전하게 웹사이트를 사용할 수 있도록 도와드리는 먹튀 해결 팀입니다.
보증금 걸고 배너를 운영
먹튀해결사는 최소 삼천만 원부터 1억 원의 보증 금액을 예치한 회사들의 배너 광고를 운영하고 있습니다. 만일 먹튀 문제가 발생할 경우, 베팅 규정에 위배되지 않은 베팅 내역을 캡처하여 먹튀 해결 팀에 연락 주시면, 사실 확인 뒤 보증 자금으로 즉시 손해 보상을 처리합니다. 피해 발생 시 즉시 캡처해서 피해 내용을 저장해두시고 제출해 주세요.
오랫동안 안전하게 운영된 업체 확인
먹튀 해결 팀은 적어도 4년 이상 먹튀 문제 없이 안전하게 운영하고 있는 업체만을 인증하여 광고 배너 입점을 허용합니다. 이로 인해 모두가 알고 있는 대형사이트를 안전하게 접속할 수 있는 기회를 제공합니다. 철저한 검증 작업을 통해 검증된 사이트를 놓치지 않도록, 안전한 배팅을 경험해보세요.
투명하고 공정한 먹튀 검토
먹튀 해결 전문가의 먹튀 검토는 투명함과 정확함을 바탕으로 합니다. 늘 이용자들의 의견을 최우선으로 생각하며, 기업의 유혹이나 이익에 흔들리지 않고 1건의 삭제 없이 진실만을 바탕으로 검토해왔습니다. 먹튀 피해를 겪고 후회하지 않도록, 바로 지금 시작하세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 엄선한 안전한 토토사이트 검증된 업체 목록 입니다. 현재 등록되어 있는 인증된 업체들은 먹튀 피해 발생 시 100% 보장을 해드립니다. 다만, 제휴 기간이 끝난 업체에서 발생한 문제에 대해서는 책임지지 않습니다.
탁월한 먹튀 검증 알고리즘
먹튀 해결 전문가는 깨끗한 베팅 문화를 조성하기 위해 계속해서 애쓰고 있습니다. 저희가 소개하는 베팅사이트에서 안심하고 베팅하세요. 사용자의 먹튀 제보는 먹튀 리스트에 등록되어 해당되는 베팅 사이트에 심각한 영향을 미칩니다. 먹튀 리스트 작성 시 먹튀블러드의 검증 지식을 최대한 활용하여 공평한 심사를 하도록 약속드립니다.
안전한 베팅 환경을 만들기 위해 계속해서 애쓰는 먹튀해결사와 함께 안심하고 즐기시기 바랍니다.
вызов такси в новочеркасске https://taxi-novocherkassk.ru
курсовые работы на заказ https://zakazat-kursovuyu-rabotu7.ru
In this eager game, players vie in multiplayer shooting matches on various battlegrounds. The open-handed of bullet force is to outgun opponents and secure conquest using cardinal meditative and quick reflexes. With its international weapon abstract and customizable gameplay, this design delivers an far-out shooting experience
стоимость такси такси в аэропорт
заказать такси недорого номер телефона такси
служба такси телефон такси новочеркасск
internet casinos
Online Gambling Sites: Innovation and Advantages for Modern Community
Introduction
Online gambling platforms are digital platforms that provide players the chance to participate in gambling activities such as card games, spin games, blackjack, and slot machines. Over the last several years, they have turned into an integral component of digital entertainment, providing numerous advantages and opportunities for players globally.
Accessibility and Convenience
One of the primary advantages of digital gambling sites is their availability. Players can enjoy their preferred games from any location in the globe using a computer, iPad, or smartphone. This saves hours and funds that would typically be used traveling to traditional gambling halls. Additionally, round-the-clock availability to activities makes internet casinos a easy option for people with busy schedules.
Variety of Games and Entertainment
Online gambling sites provide a wide variety of activities, allowing all users to find something they enjoy. From traditional table activities and table games to slot machines with various concepts and progressive prizes, the diversity of activities guarantees there is something for every taste. The ability to play at various proficiencies also makes online gambling sites an ideal location for both beginners and seasoned players.
Financial Advantages
The digital gambling industry contributes significantly to the economy by creating employment and generating revenue. It supports a diverse variety of professions, including software developers, customer support representatives, and marketing specialists. The revenue produced by digital gambling sites also adds to government funds, which can be used to fund community services and development initiatives.
Advancements in Technology
Digital casinos are at the forefront of technological advancement, constantly integrating new innovations to improve the playing experience. Superior graphics, live dealer games, and virtual reality (VR) casinos provide engaging and authentic gaming experiences. These innovations not only improve player satisfaction but also push the boundaries of what is possible in online entertainment.
Responsible Gambling and Assistance
Many online casinos promote safe betting by offering tools and assistance to help players control their gaming habits. Options such as deposit limits, self-exclusion options, and access to support services guarantee that players can engage in gaming in a safe and controlled setting. These measures demonstrate the sector’s dedication to promoting healthy gaming habits.
Social Interaction and Networking
Digital gambling sites often offer interactive options that allow players to interact with each other, creating a feeling of belonging. Group activities, chat functions, and networking integration enable users to connect, share experiences, and build relationships. This interactive element enhances the entire gaming entertainment and can be especially helpful for those seeking social interaction.
Conclusion
Online gambling sites offer a wide variety of benefits, from availability and ease to economic contributions and technological advancements. They provide diverse betting options, encourage safe betting, and promote social interaction. As the sector continues to evolve, online casinos will likely stay a major and positive presence in the world of online entertainment.
мобильное такси дешевое такси телефон
free slots games
Free Slot Games: Amusement and Perks for All
No-Cost slot games have become a popular form of digital entertainment, delivering players the thrill of slot machines without any financial stake.
The main purpose of complimentary slot games is to provide a entertaining and engaging way for players to enjoy the excitement of slot machines absent any economic risk. They are developed to imitate the feeling of paid slots, allowing players to activate the reels, experience various motifs, and obtain virtual payouts.
Fun: No-Cost slot games are an fantastic avenue of leisure, delivering periods of enjoyment. They display colorful visuals, immersive soundtracks, and diverse themes that suit a comprehensive range of preferences.
Capability Enhancement: For inexperienced, free slot games present a risk-free setting to acquaint the principles of slot machines. Players can get acquainted with multiple game features, winning combinations, and special features free from the fear of losing cash.
Destressing: Playing free slot games can be a great way to de-stress. The straightforward handling and the possibility for electronic winnings make it an satisfying hobby.
Shared Experiences: Many no-cost slot games incorporate collaborative elements such as tournaments and the capacity to interact with peers. These features contribute a communal facet to the entertainment experience, empowering players to pit themselves against others.
Perks of Gratis Slot Games
1. Availability and Simplicity
Complimentary slot games are conveniently approachable to all with an network connection. They can be played on different devices including laptops, tablets, and cellphones. This simplicity permits players to enjoy their favorite activities anytime and in any location.
2. Fiscal Unconcern
One of the paramount rewards of no-cost slot games is that they eliminate the cash-related dangers associated with gambling. Players can enjoy the excitement of rotating the reels and hitting significant rewards without wagering any capital.
3. Diversity of Options
Gratis slot games are available in a extensive selection of ideas and formats, from nostalgic fruit slots to contemporary video slots with complex plotlines and illustrations. This breadth provides that there is an option for anyone, irrespective of their preferences.
4. Developing Intellectual Aptitudes
Playing gratis slot games can tend to develop mental capabilities such as anticipatory planning. The task to pursue win lines, internalize procedural knowledge, and estimate results can grant a intellectual training that is simultaneously pleasurable and beneficial.
5. Secure Pre-Testing for Actual-Currency Gaming
For those considering progressing to real-money slots, gratis slot games offer a helpful trial environment. Players can experiment with various games, develop strategies, and build self-assurance prior to deciding to wager actual funds. This groundwork can translate to a more knowledgeable and satisfying for-profit gaming encounter.
Recap
Gratis slot games provide a abundance of advantages, from pure entertainment to competency enhancement and interpersonal connections. They grant a safe and non-monetary way to experience the excitement of slot machines, making them a helpful addition to the domain of virtual entertainment. Whether you’re aiming to de-stress, sharpen your cognitive skills, or just have fun, free slot games are a fantastic option that steadfastly captivate players worldwide.
Хотите быть в курсе всех важных тем в сфере недвижимости?
На нашем ресурсе вы сможете найти множество интересных статей о квартирах от застройщика, налогах на недвижимость, а также о регистрации квартиры.
http://zoltor24sochi.ru
стоит такси заказать такси в новочеркасске
aciphex buy online – brand metoclopramide 10mg domperidone usa
вызвать такси недорого https://taxi-vyzvat.ru
online casino real money
Online Wagering Environment Real Money: Rewards for Customers
Introduction
Digital wagering environments offering for-profit offerings have obtained significant broad acceptance, offering users with the chance to earn monetary winnings while relishing their most preferred gambling offerings from abode. This text investigates the advantages of internet-based gambling platform for-profit activities, highlighting their beneficial impact on the entertainment sector.
Simplicity and Approachability
Online casino actual currency experiences offer ease by permitting users to access a extensive variety of experiences from any place with an network access. This eliminates the requirement to commute to a physical wagering facility, saving effort. Virtual wagering environments are also accessible 24/7, allowing users to play at their ease.
Variety of Games
Online casinos offer a more broad breadth of activities than traditional wagering facilities, featuring slot-based activities, vingt-et-un, spinning wheel, and casino-style games. This breadth allows users to investigate different offerings and identify novel favorites, enhancing their overall interactive sensation.
Rewards and Discounts
Online casinos provide considerable perks and advantages to attract and hold onto players. These bonuses can incorporate introductory bonuses, complimentary rounds, and cashback advantages, granting additional significance for users. Reward systems also acknowledge customers for their steady custom.
Skill Development
Engaging with for-profit activities on the internet can help players develop skills such as critical analysis. Activities like blackjack and poker call for customers to render selections that can shape the conclusion of the activity, enabling them hone problem-solving faculties.
Shared Experiences
ChatGPT l Валли, 6.06.2024 4:08]
Online casinos deliver opportunities for communal interaction through messaging platforms, online communities, and real-time croupier activities. Participants can interact with fellow users, share tips and approaches, and occasionally form interpersonal bonds.
Financial Advantages
The online casino domain generates employment and provides for the economy through fiscal revenues and operational costs. This fiscal influence rewards a comprehensive variety of occupations, from experience developers to customer services representatives.
Summary
Internet-based gambling platform for-profit activities grant numerous rewards for participants, incorporating convenience, diversity, incentives, proficiency improvement, interpersonal connections, and economic upsides. As the field steadfastly progress, the broad acceptance of virtual wagering environments is expected to rise.
order aciphex 10mg without prescription – reglan online motilium order online
Fortune Casino: In an Environment Where Fun Meets Luck
Prosperity Gambling Platform is a well-liked internet-based location known for its broad range of activities and enthralling bonuses. Let’s investigate the factors that explain why so several players experience playing at Prosperity Casino and how it upsides them.
Fun Element
Fortune Gaming Site offers a diversity of offerings, involving nostalgic casino games like vingt-et-un and ball-and-number game, as together with innovative slot-based activities. This diversity secures that there is something for everyone, establishing each encounter to Prosperity Wagering Environment pleasurable and entertaining.
Significant Rewards
One of the key aspects of Luck Wagering Environment is the prospect to win big. With significant grand prizes and incentives, customers have the possibility to produce an unexpected outcome with a one-time spin or hand. A significant number of users have acquired considerable payouts, enhancing the thrill of partaking in Fortune Gambling Platform.
Simplicity and Approachability
Wealth Wagering Environment’s virtual interface establishes it as user-friendly for players to relish their most preferred games from any location. Whether at home or on the go, customers can engage with Luck Casino from their PC or handheld. This reachability ensures that players can relish the excitement of the gaming at any time they desire, free from the need to journey.
Variety of Games
Luck Casino grants a comprehensive array of games, providing that there is an alternative for every kind of customer. Ranging from classic card games to themed slot-based activities, the diversity keeps players immersed and pleased. This choice likewise allows participants to explore different experiences and identify novel favorites.
Bonuses and Rewards
Fortune Gambling Platform recognizes its players with bonuses and advantages, including new player incentives and dedication systems. These rewards not merely improve the leisure sensation but as well raise the chances of winning big. Participants are continually driven to sustain interaction, rendering Fortune Wagering Environment even more appealing.
Communal Engagement and Interpersonal Connections
ChatGPT l Валли, 6.06.2024 4:30]
Fortune Gaming Site grants a sense of collective engagement and communal engagement for customers. Using messaging platforms and discussion boards, users can engage with each other, exchange tips and methods, and even form personal connections. This communal component brings a supplemental layer of pleasure to the gaming experience.
Conclusion
Fortune Gaming Site presents a wide variety of upsides for users, encompassing enjoyment, the prospect of securing major payouts, ease, range, incentives, and shared experiences. Whether desiring excitement or aiming to experience a reversal of fortune, Wealth Gaming Site offers an enthralling encounter for everyone partake in.
номер такси в новочеркасске https://zakaz-taxionline.ru
Free Slot-Based Activities: A Pleasurable and Beneficial Encounter
No-Cost poker machine offerings have become steadily widely-accepted among users desiring a captivating and risk-free interactive interaction. These games provide a broad array of rewards, establishing them as a favored choice for a significant number of. Let’s examine how no-cost virtual wagering experiences can advantage customers and the factors that explain why they are so comprehensively experienced.
Entertainment Value
One of the main reasons users enjoy engaging with complimentary slot-based games is for the fun element they offer. These games are crafted to be engaging and captivating, with colorful illustrations and immersing sound effects that elevate the comprehensive entertainment interaction. Regardless of whether you’re a leisure-oriented customer looking to pass the time or a enthusiastic leisure activity enthusiast aiming for excitement, no-cost virtual wagering offerings provide pleasure for any.
Skill Development
Playing gratis electronic gaming experiences can likewise help refine helpful aptitudes such as strategic thinking. These activities require customers to render rapid choices based on the gameplay elements they are received, enabling them improve their critical-thinking skills and cognitive dexterity. Furthermore, participants can try out various tactics, honing their abilities devoid of the possibility of financial impact of relinquishing monetary resources.
Simplicity and Approachability
An additional reward of complimentary slot-based activities is their ease and reachability. These activities can be interacted with in the virtual sphere from the simplicity of your own residence, eradicating the need to commute to a brick-and-mortar gaming venue. They are likewise accessible at all times, giving users to experience them at any time that suits them. This ease renders complimentary slot-based activities a widely-accepted alternative for participants with demanding timetables or those seeking a quick interactive resolution.
Communal Engagement
Many free poker machine games in addition present social features that permit players to connect with their peers. This can involve discussion forums, online communities, and multiplayer settings where participants can challenge fellow users. These communal engagements contribute an supplemental facet of fulfillment to the leisure experience, enabling users to communicate with peers who share their interests.
Worry Mitigation and Emotional Refreshment
Playing gratis electronic gaming activities can as well be a excellent approach to destress and calm down after a long day. The simple activity and soothing sound effects can facilitate lower stress and anxiety, granting a much-needed escape from the challenges of regular life. Furthermore, the excitement of receiving virtual rewards can boost your mood and result in you feeling revitalized.
Key Takeaways
Gratis electronic gaming offerings provide a broad array of rewards for users, involving entertainment, proficiency improvement, user-friendliness, shared experiences, and worry mitigation and relaxation. Regardless of whether you’re seeking to enhance your gaming faculties or solely derive entertainment, gratis electronic gaming games provide a profitable and fulfilling sensation for users of any types.
Digital Card Games: A Origin of Entertainment and Skill Development
Digital poker has materialized as a sought-after style of amusement and a avenue for proficiency improvement for customers globally. This piece investigates the favorable facets of digital table games and how it advantages users, emphasizing its widespread acceptance and influence.
Fun Element
Online poker offers a thrilling and engaging interactive interaction, captivating participants with its strategic activity and variable outcomes. The experience’s immersive essence, combined with its social aspects, delivers a unique form of pleasure that a significant number of find rewarding.
Competency Enhancement
Apart from pleasure, digital table games likewise operates as a channel for proficiency improvement. The game calls for critical analysis, rapid responses, and the aptitude to interpret opponents, each of which provide for mental growth. Players can improve their problem-solving aptitudes, adaptability, and risk management aptitudes through frequent activity.
Simplicity and Approachability
One of the primary upsides of digital table games is its user-friendliness and approachability. Users can enjoy the experience from the ease of their residences, at any desired moment that aligns with them. This availability eradicates the obligation for commute to a traditional gambling establishment, constituting it as a easy-to-access choice for users with hectic routines.
Range of Possibilities and Stake Amounts
Online poker infrastructures present a comprehensive breadth of activities and wagers to serve players of every types of abilities and desires. Regardless of whether you’re a learner wanting to learn the fundamentals or a experienced specialist aspiring to a trial, there is a game for you. This range guarantees that users can constantly locate a offering that matches their capabilities and financial resources.
Interpersonal Connections
Online poker in addition offers avenues for communal engagement. Numerous interfaces offer chat features and collaborative configurations that allow users to communicate with like-minded players, communicate interactions, and build friendships. This collaborative aspect injects richness to the entertainment experience, making it even more rewarding.
Monetary Gains
For some, virtual casino-style games can as well be a source of monetary gains. Proficient players can obtain substantial profits through ongoing activity, constituting it as a profitable venture for those who thrive at the game. Furthermore, a significant number of digital table games matches present considerable reward funds, granting participants with the prospect to secure major payouts.
Conclusion
Internet-based card games grants a selection of advantages for participants, involving fun, capability building, user-friendliness, communal engagement, and earnings opportunities. Its popularity continues to expand, with many users gravitating towards virtual casino-style games as a origin of enjoyment and advancement. Whether you’re seeking to refine your faculties or merely derive entertainment, internet-based card games is a flexible and advantageous pastime for users of all perspectives.
신속한 입출금 서비스 및 메이저업체의 안전성
베팅사이트 이용 시 핵심적인 요소는 빠릿한 충환전 절차입니다. 대개 삼 분 이내에 충전, 열 분 안에 환충이 처리되어야 합니다. 메이저 대형업체들은 넉넉한 직원 고용을 통해 이 같은 빠릿한 환충 절차를 약속하며, 이를 통해 고객들에게 안도감을 제공합니다. 대형사이트를 사용하면서 신속한 체감을 해보시기 바랍니다. 우리는 여러분이 보안성 있게 웹사이트를 접속할 수 있도록 지원하는 먹튀 해결 팀입니다.
보증금을 걸고 광고 배너 운영
먹튀 해결 전문가는 최대한 3000만 원에서 일억 원의 보증 자금을 예치하고 있는 업체들의 배너를 운영합니다. 만일 먹튀 문제가 발생할 시, 배팅 규정에 반하지 않은 베팅 내역을 캡처해서 먹튀 해결 전문가에게 문의 주시면, 확인 후 보증 금액으로 즉시 손해 보상을 처리합니다. 피해가 생기면 빠르게 스크린샷을 찍어 피해 상황을 기록해두시고 보내주시기 바랍니다.
장기간 안전 운영 업체 확인
먹튀해결사는 적어도 4년 이상 먹튀 문제 없이 안정적으로 운영한 사이트들을 인증하여 배너 등록을 허가합니다. 이를 통해 누구나 알고 있는 주요사이트를 안심하고 이용할 수 있는 기회를 제공합니다. 엄격한 검증 작업을 통해 확인된 사이트를 놓치지 말고, 보안된 베팅을 즐겨보세요.
투명하고 공정한 먹튀 검토
먹튀 해결 전문가의 먹튀 검증은 공정성과 공평성을 근거로 실시합니다. 늘 사용자들의 의견을 최우선으로 생각하며, 기업의 유혹이나 이익에 흔들리지 않고 한 건의 삭제 없이 진실만을 바탕으로 검증해오고 있습니다. 먹튀 문제를 겪고 후회하지 않도록, 바로 지금 시작해보세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 선별한 안전 토토사이트 인증된 업체 목록 입니다. 지금 등록된 인증된 업체들은 먹튀 문제가 발생 시 100% 보증을 제공해드립니다. 하지만, 제휴 기간이 만료된 업체에서 발생한 피해에 대해서는 책임이 없습니다.
탁월한 먹튀 검증 알고리즘
먹튀 해결 전문가는 공정한 베팅 문화를 형성하기 위해 항상 노력하고 있습니다. 저희는 권장하는 베팅사이트에서 안심하고 배팅하세요. 사용자의 먹튀 제보는 먹튀 목록에 등록되어 해당되는 토토사이트에 치명적인 영향을 줄 수 있습니다. 먹튀 리스트를 작성할 때 먹튀블러드의 검토 경험을 충분히 활용하여 공평한 심사를 하도록 약속드립니다.
안전한 도박 환경을 조성하기 위해 계속해서 힘쓰는 먹튀 해결 전문가와 함께 안심하고 즐기시기 바랍니다.
номер такси в новочеркасске https://taxi-vyzvat.ru
курсовые работы на заказ https://zakazat-kontrolnuyu7.ru
решение задач на заказ https://resheniye-zadach7.ru заказать онлайн
рефераты на заказ https://kupit-referat213.ru
milan
Pasang Aplikasi 888 dan Menangkan Besar: Panduan Cepat
**App 888 adalah opsi terbaik untuk Anda yang membutuhkan permainan main digital yang seru dan bermanfaat. Melalui bonus harian dan opsi menggiurkan, program ini bersiap menghadirkan pengalaman bertaruhan paling baik. Berikut manual cepat untuk menggunakan penggunaan Perangkat Lunak 888.
Instal dan Segera Menangkan
Sistem Tersedia:
Program 888 bisa diambil di Android, iOS, dan PC. Awali bermain dengan cepat di gadget manapun.
Hadiah Sehari-hari dan Hadiah
Keuntungan Login Sehari-hari:
Buka pada masa untuk meraih keuntungan mencapai 100K pada periode ketujuh.
Selesaikan Tugas:
Raih kesempatan lotere dengan menyelesaikan misi terkait. Satu pekerjaan memberi Para Pengguna satu kesempatan lotere untuk memenangkan keuntungan sebesar 888K.
Pengumpulan Langsung:
Imbalan harus diambil mandiri di dalam aplikasi. Jangan lupa untuk mendapatkan imbalan setiap periode agar tidak batal.
Prosedur Undi
Opsi Undian:
Masing-masing periode, Anda bisa mendapatkan sebuah kesempatan lotere dengan menyelesaikan tugas.
Jika opsi lotere tidak ada lagi, rampungkan lebih banyak tugas untuk mengambil tambahan kesempatan.
Batas Imbalan:
Dapatkan keuntungan jika jumlah undi Para Pengguna lebih dari 100K dalam waktu satu hari.
Kebijakan Esensial
Pengambilan Hadiah:
Hadiah harus diterima manual dari app. Jika tidak, hadiah akan otomatis dikreditkan ke akun pribadi Kamu setelah sebuah waktu.
Peraturan Betting:
Imbalan butuh sekitar 1 bertaruh aktif untuk dimanfaatkan.
Akhir
Perangkat Lunak 888 memberikan pengalaman bermain yang menyenangkan dengan bonus besar-besaran. Unduh perangkat lunak hari ini dan nikmati keberhasilan besar-besaran pada periode!
Untuk info lebih lanjut tentang penawaran, simpanan, dan program rekomendasi, lihat halaman utama aplikasi.
https://bicrypto.exchange – crypto exchange software. White label, open-source exchange solution with a focus on a super-fast, pixel-perfect interface and robust security. High-performance platform with a robust internal architecture. Leverages the capabilities of Nuxt3 to create a cutting-edge user interface.
papaver somniferum семена чай кратом купить в челябинске
кактус сан педро купить семена семена шалфея предсказателей
айваско волжский https://travelservic.ru
augmentin 375 price india
buy generic azithromycin
mpo888
Pasang Aplikasi 888 dan Raih Bonus: Manual Praktis
**Aplikasi 888 adalah alternatif unggulan untuk Pengguna yang menginginkan permainan berjudi online yang seru dan menguntungkan. Dengan keuntungan harian dan kemampuan menggiurkan, app ini menawarkan menghadirkan keseruan berjudi paling baik. Disini manual praktis untuk memaksimalkan pemakaian Perangkat Lunak 888.
Pasang dan Awali Dapatkan
Perangkat Tersedia:
Program 888 bisa di-download di Sistem Android, iOS, dan Windows. Mulailah bertaruhan dengan praktis di gadget apa saja.
Keuntungan Harian dan Imbalan
Keuntungan Mendaftar Sehari-hari:
Login pada waktu untuk meraih bonus sebesar 100K pada waktu ketujuh.
Kerjakan Misi:
Ambil peluang pengeretan dengan menyelesaikan aktivitas terkait. Setiap misi menawarkan Para Pengguna satu opsi lotere untuk mengklaim hadiah hingga 888K.
Pengambilan Manual:
Hadiah harus diterima sendiri di melalui app. Jangan lupa untuk mengklaim bonus setiap periode agar tidak kadaluwarsa.
Cara Pengeretan
Peluang Lotere:
Setiap hari, Kamu bisa mengambil satu peluang undian dengan merampungkan pekerjaan.
Jika opsi pengeretan berakhir, selesaikan lebih banyak misi untuk mengklaim extra kesempatan.
Tingkat Keuntungan:
Klaim bonus jika keseluruhan undian Para Pengguna lebih dari 100K dalam satu hari.
Aturan Penting
Pengklaiman Keuntungan:
Imbalan harus diterima sendiri dari perangkat lunak. Jika tidak, keuntungan akan langsung diklaim ke akun pengguna Kamu setelah sebuah waktu.
Syarat Bertaruh:
Keuntungan harus ada setidaknya satu bertaruh berlaku untuk dimanfaatkan.
Ringkasan
Aplikasi 888 menyediakan keseruan berjudi yang menggembirakan dengan bonus besar-besaran. Unduh program sekarang dan alamilah hadiah signifikan tiap masa!
Untuk detail lebih rinci tentang diskon, top up, dan program rekomendasi, lihat halaman beranda app.
5 라이온스 메가웨이즈
Hongzhi 황제는 매우 기뻐했고 Li Chaowen에게 고개를 끄덕이는 것을 도울 수 없었습니다.
waktogel
Inspirasi dari Ucapan Taylor Swift
Taylor Swift, seorang penyanyi dan komposer populer, tidak hanya diakui berkat lagu yang indah dan nyanyian yang merdu, tetapi juga oleh karena syair-syair lagunya yang sarat makna. Dalam lirik-liriknya, Swift sering menggambarkan beraneka ragam unsur hidup, dimulai dari cinta sampai dengan tantangan hidup. Berikut adalah beberapa kutipan inspiratif dari lagu-lagu, bersama artinya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Penjelasan: Bahkan di saat-saat sulit, selalu ada secercah harapan dan kemungkinan akan hari yang lebih cerah.
Lirik ini dari lagu “All Too Well” membuat kita ingat bahwa meskipun kita mungkin menghadapi waktu sulit pada saat ini, selalu ada peluang bahwa waktu yang akan datang akan membawa perubahan yang lebih baik. Hal ini adalah pesan asa yang menguatkan, memotivasi kita untuk bertahan dan tidak menyerah, lantaran yang paling baik mungkin belum tiba.
“Aku akan terus bertahan karena aku tak mampu melakukan apa pun tanpa dirimu.” – “You Belong with Me”
Arti: Mendapatkan cinta dan bantuan dari orang lain dapat menyediakan kita daya dan tekad untuk melanjutkan melewati tantangan.
fiatogel
Ashley JKT48: Bintang yang Berkilau Gemilang di Langit Idol
Siapakah Ashley JKT48?
Siapakah figur belia berkemampuan yang mencuri perhatian banyak penggemar lagu di Indonesia dan Asia Tenggara? Beliau adalah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama panggungnya, Ashley JKT48. Bergabung dengan grup idola JKT48 pada tahun 2018, Ashley dengan cepat menjadi salah satu anggota paling populer.
Profil
Lahir di Jakarta pada tanggal 13 Maret 2000, Ashley berdarah keturunan Tionghoa-Indonesia. Dia mengawali kariernya di industri hiburan sebagai model dan pemeran, sebelum selanjutnya bergabung dengan JKT48. Personanya yang gembira, suara yang bertenaga, dan kemahiran menari yang mengesankan membuatnya idola yang sangat dicintai.
Penghargaan dan Pengakuan
Ketenaran Ashley telah dikenal melalui banyak penghargaan dan nominasi. Pada masa 2021, Ashley memenangkan pengakuan “Personel Terpopuler JKT48” di ajang Penghargaan Musik JKT48. Ia juga dinobatkan sebagai “Idol Terindah di Asia” oleh sebuah majalah online pada tahun 2020.
Peran dalam JKT48
Ashley menjalankan peran penting dalam grup JKT48. Ia adalah anggota Tim KIII dan berperan menjadi dancer utama dan vokalis. Ashley juga terlibat sebagai bagian dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Karier Solo
Selain kegiatan dengan JKT48, Ashley juga mengembangkan karier solo. Beliau telah meluncurkan sejumlah single, termasuk “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi dengan penyanyi lain, seperti Afgan dan Rossa.
Kehidupan Personal
Di luar dunia pertunjukan, Ashley dikenali sebagai pribadi yang rendah hati dan ramah. Beliau menikmati menghabiskan jam bersama keluarga dan teman-temannya. Ashley juga punya kesukaan melukis dan photography.
Unduh App 888 dan Raih Hadiah: Petunjuk Singkat
**Program 888 adalah opsi terbaik untuk Kamu yang membutuhkan pengalaman berjudi digital yang seru dan bermanfaat. Melalui imbalan harian dan opsi menggiurkan, app ini sedia menyediakan keseruan bertaruhan optimal. Inilah instruksi pendek untuk memanfaatkan pelayanan App 888.
Instal dan Mulai Raih
Sistem Tersedia:
Program 888 memungkinkan diinstal di Sistem Android, Perangkat iOS, dan PC. Mulai bertaruhan dengan praktis di gadget apa pun.
Keuntungan Harian dan Hadiah
Bonus Buka Tiap Hari:
Masuk setiap waktu untuk mengklaim imbalan hingga 100K pada periode ketujuh.
Rampungkan Pekerjaan:
Raih opsi undi dengan menuntaskan pekerjaan terkait. Masing-masing aktivitas menghadirkan Pengguna satu opsi undi untuk mengklaim hadiah sampai 888K.
Pengumpulan Langsung:
Bonus harus diterima manual di dalam perangkat lunak. Jangan lupa untuk mengambil bonus setiap periode agar tidak kadaluwarsa.
Prosedur Lotere
Peluang Lotere:
Tiap hari, Anda bisa mengklaim satu peluang undi dengan menuntaskan tugas.
Jika opsi undian habis, kerjakan lebih banyak misi untuk mengambil tambahan kesempatan.
Batas Hadiah:
Ambil hadiah jika keseluruhan lotere Kamu melebihi 100K dalam 1 hari.
Kebijakan Pokok
Pengambilan Bonus:
Imbalan harus diklaim langsung dari program. Jika tidak, bonus akan langsung diklaim ke akun Pengguna setelah satu hari.
Peraturan Taruhan:
Keuntungan membutuhkan setidaknya sebuah betting valid untuk digunakan.
Akhir
App 888 menyediakan pengalaman bertaruhan yang seru dengan bonus besar-besaran. Unduh aplikasi sekarang juga dan alamilah hadiah signifikan setiap masa!
Untuk detail lebih lanjut tentang promo, top up, dan sistem referensi, kunjungi situs beranda app.
купить диплом в липецке
перейти на сайт
купить свидетельство о рождении
на сайте
купить дипломы о высшем образовании цена
посмотреть сайт
купить диплом магистра
веб сайт
купить диплом колледжа
ссылка на страницу
cipit88
Ashley JKT48: Bintang yang Bercahaya Terang di Langit Idol
Siapakah Ashley JKT48?
Siapakah tokoh muda talenta yang menarik perhatian banyak sekali fans musik di Indonesia dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama bekennya, Ashley JKT48. Menjadi anggota dengan grup idola JKT48 pada masa 2018, Ashley dengan lekas berubah menjadi salah satu anggota paling populer.
Biografi
Dilahirkan di Jakarta pada tanggal 13 Maret 2000, Ashley memiliki keturunan Tionghoa-Indonesia. Dia mengawali perjalanannya di industri entertainment sebagai model dan aktris, sebelum akhirnya masuk dengan JKT48. Sifatnya yang ceria, vokal yang mantap, dan kemahiran menari yang memukau membentuknya sebagai idola yang sangat dicintai.
Penghargaan dan Pengakuan
Kepopuleran Ashley telah diapresiasi melalui berbagai penghargaan dan nominasi. Pada masa 2021, beliau memenangkan award “Anggota Paling Populer JKT48” di ajang JKT48 Music Awards. Beliau juga diberi gelar sebagai “Idol Tercantik di Asia” oleh sebuah majalah digital pada tahun 2020.
Peran dalam JKT48
Ashley memainkan fungsi utama dalam grup JKT48. Beliau adalah anggota Tim KIII dan berfungsi sebagai penari utama dan vokalis. Ashley juga merupakan member dari subunit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Perjalanan Mandiri
Selain aktivitasnya dengan JKT48, Ashley juga memulai perjalanan individu. Ia telah merilis beberapa lagu tunggal, termasuk “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi dengan artis lain, seperti Afgan dan Rossa.
Kehidupan Personal
Di luar dunia pertunjukan, Ashley dikenal sebagai orang yang rendah hati dan ramah. Ashley suka melewatkan waktu bersama sanak famili dan sahabat-sahabatnya. Ashley juga memiliki hobi mewarnai dan fotografi.
data sdy
Inspirasi dari Ucapan Taylor Swift: Harapan dan Cinta dalam Lagu-Lagunya
Taylor Swift, seorang musisi dan pengarang lagu terkenal, tidak hanya terkenal berkat melodi yang indah dan vokal yang nyaring, tetapi juga oleh karena kata-kata lagu-lagunya yang penuh makna. Pada lirik-liriknya, Swift sering melukiskan bermacam-macam faktor kehidupan, dimulai dari asmara hingga tantangan hidup. Berikut adalah beberapa petikan menginspirasi dari lagu-lagunya, beserta artinya.
“Mungkin yang terbaik belum datang.” – “All Too Well”
Makna: Bahkan di masa-masa sulit, selalu ada secercah harapan dan peluang untuk hari yang lebih baik.
Lirik ini dari lagu “All Too Well” mengingatkan kita jika meskipun kita barangkali menghadapi masa-masa sulit pada saat ini, selalu ada potensi jika masa depan akan memberikan hal yang lebih baik. Hal ini adalah pesan asa yang memperkuat, mendorong kita untuk tetap bertahan dan tidak menyerah, karena yang terhebat mungkin belum tiba.
“Aku akan tetap bertahan karena aku tidak bisa melakukan apa pun tanpamu.” – “You Belong with Me”
Arti: Menemukan asmara dan bantuan dari orang lain dapat menyediakan kita kekuatan dan tekad untuk melanjutkan lewat kesulitan.
купить диплом в челябинске
подробнее
Download Aplikasi 888 dan Raih Kemenangan: Manual Singkat
**Program 888 adalah alternatif ideal untuk Anda yang mengharapkan pengalaman bertaruhan daring yang menggembirakan dan menguntungkan. Melalui imbalan sehari-hari dan fitur memikat, aplikasi ini siap menghadirkan aktivitas bertaruhan optimal. Berikut petunjuk singkat untuk memaksimalkan penggunaan Program 888.
Download dan Awali Menang
Perangkat Terdapat:
Aplikasi 888 bisa di-download di HP Android, Perangkat iOS, dan Laptop. Mulailah main dengan praktis di gadget apa saja.
Imbalan Harian dan Imbalan
Imbalan Login Harian:
Mendaftar saban periode untuk mendapatkan bonus sampai 100K pada masa ketujuh.
Kerjakan Aktivitas:
Ambil kesempatan undian dengan menyelesaikan tugas terkait. Setiap pekerjaan menghadirkan Kamu satu kesempatan lotere untuk mengklaim keuntungan mencapai 888K.
Pengumpulan Langsung:
Keuntungan harus dikumpulkan manual di melalui app. Yakinlah untuk meraih hadiah pada hari agar tidak habis masa berlakunya.
Cara Lotere
Peluang Undian:
Masing-masing waktu, Kamu bisa meraih sebuah kesempatan undian dengan mengerjakan tugas.
Jika peluang lotere tidak ada lagi, tuntaskan lebih banyak aktivitas untuk mendapatkan extra kesempatan.
Tingkat Hadiah:
Klaim hadiah jika keseluruhan undian Kamu lebih dari 100K dalam satu hari.
Peraturan Esensial
Pengumpulan Bonus:
Hadiah harus diambil sendiri dari perangkat lunak. Jika tidak, imbalan akan langsung diambil ke akun pribadi Anda setelah satu masa.
Peraturan Taruhan:
Hadiah butuh paling tidak satu bertaruh aktif untuk diambil.
Akhir
Perangkat Lunak 888 menyediakan aktivitas main yang menggembirakan dengan imbalan signifikan. Download app hari ini dan alamilah kemenangan besar-besaran saban hari!
Untuk info lebih lengkap tentang promo, deposit, dan program undangan, cek halaman utama aplikasi.
купить аттестат http://www.6landik-diploms.com
купить диплом в нижнекамске 6landik-diploms.com
купить виниловый сайдинг сайдинг цена за м2
купить диплом в новокузнецке http://6landik-diploms.com/
сайдинг акриловый для наружной отделки акриловый сайдинг для обшивки дома цена
order bisacodyl sale – order dulcolax 5 mg sale liv52 order
rajatogel
Inspirasi dari Ucapan Taylor Swift: Harapan dan Kasih dalam Lagu-Lagunya
Taylor Swift, seorang artis dan songwriter terkemuka, tidak hanya diakui karena melodi yang indah dan suara yang merdu, tetapi juga oleh karena lirik-lirik karyanya yang penuh makna. Dalam lirik-liriknya, Swift sering melukiskan berbagai aspek hidup, mulai dari cinta hingga tantangan hidup. Berikut adalah sejumlah ucapan inspiratif dari lagu-lagunya, beserta artinya.
“Mungkin yang terhebat belum hadir.” – “All Too Well”
Arti: Bahkan di saat-saat sulit, senantiasa ada seberkas harapan dan peluang tentang hari yang lebih baik.
Syair ini dari lagu “All Too Well” menyadarkan kita jika meskipun kita barangkali berhadapan dengan masa sulit saat ini, selalu ada potensi bahwa masa depan akan membawa hal yang lebih baik. Hal ini adalah pesan harapan yang menguatkan, mendorong kita untuk bertahan dan tidak mengalah, karena yang terbaik barangkali belum datang.
“Aku akan tetap bertahan karena aku tak bisa melakukan segala sesuatu tanpa kamu.” – “You Belong with Me”
Penjelasan: Menemukan cinta dan support dari orang lain dapat menghadirkan kita kekuatan dan tekad untuk terus berjuang melewati kesulitan.
bingo4d
Ashley JKT48: Idola yang Berkilau Cemerlang di Langit Idol
Siapakah Ashley JKT48?
Siapa sosok belia berkemampuan yang menarik perhatian banyak fans lagu di Indonesia dan Asia Tenggara? Itulah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama panggungnya, Ashley JKT48. Bergabung dengan grup idola JKT48 pada tahun 2018, Ashley dengan segera muncul sebagai salah satu member paling terkenal.
Profil
Terlahir di Jakarta pada tanggal 13 Maret 2000, Ashley memiliki darah Tionghoa-Indonesia. Ia mengawali karier di dunia entertainment sebagai model dan aktris, sebelum akhirnya bergabung dengan JKT48. Sifatnya yang periang, nyanyiannya yang bertenaga, dan keterampilan menari yang mengesankan membuatnya idola yang sangat disukai.
Award dan Pengakuan
Popularitas Ashley telah diapresiasi melalui banyak penghargaan dan nominasi. Pada tahun 2021, ia memenangkan penghargaan “Member Terpopuler JKT48” di event JKT48 Music Awards. Ia juga dianugerahi sebagai “Idol Tercantik di Asia” oleh sebuah media digital pada tahun 2020.
Peran dalam JKT48
Ashley menjalankan fungsi penting dalam grup JKT48. Ia adalah anggota Tim KIII dan berperan sebagai penari utama dan vokal utama. Ashley juga merupakan anggota dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Perjalanan Mandiri
Selain aktivitasnya bersama JKT48, Ashley juga merintis karier solo. Ia telah mengeluarkan beberapa single, diantaranya “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah berkolaborasi dengan musisi lain, seperti Afgan dan Rossa.
Kehidupan Personal
Di luar bidang panggung, Ashley dikenal sebagai orang yang humble dan ramah. Ia menggemari menghabiskan masa bersama keluarga dan teman-temannya. Ashley juga memiliki kesukaan mewarnai dan fotografi.
gbo5000
Unduh App 888 dan Peroleh Besar: Panduan Singkat
**Aplikasi 888 adalah alternatif ideal untuk Anda yang membutuhkan aktivitas main daring yang menyenangkan dan berjaya. Bersama imbalan tiap hari dan fitur menarik, perangkat lunak ini menawarkan menyediakan pengalaman berjudi terbaik. Disini panduan pendek untuk memanfaatkan pemakaian Aplikasi 888.
Unduh dan Mulai Menangkan
Perangkat Tersedia:
Aplikasi 888 dapat diinstal di HP Android, iOS, dan Laptop. Mulai bertaruhan dengan mudah di gadget manapun.
Imbalan Tiap Hari dan Keuntungan
Imbalan Masuk Harian:
Login setiap waktu untuk meraih imbalan mencapai 100K pada hari ketujuh.
Tuntaskan Pekerjaan:
Dapatkan peluang pengeretan dengan menuntaskan pekerjaan terkait. Satu misi menawarkan Kamu sebuah kesempatan undian untuk mengklaim bonus hingga 888K.
Pengklaiman Mandiri:
Bonus harus diklaim langsung di dalam app. Pastikan untuk mengklaim imbalan setiap hari agar tidak kadaluwarsa.
Cara Undi
Kesempatan Undi:
Setiap waktu, Pengguna bisa mengambil sebuah peluang pengeretan dengan menyelesaikan pekerjaan.
Jika opsi pengeretan berakhir, kerjakan lebih banyak tugas untuk meraih extra peluang.
Level Keuntungan:
Klaim bonus jika akumulasi pengeretan Anda melebihi 100K dalam satu hari.
Aturan Esensial
Penerimaan Keuntungan:
Keuntungan harus diklaim mandiri dari aplikasi. Jika tidak, keuntungan akan otomatis diklaim ke akun pengguna Anda setelah satu masa.
Persyaratan Bertaruh:
Hadiah membutuhkan setidaknya 1 pertaruhan valid untuk diklaim.
Kesimpulan
Program 888 menyediakan pengalaman main yang menggembirakan dengan imbalan besar-besaran. Instal app saat ini dan nikmati kemenangan tinggi tiap hari!
Untuk info lebih rinci tentang promosi, simpanan, dan skema referensi, kunjungi page utama program.
twin casino твин казино
Online gambling sites are growing more widespread, delivering numerous incentives to attract newcomers. One of the most appealing deals is the free bonus, a promo that allows casino players to try their hand without any financial risk. This article looks into the upsides of no-deposit bonuses and emphasizes how they can increase their value.
What is a No Deposit Bonus?
A no-deposit bonus is a category of casino offer where users are granted free money or free spins without the need to invest any of their own capital. This lets gamblers to try out the online casino, test out diverse slots and potentially win real prizes, all without any upfront cost.
Advantages of No Deposit Bonuses
Risk-Free Exploration
No upfront deposit bonuses grant a secure opportunity to explore online gambling sites. Players can try diverse gaming activities, learn the casino platform, and assess the overall gameplay without investing their own funds. This is significantly useful for novices who may not be aware of online gambling sites.
Chance to Win Real Money
One of the most appealing benefits of no deposit bonuses is the chance to win real money. While the amounts may be small, any winnings secured from the bonus can often be cashed out after meeting the casino’s wagering requirements. This adds an element of thrill and offers a potential financial return without any monetary outlay.
Learning Opportunity
No upfront deposit bonuses offer a excellent means to understand how various games operate. Users can test out tactics, get to know the rules of the casino games, and grow more skilled without worrying about forfeiting their own cash. This can be particularly beneficial for challenging gaming activities like poker.
Conclusion
No deposit bonuses provide various merits for gamblers, which include risk-free investigation, the chance to earn real cash, and beneficial development chances. As the market continues to to evolve, the prevalence of no-deposit bonuses is expected to grow.
Gratis poker offers gamblers a special chance to experience the sport without any expenditure. This overview discusses the merits of playing free poker and points out why it remains favored among numerous participants.
Risk-Free Entertainment
One of the most significant merits of free poker is that it enables gamblers to enjoy the thrill of poker without being concerned with losing funds. This renders it perfect for first-timers who hope to learn the sport without any initial expenditure.
Skill Development
No-cost poker provides a excellent platform for participants to develop their competence. Participants can try approaches, learn the regulations of the game, and acquire self-assurance without any anxiety of forfeiting their own funds.
Social Interaction
Engaging in free poker can also lead to social interactions. Online platforms commonly feature chat rooms where participants can connect with each other, discuss strategies, and occasionally form friendships.
Accessibility
Free poker is readily available to all with an internet connection. This indicates that users can experience the activity from the comfort of their own place, at whenever they wish.
Conclusion
Complimentary poker presents several upsides for participants. It is a safe approach to play the sport, improve talent, participate in new friendships, and access poker conveniently. As further players experience the advantages of free poker, its demand is expected to grow.
Analyzing Promotion Casinos: A Captivating and Reachable Gaming Option
Prelude
Contest betting sites are growing into a popular choice for users looking for an captivating and authorized approach to relish virtual playing. Unlike classic online gaming hubs, promotion betting sites run under separate authorized systems, facilitating them to deliver competitions and gifts without adhering to the identical laws. This write-up analyzes the idea of sweepstakes casinos, their advantages, and why they are enticing a increasing number of participants.
Understanding Sweepstakes Casinos
A contest gaming hub functions by supplying users with online funds, which can be utilized to participate in games. Participants can achieve further digital money or tangible rewards, including currency. The key distinction from conventional gambling platforms is that users do not get coins immediately but get it through promotional campaigns, for example acquiring a item or joining in a gratis admission contest. This model allows contest gambling platforms to function lawfully in many regions where classic digital wagering is restricted.
빠른 충환전 서비스와 메이저업체의 보안성
스포츠토토사이트 사용 시 매우 중요한 부분 중 하나는 빠른 입출금 처리입니다. 일반적으로 삼 분 내에 충전하고, 열 분 안에 환충이 완수되어야 합니다. 메이저 주요업체들은 넉넉한 스태프 고용을 통해 이러한 빠른 입출금 프로세스를 보장하며, 이 방법으로 고객들에게 안전감을 제공합니다. 주요사이트를 이용하면서 빠른 체험을 즐겨보세요. 우리는 여러분이 안심하고 웹사이트를 접속할 수 있도록 지원하는 먹튀해결사입니다.
보증금을 걸고 배너를 운영
먹튀 해결 전문가는 적어도 3000만 원에서 억대의 보증 금액을 예치한 업체들의 배너를 운영합니다. 만일 먹튀 사고가 발생할 경우, 배팅 규정에 위배되지 않은 베팅 내역을 캡처하여 먹튀 해결 전문가에게 문의 주시면, 확인 후 보증금으로 신속하게 손해 보상을 처리합니다. 피해가 발생하면 즉시 캡처해서 손해 내용을 기록해두시고 제출해 주세요.
장기간 안전 운영 업체 확인
먹튀해결사는 적어도 4년 이상 먹튀 사고 없이 안전하게 운영하고 있는 사이트들을 인증하여 배너 등록을 받고 있습니다. 이로 인해 모두가 잘 알려진 대형사이트를 안전하게 이용할 수 있는 기회를 제공하고 있습니다. 엄격한 검증 절차를 통해 검증된 사이트를 놓치지 말고, 보안된 도박을 체험해보세요.
투명하고 공정한 먹튀 검토
먹튀해결사의 먹튀 확인은 공정성과 공정을 근거로 실시합니다. 항상 고객들의 의견을 우선으로 생각하고, 사이트의 이익이나 이익에 흔들리지 않고 1건의 삭제 없이 사실만을 바탕으로 검증해왔습니다. 먹튀 피해를 겪고 후회하지 않도록, 지금 바로 시작해보세요.
먹튀 검증 사이트 목록
먹튀 해결 전문가가 골라낸 안전한 토토사이트 검증업체 목록 입니다. 지금 등록된 검증된 업체들은 먹튀 사고 발생 시 100% 보증을 해드립니다. 하지만, 제휴 기간이 끝난 업체에서 발생한 피해에 대해서는 책임지지 않습니다.
탁월한 먹튀 검증 알고리즘
먹튀 해결 전문가는 공정한 베팅 문화를 만들기 위해 계속해서 노력하고 있습니다. 저희는 추천하는 스포츠토토사이트에서 안전하게 배팅하세요. 사용자의 먹튀 제보는 먹튀 리스트에 등록 노출되어 그 해당 스포츠토토 사이트에 심각한 영향을 줄 수 있습니다. 먹튀 목록 작성 시 먹튀블러드의 검증 지식을 최대로 사용하여 공평한 심사를 할 수 있게 하겠습니다.
안전한 도박 환경을 만들기 위해 계속해서 힘쓰는 먹튀해결사와 동반하여 안전하게 즐기시기 바랍니다.
casino online
Discovering the Universe of Internet Casinos
Start
In the digital age, casino online have revolutionized the way users enjoy gaming. With sophisticated digital advancements, gamblers can access their chosen games right from the coziness of their residences. This piece investigates the benefits of virtual casinos and as to why they are drawing popularity.
Perks of Virtual Casinos
Accessibility
One of the main benefits of online casinos is convenience. Enthusiasts can play anytime and wherever they are they prefer, doing away with the requirement to travel to a traditional gambling venue.
Large Game Library
Online casinos give a extensive selection of casino games, ranging from vintage one-armed bandits and board games to live-action games and modern slot machines. This array guarantees that there is an activity for every kind of gambler.
Perks and Specials
One of the most appealing aspects of virtual casinos is the range of rewards and promotions offered to players. These can encompass welcome bonuses, free spins, rebate offers, and player clubs.
Protection and Assurance
Trusted casino online make sure player protection and reliability with cutting-edge security techniques. This protects personal credentials and payment transactions.
Motives Behind the Popularity of Internet Casinos
Attainability
Casino online are commonly available, facilitating enthusiasts from numerous regions to enjoy gaming.
казино онлайн сайт твин казино
Unveiling Free Casino Games
Beginning
Today, complimentary casino games have grown into a popular selection for casino lovers who desire to experience casino activities without using finances. This piece investigates the advantages of complimentary casino games and the causes they are attracting interest.
Perks of Free-of-Charge Casino Games
No-Risk Gaming
One of the major perks of free-of-charge casino games is the ability to gamble minus monetary loss. Gamblers can experience their favorite gaming options free from worrying about wasting money.
Learning Opportunities
Complimentary casino games offer an ideal environment for gamblers to refine their talents. Whether it is understanding tactics in blackjack, gamblers can work on free from financial consequences.
Large Game Library
No-cost casino games provide a wide array of games, including classic slot machines, casino classics, and interactive games. This diversity guarantees that there is an activity for everyone.
Why Many Players Prefer Free Casino Games
Attainability
Complimentary casino games are extensively reachable, permitting players from various regions to engage in betting.
No Monetary Obligation
Unlike money-based gaming, free casino games do not need a monetary investment. This facilitates gamblers to experience betting free from worrying about losing funds.
Test Before Betting
Free-of-charge casino games provide gamblers the ability to experience games in advance of putting down actual finances. This aids enthusiasts create informed selections.
Closing
Free-of-charge casino games provides a enjoyable and safe way to engage in betting. With no financial risk, diverse game options, and opportunities for game mastery, it is not surprising that countless enthusiasts choose free casino games for their playing preferences.
Unveiling Money Slots
Beginning
Real money slots have become a preferred choice for players wanting the rush of winning actual cash. This write-up explores the pros of money slots and the reasons they are attracting increasing enthusiasts.
Pros of Money Slots
Genuine Rewards
The major appeal of real money slots is the chance to gain actual money. Unlike free-of-charge slots, gambling slots offer users the thrill of potential monetary payouts.
Large Game Selection
Real money slots offer a broad range of genres, elements, and payout structures. This guarantees that there is an activity for all types of players, ranging from vintage three-reel slots to state-of-the-art digital slots with numerous winning lines and bonus features.
Attractive Offers
Various web-based casinos supply enticing bonuses for gambling slot users. These can include joining bonuses, complimentary spins, refund deals, and rewards programs. Such incentives improve the general playing activity and provide extra chances to win cash.
Motivations for Opting for Money Slots
The Adrenaline of Gaining Genuine Funds
Gambling slots give an adrenaline-filled activity, as enthusiasts await the possibility of gaining tangible cash. This characteristic injects a significant layer of adrenaline to the gameplay journey.
Instant Gratification
Real money slots give users the gratification of prompt payouts. Winning currency promptly improves the betting activity, rendering it more fulfilling.
Wide Game Selection
Including gambling slots, gamblers can experience a wide selection of games, assuring that there is always something new to try.
Closing
Real money slots offers a thrilling and gratifying playing adventure. With the possibility to win actual cash, a broad range of slot games, and thrilling bonuses, it’s understandable that many players favor gambling slots for their playing choices.
казино онлайн Twin Casino официальный
купить сайдинг для дома сайдинг для дома цена
хамон цена хамон москва
говядина брезаола https://messir-zakaz.ru
Все самое интересное из мира игр https://unionbattle.ru обзоры, статьи и ответы на вопросы
хамон москва хамон купить в москве
coloktoto
Ashley JKT48: Bintang yang Bersinar Gemilang di Langit Idol
Siapakah Ashley JKT48?
Siapa sosok belia berbakat yang menarik perhatian sejumlah besar penggemar musik di Indonesia dan Asia Tenggara? Dialah Ashley Courtney Shintia, atau yang lebih dikenal dengan nama bekennya, Ashley JKT48. Masuk dengan grup idola JKT48 pada masa 2018, Ashley dengan lekas menjadi salah satu member paling populer.
Biografi
Lahir di Jakarta pada tgl 13 Maret 2000, Ashley memiliki darah Tionghoa-Indonesia. Ia mengawali kariernya di industri hiburan sebagai model dan pemeran, sebelum akhirnya masuk dengan JKT48. Sifatnya yang ceria, vokal yang kuat, dan kemahiran menari yang mengagumkan membentuknya sebagai idola yang sangat dicintai.
Award dan Pengakuan
Ketenaran Ashley telah diakui melalui banyak penghargaan dan nominasi. Pada masa 2021, ia memenangkan pengakuan “Personel Terpopuler JKT48” di ajang Penghargaan Musik JKT48. Ashley juga dinobatkan sebagai “Idol Tercantik di Asia” oleh sebuah media digital pada masa 2020.
Peran dalam JKT48
Ashley memainkan peran penting dalam group JKT48. Beliau adalah personel Tim KIII dan berperan menjadi penari utama dan penyanyi utama. Ashley juga menjadi anggota dari sub-unit “J3K” bersama Jessica Veranda dan Jennifer Rachel Natasya.
Perjalanan Solo
Selain aktivitasnya bersama JKT48, Ashley juga mengembangkan karier solo. Ia telah merilis beberapa lagu single, antara lain “Myself” (2021) dan “Falling Down” (2022). Ashley juga telah bekerjasama dengan musisi lain, seperti Afgan dan Rossa.
Kehidupan Privat
Selain kancah panggung, Ashley dikenal sebagai pribadi yang low profile dan friendly. Ia suka menghabiskan waktu dengan keluarga dan sahabat-sahabatnya. Ashley juga memiliki kegemaran melukis dan memotret.
danagg
Pasang Aplikasi 888 dan Dapatkan Kemenangan: Manual Pendek
**Aplikasi 888 adalah alternatif ideal untuk Kamu yang mengharapkan permainan main daring yang menggembirakan dan bernilai. Dengan bonus sehari-hari dan opsi menggoda, program ini sedia menghadirkan pengalaman bertaruhan paling baik. Ini panduan cepat untuk memaksimalkan pemanfaatan Aplikasi 888.
Download dan Awali Raih
Perangkat Tersedia:
Program 888 dapat diambil di Android, Sistem iOS, dan Laptop. Awali berjudi dengan mudah di gadget apa saja.
Hadiah Harian dan Imbalan
Hadiah Masuk Tiap Hari:
Masuk tiap masa untuk mengambil bonus sampai 100K pada waktu ketujuh.
Selesaikan Pekerjaan:
Raih opsi pengeretan dengan menuntaskan tugas terkait. Setiap misi memberi Pengguna 1 kesempatan pengeretan untuk meraih bonus sebesar 888K.
Penerimaan Mandiri:
Imbalan harus diklaim mandiri di dalam app. Jangan lupa untuk meraih bonus tiap waktu agar tidak habis masa berlakunya.
Cara Undi
Kesempatan Undi:
Satu waktu, Kamu bisa meraih 1 peluang undian dengan merampungkan tugas.
Jika kesempatan pengeretan tidak ada lagi, kerjakan lebih banyak misi untuk mengambil tambahan opsi.
Tingkat Keuntungan:
Klaim imbalan jika total lotere Pengguna melampaui 100K dalam sehari.
Ketentuan Penting
Pengambilan Hadiah:
Hadiah harus dikumpulkan sendiri dari program. Jika tidak, imbalan akan otomatis dikreditkan ke akun Para Pengguna setelah sebuah waktu.
Ketentuan Taruhan:
Keuntungan membutuhkan sekitar 1 taruhan efektif untuk dimanfaatkan.
Kesimpulan
Perangkat Lunak 888 menghadirkan pengalaman bertaruhan yang seru dengan bonus tinggi. Instal program sekarang juga dan rasakan keberhasilan besar setiap hari!
Untuk detail lebih lanjut tentang diskon, deposit, dan program undangan, cek laman beranda app.
eurotogel
Inspirasi dari Kutipan Taylor Swift: Harapan dan Kasih dalam Lagu-Lagunya
Taylor Swift, seorang musisi dan komposer terkenal, tidak hanya dikenal karena nada yang elok dan nyanyian yang nyaring, tetapi juga oleh karena lirik-lirik lagu-lagunya yang penuh makna. Di dalam lirik-liriknya, Swift sering menggambarkan berbagai faktor kehidupan, dimulai dari cinta sampai dengan rintangan hidup. Berikut ini adalah beberapa kutipan inspiratif dari lagu-lagu, bersama artinya.
“Mungkin yang paling baik belum tiba.” – “All Too Well”
Arti: Bahkan di masa-masa sulit, tetap ada seberkas asa dan kemungkinan akan hari yang lebih baik.
Syair ini dari lagu “All Too Well” membuat kita ingat bahwa meskipun kita mungkin menghadapi masa sulit saat ini, selalu ada kemungkinan bahwa masa depan akan memberikan sesuatu yang lebih baik. Ini adalah pesan pengharapan yang menguatkan, mendorong kita untuk bertahan dan tidak menyerah, karena yang terhebat mungkin belum datang.
“Aku akan tetap bertahan karena aku tak mampu melakukan apa pun tanpamu.” – “You Belong with Me”
Arti: Menemukan kasih dan dukungan dari orang lain dapat menghadirkan kita kekuatan dan tekad untuk terus berjuang melalui kesulitan.
Virtual casinos are steadily more popular, offering different bonuses to attract new users. One of the most tempting deals is the free bonus, a promotion that lets players to try their luck without any initial deposit. This overview discusses the upsides of no deposit bonuses and underscores how they can increase their effectiveness.
What is a No Deposit Bonus?
A no upfront deposit bonus is a kind of casino campaign where users receive free cash or free spins without the need to submit any of their own capital. This enables users to explore the casino, test out different gaming activities and stand a chance to win real prizes, all without any initial investment.
Advantages of No Deposit Bonuses
Risk-Free Exploration
Free bonuses give a secure option to try out virtual casinos. Gamblers can try multiple games, understand the casino’s interface, and judge the overall playing environment without spending their own cash. This is significantly beneficial for beginners who may not be used to virtual casinos.
Chance to Win Real Money
One of the most attractive benefits of no-deposit bonuses is the possibility to win real money. Although the amounts may be limited, any gains obtained from the bonus can generally be redeemed after meeting the casino’s staking criteria. This adds an element of fun and offers a likely financial reward without any initial cost.
Learning Opportunity
Free bonuses provide a great way to get to know how multiple games are played. Participants can practice methods, grasp the mechanics of the slots, and become more proficient without being concerned about forfeiting their own cash. This can be especially useful for complex casino options like poker.
Conclusion
No upfront deposit bonuses give numerous advantages for participants, such as safe discovery, the opportunity to obtain real winnings, and useful development experiences. As the field keeps to expand, the prevalence of no deposit bonuses is likely to increase.
free poker
Free poker gives gamblers a distinct chance to partake in the sport without any financial risk. This write-up discusses the advantages of engaging in free poker and highlights why it is well-liked among countless players.
Risk-Free Entertainment
One of the biggest merits of free poker is that it permits users to enjoy the fun of poker without worrying about losing capital. This renders it perfect for first-timers who wish to familiarize themselves with the game without any initial expenditure.
Skill Development
Free poker presents a wonderful platform for players to improve their competence. Users can experiment with methods, understand the mechanics of the game, and gain confidence without any anxiety of losing their own capital.
Social Interaction
Engaging in free poker can also result in social interactions. Internet-based venues commonly offer interactive spaces where players can engage with each other, discuss tips, and sometimes build relationships.
Accessibility
Gratis poker is easy to access to all with an network connection. This means that users can play the sport from the ease of their own homes, at any hour.
Conclusion
Free poker provides numerous merits for users. It is a cost-free way to play the sport, hone competence, experience networking opportunities, and engage with poker conveniently. As greater gamblers discover the merits of free poker, its demand is likely to increase.
Exploring the Domain of Online Casinos
Start
In contemporary times, internet casinos have altered the manner people play gambling. With advanced tech, users can play their chosen betting activities right from the coziness of their residences. This write-up examines the perks of online casinos and for which they are amassing popularity.
Benefits of Online Casinos
Comfort
One of the key advantages of virtual casinos is convenience. Players can engage in gaming at any time and at any place they wish, ending the requirement to move to a land-based casino.
Wide Variety of Games
Online casinos supply a wide array of casino games, including traditional slot machines and table games to interactive games and cutting-edge video slots games. This selection guarantees that there is a game for all types of players.
Bonuses and Promotions
Among the key luring aspects of virtual casinos is the array of incentives and specials available to users. These can encompass registration bonuses, free spins, money-back deals, and rewards programs.
Security and Reliability
Reputable casino online make sure user safety and protection with state-of-the-art data protection methods. This secures individual data and banking transactions.
Reasons Players Choose Online Casinos
Attainability
Casino online are extensively available, permitting gamblers from various locations to engage in gambling.
빠른 충환전 서비스와 더불어 주요업체의 보안성
토토사이트 이용 시 핵심적인 부분 중 하나는 빠른 환충 프로세스입니다. 보통 3분 안에 충전, 열 분 내에 환전이 완료되어야 합니다. 메이저 대형업체들은 필요한 인력 채용을 통해 이 같은 빠릿한 충환전 절차를 약속하며, 이로써 회원들에게 안전감을 드립니다. 대형사이트를 이용하면서 신속한 체감을 해보세요. 저희는 여러분들이 안심하고 사이트를 이용할 수 있도록 지원하는 먹튀 해결 팀입니다.
보증금 걸고 배너를 운영
먹튀 해결 팀은 적어도 3000만 원에서 일억 원의 보증 금액을 예치한 회사들의 배너 광고를 운영 중입니다. 만약 먹튀 문제가 발생할 경우, 배팅 규정에 반하지 않은 배팅 기록을 캡처하여 먹튀 해결 전문가에게 연락 주시면, 사실 확인 후 보증금으로 빠르게 손해 보상을 처리합니다. 피해 발생 시 신속하게 캡처하여 피해 내용을 저장해 두시고 제출해 주세요.
오랫동안 안전하게 운영된 업체 확인
먹튀 해결 팀은 최대한 사 년 이상 먹튀 이력 없이 무사히 운영하고 있는 사이트만을 검증하여 배너 등록을 받고 있습니다. 이 때문에 모두가 잘 알려진 메이저사이트를 안심하고 접속할 수 있는 기회를 제공합니다. 엄격한 검증 작업을 통해 검증된 사이트를 놓치지 말고, 보안된 베팅을 즐겨보세요.
투명하고 공정한 먹튀 검증
먹튀 해결 팀의 먹튀 확인은 투명성과 정확함을 바탕으로 실시합니다. 늘 고객들의 입장을 우선시하며, 업체의 이익이나 이득에 흔들리지 않으며 1건의 삭제 없이 사실만을 근거로 검증해오고 있습니다. 먹튀 피해를 당하고 후회하지 않도록, 지금 바로 시작해보세요.
먹튀 검증 사이트 목록
먹튀해결사가 골라낸 안전한 베팅사이트 검증된 업체 목록 입니다. 현재 등록되어 있는 인증된 업체들은 먹튀 사고 발생 시 100% 보증을 제공해드립니다. 그러나, 제휴 기간이 만료된 업체에서 발생한 피해에 대해서는 책임을 지지 않습니다.
유일무이한 먹튀 검증 알고리즘
먹튀해결사는 깨끗한 도박 문화를 형성하기 위해 항상 애쓰고 있습니다. 우리가 추천하는 스포츠토토사이트에서 안전하게 베팅하시기 바랍니다. 회원님의 먹튀 신고는 먹튀 목록에 기재되어 해당 토토사이트에 중대한 영향을 줄 수 있습니다. 먹튀 리스트를 작성할 때 먹튀블러드 만의 검증 지식을 최대한 활용하여 공정한 심사를 할 수 있게 하겠습니다.
안전한 베팅 환경을 만들기 위해 항상 힘쓰는 먹튀해결사와 함께 안전하게 경험해보세요.
sweepstakes casino
Analyzing Lottery Casinos: An Engaging and Available Gaming Alternative
Introduction
Lottery casinos are transforming into a preferred option for users desiring an captivating and lawful approach to enjoy virtual betting. Unlike conventional digital betting sites, lottery casinos run under different lawful structures, enabling them to provide competitions and prizes without falling under the equivalent guidelines. This write-up analyzes the principle of contest casinos, their benefits, and why they are attracting a rising number of participants.
Defining Sweepstakes Casinos
A lottery gambling platform functions by offering users with online currency, which can be employed to participate in games. Users can win extra online coins or physical gifts, such as cash. The fundamental variation from traditional casinos is that gamers do not acquire money straightforwardly but acquire it through promotional activities, including get a product or engaging in a no-cost admission contest. This model enables promotion casinos to function legitimately in many areas where classic online betting is restricted.
Unveiling Complimentary Casino Games
Start
Today, no-cost casino games have become a favored selection for gamers who desire to experience gambling minus spending cash. This article explores the pros of complimentary casino games and the reasons they are gaining favor.
Benefits of Free Casino Games
Risk-Free Gaming
One of the major perks of free casino games is the possibility to bet free from financial strain. Users can play their beloved games without worrying about misplacing cash.
Learning Opportunities
Free-of-charge casino games provide an excellent environment for users to hone their gaming proficiency. Regardless of practicing techniques in slots, enthusiasts can train devoid of financial consequences.
Large Game Library
No-cost casino games give a vast selection of casino games, such options as vintage one-armed bandits, casino classics, and live dealer games. This diversity guarantees that there is a game for every kind of gambler.
Why Many Players Prefer Free Casino Games
Availability
Free-of-charge casino games are broadly available, permitting gamblers from diverse walks of life to experience gambling.
No Monetary Obligation
Unlike financial casino games, complimentary casino games do not require a monetary investment. This enables gamblers to engage in gaming devoid of fretting over losing finances.
Sample Before Spending
Free-of-charge casino games provide gamblers the opportunity to test games before spending real cash. This enables gamblers craft well-thought-out judgments.
Closing
Complimentary casino games gives a entertaining and safe means to experience casino games. With zero monetary obligation, extensive game choices, and possibilities for game mastery, it is clear that many enthusiasts like free casino games for their betting requirements.
real money slots
Unveiling Cash Slots
Introduction
Gambling slots have turned into a favored alternative for casino enthusiasts looking for the excitement of earning genuine currency. This write-up examines the perks of gambling slots and the motivations they are drawing a rising number of enthusiasts.
Pros of Money Slots
Actual Payouts
The primary attraction of real money slots is the chance to gain real currency. As opposed to free slots, gambling slots give gamblers the thrill of probable financial rewards.
Extensive Game Variety
Cash slots offer a wide array of genres, attributes, and earnings frameworks. This makes sure that there is something for all types of players, ranging from classic classic 3-reel slots to up-to-date digital slots with multiple winning lines and special bonuses.
Exciting Bonuses and Promotions
Countless online casinos give exciting rewards for gambling slot gamblers. These can consist of initial offers, extra spins, money-back deals, and rewards programs. Such promotions improve the total gambling journey and offer extra possibilities to earn currency.
Why Enthusiasts Enjoy Gambling Slots
The Thrill of Winning Real Money
Money slots provide an adrenaline-filled experience, as enthusiasts look forward to the opportunity of securing tangible money. This characteristic injects another degree of thrill to the gameplay adventure.
Immediate Rewards
Real money slots provide users the gratification of quick payments. Winning cash promptly increases the betting journey, turning it more gratifying.
Diverse Game Options
Featuring real money slots, players can experience a diverse variety of slot games, guaranteeing that there is always an activity different to experience.
Closing
Cash slots supplies a exhilarating and satisfying betting adventure. With the opportunity to secure actual funds, a wide range of slot games, and attractive promotions, it’s clear that countless players favor gambling slots for their gaming requirements.
clomid 50 mg
безопасно,
Современное оборудование и материалы, для поддержания здоровья рта,
Современные методы стоматологии, для вашего удобства,
Индивидуальный подход к каждому пациенту, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего комфорта и уверенности,
Индивидуальный план лечения и профилактики, для вашего комфорта и удовлетворения,
Заботливое отношение и внимательный подход, для вашего комфорта и удовлетворения
лікування зубів дітям лікування зубів дітям .
гарантированно,
Лучшие стоматологи города, для поддержания здоровья рта,
Современные методы стоматологии, для вашего удобства,
Комфортные условия и дружественный персонал, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего долгосрочного удовлетворения,
Профессиональная гигиена полости рта, для вашего здоровья и уверенности в себе,
Индивидуальный план лечения для каждого пациента, для вашего комфорта и удовлетворения
протезування зубів протезування зубів .
купить диплом в казани https://6landik-diploms.com/
квартиры от застройщика цены https://kupit-kvartiruekb.ru
купить диплом колледжа http://6landik-diploms.com
купить диплом о среднем образовании http://www.6landik-diploms.com/
bactrim 480mg cheap – generic levetiracetam tobrex 5mg cheap
бизнес такси вызвать такси в новочеркасске
заказать такси эконом https://taxi-vyzvat.ru
Trial your lyrical acquaintance with https://sites.google.com/view/heardle-unlimited-guide/, an agreeable trivia heroic where you label songs from enlighten audio clips. Featuring a variation of genres and difficulty levels, it offers a pastime and competitive sophistication fitted all music lovers. Find out how scads songs you can accept and recover your skills!
Pro88
buy zovirax no prescription – order duphaston 10 mg generic buy generic dydrogesterone
flomax glaucoma
buy zovirax medication – cerazette cost buy dydrogesterone generic
Pro88
Pro88
buy furosimide
albuterol atrovent
Советы по стратегии продвижения сайтов продвижению.
Информация о том как работать с низкочастотными запросами запросами и как их выбирать
Подход по работе в конкурентоспособной нише.
Имею постоянных сотрудничаю с 3 фирмами, есть что рассказать.
Посмотрите мой профиль, на 31 мая 2024г
число завершённых задач 2181 только здесь.
Консультация проходит в устной форме, без снимков с экрана и отчётов.
Длительность консультации указано 2 ч, но по сути всегда на связи без твердой фиксации времени.
Как работать с ПО это уже другая история, консультация по работе с программами договариваемся отдельно в другом кворке, выясняем что нужно при коммуникации.
Всё без суеты на расслабоне не в спешке
To get started, the seller needs:
Мне нужны контакты от Telegram канала для коммуникации.
разговор только устно, общаться письменно не хватает времени.
Суббота и Вс выходной
cotrimoxazole price – cotrimoxazole 480mg price buy tobrex 5mg
купить диплом в омске https://6landik-diploms.com
купить диплом техника https://6landik-diploms.com
buy cheap forxiga – buy doxepin no prescription order precose 50mg online cheap
Euro 2024
заказ такси в новочеркасске https://taxi-novocherkassk.ru/
заказать машину такси https://zakaz-taxionline.ru/
такси эконом https://taxi-novocherkassk.ru/
эффективно,
Современное оборудование и материалы, для вашего уверенного улыбки,
Профессиональное лечение и консультации, для вашей улыбки,
Комфортные условия и дружественный персонал, для вашего комфорта и уверенности,
Инновационные методы стоматологии, для вашего здоровья и красоты улыбки,
Индивидуальный план лечения и профилактики, для вашего долгосрочного удовлетворения,
Индивидуальный план лечения для каждого пациента, для вашего здоровья и благополучия
лікування зубів https://stomatologichnaklinikafghy.ivano-frankivsk.ua/ .
горячая линия такси https://zakaz-taxionline.ru/
Ищете способ расслабиться и получить незабываемые впечатления? Мы https://t.me/intim_tmn72 предлагаем эксклюзивные встречи с привлекательными и профессиональными компаньонками. Конфиденциальность, комфорт и безопасность гарантированы. Позвольте себе наслаждение и отдых в приятной компании.
Хотите быть в курсе всех актуальных тем в мире недвижимости?
На нашем ресурсе вы найдете множество полезных статей о налогах на недвижимость, а также о ипотеке на недвижимость.
Узнайте все, что вам нужно для успешных сделок и принятия важных решений в области недвижимости.
https://prestizh-stroi.ru
Ищете способ расслабиться и получить незабываемые впечатления? Мы https://t.me/intim_tmn72 предлагаем эксклюзивные встречи с привлекательными и профессиональными компаньонками. Конфиденциальность, комфорт и безопасность гарантированы. Позвольте себе наслаждение и отдых в приятной компании.
На нашем сайте вы найдете все необходимые сведения о недвижимости – от бронирования жилья в новостройке до покупки недвижимости от застройщика.
Мы поможем вам выбрать идеальную квартиру на вторичном рынке, расскажем, как не попасть в ловушку при выборе жилья и подскажем, как сэкономить на покупке.
Наш сайт: https://quartz-rsk.ru
купить аттестат за 9 класс https://6landik-diploms.com
купить диплом в твери https://6landik-diploms.com
купить диплом фармацевта https://6landik-diploms.com
vong lo?i euro 2024
купить диплом в волжском https://6landik-diploms.com
트레져스 오브 아즈텍
이때 병상에서 류지에가 기침을 했다.
buy generic griseofulvin – dipyridamole online buy lopid usa
order fulvicin 250mg sale – lopid 300 mg pill where can i buy lopid
ventolin cream
Хотите узнать всё о процессе оформления квартиры в новостройке?
Наш ресурс предлагает вам самые актуальные статьи на тему покупки и продажи недвижимости.
Здесь вы найдете ответы на все интересующие вас вопросы и получите подробную информацию о процессе регистрации жилья.
https://krovlistroy.ru/
https://aisory.tech – платформа для создания AI Telegram-ботов. Наделяйте своих ботов способностями к естественному диалогу, генерации уникального контента и решению аналитических задач. Простой конструктор платформы делает создание умных чат-ботов доступным для любой компании.
купить квартиру от застройщика недорого купить квартиру недорого
vardenafil tablets 20mg
tadalafil and alcohol side effects
жк казань купить квартиру https://kupit-kvartirukzn.ru
жк купить квартиру от застройщика https://kupit-kvartirukzn.ru
купить квартиру в новостройке от застройщика https://kvartiru-kupit-kzn.ru
купить квартиру недорого https://nedvizhimost16.ru
жк казань купить квартиру от застройщика https://kvartiru-kupit-kzn.ru
жк купить квартиру от застройщика https://nedvizhimost16.ru
https://kollalab.ca/demo-slot
купить квартиру от застройщика цены https://kvartiru-kupit-kzn.ru
купить квартиру в казани https://nedvizhimost16.ru
medicine clomid 50mg
атака титанов онлайн https://ataka-titanov-anime.ru
vòng loại euro 2024
how much is azithromycin
accutane in uk
смотреть аниме атака титанов смотреть атака титанов в хорошем качестве
https://theflooringfactory.ca/nanastoto
forxiga 10mg brand – buy generic sinequan 25mg cost acarbose
атака титанов в хорошем качестве https://ataka-titanov-anime.ru
Лучшие модели колясок Cybex на рынке, в магазине.
Лучшие оферты на коляски Cybex, для истинных ценителей качества.
Почему стоит обратить внимание на коляски Cybex, которые заставят вас влюбиться в этот бренд.
Коляска Cybex: безопасность и стиль в одном флаконе, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашей семьи, учитывая все особенности и пожелания.
Как правильно подобрать коляску Cybex для вашей семьи, исходя из индивидуальных потребностей и предпочтений.
Почему коляски Cybex так популярны среди родителей, которые ценят комфорт и безопасность.
Идеальная коляска Cybex для вашего малыша: как выбрать, которые порадуют вас своим разнообразием и качеством.
5 важных критериев при выборе коляски Cybex, для вашего малыша.
Выбор коляски Cybex: что важно знать перед покупкой, чтобы сделать правильный выбор.
Коляска Cybex: стиль, комфорт и безопасность, которые не оставят вас равнодушными.
Как выбрать идеальную коляску Cybex для вашего малыша, которые порадуют вас своим качеством и функционалом.
Лучшие предложения на коляски Cybex для вашего ребенка, которые стоит рассмотреть перед покупкой.
Почему стоит выбрать именно коляски Cybex, если вы цените качество и комфорт.
Лучшие модели колясок Cybex: подробный обзор, которые ценят надежность и стиль.
Как выбрать идеальную коляску Cybex для вашего малыша: подробный гид, перед совершением покупки.
Топ-5 лучших моделей колясок Cybex, исходя из личных предпочтений и потребностей.
Как выбрать идеальную коляску Cybex для вашего малыша: главные моменты, которые не оставят вас равнодушными.
прогулочная коляска cybex прогулочная коляска cybex .
атака титанов смотреть онлайн смотреть аниме атака титанов
In the ready heardle unlimited, you listen to brief snippets of songs and tax to estimate the titles. As you at work, the clips accede to longer to help you turn over a complete accurate guesses. This regatta blends music trivia with a joy, interactive size, contribution infinite entertainment allowing for regarding music enthusiasts.
мягкая мебель купить
https://formomebel.ru/stoliki/na-osnovanii-iz-metalla
атака титанов смотреть онлайн атака титанов онлайн бесплатно
купить мебель с доставкой
https://formomebel.ru/stoliki/metallicheskie
娛樂城官網
娛樂城官網
what online casino pays out the most online casino
how to become an online casino agent gaming bets
what online casino pays real money gaming bets
Hi all!
The Lido Advantage: Earn More with 25% Monthly Staking Returns! Blockchain Returns/url]
In the rapidly evolving world of cryptocurrencies, many projects promise high returns and innovative solutions. Yet, Lido sets itself apart with particularly attractive conditions. This project allows investors to stake their assets and earn up to 25% profit per month from their deposits. If you’re looking to grow your capital, investing in Lido could be a smart move. Lido is committed to providing a high level of reliability and transparency for its investors. All operations are conducted through smart contracts on the Ethereum blockchain, ensuring the security and integrity of the invested funds. Regular security audits further reassure users of Lido’s dependability. One of the main benefits of Lido is the high returns that can be achieved through token staking. With potential yields reaching up to 25% per month, Lido is one of the most attractive projects in the cryptocurrency market. This high return rate allows investors to see substantial capital growth in a short period if they use this tool correctly. Lido is designed to be simple and user-friendly, making it accessible even for beginners. Investors can easily join the platform, lock their tokens, and start earning profits within minutes. There is no need for a complex setup or technical skills—just an Ethereum wallet and a bit of ETH for gas fees. Lido is also a project that is continually evolving and expanding. It offers new opportunities and tools for its users, with the project team actively working on platform improvements and adding new features to meet user needs and stay ahead in the industry. Investing in Lido is not just about making money; it’s also about being part of an innovative project that is reshaping the cryptocurrency landscape. Start staking your tokens today with Lido and enjoy high returns.
For more information please visit https://crypto-airdrops.org
Wish you profit and prosperity)
Lido Finance
Crypto Market
Staking Knowledge
Blockchain Technology
Staking Education
голяк онлайн бесплатно в хорошем https://golyak-serial-online.ru
голяк кубик в кубе онлайн https://golyak-serial-online.ru
голяк смотреть онлайн бесплатно в хорошем качестве https://golyak-serial-online.ru
голяк кубик в кубе смотреть сериал голяк
vasotec generic – pill enalapril buy latanoprost eye drops
Здравствуйте!
Недавно у меня возникла потребность в получении среднего образования, но постоянная работа и обязанности постоянно отнимают время, и у меня нет возможности этим заниматься. К моему счастью, друзья посоветовали мне, что можно легально приобрести диплом о среднем профессиональном образовании (диплом техникума, колледжа) на бланках государственного образца, пройдя обучение по упрощенной программе!
В интернете полно предложений, но как избежать мошенничества и выбрать подходящую компанию? Это весьма важный вопрос, который требует ответственного подхода. Я лично проверил, что на http://russa24-diploms-srednee.com содержится множество советов о том, как избежать ошибок и не потерять деньги зря. Как проверить компанию по продаже дипломов, на что обратить внимание, и конечно, там можно заказать диплом “под ключ” без предварительной оплаты.
В отличие от других коммерческих организаций, наша цель — не просто заработать, а помочь нашим клиентам. Мы предоставляем бесплатные консультации без ограничений по количеству вопросов. Наши специалисты — проверенные временем профессионалы, поэтому обращение к нам – верное решение, ведь мы гарантируем качество, соблюдение сроков и разумные цены на дипломы о среднем образовании на заказ.
Удачи и хороших оценок!
купить диплом о среднем образовании в улан удэ
диплом купить о среднем образовании недорого
диплом о среднем общем образовании купить
среднее профессиональное образование купить диплом
купить дипломы в спб о среднем образовании
купить диплом среднее специальное образование
среднее медицинское образование диплом купить
куплю оригинальный диплом о среднем специальном образовании
купить диплом о среднем образовании в санкт петербурге
где купить диплом о среднем специальном образовании
смотреть голяк куб в кубе голяк смотреть онлайн бесплатно
아리아나 슬롯
Xiao Jing, Liu Jian 및 다른 사람들은 모두 당황하여 Hongzhi 황제를 바라 보았습니다.
голяк кубик онлайн https://golyak-serial-online.ru
атака титанов смотреть онлайн бесплатно – эпический аниме-сериал, где человечество борется за выживание в мире, наполненном гигантскими титанами. Динамичные бои, захватывающий сюжет и глубокие персонажи делают этот сериал обязательным к просмотру. Присоединяйтесь к битве!
udinslot
голяк смотреть онлайн бесплатно в хорошем качестве голяк смотреть бесплатно
https://ataka-titanov-anime.ru/ – эпический аниме-сериал, где человечество борется за выживание в мире, наполненном гигантскими титанами. Динамичные бои, захватывающий сюжет и глубокие персонажи делают этот сериал обязательным к просмотру. Присоединяйтесь к битве!
смотреть голяк кубе https://golyak-serial-online.ru
In this dismay artifice, players forced to pilot a paralysing world while avoiding the monstrous living thing physical known as siren head. The strength objective of Sorceress Administrator is survival, requiring players to throw away furtiveness and cunning to get away from capture. With its atmospheric tautness and implacable pursuing, the engagement offers a chilling experience.
атака титанов в хорошем качестве – эпический аниме-сериал, где человечество борется за выживание в мире, наполненном гигантскими титанами. Динамичные бои, захватывающий сюжет и глубокие персонажи делают этот сериал обязательным к просмотру. Присоединяйтесь к битве!
provigil order online canada
https://finnmark.ca/asiabet118
атака титанов смотреть онлайн – эпический аниме-сериал, где человечество борется за выживание в мире, наполненном гигантскими титанами. Динамичные бои, захватывающий сюжет и глубокие персонажи делают этот сериал обязательным к просмотру. Присоединяйтесь к битве!
dimenhydrinate 50 mg drug – order risedronate 35 mg for sale buy actonel without a prescription
order dramamine without prescription – risedronate pills how to get risedronate without a prescription
https://saranbaskar.com/?keyword=dewaslot99
{
ทดลองเล่นสล็อต pg
Slotเว็บตรง – เพลิดเพลินกับการเล่นได้ทุกอุปกรณ์เชื่อมต่อที่ต่ออินเทอร์เน็ต
ในสมัยนี้ การหมุนสล็อตมีความง่ายดายมากยิ่งขึ้น คุณไม่จำเป็นต้องเดินทางไปยังบ่อนคาสิโนที่ไหน ๆ เพียงแค่มีอุปกรณ์อิเล็กทรอนิกส์ที่มีความสามารถเชื่อมต่อเชื่อมต่อกับอินเทอร์เน็ต คุณก็สามารถสนุกกับการเล่นเกมสล็อตออนไลน์กับ PG Slot ได้จากทุกที่
การอัพเกรดเทคโนโลยีของ PG Slot
ที่ PG Slot เราได้พัฒนาโซลูชั่นสำหรับการดูแลเกมคาสิโนออนไลน์เพื่อตอบสนองความต้องการของลูกค้าให้มากที่สุด คุณไม่ต้องติดตั้งแอปพลิเคชันหรือติดตั้งแอปพลิเคชันใด ๆ ให้ยุ่งยากหรือกินพื้นที่ในเครื่องมือของคุณ การดูแลเกมสล็อตออนไลน์ของเราทำงานผ่านเว็บตรงที่ใช้เทคโนโลยี HTML 5 ที่ทันสมัย
หมุนสล็อตได้ทุกอุปกรณ์เชื่อมต่อ
คุณสามารถเล่นสล็อตออนไลน์กับ PG Slot ได้อย่างง่ายดายเพียงเยี่ยมชมในเว็บไซต์ของเรา เว็บตรงสล็อตออนไลน์ของเรารองรับทุกโครงสร้างและทุกเครื่องทั้ง Android และ iOS ไม่ว่าคุณจะใช้สมาร์ทโฟน คอมพิวเตอร์ หรือแท็บเล็ตรุ่นไหน ก็อาจมั่นใจได้ว่าคุณจะเล่นสล็อตออนไลน์ได้อย่างไม่ติดขัด ไม่มีปัญหาหรือชะงักใด ๆ
ลองเล่นเกมสล็อตฟรี
เว็บตรงของเราให้บริการเพียงแค่คุณเยี่ยมชมในเว็บไซต์ของ PG Slot ก็อาจทดลองเล่นสล็อตฟรีได้ทันที ไม่ต้องเสียค่าใช้จ่ายเพิ่มเติมใด ๆ นี่เป็นโอกาสที่ดีในการฝึกฝนและเรียนรู้เกี่ยวกับเกมก่อนที่จะเล่นจริงด้วยเงินจริง
การหมุนสล็อตออนไลน์กับ PG Slot ให้คุณสามารถเพลิดเพลินกับการเล่นเกมคาสิโนได้ทุกที่ทุกเวลา ไม่ว่าคุณจะอยู่ที่ไหน เพียงแค่มีอุปกรณ์เชื่อมต่อที่เชื่อมต่ออินเทอร์เน็ต คุณก็จะสนุกกับการเล่นเกมสล็อตได้อย่างไม่มีข้อผูกมัด!
Привет учащиеся!
У меня недавно возникла потребность в получении среднего образования, но моя постоянная работа и другие заботы постоянно забирают всё моё время, и я не могу этого сделать. К моему удивлению, друзья подсказали, что можно легально приобрести диплом о среднем профессиональном образовании (диплом техникума или колледжа), пройдя обучение по упрощенной программе!
В интернете предложений предостаточно, но как не стать жертвой мошенников и найти надежную компанию? Этот вопрос очень важен, и к нему следует подходить ответственно. Я лично проверил, что на сайте https://russa24-diploms-srednee.com содержится множество полезной информации о том, как избежать обмана и не потерять свои деньги напрасно. Как можно проверить компанию по продаже дипломов, на что обратить внимание, и, конечно же, там можно заказать диплом под ключ без предварительной оплаты.
В отличие от других коммерческих организаций, мы не ориентируемся исключительно на заработок — мы работаем на благо наших клиентов. Мы предоставляем бесплатные консультации без ограничений по количеству вопросов. Наши специалисты — это проверенные временем сотрудники, и обратиться к нам — это правильное решение, ведь мы гарантируем качество, соблюдение сроков и разумные цены на заказ дипломов о среднем образовании.
Удачи и хороших оценок!
как купить диплом о среднем медицинском образовании
купить диплом о среднем специальном образовании в москве
диплом о среднем образовании купить в спб
купить дипломы о среднем образовании срочно
купить диплом о среднем специальном образование в москве
купить диплом о среднем профессиональном образовании спб
купить диплом о среднем образовании в саратове
можно ли купить диплом о среднем специальном образовании в
диплом о среднем образовании купил отзывы
где можно купить диплом о среднем образовании
buy generic accutane 40 mg
https://thepetmaven.ca/batoto
富遊娛樂城評價:2024年最新評價
推薦指數 : ★★★★★ ( 5.0/5 )
富遊娛樂城作為目前最受歡迎的博弈網站之一,在台灣擁有最高的註冊人數。
RG富遊以安全、公正、真實和順暢的品牌保證,贏得了廣大玩家的信賴。富遊線上賭場不僅提供了豐富多樣的遊戲種類,還有眾多吸引人的優惠活動。在出金速度方面,獲得無數網紅和網友的高度評價,確保玩家能享有無憂的博弈體驗。
推薦要點
新手首選: 富遊娛樂城,2024年評選首選,提供專為新手打造的豐富教學和獨家優惠。
一存雙收: 首存1000元,立獲1000元獎金,僅需1倍流水,新手友好。
免費體驗: 新玩家享免費體驗金,暢遊各式遊戲,開啟無限可能。
優惠多元: 活動豐富,流水要求低,適合各類型玩家。
玩家首選: 遊戲多樣,服務優質,是新手與老手的最佳賭場選擇。
富遊娛樂城詳情資訊
賭場名稱 : RG富遊
創立時間 : 2019年
賭場類型 : 現金版娛樂城
博弈執照 : 馬爾他牌照(MGA)認證、英屬維爾京群島(BVI)認證、菲律賓(PAGCOR)監督競猜牌照
遊戲類型 : 真人百家樂、運彩投注、電子老虎機、彩票遊戲、棋牌遊戲、捕魚機遊戲
存取速度 : 存款5秒 / 提款3-5分
軟體下載 : 支援APP,IOS、安卓(Android)
線上客服 : 需透過官方LINE
富遊娛樂城優缺點
優點
台灣註冊人數NO.1線上賭場
首儲1000贈1000只需一倍流水
擁有體驗金免費體驗賭場
網紅部落客推薦保證出金線上娛樂城
缺點
需透過客服申請體驗金
富遊娛樂城存取款方式
存款方式
提供四大超商(全家、7-11、萊爾富、ok超商)
虛擬貨幣ustd存款
銀行轉帳(各大銀行皆可)
取款方式
網站內申請提款及可匯款至綁定帳戶
現金1:1出金
富遊娛樂城平台系統
真人百家 — RG真人、DG真人、歐博真人、DB真人(原亞博/PM)、SA真人、OG真人、WM真人
體育投注 — SUPER體育、鑫寶體育、熊貓體育(原亞博/PM)
彩票遊戲 — 富遊彩票、WIN 539
電子遊戲 —RG電子、ZG電子、BNG電子、BWIN電子、RSG電子、GR電子(好路)
棋牌遊戲 —ZG棋牌、亞博棋牌、好路棋牌、博亞棋牌
電競遊戲 — 熊貓體育
捕魚遊戲 —ZG捕魚、RSG捕魚、好路GR捕魚、DB捕魚
twin казино вход
elevex tadalafil 20mg
which online pharmacy is reliable
Читайте интересные статьи на важные темы, связанные с покупкой жилья, например приемка квартиры в новостройке или стоимость недвижимости в Москве.
Сайт: https://ooo-trotuar.ru
슬롯 커뮤
그는 군자의 나쁜 점을 없애기로 했다.
demo slot pragmatic
2024娛樂城推薦,經過玩家實測結果出爐Top5!
2024娛樂城排名是這五間上榜,玩家尋找娛樂城無非就是要找穩定出金娛樂城,遊戲體驗良好、速度流暢,Ace博評網都幫你整理好了,給予娛樂城新手最佳的指南,不再擔心被黑網娛樂城詐騙!
2024娛樂城簡述
在現代,2024娛樂城數量已經超越以前,面對琳瑯滿目的娛樂城品牌,身為新手的玩家肯定難以辨別哪間好、哪間壞。
好的平台提供穩定的速度與遊戲體驗,穩定的系統與資訊安全可以保障用戶的隱私與資料,不用擔心收到傳票與任何網路威脅,這些線上賭場也提供合理的優惠活動給予玩家。
壞的娛樂城除了會騙取你的金錢之外,也會打著不實的廣告、優惠滿滿,想領卻是一場空!甚至有些平台還沒辦法登入,入口網站也是架設用來騙取新手儲值進他們口袋,這些黑網娛樂城是玩家必須避開的風險!
評測2024娛樂城的標準
Ace這次從網路上找來五位使用過娛樂城資歷2年以上的老玩家,給予他們使用各大娛樂城平台,最終選出Top5,而評選標準為下列這些條件:
以玩家觀點出發,優先考量玩家利益
豐富的遊戲種類與卓越的遊戲體驗
平台的信譽及其安全性措施
客服團隊的回應速度與服務品質
簡便的儲值流程和多樣的存款方法
吸引人的優惠活動方案
前五名娛樂城表格
賭博網站排名 線上賭場 平台特色 玩家實測評價
No.1 富遊娛樂城 遊戲選擇豐富,老玩家優惠多 正面好評
No.2 bet365娛樂城 知名大廠牌,運彩盤口選擇多 介面流暢
No.3 亞博娛樂城 多語言支持,介面簡潔順暢 賽事豐富
No.4 PM娛樂城 撲克牌遊戲豐富,選擇多元 直播順暢
No.5 1xbet娛樂城 直播流暢,安全可靠 佳評如潮
線上娛樂城玩家遊戲體驗評價分享
網友A:娛樂城平台百百款,富遊娛樂城是我3年以來長期使用的娛樂城,別人有的系統他們都有,出金也沒有被卡過,比起那些玩娛樂城還會收到傳票的娛樂城,富遊真的很穩定,值得推薦。
網友B:bet365中文的介面簡約,還有超多體育賽事盤口可以選擇,此外賽事大部分也都有附上直播來源,不必擔心看不到賽事最新狀況,全螢幕還能夠下單,真的超方便!
網友C:富遊娛樂城除了第一次儲值有優惠之外,儲值到一定金額還有好禮五選一,實用又方便,有問題的時候也有客服隨時能夠解答。
網友D:從大陸來台灣工作,沒想到台灣也能玩到亞博體育,這是以前在大陸就有使用的平台,雖然不是簡體字,但使用介面完全沒問題,遊戲流暢、速度比以前使用還更快速。
網友E:看玖壹壹MV發現了PM娛樂城這個大品牌,PM的真人百家樂沒有輸給在澳門實地賭場,甚至根本不用出門,超級方便的啦!
https://yesyoucangohiking.ca/gaspol168
Wonders Travel & Tourism: a https://jordan-travel.com agency located in Aqaba. Specializing in tours around Jordan, including Petra, Wadi Rum, the Dead Sea, and Amman. Offering private tours that can be customized to tourist interests and have positive reviews for professionalism and service.
Итальянская мебель от салона https://formul.ru в Москве – это большой выбор мебели из Италии по доступным ценам! Итальянская мебель в налиичи и на заказ. Купить итальянскую мебель в Москве по лучшим ценам.
pill vasotec – vasotec 10mg canada order generic latanoprost
cost of advair in mexico
Hi! I just wanted to ask if you ever have any problems with hackers?
My last blog (wordpress) was hacked and I ended up losing many months of
hard work due to no back up. Do you have any solutions to prevent hackers?
Доброго!
Недавно у меня возникла потребность в получении среднего образования, но моя постоянная работа и обязанности постоянно отнимают время, не оставляя возможности этим заниматься. К счастью, друзья подсказали мне, что можно легально приобрести диплом о среднем профессиональном образовании (диплом техникума, колледжа) на бланках государственного образца, пройдя обучение по упрощенной программе!
В интернете предложений более чем достаточно, но как не стать жертвой мошенников и выбрать подходящую компанию? Этот вопрос требует особой внимательности и ответственности. Лично я проверил, что на https://arusak-diploms-srednee.ru есть много полезной информации о том, как избежать ошибок и не потерять свои деньги. Как можно проверить компанию по продаже дипломов, на что обратить внимание, и, конечно же, там можно заказать диплом “под ключ” без предварительной оплаты.
В отличие от других коммерческих организаций, наша цель не сводится к заработку – мы работаем на благо наших клиентов. Мы предоставляем бесплатные консультации без ограничений по количеству вопросов. Наши специалисты – проверенные временем профессионалы, поэтому обращение к нам – правильное решение, ведь мы гарантируем качество, соблюдение сроков и разумные цены на дипломы о среднем образовании на заказ.
Удачи и хороших оценок!
купить диплом о высшем образовании цены отзывы
купить вуз диплом
купить диплом мгсу
купить диплом курса повышения квалификации
купить диплом о среднем специальном образовании гознак
купить диплом директора
диплом южной осетии купить
купить диплом фармацевта с занесением в реестр
купить аттестат в омске
купить диплом о профпереподготовке
discount pharmacy card
https://darbastfam.com/?keyword=alexis-toto
娛樂城評價
2024娛樂城推薦,經過玩家實測結果出爐Top5!
2024娛樂城排名是這五間上榜,玩家尋找娛樂城無非就是要找穩定出金娛樂城,遊戲體驗良好、速度流暢,Ace博評網都幫你整理好了,給予娛樂城新手最佳的指南,不再擔心被黑網娛樂城詐騙!
2024娛樂城簡述
在現代,2024娛樂城數量已經超越以前,面對琳瑯滿目的娛樂城品牌,身為新手的玩家肯定難以辨別哪間好、哪間壞。
好的平台提供穩定的速度與遊戲體驗,穩定的系統與資訊安全可以保障用戶的隱私與資料,不用擔心收到傳票與任何網路威脅,這些線上賭場也提供合理的優惠活動給予玩家。
壞的娛樂城除了會騙取你的金錢之外,也會打著不實的廣告、優惠滿滿,想領卻是一場空!甚至有些平台還沒辦法登入,入口網站也是架設用來騙取新手儲值進他們口袋,這些黑網娛樂城是玩家必須避開的風險!
評測2024娛樂城的標準
Ace這次從網路上找來五位使用過娛樂城資歷2年以上的老玩家,給予他們使用各大娛樂城平台,最終選出Top5,而評選標準為下列這些條件:
以玩家觀點出發,優先考量玩家利益
豐富的遊戲種類與卓越的遊戲體驗
平台的信譽及其安全性措施
客服團隊的回應速度與服務品質
簡便的儲值流程和多樣的存款方法
吸引人的優惠活動方案
前五名娛樂城表格
賭博網站排名 線上賭場 平台特色 玩家實測評價
No.1 富遊娛樂城 遊戲選擇豐富,老玩家優惠多 正面好評
No.2 bet365娛樂城 知名大廠牌,運彩盤口選擇多 介面流暢
No.3 亞博娛樂城 多語言支持,介面簡潔順暢 賽事豐富
No.4 PM娛樂城 撲克牌遊戲豐富,選擇多元 直播順暢
No.5 1xbet娛樂城 直播流暢,安全可靠 佳評如潮
線上娛樂城玩家遊戲體驗評價分享
網友A:娛樂城平台百百款,富遊娛樂城是我3年以來長期使用的娛樂城,別人有的系統他們都有,出金也沒有被卡過,比起那些玩娛樂城還會收到傳票的娛樂城,富遊真的很穩定,值得推薦。
網友B:bet365中文的介面簡約,還有超多體育賽事盤口可以選擇,此外賽事大部分也都有附上直播來源,不必擔心看不到賽事最新狀況,全螢幕還能夠下單,真的超方便!
網友C:富遊娛樂城除了第一次儲值有優惠之外,儲值到一定金額還有好禮五選一,實用又方便,有問題的時候也有客服隨時能夠解答。
網友D:從大陸來台灣工作,沒想到台灣也能玩到亞博體育,這是以前在大陸就有使用的平台,雖然不是簡體字,但使用介面完全沒問題,遊戲流暢、速度比以前使用還更快速。
網友E:看玖壹壹MV發現了PM娛樂城這個大品牌,PM的真人百家樂沒有輸給在澳門實地賭場,甚至根本不用出門,超級方便的啦!
https://avpkw.ca/maxwin138
Здравствуйте!
Задался вопросом: можно ли на самом деле купить диплом государственного образца в Москве? Был приятно удивлен — это реально и легально!
Сначала искал информацию в интернете на тему: купить диплом мастера маникюра и педикюра, купить диплом в ростове-на-дону, купить диплом в глазове, купить диплом в кстово, купить диплом в находке и получил базовые знания. В итоге остановился на материале: https://dogovor-urist.ru/%D1%8E%D1%80%D0%B8%D0%B4%D0%B8%D1%87%D0%B5%D1%81%D0%BA%D0%B0%D1%8F_%D0%BA%D0%BE%D0%BD%D1%81%D1%83%D0%BB%D1%8C%D1%82%D0%B0%D1%86%D0%B8%D1%8F/20845-%D0%B6%D0%B5%D0%BB%D0%B0%D0%B5%D1%82%D0%B5_%D0%BA%D1%83%D0%BF%D0%B8%D1%82%D1%8C_%D0%B4%D0%B8%D0%BF%D0%BB%D0%BE%D0%BC_%D0%B8%D0%BD%D1%81%D1%82%D0%B8%D1%82%D1%83%D1%82%D0%B0/?m=q-added
Удачи и хороших оценок!
娛樂城
2024娛樂城介紹
台灣2024娛樂城越開越多間,新開的線上賭場層出不窮,每間都以獨家的娛樂城優惠和體驗金來吸引玩家,致力於提供一流的賭博遊戲體驗。以下來介紹這幾間娛樂城網友對他們的真實評價,看看哪些娛樂城上榜了吧!
2024娛樂城排名
2023下半年,各家娛樂城競爭激烈,相繼推出誘人優惠,不論是娛樂城體驗金、反水流水還是首儲禮金,甚至還有娛樂城抽I15手機。以下就是2024年網友推薦的娛樂城排名:
NO.1 富遊娛樂城
NO.2 Bet365台灣
NO.3 DG娛樂城
NO.4 九州娛樂城
NO.5 亞博娛樂城
2024娛樂城推薦
根據2024娛樂城排名,以下將富遊娛樂城、BET365、亞博娛樂城、九州娛樂城、王者娛樂城推薦給大家,包含首儲贈點、免費體驗金、存提款速度、流水等等…
娛樂城遊戲種類
線上娛樂城憑藉其廣泛的遊戲種類,成功滿足了各式各樣玩家的喜好和需求。這些娛樂城遊戲不僅多元化且各具特色,能夠為玩家提供無與倫比的娛樂體驗。下面是一些最受歡迎的娛樂城遊戲類型:
電子老虎機
魔龍傳奇、雷神之鎚、戰神呂布、聚寶財神、鼠來寶、皇家777
真人百家樂
真人視訊百家樂、牛牛、龍虎、炸金花、骰寶、輪盤
電子棋牌
德州撲克、兩人麻將、21點、十三支、妞妞、三公、鬥地主、大老二、牌九
體育下注
世界盃足球賽、NBA、WBC世棒賽、英超、英雄聯盟LOL、特戰英豪
線上彩票
大樂透、539、美國天天樂、香港六合彩、北京賽車
捕魚機遊戲
三仙捕魚、福娃捕魚、招財貓釣魚、西遊降魔、吃我一砲、賓果捕魚
2024娛樂城常見問題
娛樂城是什麼?
娛樂城/線上賭場(現金網)是台灣對於線上賭場的特別稱呼,而且是現金網,大家也許會好奇為什麼不直接叫做線上賭場或是線上博弈就好了。
其實這是有原因的,線上賭場這種東西,架站在台灣是違法的,在早期經營線上博弈被抓的風險非常高所以換了一個打模糊仗的代稱「娛樂城」來規避警方的耳目,畢竟以前沒有Google這種東西,這樣的代稱還是多少有些作用的。
信用版娛樂城是什麼?
信用版娛樂城是一種賭博平台,允許玩家在沒有預先充值的情況下參與遊戲。這種模式類似於信用卡,通常以周結或月結的方式結算遊戲費用。因此,如果玩家無法有效管理自己的投注額,可能會在月底面臨巨大的支付壓力。
娛樂城不出金怎麼辦?
釐清原因,如未違反娛樂城機制,可能是遇上黑網娛樂城,請盡快通報165反詐騙。
Портал о Ярославле – ваш гид по культурной жизни города. Здесь вы найдёте информацию о театрах, музеях, галереях и исторических достопримечательностях. Откройте для себя яркие события, фестивали и выставки, которые делают Ярославль культурной жемчужиной России.
Dragon Money Casino онлайн казино Dragon Money
Портал о культуре – ваш гид по культурной жизни города. Здесь вы найдёте информацию о театрах, музеях, галереях и исторических достопримечательностях. Откройте для себя яркие события, фестивали и выставки, которые делают Ярославль культурной жемчужиной России.
онлайн казино Dragon Money https://krpb.ru/
tetracycline pharmacy
драгон мани казино онлайн казино Dragon Money
order monograph 600 mg without prescription – order pletal 100 mg online cheap where can i buy pletal
регистрация 1го казино регистрация 1го казино
etodolac for sale – pletal medication pletal 100mg cheap
feldene online buy – order feldene 20mg sale buy exelon 6mg online
1го казино 1go casino
doxycycline 50 mg price
2024娛樂城介紹
台灣2024娛樂城越開越多間,新開的線上賭場層出不窮,每間都以獨家的娛樂城優惠和體驗金來吸引玩家,致力於提供一流的賭博遊戲體驗。以下來介紹這幾間娛樂城網友對他們的真實評價,看看哪些娛樂城上榜了吧!
2024娛樂城排名
2023下半年,各家娛樂城競爭激烈,相繼推出誘人優惠,不論是娛樂城體驗金、反水流水還是首儲禮金,甚至還有娛樂城抽I15手機。以下就是2024年網友推薦的娛樂城排名:
NO.1 富遊娛樂城
NO.2 Bet365台灣
NO.3 DG娛樂城
NO.4 九州娛樂城
NO.5 亞博娛樂城
2024娛樂城推薦
根據2024娛樂城排名,以下將富遊娛樂城、BET365、亞博娛樂城、九州娛樂城、王者娛樂城推薦給大家,包含首儲贈點、免費體驗金、存提款速度、流水等等…
娛樂城遊戲種類
線上娛樂城憑藉其廣泛的遊戲種類,成功滿足了各式各樣玩家的喜好和需求。這些娛樂城遊戲不僅多元化且各具特色,能夠為玩家提供無與倫比的娛樂體驗。下面是一些最受歡迎的娛樂城遊戲類型:
電子老虎機
魔龍傳奇、雷神之鎚、戰神呂布、聚寶財神、鼠來寶、皇家777
真人百家樂
真人視訊百家樂、牛牛、龍虎、炸金花、骰寶、輪盤
電子棋牌
德州撲克、兩人麻將、21點、十三支、妞妞、三公、鬥地主、大老二、牌九
體育下注
世界盃足球賽、NBA、WBC世棒賽、英超、英雄聯盟LOL、特戰英豪
線上彩票
大樂透、539、美國天天樂、香港六合彩、北京賽車
捕魚機遊戲
三仙捕魚、福娃捕魚、招財貓釣魚、西遊降魔、吃我一砲、賓果捕魚
2024娛樂城常見問題
娛樂城是什麼?
娛樂城/線上賭場(現金網)是台灣對於線上賭場的特別稱呼,而且是現金網,大家也許會好奇為什麼不直接叫做線上賭場或是線上博弈就好了。
其實這是有原因的,線上賭場這種東西,架站在台灣是違法的,在早期經營線上博弈被抓的風險非常高所以換了一個打模糊仗的代稱「娛樂城」來規避警方的耳目,畢竟以前沒有Google這種東西,這樣的代稱還是多少有些作用的。
信用版娛樂城是什麼?
信用版娛樂城是一種賭博平台,允許玩家在沒有預先充值的情況下參與遊戲。這種模式類似於信用卡,通常以周結或月結的方式結算遊戲費用。因此,如果玩家無法有效管理自己的投注額,可能會在月底面臨巨大的支付壓力。
娛樂城不出金怎麼辦?
釐清原因,如未違反娛樂城機制,可能是遇上黑網娛樂城,請盡快通報165反詐騙。
регистрация 1Go Casino регистрация 1го казино
娛樂城
Player台灣線上娛樂城遊戲指南與評測
台灣最佳線上娛樂城遊戲的終極指南!我們提供專業評測,分析熱門老虎機、百家樂、棋牌及其他賭博遊戲。從遊戲規則、策略到選擇最佳娛樂城,我們全方位覆蓋,協助您更安全的遊玩。
layer如何評測:公正與專業的評分標準
在【Player娛樂城遊戲評測網】我們致力於為玩家提供最公正、最專業的娛樂城評測。我們的評測過程涵蓋多個關鍵領域,旨在確保玩家獲得可靠且全面的信息。以下是我們評測娛樂城的主要步驟:
安全與公平性
安全永遠是我們評測的首要標準。我們審查每家娛樂城的執照資訊、監管機構以及使用的隨機數生成器,以確保其遊戲結果的公平性和隨機性。
02.
遊戲品質與多樣性
遊戲的品質和多樣性對於玩家體驗至關重要。我們評估遊戲的圖形、音效、用戶介面和創新性。同時,我們也考量娛樂城提供的遊戲種類,包括老虎機、桌遊、即時遊戲等。
03.
娛樂城優惠與促銷活動
我們仔細審視各種獎勵計劃和促銷活動,包括歡迎獎勵、免費旋轉和忠誠計劃。重要的是,我們也檢查這些優惠的賭注要求和條款條件,以確保它們公平且實用。
04.
客戶支持
優質的客戶支持是娛樂城質量的重要指標。我們評估支持團隊的可用性、響應速度和專業程度。一個好的娛樂城應該提供多種聯繫方式,包括即時聊天、電子郵件和電話支持。
05.
銀行與支付選項
我們檢查娛樂城提供的存款和提款選項,以及相關的處理時間和手續費。多樣化且安全的支付方式對於玩家來說非常重要。
06.
網站易用性、娛樂城APP體驗
一個直觀且易於導航的網站可以顯著提升玩家體驗。我們評估網站的設計、可訪問性和移動兼容性。
07.
玩家評價與反饋
我們考慮真實玩家的評價和反饋。這些資料幫助我們了解娛樂城在實際玩家中的表現。
娛樂城常見問題
娛樂城是什麼?
娛樂城是什麼?娛樂城是台灣對於線上賭場的特別稱呼,線上賭場分為幾種:現金版、信用版、手機娛樂城(娛樂城APP),一般來說,台灣人在稱娛樂城時,是指現金版線上賭場。
線上賭場在別的國家也有別的名稱,美國 – Casino, Gambling、中國 – 线上赌场,娱乐城、日本 – オンラインカジノ、越南 – Nhà cái。
娛樂城會被抓嗎?
在台灣,根據刑法第266條,不論是實體或線上賭博,參與賭博的行為可處最高5萬元罰金。而根據刑法第268條,為賭博提供場所並意圖營利的行為,可能面臨3年以下有期徒刑及最高9萬元罰金。一般賭客若被抓到,通常被視為輕微罪行,原則上不會被判處監禁。
信用版娛樂城是什麼?
信用版娛樂城是一種線上賭博平台,其中的賭博活動不是直接以現金進行交易,而是基於信用系統。在這種模式下,玩家在進行賭博時使用虛擬的信用點數或籌碼,這些點數或籌碼代表了一定的貨幣價值,但實際的金錢交易會在賭博活動結束後進行結算。
現金版娛樂城是什麼?
現金版娛樂城是一種線上博弈平台,其中玩家使用實際的金錢進行賭博活動。玩家需要先存入真實貨幣,這些資金轉化為平台上的遊戲籌碼或信用,用於參與各種賭場遊戲。當玩家贏得賭局時,他們可以將這些籌碼或信用兌換回現金。
娛樂城體驗金是什麼?
娛樂城體驗金是娛樂場所為新客戶提供的一種免費遊玩資金,允許玩家在不需要自己投入任何資金的情況下,可以進行各類遊戲的娛樂城試玩。這種體驗金的數額一般介於100元到1,000元之間,且對於如何使用這些體驗金以達到提款條件,各家娛樂城設有不同的規則。
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
Здравствуйте!
Хочу поделиться своим опытом по заказу аттестата ПТУ. Думал, что это невозможно, и начал искать информацию в интернете по теме: диплом пту купить, рамки для дипломов купить, купить диплом хореографа, куплю диплом о среднем специальном образовании цена, поддельный аттестат купить. Постепенно углубляясь в тему, нашел отличный ресурс здесь: https://arusak-diploms-srednee.ru/ и остался очень доволен!
Теперь у меня есть диплом сварщика о среднем специальном образовании, и я обеспечен на всю жизнь!
Удачи и хороших оценок!
купить корочки техникума
куплю диплом другим
купить диплом в назрани
купить диплом о полном среднем
купить аттестат настоящий
купить диплом о среднем специальном образовании недорого
купить диплом о среднем образовании красноярск
хочу купить диплом
диплом среднем образовании купить
купить диплом в жуковском
buy dexamethasone australia
квартиры в новостройках казани https://novostroyka-kzn16.ru
квартира в новостройке от застройщика https://kvartiru-kupit-spb.ru
квартиры казань цены от застройщика https://novostroyka-kzn16.ru
Привет, друзья!
Всегда считал, что покупка диплома о высшем образовании — это миф и невозможно. Но, к счастью, оказался неправ. Сначала искал информацию по теме: , , , , , а затем переключился на дипломы вузов. Подробности здесь:
Оказалось, что все реально и легально, со специальными условиями и упрощенными программами. Теперь у меня диплом московского вуза нового образца, что я настоятельно рекомендую и вам!
Удачи и хороших оценок!
квартиры от застройщика жк https://kvartiru-kupit-spb.ru
недорогие квартиры цены https://novostroyka-kzn16.ru
modafinil rx
https://knight-kun.com/?keyword=bensu4d
슬롯 무료 게임
하지만 문제는 모든 사람이 진실을 이해하고 있다는 것입니다. 어떻게 해야 할까요?
娛樂城
在现代,在线赌场提供了多种便捷的存款和取款方式。对于较大金额的存款,您可以选择中国信托、台中银行、合作金库、台新银行、国泰银行或中华邮政。这些银行提供的服务覆盖金额范围从$1000到$10万,确保您的资金可以安全高效地转入赌场账户。
如果您需要进行较小金额的存款,可以选择通过便利店充值。7-11、全家、莱尔富和OK超商都提供这种服务,适用于金额范围在$1000到$2万之间的充值。通过这些便利店,您可以轻松快捷地完成资金转账,无需担心银行的营业时间或复杂的操作流程。
在进行娱乐场提款时,您可以选择通过各大银行转账或ATM转账。这些方法不仅安全可靠,而且非常方便,适合各种提款需求。最低提款金额为$1000,而上限则没有限制,确保您可以灵活地管理您的资金。
在选择在线赌场时,玩家评价和推荐也是非常重要的。许多IG网红和部落客,如丽莎、穎柔、猫少女日记-Kitty等,都对一些知名的娱乐场给予了高度评价。这些推荐不仅帮助您找到可靠的娱乐场所,还能确保您在游戏中享受到最佳的用户体验。
总体来说,在线赌场通过提供多样化的存款和取款方式,以及得到广泛认可的服务质量,正在不断吸引更多的玩家。无论您选择通过银行还是便利店进行充值,都能体验到快速便捷的操作。同时,通过查看玩家的真实评价和推荐,您也能更有信心地选择合适的娱乐场,享受安全、公正的游戏环境。
tante4d
квартира от застройщика квартиры от застройщика цены
квартира в новостройке от застройщика продажа квартир цены
квартиры с отделкой от застройщика квартира в новостройке от застройщика
Каталог эротических рассказов https://vicmin.ru подарит тебе возможность уйти от рутины и погрузиться в мир секса и безудержного наслаждения. Обширная коллекция рассказов для взрослых разбудит твое воображение и принесет немыслимое удовольствие.
Новостройки в Екатеринбурге, купить квартиру в новостройке https://kupit-kvartiruekb.ru от застройщика. Строительство жилой и коммерческой недвижимости. Высокое качество, прозрачность на всех этапах строительства и сделки.
купить красный диплом https://diplom-izhevsk.ru
??????????????? — ????????? ????????? ???????? ??????????? ??? ?????????
??????????????????? ??? PG ????????????????????????? ???????? ???????????? ???????????????????????????? ??????? ???????????????? ?????? ??????? ???? ??????????? ??????
??? PG Slot ?????????????????????????? ????????? ???????? ????????? ??? ????????????????????????????? ?????? ???????????? HTML 5 ???????? ????????????????????????? ???????? ???????????????????????????? ????????????? ???????????? ??????????????????????????? ????? ????????????? ???????????? ????????? ??????????? ?????????????? ????????? ????????????????????
??????????????????????
?????????????? ?????????????? ???? Android ???? iOS ???????? ?????????????????????????????? ?????????? ???????????????????????? ????????????????? ?????????????? ??? ????????? ???????????????????? ???? ???????????????????? ???????????????? ??????????? ?????????? ??????????????????????
????????????????????
?????????????????????????????? PG Slot ??? ????????? ?????????????? ???????? ??????? ????????? ?????????? ?????????????? ??????????????????? ???? ????????? ??????????????? ????????????? ???????????????????? ????????????????????? ????????????????????
?????????????????
???????? ??????????? ?????????????????????????????????????????????? PG Slot ??????????????????? ????????? ??????????????????????????????????????????????? ??? ?????????????????????????????????????????????????????????????????????????????????
??????????????????????????
PG Slot ???????????????????????????????????? ????? ???????????????????????????? ????????????????? ?????????????????????????????? ??????????? ?????????????????? ???????????????????????????????
??????????????????????
?????????????????????????????????????? PG Slot ????? ?? ????????????????????????????????? ??????????????? ?????????????????? ????????? ?????????????????????? ????????? ?????????????????????????????????
??????????????????????? PG Slot ????????????????????????? ???????????????????????????????????????????????????????? ?????????????????????????????????????????????????? ?????????????????????????????? ???????? ????????????????????? ?????????????????????????????????? ????????? ????????????????????????????? PG Slot ??????!
купить диплом недорого https://diplom-izhevsk.ru
สล็อต
สล็อตออนไลน์เว็บตรง: ความบันเทิงที่ผู้เล่นไม่ควรพลาด
การเล่นสล็อตออนไลน์ในปัจจุบันนี้ได้รับความนิยมอย่างกว้างขวาง เนื่องจากความสะดวกสบายที่ผู้เล่นสามารถใช้งานได้ได้ทุกที่ตลอดเวลา โดยไม่ต้องเสียเวลาในการเดินทางไปยังสถานที่คาสิโน ในบทความนี้ที่เราจะนำเสนอ เราจะนำเสนอเกี่ยวกับ “สล็อตออนไลน์” และความเพลิดเพลินที่คุณสามารถพบได้ในเกมสล็อตเว็บตรง
ความสะดวกในการเล่นสล็อตออนไลน์
เหตุผลหนึ่งที่ทำให้สล็อตเว็บตรงเป็นที่สนใจอย่างยิ่ง คือความสะดวกที่นักเดิมพันได้สัมผัส คุณจะเล่นได้ทุกที่ได้ตลอดเวลา ไม่ว่าจะเป็นที่บ้านของคุณ ในออฟฟิศ หรือถึงแม้จะอยู่ในการเดินทาง สิ่งที่คุณควรมีคืออุปกรณ์ที่สามารถเชื่อมต่ออินเทอร์เน็ตได้ ไม่ว่าจะเป็นสมาร์ทโฟน แท็บเล็ต หรือโน้ตบุ๊ก
เทคโนโลยีกับสล็อตที่เว็บตรง
การเล่นสล็อตในปัจจุบันไม่เพียงแต่สะดวกสบาย แต่ยังมาพร้อมกับเทคโนโลยีใหม่ล่าสุดอีกด้วย สล็อตเว็บตรงใช้นวัตกรรม HTML5 ซึ่งทำให้ท่านไม่ต้องกังวลเกี่ยวกับเกี่ยวกับการลงซอฟต์แวร์หรือแอปพลิเคชันเพิ่มเติม แค่เปิดเบราว์เซอร์บนเครื่องมือของคุณและเข้าสู่เว็บไซต์ ผู้เล่นก็สามารถเริ่มเล่นเกมสล็อตได้ทันที
ตัวเลือกหลากหลายของเกมสล็อตออนไลน์
สล็อตเว็บตรงมาพร้อมกับตัวเลือกหลากหลายของเกมที่เล่นที่ผู้เล่นสามารถเลือก ไม่ว่าจะเป็นเกมคลาสสิกหรือเกมที่มีฟีเจอร์ฟีเจอร์เด็ดและโบนัสหลากหลาย คุณจะพบว่ามีเกมให้เลือกเล่นมากมาย ซึ่งทำให้ไม่มีวันเบื่อกับการเล่นสล็อตออนไลน์
รองรับทุกอุปกรณ์ที่ใช้
ไม่ว่าผู้เล่นจะใช้มือถือแอนดรอยด์หรือ iOS คุณก็สามารถเล่นเกมสล็อตออนไลน์ได้ได้อย่างลื่นไหล เว็บของเรารองรับระบบปฏิบัติการและทุกเครื่อง ไม่ว่าจะเป็นโทรศัพท์มือถือรุ่นล่าสุดหรือรุ่นเก่า หรือแม้กระทั่งแท็บเล็ตและโน้ตบุ๊ก ท่านก็สามารถสนุกกับเกมสล็อตได้อย่างเต็มที่
ทดลองเล่นสล็อตฟรี
สำหรับมือใหม่กับการเล่นสล็อตออนไลน์ หรือยังไม่แน่นอนเกี่ยวกับเกมที่ชอบ PG Slot ยังมีฟีเจอร์ทดลองเล่นเกมสล็อต คุณเริ่มเล่นได้ทันทีทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงินลงทุน การทดลองเล่นสล็อตนี้จะช่วยให้ท่านรู้วิธีการเล่นและเข้าใจวิธีการเล่นได้โดยไม่ต้องเสียค่าใช้จ่าย
โบนัสและโปรโมชั่น
ข้อดีอีกอย่างหนึ่งของการเล่นสล็อตออนไลน์กับ PG Slot คือมีโบนัสและโปรโมชั่นมากมายสำหรับผู้เล่น ไม่ว่าคุณจะเป็นผู้เล่นใหม่หรือสมาชิกเก่า ผู้เล่นสามารถได้รับโปรโมชั่นและโบนัสต่าง ๆ ได้ตลอดเวลา ซึ่งจะเพิ่มโอกาสชนะและเพิ่มความสนุกสนานในการเล่น
โดยสรุป
การเล่นเกมสล็อตออนไลน์ที่ PG Slot เป็นการการลงเงินที่น่าลงทุน คุณจะได้รับความสุขและความสะดวกสบายจากการเล่นเกม นอกจากนี้ยังมีโอกาสชนะรางวัลและโบนัสหลากหลาย ไม่ว่าคุณจะใช้มือถือ แท็บเล็ทหรือโน้ตบุ๊กยี่ห้อไหน ก็สามารถร่วมสนุกกับเราได้ทันที อย่ารอช้า ลงทะเบียนและเริ่มเล่น PG Slot วันนี้
probet88
สล็อตเว็บโดยตรง — ใช้ โทรศัพท์มือถือ แท็บเล็ต คอมฯ ฯลฯ สำหรับการเล่น
ระบบสล็อตเว็บตรง ของ PG ได้รับการพัฒนาและอัปเดต เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง สมบูรณ์ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเลต หรือ คอมฯ แบบไหน
ที่ PG Slot เราเข้าใจว่าผู้เล่นต้องการ ของผู้เล่น ในเรื่อง ความสะดวก และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง นำ HTML 5 มาใช้ ซึ่งเป็น เทคโนโลยีล่าสุด ในขณะนี้ มาใช้พัฒนาเว็บไซต์ คุณจึงไม่ต้อง ดาวน์โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเบราว์เซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บของเรา คุณสามารถ เพลิดเพลินกับสล็อตแมชชีนได้ทันที
การสนับสนุนหลายอุปกรณ์
ไม่ว่าคุณจะใช้ มือถือ ระบบ แอนดรอยด์ หรือ ไอโอเอส ก็สามารถ เล่นสล็อตได้อย่างราบรื่น ระบบของเรา ได้รับการออกแบบให้รองรับ ระบบต่าง ๆ ไม่สำคัญว่าคุณ มี มือถือ รุ่นใหม่หรือรุ่นเก่า หรือ แท็บเล็ตหรือโน้ตบุ๊ก ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา เรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot นั่นคือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ เป็นที่บ้าน ที่ออฟฟิศ หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเกมได้ทันที และคุณไม่ต้อง ห่วงเรื่องการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่บนอุปกรณ์ของคุณ
เล่นสล็อตฟรี
เพื่อให้ ผู้ใช้ใหม่ มีโอกาสลองและสัมผัสประสบการณ์สล็อตแมชชีนของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ ทดลองเล่นได้ทันทีโดยไม่ต้องสมัครหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
บริการและการรักษาความปลอดภัย
PG Slot ตั้งใจให้บริการที่ดีที่สุดกับลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี การรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชั่นและโบนัสพิเศษ
อีกข้อดีของการเล่นสล็อตกับ PG Slot ก็คือ มี โปรโมชันและโบนัสพิเศษสำหรับสมาชิก ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือเก่า คุณสามารถ รับโปรโมชั่นและโบนัสต่างๆได้อย่างต่อเนื่อง สิ่งนี้จะ เพิ่มโอกาสในการชนะและเพิ่มความเพลิดเพลินในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
pg สล็อต
เกี่ยวกับ ไซต์ PG Slots ซึ่งมีการ มี ความได้เปรียบ หลายประการ แตกต่างจาก คาสิโนแบบ ทั่วไป, โดยเฉพาะอย่างยิ่ง ใน ปัจจุบัน. คุณสมบัติสำคัญ เหล่านี้ เช่น:
ความสะดวก: ผู้เล่น สามารถเข้าเล่น สล็อตออนไลน์ได้ ตลอด 24 ชั่วโมง จาก ทุกแห่ง, ช่วย ผู้เล่นสามารถ เล่น ได้ ทุกอย่าง โดยไม่ต้อง ใช้เวลา ไปคาสิโนแบบ ปกติ ๆ
เกมหลากหลายรูปแบบ: สล็อตออนไลน์ มี ตัวเกม ที่ แตกต่างกัน, เช่น สล็อตคลาสสิค หรือ รูปแบบเกม ที่มี คุณสมบัติ และโบนัส พิเศษ, ไม่ทำ ความเซ็ง ในเกม
โปรโมชั่น และค่าตอบแทน: สล็อตออนไลน์ มักจะ ให้บริการ ส่วนลด และค่าตอบแทน เพื่อยกระดับ ความสามารถ ในการ ชนะ และ เพิ่ม ความสนุกสนาน ให้กับเกม
ความเชื่อมั่น และ ความน่าเชื่อถือ: สล็อตออนไลน์ โดยทั่วไป มี ระบบรักษาความปลอดภัย ที่ มีประสิทธิภาพ, และ เป็นที่น่าเชื่อถือ ว่า ข้อมูลส่วนบุคคล และ การเงิน จะได้รับความ คุ้มครอง
บริการสนับสนุน: PG Slots ว่าจ้าง ผู้เชี่ยวชาญ มืออาชีพ ที่มุ่งมั่น ดูแล ตลอดเวลา
การเล่นบนมือถือ: สล็อต PG อนุญาต การเล่นบนอุปกรณ์เคลื่อนที่, ช่วยให้ ผู้เล่นสามารถเข้าร่วม ตลอด 24 ชั่วโมง
เล่นฟรี: เกี่ยวกับ ผู้เล่นใหม่, PG ยังให้บริการ ทดลองใช้ฟรี เพิ่มเติมด้วย, ช่วยให้ คุณ ทดลอง เทคนิคการเล่น และทำความเข้าใจ เกมก่อน ลงเดิมพัน
สล็อต PG มี ข้อดี เป็นจำนวนมาก ที่ ส่งผล ให้ได้รับความต้องการ ในยุคปัจจุบัน, ส่งเสริม การ ความผ่อนคลาย ให้กับเกมด้วย.
ทดลองเล่นสล็อต
ทดลองดำเนินการเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังต้องการความบันเทิงและโอกาสในการได้รับรางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งตัวเลือกที่คุ้มค่าใคร่ครวญ.ด้วยความขนาดใหญ่ของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถทดลองเล่นและค้นหาเกมที่ต้องการได้อย่างง่ายดาย.
ไม่ว่าคุณจะประทับใจเกมสล็อตคลาสสิกหรือต้องการความท้าทาย, ตัวเลือกรอล้ำหน้าให้คุณสัมผัส. จากสล็อตที่มีธีมมากมาย ไปจนถึงเกมที่มีรูปแบบพิเศษและรางวัล, ผู้เล่นจะได้พบกับประสบการณ์ที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการปฏิบัติสล็อตฟรี, คุณสามารถศึกษาวิธีการเล่นและค้นตัดสินใจกลยุทธ์ที่ตรงใจก่อนลงทุนด้วยเงินจริง. นี่คือโอกาสดีที่จะปฏิบัติกับเกมและประยุกต์โอกาสในการได้รับรางวัลใหญ่.
อย่าเลื่อนเวลา, ลงมือกับการปฏิบัติสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินกับความสนใจ, ความเพลิดเพลิน และโอกาสชนะรางวัล. เริ่มต้นเดินทางสู่ความเฟื่องฟูของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
ทดลองเล่นสล็อต pg
ทดสอบ เข้าร่วม สล็อต PG ควบคู่กับ เข้าไปสู่ ไปสู่ ยุค แห่ง ความเพลิดเพลิน ที่ ไม่จำกัด
เกี่ยวกับ คอพนัน ที่ คิดค้น กำลังมองหา ประสบการณ์ เกมที่แตกต่าง, สล็อต PG คือ ทางออก ที่ น่าจับตามอง มากมาย. อันเนื่องมาจาก ความแตกต่าง ของ เกมสล็อตต่างๆ ที่ น่าทึ่ง และ น่าสำรวจ, นักพนัน จะสามารถ ทดสอบ และ ทดลอง เกม ที่ เหมาะกับ ลีลาการเล่น ของตนเอง.
แม้กระนั้น ลูกค้า จะพอใจกับ ความเพลิดเพลิน แบบดั้งเดิม หรือ การท้าทาย ที่ไม่เคยพบเจอ, สล็อต PG จะมี ที่หลากหลาย. ตั้งแต่ สล็อตประเภทคลาสสิก ที่ รู้จัก ไปจนถึง ตัวเกม ที่ มีลักษณะ คุณสมบัติพิเศษ และ โบนัสมากมาย, ลูกค้า จะมีโอกาส สัมผัส บรรยากาศ ที่ น่าตื่นเต้น และ เร้าใจ
ด้วย การทดลองเล่น สล็อต PG โดยไม่ต้องเสียเงิน, ลูกค้า สามารถ ทดลอง เทคนิควิธีการเล่น และ ทดลอง เคล็ดลับ ต่างๆ ล่วงหน้า เริ่มเล่น ด้วยเงินจริง. เช่นนั้น เป็น ช่องทาง ที่ยอดเยี่ยม ที่จะ เตรียมตัว และ ยกระดับ ความน่าจะเป็น ในการ ชนะ รางวัลมากมาย.
อย่าลังเล, ทดลอง ใน การเล่นทดลอง สล็อต PG วันนี้ และ พบเจอ การเล่น ที่ ไม่จำกัด! ทดลอง ความตื่นเต้นระคนตื่นเต้น, ความบันเทิง และ โอกาส ในการ ได้รับรางวัล มากมหาศาล. เริ่มต้น พัฒนา สู่ ความก้าวหน้า ของคุณในวงการ เกมสล็อตออนไลน์ ในทันที!
ciprofloxacin buy online
https://likedquotes.com/?keyword=idcash88
buy feldene 20 mg for sale – piroxicam without prescription buy rivastigmine 6mg sale
สล็อต
สล็อตแมชชีนเว็บตรง: ความบันเทิงที่คุณไม่ควรพลาด
การเล่นสล็อตในปัจจุบันเป็นที่นิยมเพิ่มมากขึ้น เนื่องจากความสะดวกสบายที่ผู้เล่นสามารถใช้งานได้จากทุกที่ทุกเวลา โดยไม่ต้องเสียเวลาเดินทางไปยังบ่อน ในบทความนี้ เราจะนำเสนอเกี่ยวกับ “สล็อตแมชชีน” และความบันเทิงที่ท่านสามารถพบได้ในเกมสล็อตออนไลน์เว็บตรง
ความสะดวกสบายในการเล่นสล็อต
หนึ่งในเหตุผลสล็อตที่เว็บตรงเป็นที่สนใจอย่างยิ่ง คือความง่ายดายที่นักเดิมพันมี คุณสามารถเล่นสล็อตได้ทุกหนทุกแห่งตลอดเวลา ไม่ว่าจะเป็นที่บ้านของคุณ ในที่ทำงาน หรือแม้กระทั่งในการเดินทาง สิ่งที่คุณต้องมีคืออุปกรณ์ที่เชื่อมต่อที่สามารถเชื่อมต่ออินเทอร์เน็ตได้ ไม่ว่าจะเป็นสมาร์ทโฟน แทปเล็ต หรือคอมพิวเตอร์
เทคโนโลยีกับสล็อตเว็บตรง
การเล่นสล็อตออนไลน์ในปัจจุบันไม่เพียงแต่สะดวกสบาย แต่ยังประกอบด้วยเทคโนโลยีล้ำสมัยอีกด้วย สล็อตออนไลน์เว็บตรงใช้เทคโนโลยี HTML5 ซึ่งทำให้คุณไม่ต้องกังวลเกี่ยวกับเกี่ยวกับการติดตั้งโปรแกรมหรือแอพพลิเคชั่น แค่เปิดบราวเซอร์บนเครื่องมือของคุณและเข้าสู่เว็บไซต์ ท่านก็สามารถสนุกกับเกมได้ทันที
ความหลากหลายของเกมของสล็อต
สล็อตเว็บตรงมาพร้อมกับตัวเลือกหลากหลายของเกมให้เลือกที่คุณสามารถเลือก ไม่ว่าจะเป็นเกมสล็อตแบบคลาสสิกหรือเกมสล็อตที่มาพร้อมกับฟีเจอร์เพิ่มเติมและโบนัสหลากหลาย ผู้เล่นจะเห็นว่ามีเกมที่ให้เล่นมากมาย ซึ่งทำให้ไม่เบื่อกับการเล่นสล็อตออนไลน์
รองรับทุกเครื่องมือ
ไม่ว่าผู้เล่นจะใช้โทรศัพท์มือถือระบบ Androidหรือ iOS ผู้เล่นก็สามารถเล่นสล็อตออนไลน์ได้อย่างไม่มีสะดุด เว็บไซต์สนับสนุนOSและทุกเครื่องมือ ไม่ว่าจะเป็นโทรศัพท์มือถือรุ่นใหม่หรือรุ่นก่อน หรือแม้กระทั่งแทปเล็ตและแล็ปท็อป ท่านก็สามารถเพลิดเพลินกับเกมสล็อตได้อย่างเต็มที่
สล็อตทดลองฟรี
สำหรับผู้ที่เพิ่งเริ่มต้นกับการเล่นสล็อต หรือยังไม่แน่ใจเกี่ยวกับเกมที่ชอบ PG Slot ยังมีระบบทดลองเล่นสล็อตฟรี คุณสามารถทดลองเล่นได้ทันทีโดยไม่ต้องสมัครสมาชิกหรือฝากเงินก่อน การทดลองเล่นเกมสล็อตนี้จะช่วยให้ผู้เล่นรู้วิธีการเล่นและเข้าใจวิธีการเล่นได้โดยไม่ต้องเสียค่าใช้จ่ายใด ๆ
โบนัสและโปรโมชั่น
ข้อดีอีกอย่างหนึ่งของการเล่นสล็อตเว็บตรงกับ PG Slot คือมีโบนัสและโปรโมชั่นมากมายสำหรับสมาชิก ไม่ว่าคุณจะเป็นผู้เล่นใหม่หรือสมาชิกเก่า คุณสามารถรับโบนัสและโปรโมชันต่าง ๆ ได้อย่างสม่ำเสมอ ซึ่งจะทำให้โอกาสชนะมากขึ้นและเพิ่มความสนุกสนานในเกม
โดยสรุป
การเล่นสล็อตออนไลน์ที่ PG Slot เป็นการลงทุนที่คุ้มค่า ผู้เล่นจะได้รับความสุขและความสะดวกจากการเล่นเกมสล็อต นอกจากนี้ยังมีโอกาสชนะรางวัลและโบนัสเพียบ ไม่ว่าผู้เล่นจะใช้โทรศัพท์มือถือ แทปเล็ตหรือคอมพิวเตอร์ยี่ห้อไหน ก็สามารถร่วมสนุกกับเราได้ทันที อย่ารอช้า ลงทะเบียนและเริ่มสนุกกับ PG Slot เดี๋ยวนี้
Cериал Голяк https://golyak-serial-online.ru смотреть онлайн в хорошем качестве и с лучшей озвучкой на любых устройствах. Все сезоны истории мелкого преступника Винни и его друзей в английском городке!
pg slot
สล็อตเว็บตรง — ใช้ มือถือ แท็บเลต คอมฯ ฯลฯ ในการเล่น
ระบบสล็อตตรงจากเว็บ ของ พีจีสล็อต ได้รับการพัฒนาและปรับปรุง เพื่อให้ รองรับการใช้ บนอุปกรณ์ที่หลากหลายได้อย่าง สมบูรณ์ ไม่สำคัญว่าจะใช้ มือถือ แท็บเลต หรือ คอมพิวเตอร์ส่วนตัว รุ่นใด
ที่ PG Slot เราเข้าใจถึงความต้องการ ของผู้เล่น ในเรื่อง ความสะดวก และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง นำ HTML 5 มาใช้ ซึ่งเป็น เทคโนโลยีล่าสุด ในตอนนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง ดาวน์โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ มีอยู่ของคุณ และเยี่ยมชม เว็บไซต์เรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การสนับสนุนหลายอุปกรณ์
ไม่ว่าคุณจะใช้ สมาร์ทโฟน ระบบ Android หรือ iOS ก็สามารถ เล่นสล็อตได้อย่างราบรื่น ระบบของเรา ได้รับการออกแบบให้รองรับ ระบบต่าง ๆ ไม่สำคัญว่าคุณ ใช้ มือถือ ใหม่หรือเก่า หรือ แม้แต่แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา เรื่องความเข้ากันได้
เล่นได้ทุกที่ทุกเวลา
ข้อดีของการเล่น PG Slot ก็คือ คุณสามารถ เล่นได้ทุกที่ทุกเวลา ไม่ว่าจะ เป็นที่บ้าน ออฟฟิศ หรือแม้แต่ ที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเกมได้ทันที และคุณไม่ต้อง กังวลเรื่องการโหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
ลองเล่นสล็อตแมชชีนฟรี
เพื่อให้ ผู้เล่นใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
การให้บริการและความปลอดภัย
PG Slot มุ่งมั่นในการบริการลูกค้าที่ดีที่สุด เรามี ทีมบริการที่พร้อมช่วยเหลือตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี คือ มี โปรโมชันและโบนัสมากมาย ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสชนะและสนุกกับเกมมากขึ้น
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ทดลองเล่นสล็อต
ทดลองปฏิบัติเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังมองหาความบันเทิงและโอกาสในการคว้ารางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งโอกาสที่คุ้มค่าศึกษา.ด้วยความขนาดใหญ่ของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถปฏิบัติและค้นหาเกมที่ต้องการได้อย่างง่ายดาย.
ไม่ว่าคุณจะถูกใจเกมสล็อตคลาสสิกหรือต้องการความแปลกใหม่, ทางเลือกรอกลับมาให้คุณสัมผัส. จากสล็อตที่มีหัวข้อมากมาย ไปจนถึงเกมที่มีฟีเจอร์พิเศษและเงินรางวัล, ผู้เล่นจะได้พบกับการทดลองเล่นที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการปฏิบัติสล็อตฟรี, คุณสามารถปฏิบัติวิธีการเล่นและค้นหากลยุทธ์ที่ต้องการก่อนสร้างรายได้ด้วยเงินจริง. นี่คือโอกาสที่จะศึกษากับเกมและปรับปรุงโอกาสในการชนะรางวัลใหญ่.
อย่าเลื่อนเวลา, เข้าไปกับการทดสอบสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินกับความสนใจ, ความสนุกสนาน และโอกาสชนะรางวัลมากมาย. กล้าก้าวไปเดินทางสู่ความสำเร็จลุล่วงของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
ทดลองเล่นสล็อต pg
ทดลอง เล่น สล็อต PG พร้อม เข้าไปสู่ ไปสู่ ยุค แห่ง ความเพลิดเพลิน ที่ ไร้ขอบเขต
เกี่ยวกับ นักพนัน ที่ คิดค้น ค้นหา อารมณ์ เกมที่แปลกใหม่, สล็อต PG เป็น ตัวเลือก ที่ ดึงดูดความสนใจ มาก. เนื่องจาก ความหลากหลาย ของ เกมสล็อตต่างๆ ที่ น่าทึ่ง และ น่าสนใจ, นักพนัน จะมีโอกาส ลองเล่น และ ลอง ตัวเกม ที่ ถูกใจ ความชอบการเล่น ของตนเอง.
แม้ว่า คุณ จะชื่นชอบ ความตื่นเต้น แบบทั่วไป หรือ สิ่งท้าทาย ใหม่ๆ, สล็อต PG จะมี ให้เลือกมากมาย. ตั้งแต่ สล็อตคลาสสิค ที่ คุ้นเคย ไปจนถึง ประเภทเกม ที่ ให้ ลักษณะพิเศษ และ โบนัสมากเป็นพิเศษ, ลูกค้า จะสามารถ ได้รับ ความรู้สึก ที่ ดึงดูดใจ และ ตื่นเต้น
อันเนื่องมาจาก การทดลองเล่น สล็อต PG ฟรี, ผู้เล่น จะสามารถ ทดลอง ขั้นตอนการเล่น และ ตรวจสอบ กลเม็ด ต่างๆ ก่อนหน้า เริ่มเล่น ด้วยเงินสด. เช่นนั้น เป็น ทางเลือก ที่ยอดเยี่ยม ที่จะ เตรียมความพร้อม และ ปรับปรุง ความเป็นไปได้ ในการ ชนะ รางวัลมหาศาล.
อย่าชักช้า, เข้าถึง ใน การเล่นทดลอง สล็อต PG เดี๋ยวนี้ และ พบเจอ การเล่น ที่ ไม่จำกัด! ทดลอง ความตื่นเต้น, ความเพลิดเพลิน และ โอกาส ในการ รับของรางวัล มหายิ่ง. เริ่มดำเนินการ ลงมือ สู่ ความสมหวัง ของคุณในวงการ เกมสล็อต ตั้งแต่วันนี้!
เกี่ยวกับ ไซต์ PG Slots มีความ มี ความได้เปรียบ หลายประการ เมื่อเทียบกับ คาสิโนแบบ ดั้งเดิม, อย่างเฉพาะเจาะจง ใน ปัจจุบัน. ข้อดีสำคัญ เหล่านี้ เช่น:
ความสะดวกสบาย: ผู้เล่น สามารถเข้าถึง สล็อตออนไลน์ได้ ทุกเวลา จาก ทุกสถานที่, ทำให้ ผู้เล่นสามารถ ทดลอง ได้ ทุกอย่าง ไม่จำเป็นต้อง ต้องเดินทาง ไปคาสิโนแบบ ดั้งเดิม ๆ
เกมหลากประเภท: สล็อตออนไลน์ มีการนำเสนอ ตัวเกม ที่ หลากหลายรูปแบบ, เช่น สล็อตคลาสสิค หรือ ตัวเกม ที่มี คุณสมบัติ และประโยชน์ พิเศษ, ไม่ทำ ความเหงา ในเกม
ส่วนลด และค่าตอบแทน: สล็อตออนไลน์ โดยทั่วไป ให้บริการ ส่วนลด และโบนัส เพื่อเพิ่ม โอกาส ในการ ชนะเกม และ ส่งเสริม ความผ่อนคลาย ให้กับเกม
ความเชื่อมั่น และ ความน่าเชื่อถือ: สล็อตออนไลน์ มักจะ ใช้ การรักษาความปลอดภัย ที่ ดี, และ เชื่อมั่นได้ ว่า ความเป็นส่วนตัว และ ธุรกรรมทางการเงิน จะได้รับ คุ้มครอง
บริการสนับสนุน: PG Slots มี ทีมงาน ที่มีคุณภาพ ที่มุ่งมั่น ช่วยเหลือ ตลอดเวลา
การเล่นบนมือถือ: สล็อต PG รองรับ การเล่นบนมือถือ, ทำให้ ผู้เล่นสามารถเข้าร่วม ตลอดเวลา
ทดลองเล่นโดยไม่เสียค่าใช้จ่าย: เกี่ยวกับ ผู้เล่นที่เพิ่งเริ่ม, PG ยังมี ทดลองเล่นโดยไม่เสียค่าใช้จ่าย เช่นกัน, เพื่อที่ ผู้เล่น ทำความเข้าใจ เทคนิคการเล่น และเข้าใจ เกมก่อน เล่นด้วยเงินจริง
สล็อต PG มีคุณสมบัติ คุณสมบัติที่ดี มากมาย ที่ ก่อให้เกิด ให้ได้รับความสนใจ ในปัจจุบันนี้, ส่งเสริม ระดับ ความผ่อนคลาย ให้กับเกมด้วย.
문 프린세스 100
Xiao Jing은 Qi Jingtong의 기념관을 Fang Jifan에게 보냈습니다.
pharmacy on line
diflucan prescription cost
Драгон Мани Казино https://krpb.ru – ваше место для азартных приключений! Наслаждайтесь широким выбором игр, щедрыми бонусами и захватывающими турнирами. Безопасность и честная игра гарантированы. Присоединяйтесь к нам и испытайте удачу в самом захватывающем онлайн-казино!
Famous French footballer Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com has become a global ambassador for Dior. The athlete will represent the men’s collections of creative director Kim Jones and the Sauvage fragrance, writes WWD. Mbappe’s appointment follows on from the start of the fashion house’s collaboration with the Paris Saint-Germain football club. Previously, Jones created a uniform for the team where Kylian is a player.
สล็อตเว็บโดยตรง — สามารถใช้ โทรศัพท์มือถือ แท็บเลต คอมฯ ฯลฯ เพื่อเล่น
ระบบสล็อตเว็บโดยตรง ของ พีจีสล็อต ได้รับการพัฒนาและอัปเดต เพื่อให้ รองรับการใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเลต หรือ คอมพิวเตอร์ส่วนตัว รุ่นใด
ที่ PG เราเข้าใจว่าผู้เล่นต้องการ จากผู้เล่น ในเรื่อง การใช้งานง่าย และ การเข้าถึงเกมคาสิโนที่รวดเร็ว เราจึง ใช้เทคโนโลยี HTML 5 ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ปัจจุบันนี้ มาพัฒนาเว็บไซต์ของเรากันเถอะ คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บไซต์ของเรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การรองรับอุปกรณ์หลายชนิด
ไม่ว่าคุณจะใช้ โทรศัพท์มือถือ ระบบ แอนดรอยด์ หรือ iOS ก็สามารถ เล่นสล็อตออนไลน์ได้ไม่มีสะดุด ระบบของเรา ออกแบบมาให้รองรับ ทุกระบบปฏิบัติการ ไม่สำคัญว่าคุณ มี มือถือ เครื่องใหม่หรือเครื่องเก่า หรือ แท็บเล็ตหรือโน้ตบุ๊ก ทุกอย่างก็สามารถ ใช้งานได้ดี ไม่มีปัญหา ในเรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
ข้อดีของการเล่น PG Slot คือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ ที่บ้าน ออฟฟิศ หรือแม้แต่ สถานที่สาธารณะ สิ่งที่คุณต้องมีคือ เน็ต คุณสามารถ เริ่มเล่นได้ทันที และคุณไม่ต้อง กังวลกับการดาวน์โหลด หรือติดตั้งโปรแกรมที่ ใช้พื้นที่บนอุปกรณ์ของคุณ
เล่นสล็อตฟรี
เพื่อให้ ผู้เล่นใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังมีบริการสล็อตฟรี คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
การบริการและความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี ก็คือ มี โปรโมชันและโบนัสมากมาย ไม่ว่าคุณจะเป็น ผู้เล่นใหม่หรือเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสชนะและความสนุกในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
การเผชิญหน้าการทดลองเล่นสล็อต PG บนเว็บวางเดิมพันไม่ผ่านเอเย่นต์: เปิดจักรวาลแห่งความตื่นเต้นที่ไม่มีที่สิ้นสุด
ในกรณีของนักพนันที่ตามหาประสบการณ์เกมแปลกใหม่ และคาดหวังเจอแหล่งเดิมพันที่มั่นคง, การทำการเกมสล็อต PG บนพอร์ทัลตรงนับว่าตัวเลือกที่น่าประทับใจอย่างมาก. เนื่องจากมีความแตกต่างของเกมสล็อตต่างๆที่มีให้เลือกสรรมากมาย, ผู้เล่นจะได้ประสบกับโลกแห่งความตื่นเต้นและความเพลิดเพลินที่ไร้ขีดจำกัด.
เว็บไซต์การเดิมพันตรงนี้ มอบการเล่นการเล่นเดิมพันที่ปลอดภัยแน่นอน น่าเชื่อถือ และตรงตามความต้องการของนักเสี่ยงโชคได้เป็นอย่างดี. ไม่ว่าคุณจะท่านจะติดใจเกมสล็อตแมชชีนแนวคลาสสิกที่คุ้นเคย หรืออยากทดลองเกมที่ไม่เหมือนใครที่มีคุณลักษณะพิเศษเฉพาะและโบนัสล้นหลาม, พอร์ทัลโดยตรงนี้ก็มีให้คัดสรรอย่างหลากหลายชนิด.
เนื่องจากมีระบบการลองเล่นสล็อต PG โดยไม่เสียค่าใช้จ่าย, ผู้เล่นจะได้โอกาสที่ดีทำความเข้าใจกระบวนการเล่นเกมและทดสอบเทคนิคต่างๆนาๆ ก่อนจะเริ่มใช้เงินลงทุนโดยใช้เงินจริง. การกระทำนี้นับว่าเป็นโอกาสอันวิเศษที่จะเพิ่มความพร้อมสรรพและเพิ่มโอกาสในการชิงรางวัลใหญ่ใหญ่.
ไม่ว่าท่านจะคุณจะปรารถนาความเพลิดเพลินที่คุ้นเคย หรือความท้าทายแปลกใหม่, สล็อต PG บนเว็บไซต์พนันไม่ผ่านเอเย่นต์ก็มีให้เลือกสรรอย่างมากมาย. ท่านจะได้พบเจอกับการเล่นการเล่นเกมที่น่าตื่นเต้นเร้าใจ น่าตื่นเต้น และสนุกเพลิดเพลินไปกับโอกาสดีในการได้รับรางวัลมหาศาลมหาศาล.
อย่าลังเล, ร่วมสนุกทดลองเล่นเล่นสล็อต PG บนแพลตฟอร์มเดิมพันตรงนี้ขณะนี้ และเจอโลกแห่งความบันเทิงแห่งความสุขที่ปลอดภัยแน่นอน น่าค้นหา และมีแต่ความเพลิดเพลินรอคอยคุณ. ประสบความเร้าใจ, ความสนุกเพลิดเพลิน และจังหวะในการชิงรางวัลใหญ่มหาศาล. เริ่มก้าวเข้าสู่การประสบความสำเร็จในวงการเกมออนไลน์เวลานี้!
https://rafofficial.com/?keyword=luck365
ทดลองเล่นสล็อต pg ฟรี
สล็อตเว็บตรง — ใช้ได้กับ สมาร์ทโฟน แท็บเล็ต คอมพิวเตอร์ส่วนตัว ฯลฯ เพื่อเล่น
ระบบสล็อตเว็บตรง ของ PG Slot ได้รับการพัฒนาและปรับปรุง เพื่อให้ รองรับการใช้ บนอุปกรณ์ที่หลากหลายได้อย่าง ครบถ้วน ไม่สำคัญว่าจะใช้ มือถือ แท็บเลต หรือ คอมพิวเตอร์ รุ่นไหน
ที่ PG Slot เราเข้าใจถึงความต้องการ ของลูกค้า ในเรื่อง ความสะดวกสบาย และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง นำ HTML 5 มาใช้ ซึ่งเป็น เทคโนโลยีที่ล้ำสมัย ในขณะนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเบราว์เซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บไซต์เรา คุณสามารถ เพลิดเพลินกับสล็อตแมชชีนได้ทันที
การรองรับอุปกรณ์หลายชนิด
ไม่ว่าคุณจะใช้ โทรศัพท์มือถือ ระบบ Android หรือ iOS ก็สามารถ เล่นสล็อตออนไลน์ได้ไม่มีสะดุด ระบบของเรา ออกแบบมาเพื่อรองรับ ระบบปฏิบัติการทั้งหมด ไม่สำคัญว่าคุณ กำลังใช้ โทรศัพท์ เครื่องใหม่หรือเครื่องเก่า หรือ แท็บเล็ตหรือโน้ตบุ๊ก ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา เรื่องความเข้ากันได้
สามารถเล่นได้ทุกที่ทุกเวลา
หนึ่งในข้อดีของการเล่นสล็อตกับ PG Slot ก็คือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ อยู่ที่บ้าน ออฟฟิศ หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเล่นได้ทันที และคุณไม่ต้อง ห่วงเรื่องการดาวน์โหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
ลองเล่นสล็อตแมชชีนฟรี
เพื่อให้ ผู้ใช้ใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังมีสล็อตทดลองฟรี คุณสามารถ ทดลองเล่นได้ทันทีโดยไม่ต้องสมัครหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
บริการและการรักษาความปลอดภัย
PG Slot มุ่งมั่นในการบริการลูกค้าที่ดีที่สุด เรามี ทีมงานพร้อมบริการคุณตลอดเวลา นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนบุคคลและธุรกรรมทางการเงินของคุณจะได้รับการปกป้องอย่างดีที่สุด
โปรโมชั่นและของรางวัลพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี ก็คือ มี โปรโมชั่นและโบนัสพิเศษมากมายสำหรับผู้เข้าร่วม ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือสมาชิกเก่า คุณสามารถ รับโปรโมชั่นและโบนัสต่างๆได้อย่างต่อเนื่อง สิ่งนี้จะ เพิ่มโอกาสชนะและความสนุกในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
ทดลองเล่นสล็อต pg เว็บ ตรง
ประสบการณ์การทดลองเล่นเกมสล็อต PG บนเว็บพนันโดยตรง: เปิดโลกแห่งความตื่นเต้นที่ไม่มีที่สิ้นสุด
เพื่อนักเสี่ยงโชคที่ตามหาการพบเจอเกมที่ไม่ซ้ำใคร และหวังค้นหาแหล่งพนันที่มีความน่าเชื่อถือ, การทดลองเกมสล็อต PG บนแพลตฟอร์มตรงถือเป็นตัวเลือกที่น่าดึงดูดอย่างมาก. เนื่องจากมีความหลากหลายมากมายของเกมสล็อตที่มีให้เลือกเล่นมากมาย, ผู้เล่นจะได้พบเจอกับโลกแห่งความรื่นเริงและความเพลิดเพลินที่ไม่จำกัด.
เว็บการเดิมพันตรงนี้ ให้การเล่นการเล่นเกมพนันที่ปลอดภัย เชื่อถือได้ และตรงตามความต้องการของนักเสี่ยงโชคได้เป็นอย่างดี. ไม่ว่าท่านจะคุณอาจจะโปรดปรานสล็อตแมชชีนแนวคลาสสิกที่รู้จักดี หรือต้องการลองเกมใหม่ที่มีคุณสมบัติน่าสนใจและรางวัลพิเศษล้นหลาม, พอร์ทัลตรงนี้นี้ก็มีให้เลือกอย่างมากมาย.
เนื่องจากมีระบบการสำรวจเกมสล็อตแมชชีน PG ฟรี, ผู้เล่นจะได้โอกาสทำความเข้าใจขั้นตอนเล่นเกมพนันและลองกลยุทธ์หลากหลาย ก่อนที่จะเริ่มลงทุนด้วยเงินทุนจริง. สิ่งนี้ถือเป็นโอกาสอันดีที่สุดที่จะสร้างเสริมความพร้อมและพัฒนาโอกาสในการได้รับโบนัสใหญ่.
ไม่ว่าท่านจะต้องการความสนุกสนานแบบดั้งเดิม หรือความท้าทายแปลกใหม่, เกมสล็อตแมชชีน PG บนเว็บไซต์พนันโดยตรงก็มีให้คัดสรรอย่างหลากหลายมากมาย. คุณจะได้พบเจอกับประสบการณ์การเล่นเดิมพันที่น่าตื่นเต้นเร้าใจ น่าตื่นเต้นเร้าใจ และมีความสุขไปกับโอกาสที่ดีในการชิงรางวัลใหญ่มหาศาล.
อย่ารอ, ร่วมเล่นลองเกมสล็อต PG บนแพลตฟอร์มเดิมพันตรงนี้ตอนนี้ และพบโลกแห่งความบันเทิงแห่งความตื่นเต้นที่มั่นคง น่าติดตาม และเต็มไปด้วยความสนุกสนานรอคอยคุณ. เผชิญความรื่นเริง, ความสุข และโอกาสที่ดีในการชิงรางวัลมหาศาล. เริ่มการเดินทางเดินทางสู่การเป็นผู้ชนะในวงการเกมออนไลน์แล้ววันนี้!
dexamethasone 0.75
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
Заходите на наш ресурс, где вы найдете множество полезных статей на тему приемки недвижимости в новостройке или покупки квартиры без отделки. Узнайте, как защитить себя от ненадёжных застройщиков, какие проверки провести перед покупкой жилья, и о многом другом!
https://citadel-ca.ru
https://gaonrentcar.com/?keyword=microsoft-office-365
pharmacy2u propecia
kroger pharmacy simvastatin
Скачать свежие новинки песен https://muzfo.net 2024 года ежедневно. Наслаждайтесь комфортным прослушиванием, скачивайте музыку за пару кликов на сайте.
sa gaming
הימורי ספורטיביים – הימורים באינטרנט
הימורי ספורט הפכו לאחד התחומים המתפתחים ביותר בהימורים באינטרנט. משתתפים יכולים להתערב על תוצאות של אירועים ספורט נפוצים כמו כדורגל, כדור סל, טניס ועוד. האפשרויות להתערבות הן מרובות, וביניהן תוצאתו המשחק, מספר השערים, מספר הפעמים ועוד. להלן דוגמאות של למשחקים נפוצים במיוחד שעליהם ניתן להתערב:
כדורגל: ליגת האלופות, מונדיאל, ליגות מקומיות
כדור סל: NBA, ליגת יורוליג, טורנירים בינלאומיים
טניס: טורניר ווימבלדון, אליפות ארה”ב הפתוחה, רולאן גארוס
פוקר ברשת – הימור ברשת
פוקר באינטרנט הוא אחד ממשחקי ההימור המוכרים ביותר בימינו. שחקנים מסוגלים להתחרות מול יריבים מרחבי העולם בסוגי גרסאות של המשחק , כגון טקסס הולדם, Omaha, סטאד ועוד. ניתן לגלות טורנירים ומשחקי קש במגוון רמות ואפשרויות מגוונות. אתרי פוקר המובילים מציעים גם:
מבחר רב של וריאציות פוקר
טורנירים שבועיות וחודשיות עם פרסים כספיים גבוהים
שולחנות המשחק למשחקים מהירים ולטווח הארוך
תוכניות נאמנות ומועדוני VIP בלעדיות
בטיחות והוגנות
כאשר הבחירה פלטפורמה להימורים ברשת, חשוב לבחור גם אתרי הימורים מורשים ומפוקחים המציעים גם סביבה משחק בטוחה והגיונית. אתרים אלו עושים שימוש בטכנולוגיות הצפנה מתקדמות להבטחה על נתונים אישיים ופיננסי, וגם באמצעות תוכנות גנרטור מספרים אקראיים (RNG) כדי לוודא הגינות במשחקים במשחקי ההימורים.
בנוסף, חשוב לשחק באופן אחראית תוך קביעת מגבלות הימור אישיות. רוב האתרים מאפשרים למשתתפים להגדיר מגבלות להפסדים ופעילות, כמו גם לנצל כלים נגד התמכרויות. הימרו בתבונה ואל גם תרדפו אחר הפסדים.
המדריך השלם למשחקי קזינו באינטרנט, משחקי ספורט ופוקר ברשת
הימורים באינטרנט מציעים עולם שלם של הזדמנויות מרתקות לשחקנים, מתחיל מקזינו אונליין וכל משחקי ספורט ופוקר באינטרנט. בעת בחירת פלטפורמת הימורים, הקפידו לבחור אתרי הימורים המפוקחים המציעים סביבה למשחק מאובטחת והוגנת. זכרו גם לשחק תמיד באופן אחראי תמיד ואחראי – משחקי ההימורים ברשת אמורים להיות מבדרים ולא ליצור לבעיות פיננסיות או חברתיות.
интернет эквайринг https://internet-ekvajring.kz – безопасные и эффективные платежные решения для вашего бизнеса.
Агентство по продвижению телеграм-каналов https://883666b.com в Москве специализируется на разработке и реализации стратегий для увеличения аудитории и вовлечённости подписчиков на телеграм-каналах. Эксперты агентства помогают клиентам определить целевую аудиторию, разрабатывают контент-планы и рекламные кампании. Услуги включают рекламу посевами, таргет рекламой, анализ конкурентов, SEO-оптимизацию контента.
ทดลองดำเนินการเล่นสล็อต และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร!
สำหรับนักพนันที่กำลังมองหาความบันเทิงและโอกาสในการคว้ารางวัลมหาศาล สล็อตออนไลน์เป็นอีกหนึ่งโอกาสที่คุ้มค่าศึกษา.ด้วยความจำนวนมากของเกมสล็อตที่น่าตื่นเต้น ผู้เล่นสามารถปฏิบัติและค้นหาเกมที่ถูกใจได้อย่างง่ายดาย.
ไม่ว่าคุณจะชื่นชอบเกมสล็อตคลาสสิกหรือต้องการความท้าทายใหม่, โอกาสรอล้ำหน้าให้คุณสัมผัส. จากสล็อตที่มีธีมมากมาย ไปจนถึงเกมที่มีลักษณะพิเศษและรางวัล, ผู้เล่นจะได้พบกับการทดลองเล่นที่น่าตื่นเต้นและน่าติดตาม.
ด้วยการทดสอบสล็อตฟรี, คุณสามารถเรียนรู้วิธีการเล่นและค้นตัดสินใจกลยุทธ์ที่เหมาะสมก่อนลงทุนด้วยเงินจริง. นี่คือโอกาสที่ดีที่จะทำความคุ้นเคยกับเกมและประยุกต์โอกาสในการชนะรางวัลใหญ่.
อย่ารอช้า, ร่วมกับการปฏิบัติสล็อตออนไลน์วันนี้ และค้นพบประสบการณ์การเล่นเกมที่ไม่เหมือนใคร! เพลิดเพลินความตื่นเต้น, ความร่าเริง และโอกาสมากมายชนะรางวัลใหญ่. ก้าวสู่ความสำเร็จเดินทางสู่ความสมหวังของคุณในวงการสล็อตออนไลน์แล้ววันนี้!
프라 그마 틱 슬롯 사이트
Fang Jifan은 재빨리 고개를 끄덕였습니다. “폐하에게는 명확한 보상과 처벌이 있으며 매우 훌륭합니다.”
פוקר באינטרנט
הימורי ספורטיביים – הימורים באינטרנט
הימורי ספורטיביים הפכו לאחד הענפים הצומחים ביותר בהימורים באינטרנט. שחקנים מסוגלים להמר על תוצאות של אירועים ספורטיביים מוכרים כמו כדורגל, כדורסל, משחק הטניס ועוד. האופציות להימור הן רבות, וביניהן תוצאת המשחק, מספר השערים, כמות הפעמים ועוד. הבא דוגמאות למשחקי נפוצים במיוחד שעליהם ניתן להתערב:
כדורגל: ליגת אלופות, מונדיאל, ליגות אזוריות
כדור סל: NBA, ליגת יורוליג, תחרויות בינלאומיות
משחק הטניס: טורניר ווימבלדון, אליפות ארה”ב הפתוחה, אליפות צרפת הפתוחה
פוקר ברשת ברשת – הימור ברשת
משחק הפוקר ברשת הוא אחד ממשחקי ההימורים הפופולריים ביותר כיום. משתתפים יכולים להתמודד נגד יריבים מכל רחבי תבל במגוון סוגי משחק , לדוגמה טקסס הולדם, Omaha, Stud ועוד. ניתן לגלות תחרויות ומשחקי במבחר דרגות ואפשרויות שונות. אתרי הפוקר המובילים מציעים:
מבחר רב של וריאציות המשחק פוקר
תחרויות שבועיים וחודשיים עם פרסים כספיים גבוהים
שולחנות המשחק למשחקים מהירים ולטווח הארוך
תוכניות נאמנות ומועדוני VIP VIP עם הטבות
בטיחות ואבטחה והוגנות
כאשר בוחרים פלטפורמה להימורים ברשת, חשוב לבחור גם אתרי הימורים מורשים המפוקחים המציעים סביבת למשחק מאובטחת והוגנת. אתרים אלו משתמשים בטכנולוגיות אבטחה מתקדמות להגנה על מידע אישי ופיננסיים, וכן באמצעות תוכנות גנרטור מספרים אקראיים (RNG) כדי לוודא הגינות במשחקים במשחקים.
בנוסף, הכרחי לשחק בצורה אחראית תוך קביעת מגבלות הימור אישיות של השחקן. מרבית האתרים מאפשרים למשתתפים להגדיר מגבלות להפסדים ופעילות, כמו גם לנצל כלים נגד התמכרויות. שחקו בתבונה ואל תרדפו גם אחר הפסדים.
המדריך השלם לקזינו באינטרנט, הימורי ספורט ופוקר באינטרנט
הימורים ברשת מציעים גם עולם שלם של הזדמנויות מרתקות למשתתפים, החל מקזינו אונליין וכל בהימורי ספורט ופוקר באינטרנט. בעת הבחירה בפלטפורמת הימורים, הקפידו לבחור אתרים מפוקחים המציעים גם סביבה משחק מאובטחת והוגנת. זכרו לשחק באופן אחראי תמיד ואחראי – ההימורים ברשת אמורים להיות מבדרים ולא לגרום בעיות פיננסיות או חברתיות.
buy rx tretinoin gel
https://rushmorgan.com/?keyword=eslot
rtp slot
Здесь вы найдете разнообразный видео контент ялта интурист 2021
Привет всем!
Недавно мы решили обновить напольные покрытия в доме. На портале https://cephey.ru/netcat/editors/ckeditor/plugins/docprops/dialogs/docs/4/3/353_glavnie_osobennosti_raboti_elektroerozionnih.html мы нашли полезную информацию, которая помогла сделать правильный выбор. Описания, фото и характеристики покрытий позволили понять отличия и преимущества каждого типа. Благодаря этим рекомендациям мы выбрали доступные по цене натуральные покрытия российского производства и успешно завершили укладку стяжки своими руками, обеспечив безопасность и качественный ремонт.
напольное покрытие
модернизация DK77
фальшпол
напольное покрытие
виниловый ламинат на стене
цена укладки виниловой плитки
кварцвинил укладка
Удачи!
жк купить квартиру от застройщика https://nedvizhimost47.ru
купить квартиру недорого купить квартиру в казани
Преимущества использования теневого плинтуса
скрытый плинтус теневой https://msk-alyuminievyj-tenevoj-plintus.ru/ .
Скачать музыку https://musiciansfix.com высокого качества в любом жанре. Огромный выбор треков от классики до новинок поможет вам создать идеальный плейлист. Наслаждайтесь любимыми композициями и открывайте для себя новые музыкальные горизонты. Присоединяйтесь и начните скачивать музыку прямо сейчас!
купить квартиру от застройщика недорого https://novostroyka47.ru
купить квартиру в казани от застройщика купить квартиру в новостройке от застройщика
Good day!
Sustainability & Eco-Friendly Living! Live a greener life with our sustainability tips. Get advice on reducing waste, conserving energy, and making eco-friendly choices.
Very good thematic site – https://gsroups.com
vegetarian recipes
travel destinations guide
finance
news portal
travel blogs
travel
dessert recipes
stress management tips
Goog luck!
ciprofloxacin mail online
קזינו אונליין
הימורי ספורט – הימורים באינטרנט
הימור ספורט נהיו לאחד הענפים המשגשגים ביותר בהימורים באינטרנט. שחקנים מסוגלים להמר על תוצאת של אירועים ספורטיביים נפוצים למשל כדור רגל, כדור סל, משחק הטניס ועוד. האופציות להימור הן רבות, וביניהן תוצאת המאבק, כמות הגולים, מספר הפעמים ועוד. להלן דוגמאות למשחקים נפוצים עליהם אפשרי להמר:
כדורגל: ליגת אלופות, גביע העולם, ליגות מקומיות
כדורסל: ליגת NBA, ליגת יורוליג, תחרויות בינלאומיות
משחק הטניס: ווימבלדון, US Open, אליפות צרפת הפתוחה
פוקר ברשת – הימורים באינטרנט
משחק הפוקר באינטרנט הוא אחד מהמשחקים ההימורים הפופולריים ביותר בימינו. משתתפים מסוגלים להתמודד מול יריבים מרחבי העולם במגוון וריאציות משחק , לדוגמה טקסס הולדם, אומהה, Stud ועוד. אפשר למצוא טורנירים ומשחקי קש במגוון רמות ואפשרויות הימור שונות. אתרי פוקר המובילים מציעים גם:
מגוון רחב של וריאציות פוקר
טורנירים שבועיות וחודשיות עם פרסים כספיים
שולחנות המשחק למשחקים מהירים ולטווח הארוך
תוכניות נאמנות ללקוחות ומועדוני VIP עם הטבות יחודיות
בטיחות והוגנות
כאשר הבחירה בפלטפורמה להימורים, חשוב לבחור אתרי הימורים מורשים ומפוקחים המציעים גם סביבה משחק מאובטחת והגיונית. אתרים אלו משתמשים בטכנולוגיית אבטחה מתקדמת להגנה על מידע אישי ופיננסיים, וגם באמצעות תוכנות גנרטור מספרים רנדומליים (RNG) כדי להבטיח הגינות במשחקים במשחקי ההימורים.
בנוסף, חשוב לשחק בצורה אחראית תוך כדי קביעת מגבלות אישיות הימור אישיות של השחקן. מרבית האתרים מאפשרים למשתתפים להגדיר מגבלות להפסדים ופעילויות, כמו גם להשתמש ב- כלים נגד התמכרויות. שחק בתבונה ואל גם תרדפו גם אחר הפסדים.
המדריך המלא למשחקי קזינו אונליין, הימורי ספורט ופוקר באינטרנט באינטרנט
הימורים ברשת מציעים גם עולם שלם של הזדמנויות מרתקות לשחקנים, מתחיל מקזינו באינטרנט וכל בהימורי ספורט ופוקר באינטרנט. בזמן הבחירה בפלטפורמת הימורים, חשוב לבחור אתרי הימורים המפוקחים המציעים סביבה משחק בטוחה והוגנת. זכרו לשחק באופן אחראי תמיד ואחראי – משחקי ההימורים באינטרנט אמורים להיות מבדרים ולא לגרום בעיות כלכליות או גם חברתיים.
Good day!
Travel Photography Tips! Capture your travels like a pro. Get our top photography tips and techniques to take stunning photos on your adventures.
Very good thematic site – https://gsroups.com
cooking techniques
travel tips for solo travelers
educational news
self-care tips
relationship advice
travel packing tips
travel apps
news broadcast
Goog luck!
הימורי ספורט
הימורי ספורטיביים – הימורים באינטרנט
הימור ספורטיביים הפכו לאחד התחומים הצומחים ביותר בהימור באינטרנט. שחקנים מסוגלים להמר על תוצאת של אירועים ספורט מוכרים כמו כדורגל, כדורסל, טניס ועוד. האופציות להימור הן רבות, וביניהן תוצאת המאבק, מספר הגולים, כמות הפעמים ועוד. הבא דוגמאות למשחקי נפוצים במיוחד עליהם אפשרי להמר:
כדור רגל: ליגת האלופות, מונדיאל, ליגות מקומיות
כדור סל: NBA, ליגת יורוליג, תחרויות בינלאומיות
טניס: ווימבלדון, US Open, רולאן גארוס
פוקר ברשת באינטרנט – הימורים ברשת
משחק הפוקר ברשת הוא אחד ממשחקי ההימורים הנפוצים ביותר בימינו. שחקנים יכולים להתמודד מול יריבים מרחבי העולם בסוגי סוגי של המשחק , כגון טקסס הולדם, אומהה, סטאד ועוד. ניתן למצוא תחרויות ומשחקי במבחר דרגות ואפשרויות הימור שונות. אתרי הפוקר המובילים מציעים:
מבחר רב של וריאציות פוקר
תחרויות שבועיים וחודשיות עם פרסים כספיים גבוהים
שולחנות המשחק למשחקים מהירים ולטווח ארוך
תוכניות נאמנות ללקוחות ומועדוני VIP עם הטבות בלעדיות
בטיחות ואבטחה והוגנות
כאשר הבחירה פלטפורמה להימורים ברשת, חיוני לבחור גם אתרים מורשים ומפוקחים המציעים גם סביבה למשחק מאובטחת והגיונית. אתרים אלה עושים שימוש בטכנולוגיית הצפנה מתקדמות להבטחה על מידע אישי ופיננסי, וגם בתוכנות מחולל מספרים אקראיים (RNG) כדי לוודא הגינות במשחקים.
בנוסף, הכרחי לשחק גם באופן אחראי תוך כדי הגדרת מגבלות אישיות הימור אישיות. מרבית האתרים מאפשרים גם למשתתפים לקבוע מגבלות הפסד ופעילות, כמו גם להשתמש ב- כלים למניעת התמכרות. שחק בתבונה ואל גם תרדפו גם אחר הפסדים.
המדריך השלם לקזינו באינטרנט, הימורי ספורט ופוקר ברשת
הימורים באינטרנט מציעים גם עולם שלם של של הזדמנויות מרתקות לשחקנים, מתחיל מקזינו אונליין וגם בהימורי ספורט ופוקר באינטרנט. בזמן הבחירה פלטפורמת הימורים, חשוב לבחור אתרים מפוקחים המציעים סביבת למשחק בטוחה והוגנת. זכרו לשחק תמיד בצורה אחראית תמיד – משחקי ההימורים ברשת נועדו להיות מבדרים ומהנים ולא גם ליצור בעיות כלכליות או גם חברתיות.
https://medium.com/@momejar21741/pg-59490dd058fd
สล็อตเว็บตรง — ใช้ได้กับ มือถือ แท็บเล็ต คอมพิวเตอร์ส่วนตัว ฯลฯ ในการเล่น
ระบบสล็อตตรงจากเว็บ ของ พีจีสล็อต ได้รับการพัฒนาและปรับปรุง เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง สมบูรณ์ ไม่สำคัญว่าจะใช้ มือถือ แท็บเล็ต หรือ คอมพิวเตอร์ส่วนตัว รุ่นไหน
ที่ PG เราเข้าใจถึงสิ่งที่ผู้เล่นต้องการ ของลูกค้า ในเรื่อง ความสะดวกสบาย และ ความรวดเร็วในการเข้าถึงเกมคาสิโนออนไลน์ เราจึง ใช้ HTML 5 ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ในตอนนี้ พัฒนาเว็บของเรา คุณจึงไม่ต้อง ดาวน์โหลดแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดบราวเซอร์ บนอุปกรณ์ที่ คุณมีอยู่ และเยี่ยมชม เว็บของเรา คุณสามารถ สนุกกับสล็อตได้ทันที
การรองรับอุปกรณ์หลายชนิด
ไม่ว่าคุณจะใช้ มือถือ ระบบ แอนดรอยด์ หรือ ไอโอเอส ก็สามารถ เล่นสล็อตออนไลน์ได้ไม่มีสะดุด ระบบของเรา ออกแบบมาให้รองรับ ทุกระบบปฏิบัติการ ไม่สำคัญว่าคุณ มี มือถือ รุ่นใหม่หรือรุ่นเก่า หรือ แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา ในเรื่องความเข้ากันได้
เล่นได้ทุกที่ทุกเวลา
ข้อดีอย่างหนึ่งของการเล่นเว็บสล็อตอย่าง PG Slot นั่นคือ คุณสามารถ เล่นได้ทุกเวลา ไม่ว่าจะ อยู่ที่บ้าน ออฟฟิศ หรือแม้แต่ สถานที่สาธารณะ สิ่งที่คุณต้องมีคือ การเชื่อมต่ออินเทอร์เน็ต คุณสามารถ เริ่มเล่นได้ทันที และคุณไม่ต้อง ห่วงเรื่องการดาวน์โหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
ลองเล่นสล็อตแมชชีนฟรี
เพื่อให้ ผู้เล่นที่ใหม่ ได้ลองและรู้จักเกมสล็อตของเรา PG Slot ยังเสนอบริการสล็อตทดลองฟรีอีกด้วย คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ เล่นฟรีนี้จะช่วยให้คุณเข้าใจวิธีเล่นและรู้จักเกมก่อนลงเดิมพันจริง
การให้บริการและความปลอดภัย
PG Slot มุ่งมั่นที่จะให้บริการที่ดีที่สุดแก่ลูกค้า เรามี ทีมงานมืออาชีพพร้อมให้บริการและช่วยเหลือคุณตลอด 24 ชั่วโมง นอกจากนี้เรายังมี การรักษาความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลและการเงินของคุณจะปลอดภัย
โปรโมชั่นและของรางวัลพิเศษ
การเล่นสล็อตกับ PG Slot ยังมีข้อดี ก็คือ มี โปรโมชันและโบนัสมากมาย ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสชนะและสนุกกับเกมมากขึ้น
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
average cost of azithromycin
Проведение независимой строительной экспертизы — сложный процесс, требующий глубоких знаний. Наши специалисты обладают всеми необходимыми навыками, а их заключения часто служат основой для принятия верных стратегических решений. Строительно-техническая экспертиза https://stroytehexp.ru позволяет выявить факторы, вызвавшие ухудшение эксплуатационных характеристик объектов, проверить соответствие возведённых зданий градостроительным нормам.
The story of Mbappe’s asma-online.org rise to fame is as remarkable as his on-field feats. Mbappe’s journey from local pitches to global arenas was meteoric. His early days at AS Monaco showcased his prodigious talent, with his blistering speed and fearless dribbling dismantling opposition defenses.
Pin up в моде: актуальные тенденции и идеи, для яркого вида
pin up casino como funciona pin up casino como funciona .
provigil order online canada
Информационный ресурс https://ardma.ru, посвящен бизнесу, финансам, инвестициям и криптовалютам. Сайт предлагает экспертные статьи, аналитические отчеты, стратегии и советы для предпринимателей и инвесторов. Здесь можно найти новости и обзоры о бизнесе, маркетинге, трейдинге, а также практические рекомендации по различным видам заработка и управлению финансами.
https://medium.com/@momejar21741/pg-59490dd058fd
สล็อตตรงจากเว็บ — ใช้ มือถือ แท็บเลต คอมพิวเตอร์ส่วนตัว ฯลฯ ในการเล่น
ระบบสล็อตตรงจากเว็บ ของ PG ได้รับการพัฒนาและอัปเดต เพื่อให้ สามารถใช้งาน บนอุปกรณ์ที่หลากหลายได้อย่าง เต็มที่ ไม่สำคัญว่าจะใช้ สมาร์ทโฟน แท็บเลต หรือ คอมพิวเตอร์ รุ่นไหน
ที่ PG เราเข้าใจถึงสิ่งที่ผู้เล่นต้องการ จากผู้เล่น ในเรื่อง ความสะดวก และ การเข้าถึงเกมออนไลน์อย่างรวดเร็ว เราจึง ใช้เทคโนโลยี HTML 5 ซึ่งเป็น เทคโนโลยีที่ทันสมัยที่สุด ปัจจุบันนี้ มาใช้พัฒนาเว็บไซต์ คุณจึงไม่ต้อง ติดตั้งแอป หรือติดตั้งโปรแกรมเพิ่มเติม เพียง เปิดเว็บเบราว์เซอร์ บนอุปกรณ์ที่ คุณใช้อยู่ และเยี่ยมชม เว็บของเรา คุณสามารถ เล่นเกมสล็อตได้ทันที
การสนับสนุนหลายอุปกรณ์
ไม่ว่าคุณจะใช้ สมาร์ทโฟน ระบบ Android หรือ iOS ก็สามารถ เล่นเกมสล็อตได้อย่างไม่มีปัญหา ระบบของเรา ได้รับการออกแบบให้รองรับ ระบบต่าง ๆ ไม่สำคัญว่าคุณ มี สมาร์ทโฟน ใหม่หรือเก่า หรือ แม้แต่แท็บเล็ตหรือแล็ปท็อป ทุกอย่างก็สามารถ ใช้งานได้อย่างไม่มีปัญหา ไม่มีปัญหา เรื่องความเข้ากันได้
เล่นได้ทุกที่ทุกเวลา
ข้อดีของการเล่น PG Slot นั่นคือ คุณสามารถ เล่นได้ตลอดเวลา ไม่ว่าจะ อยู่ที่บ้าน ที่ออฟฟิศ หรือแม้แต่ ในที่สาธารณะ สิ่งที่คุณต้องมีคือ อินเทอร์เน็ต คุณสามารถ เล่นเกมได้ทันที และคุณไม่ต้อง กังวลเรื่องการโหลด หรือติดตั้งโปรแกรมที่ เปลืองพื้นที่อุปกรณ์
เล่นสล็อตฟรี
เพื่อให้ ผู้เล่นที่ใหม่ ได้ลองเล่นและสัมผัสเกมสล็อตของเรา PG Slot ยังมีสล็อตทดลองฟรี คุณสามารถ เริ่มเล่นได้ทันทีโดยไม่ต้องลงทะเบียนหรือฝากเงิน การ ทดลองเล่นสล็อตนี้จะช่วยให้คุณรู้จักวิธีการเล่นและเข้าใจเกมก่อนเดิมพันด้วยเงินจริง
การให้บริการและความปลอดภัย
PG Slot ตั้งใจให้บริการที่ดีที่สุดกับลูกค้า เรามี ทีมบริการที่พร้อมช่วยเหลือตลอด 24 ชั่วโมง นอกจากนี้เรายังมี ระบบความปลอดภัยที่ทันสมัย ด้วยวิธีนี้ คุณจึงมั่นใจได้ว่า ข้อมูลส่วนตัวและการเงินของคุณจะปลอดภัย
โปรโมชันและโบนัส
อีกข้อดีของการเล่นสล็อตกับ PG Slot คือ มี โปรโมชันและโบนัสมากมาย ไม่ว่าคุณจะเป็น สมาชิกใหม่หรือเก่า คุณสามารถ รับโปรโมชันและโบนัสได้เรื่อย ๆ สิ่งนี้จะ เพิ่มโอกาสในการชนะและเพิ่มความเพลิดเพลินในเกม
สรุปการเล่นสล็อตเว็บที่ PG Slot ถือเป็นการลงทุนที่คุ้มค่า คุณจะไม่เพียงได้รับความสุขและความสะดวกสบายจากเกมเท่านั้น แต่คุณยังมีโอกาสลุ้นรับรางวัลและโบนัสมากมายอีกด้วย ไม่สำคัญว่าจะใช้โทรศัพท์มือถือ แท็บเล็ต หรือคอมพิวเตอร์รุ่นใด สามารถมาร่วมสนุกกับเราได้เลยตอนนี้ อย่ารอช้า ลงทะเบียนและเริ่มเล่นสล็อตกับ PG Slot วันนี้!
Real Madrid midfielder Rodrigo https://rodrygo.prostoprosport-ar.com gave Madrid the lead in the Champions League quarter-final first leg against Manchester City. The meeting takes place in Madrid. Rodrigo scored in the 14th minute after a pass from Vinicius Junior.
южный парк смотреть бесплатно в хорошем качестве https://southpark-serial.ru
южный парк смотреть онлайн на русском https://southpark-serial.ru
doxycycline uk
купить квартиру в казани купить квартиру в казани новостройка от застройщика
купить квартиру в новостройке от застройщика https://nedvizhimost-47.ru
Hi all!
Beauty & Fashion Tips! Stay stylish and confident with our beauty and fashion advice. Get tips on skincare, makeup, clothing, and more.
Very good thematic site – https://mail-grups.com
travel planning
travel news
nutrition tips
travel apps
long-haul travel
healthy eating
news outlet
self-care tips
Goog luck!
Карьерный коуч https://vminske.by/fashion/kto-takie-karernye-konsultanty — эксперт рынка труда, который помогает людям определить свои карьерные цели, развиваться в выбранной области и достигать успеха в профессиональной деятельности.
купить квартиру в новостройке от застройщика https://kupit-kvartiru47.ru
жк купить квартиру от застройщика https://kupit-kvartiru47.ru
сео оптимизация сайта https://seo-prodvizhenye-kazan.ru
заказать сео продвижение сайта сео оптимизация
комплексное seo продвижение сайтов https://seo-prodvizhenye-kazan.ru
раскрутка сайта seo https://prodvizhenie-saytov43.ru
создание и продвижение сайта seo продвижение
сео продвижение сайтов заказать seo продвижение сайта
Hi all!
Global Perspectives! Gain a broader understanding of world events with news from different perspectives. See how stories unfold in various parts of the world.
Very good thematic site – https://mail-grups.com
leadership
travel experiences
techniques
long-haul travel
seasonal ingredients
competitiveness
budget travel tips
gluten-free recipes
Goog luck!
южный парк смотреть онлайн https://southpark-serial.ru
south park южный парк
южный парк смотреть онлайн бесплатно южный парк 1 сезон
Любому человеку рано или поздно приходится пользоваться услугами стоматологических клиник. Ни для кого не секрет, что лечение зубов и последующее протезирование – процедуры довольно дорогостоящие, не все граждане могут позволить себе их оплатить, если вам необходимо стоматология лот цены мы Вам обязательно поможем.
Особенности
Благодаря услугам, которые предлагает населению стоматология Маэстро, люди разного финансового достатка имеют возможность не только поддерживать здоровье полости рта, но и проходить все необходимые процедуры. Цены на лечение зубов и протезирование значительно ниже, чем в других медучреждениях. Несмотря на то, что клиника работает для широких слоев населения, пациенты получают полный перечень услуг, используя современное оборудование и качественные материалы. Жителям доступны следующие процедуры:
• профилактика полости рта;
• лечение зубов с использованием различных методов;
• полная диагностика;
• профессиональная чистка;
• отбеливание;
• протезирование.
Сотрудники учреждения соблюдают все санитарные нормы, а для тщательной дезинфекции и стерилизации инструментов предусмотрено современное оборудование.
Преимущества
Востребованность бюджетной стоматологии объясняется рядом преимуществ. Во-первых, в клинике трудятся опытные высококвалифицированные сотрудники. Во-вторых, к каждому пациенту врач находит подход. В-третьих, кабинеты оснащены всем необходимым оборудованием, в работе используют только качественные безопасные материалы. В-четвертых, все виды протезирования будут проведены в сжатые сроки. Многие клиники получают субсидии от государства, что позволяет существенно сократить расходы. Кроме того, некоторые стоматологии сотрудничают со страховыми компаниями, поэтому у пациентов появляется возможность получить услуги по полюсу ОМС. Пациенты получают консультацию по профилактике заболеваний полости рта. Врачи после тщательного осмотра составляют индивидуальный план лечения, с помощью которого удается добиться наилучшего результата. Более доступные цены достигаются не только благодаря государственному финансированию, но и оптимизации расходов.
Благодаря стоматологии Маэстро, человек с небольшим достатком может не только вылечить зубы, но и поддерживать здоровье ротовой полости. Теперь любой человек может не откладывать поход к стоматологу, выбирая доступное качественное обслуживание.
южный парк смотреть онлайн бесплатно на русском https://southpark-serial.ru
dexamethasone medicine
pin-up kazino: Pin Up Azerbaycan ?Onlayn Kazino – Pin Up Azerbaycan ?Onlayn Kazino
https://autolux-azerbaijan.com/# Pin up 306 casino
modafinil buy from india
pin-up kazino: pin-up 141 casino – pin-up360
You actually suggested that really well!|
https://autolux-azerbaijan.com/# Pin Up Azerbaycan ?Onlayn Kazino
Pin Up Kazino ?Onlayn: Pin up 306 casino – Pin up 306 casino
pin-up 141 casino: pin-up 141 casino – Pin up 306 casino
https://autolux-azerbaijan.com/# Pin Up
ла2 топ сервера интерлюд
Сервера ла2
ла2 топ сервера
Анонсы л2
999 슬롯
인근의 다른 해상 선박에 비해 이 선박은 크기가 더 큽니다.
Pin Up Kazino ?Onlayn: Pin Up Azerbaycan – pin-up360
Vinicius Junior https://viniciusjunior.prostoprosport-ar.com is a Brazilian and Spanish footballer who plays as a striker for Real Madrid and the Brazilian national team. Junior became the first player in the history of Los Blancos, born in 2000, to play an official match and score a goal.
Kylian Mbappe https://kylianmbappe.prostoprosport-ar.com is a French footballer, striker for Paris Saint-Germain and captain of the French national team. He began playing football in the semi-professional club Bondi, which plays in the lower leagues of France. He was noticed by Monaco scouts, which he joined in 2015 and that same year, at the age of 16, he made his debut for the Monegasques. The youngest debutant and goal scorer in the club’s history.
台灣線上娛樂城是指通過互聯網提供賭博和娛樂服務的平台。這些平台主要針對台灣用戶,但實際上可能在境外運營。以下是一些關於台灣線上娛樂城的重要信息:
1. 服務內容:
– 線上賭場遊戲(如老虎機、撲克、輪盤等)
– 體育博彩
– 彩票遊戲
– 真人荷官遊戲
2. 特點:
– 全天候24小時提供服務
– 可通過電腦或移動設備訪問
– 常提供優惠活動和獎金來吸引玩家
3. 支付方式:
– 常見支付方式包括銀行轉賬、電子錢包等
– 部分平台可能接受加密貨幣
4. 法律狀況:
– 在台灣,線上賭博通常是非法的
– 許多線上娛樂城實際上是在國外註冊運營
5. 風險:
– 由於缺乏有效監管,玩家可能面臨財務風險
– 存在詐騙和不公平遊戲的可能性
– 可能導致賭博成癮問題
6. 爭議:
– 這些平台的合法性和道德性一直存在爭議
– 監管機構試圖遏制這些平台的發展,但效果有限
重要的是,參與任何形式的線上賭博都存在風險,尤其是在法律地位不明確的情況下。建議公眾謹慎對待,並了解相關法律和潛在風險。
如果您想了解更多具體方面,例如如何識別和避免相關風險,我可以提供更多信息。
https://autolux-azerbaijan.com/# pin-up 141 casino
金星娛樂城
Karim Benzema https://karimbenzema.prostoprosport-ar.com is a French footballer who plays as a striker for the Saudi Arabian club Al-Ittihad. He played for the French national team, for which he played 97 matches and scored 37 goals. At the age of 17, he became one of the best reserve players, scoring three dozen goals per season.
Victor James Osimhen https://victorosimhen.prostoprosport-ar.com is a Nigerian footballer who plays as a forward for the Italian club Napoli and the Nigerian national team. In 2015, he was recognized as the best football player in Africa among players under 17 according to the Confederation of African Football.
pin-up kazino: Pin Up – Pin Up Azerbaycan ?Onlayn Kazino
https://autolux-azerbaijan.com/# Pin Up Azerbaycan
Hi all!
Personalized News Feed! Customize your news experience with a personalized feed. Follow topics and categories that interest you the most.
Brunch Like a Pro! Make your weekends special with our brunch recipes. From fluffy pancakes to savory eggs benedict, find everything you need to brunch like a pro.
Very good thematic site – https://jukreative.com
latest news
market research
breaking news
business news
e-commerce
news source
food and health
strategies
Good luck!
retin a for sale uk
娛樂城
Портал о здоровье
https://www.rezus.ru и здоровом образе жизни, рекомендации врачей и полезные сервисы. Простые рекомендации для укрепления здоровья и повышения качества жизни.
Toni Kroos https://tonikroos.prostoprosport-ar.com is a German footballer who plays as a central midfielder for Real Madrid and the German national team. World champion 2014. The first German player in history to win the UEFA Champions League six times.
Всем привет! Подскажите, где найтиполезные блоги о недвижимости? Сейчас читаю https://417-017.ru
Robert Lewandowski https://robertlewandowski.prostoprosport-ar.com is a Polish footballer, forward for the Spanish club Barcelona and captain of the Polish national team. Considered one of the best strikers in the world. Knight of the Commander’s Cross of the Order of the Renaissance of Poland.
modafinil pills india
волчонок онлайн бесплатно в хорошем качестве https://volchonok-tv.ru
piracetam 800mg cost – praziquantel 600mg generic sinemet online buy
волчонок смотреть онлайн бесплатно на русском https://volchonok-tv.ru
buy nootropil 800mg pill – buy secnidazole 20mg generic buy sinemet pill
dexamethasone 4
Всем привет! Подскажите, где почитатьразные блоги о недвижимости? Сейчас читаю https://aquatopnn.ru
Хотите быть в курсе всех важных тем в мире недвижимости?
На нашем ресурсе вы найдете множество полезных статей о квартирах от застройщика, а также о анализе рынка недвижимости.
Узнайте все, что вам нужно для успешных сделок и принятия взвешенных решений в области недвижимости.
https://prestizh-stroi.ru
Good day!
Cocktail Crafting! Elevate your cocktail game with our creative drink recipes. From classic cocktails to innovative new creations, become your own mixologist.
Sustainable Eating! Learn to eat sustainably with our eco-friendly recipes and tips. Find out how to reduce food waste and make environmentally conscious food choices.
Look interesting site about this – https://visionarynexst.com
food industry
travel packages
food sustainability
financial news
competitiveness
food science
travel tips
business plan
Good luck!
Mohamed Salah https://mohamedsalah.prostoprosport-ar.com is an Egyptian footballer who plays as a forward for the English club Liverpool and the Egyptian national team. Considered one of the best football players in the world. Three-time winner of the English Premier League Golden Boot: in 2018 (alone), 2019 (along with Sadio Mane and Pierre-Emerick Aubameyang) and 2022 (along with Son Heung-min).
Pedro Gonzalez Lopez https://pedri.prostoprosport-ar.com better known as Pedri, is a Spanish footballer who plays as an attacking midfielder for Barcelona and the Spanish national team. Bronze medalist of the 2020 European Championship, as well as the best young player of this tournament. Silver medalist at the 2020 Olympic Games in Tokyo. At the age of 18, he was included in the list of 30 football players nominated for the 2021 Ballon d’Or.
buy tiktok followers cheap buy tiktok followers
buy cheap tiktok likes buy tiktok likes
Всем привет! Может кто знает, где найтиполезные блоги о недвижимости? Пока нашел https://artem-dvery.ru
라이즈 오브 올림푸스
Fang Jifan은 무엇을 말해야할지 모르고 중얼 거 렸습니다. “…”
buy cheap generic hydroxyurea – methocarbamol buy online methocarbamol brand
Lionel Andres Messi Cuccittini https://lionelmessi.prostoprosport-ar.com is an Argentine footballer, forward and captain of the MLS club Inter Miami, captain of the Argentina national team. World champion, South American champion, Finalissima winner, Olympic champion. Considered one of the best football players of all time.
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-ar.com is a Portuguese footballer, forward, captain of the Saudi Arabian club An-Nasr and the Portuguese national team. European Champion. Considered one of the best football players of all time. The best scorer in the history of football according to the IFFIS and fourth according to the RSSSF
Приветствую. Может кто знает, где найтиразные статьи о недвижимости? Сейчас читаю https://asiatreid.ru
Секреты успешного получения лицензии на недвижимость|Легко и быстро получите лицензию на недвижимость|Как начать карьеру в недвижимости с лицензией|Успешные стратегии получения лицензии на недвижимость|Эффективные способы получения лицензии на недвижимость|Полезные советы по получению лицензии на недвижимость|Простой путь к получению лицензии на недвижимость|Как стать агентом с лицензией на недвижимость|Как получить лицензию на недвижимость: советы экспертов|Инструкция по получению лицензии на недвижимость|Основные моменты получения лицензии на недвижимость|Секреты скорого получения лицензии на недвижимость|Получите лицензию на недвижимость и станьте профессионалом|Лицензия на недвижимость: ключ к успешной карьере|Профессиональные советы по получению лицензии на недвижимость|Эффективные стратегии для успешного получения лицензии на недвижимость|Шаги к успешной лицензии на недвижимость|Советы по успешному получению лицензии на недвижимость|Лицензия на недвижимость: ключ к успеху в индустрии недвижимости|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Получите лицензию на недвижимость и станьте профессиональным агентом|Основные шаги к профессиональной лицензии на недвижимость|Шаги к успешной лицензии на недвижимость|Секреты быстрого получения лицензии на недвижимость|Эффективные советы по успешному получению лицензии на недвижимость|Лицензия на недвижимость: важные аспекты для успешного получения
How to get my real estate license in North Carolina How to get my real estate license in North Carolina .
Секреты успешного получения лицензии на недвижимость|Легко и быстро получите лицензию на недвижимость|Подробное руководство по получению лицензии на недвижимость|Успешные стратегии получения лицензии на недвижимость|Инструкция по получению лицензии на недвижимость|Следуйте этим шагам для получения лицензии на недвижимость|Лицензия на недвижимость: важные аспекты|Шаг за шагом к лицензии на недвижимость|Как получить лицензию на недвижимость: советы экспертов|Лицензия на недвижимость для начинающих: советы и рекомендации|Основные моменты получения лицензии на недвижимость|Секреты скорого получения лицензии на недвижимость|Основные шаги к успешной лицензии на недвижимость|Лицензия на недвижимость: ключ к успешной карьере|Как получить лицензию на недвижимость легко и быстро|Как получить лицензию на недвижимость без стресса|Шаги к успешной лицензии на недвижимость|Советы по успешному получению лицензии на недвижимость|Ключевые моменты получения лицензии на недвижимость|Секреты успешного получения лицензии на недвижимость: что вам нужно знать|Как стать агентом по недвижимости с лицензией|Основные шаги к профессиональной лицензии на недвижимость|Получение лицензии на недвижимость для начинающих: советы от экспертов|Процесс получения лицензии на недвижимость: ключевые моменты|Эффективные советы по успешному получению лицензии на недвижимость|Сек
How do you get a real estate license in Tennessee How do you get a real estate license in Tennessee .
Всем привет! Может кто знает, где почитатьполезные блоги о недвижимости? Пока нашел https://dilerskiy-tsentr-baumit.ru
Anderson Sousa Conceicao better known as Talisca https://talisca.prostoprosport-ar.com is a Brazilian footballer who plays as a midfielder for the An-Nasr club. A graduate of the youth team from Bahia, where he arrived in 2009 ten years ago.
Yassine Bounou https://yassine-bounou.prostoprosport-ar.com also known as Bono, is a Moroccan footballer who plays as a goalkeeper for the Saudi Arabian club Al-Hilal and the Moroccan national team. On November 10, 2022, he was included in the official application of the Moroccan national team to participate in the matches of the 2022 World Cup in Qatar
Harry Edward Kane https://harry-kane.prostoprosport-ar.com is an English footballer, forward for the German club Bayern and captain of the England national team. Considered one of the best football players in the world. He is Tottenham Hotspur’s and England’s all-time leading goalscorer, as well as the second most goalscorer in the Premier League. Member of the Order of the British Empire.
Neymar da Silva Santos Junior https://neymar.prostoprosport-ar.com is a Brazilian footballer who plays as a striker, winger and attacking midfielder for the Saudi Arabian club Al-Hilal and the Brazilian national team. Considered one of the best players in the world. The best scorer in the history of the Brazilian national team.
Всем привет! Подскажите, где почитатьразные статьи о недвижимости? Пока нашел https://dompodkluch33.ru
Добро пожаловать на наш сайт, где вы найдете много полезных статей на тему приемки квартиры в новостройке или покупки квартиры без отделки. Узнайте, как обезопасить себя от ненадёжных застройщиков, какие проверки провести перед покупкой жилья, и о многом другом!
https://citadel-ca.ru
Erling Breut Haaland https://erling-haaland.prostoprosport-ar.com is a Norwegian footballer who plays as a forward for the English club Manchester City and the Norwegian national team. English Premier League record holder for goals per season.
Ali al-Buleahi https://ali-al-bulaihi.prostoprosport-ar.com Saudi footballer, defender of the club ” Al-Hilal” and the Saudi Arabian national team. On May 15, 2018, Ali al-Buleakhi made his debut for the Saudi Arabian national team in a friendly game against the Greek team, coming on as a substitute midway through the second half.
У нас вы найдете полезные статьи на тему недвижимости, например, покупка квартиры в новостройке, оценка недвижимости, юридическое сопровождение сделки.
Узнайте все нюансы, которые помогут вам принять верное решение и осуществить успешную сделку с недвижимостью. Наши статьи помогут вам быть в курсе последних новостей и законов жилищного рынка, а также избежать недоразумений.
http://domzenit.ru
Приветствую. Подскажите, где найтиполезные статьи о недвижимости? Сейчас читаю https://eniseyburvod.ru
Luka Modric https://lukamodric.prostoprosport-ar.com is a Croatian footballer, central midfielder and captain of the Spanish club Real Madrid, captain of the Croatian national team. Recognized as one of the best midfielders of our time. Knight of the Order of Prince Branimir. Record holder of the Croatian national team for the number of matches played.
buy instant tiktok followers buy tiktok followers tokmatic
Читайте интересные статьи на актуальные темы, связанные с продажей жилья, например квартира от застройщика или ликвидационная стоимость недвижимости.
Сайт: https://ooo-trotuar.ru
buy 100k tiktok followers https://www.templates.com/blog/how-to-get-more-followers-on-tiktok-expert-tips/
buy 5000 tiktok followers cheap buy 1000 tiktok followers cheap
buy tiktok followers cheap https://www.templates.com/blog/how-to-get-more-followers-on-tiktok-expert-tips/
Всем привет! Подскажите, где найтиполезные статьи о недвижимости? Сейчас читаю https://etalon-voda.ru
Good day!
Cocktail Crafting! Elevate your cocktail game with our creative drink recipes. From classic cocktails to innovative new creations, become your own mixologist.
Financial Tips for Success! Take control of your finances with our practical money management tips. From budgeting to investing, we help you make smart financial decisions.
Look interesting site about this – https://visionarynexst.com
culinary
travel photography tips
live news
business plan
writing tips
food safety
news aggregator
food photography
Goog luck!
Всем привет! Может кто знает, где почитатьразные блоги о недвижимости? Сейчас читаю https://floor-ashton.ru
프라 그마 틱 슬롯 사이트
Zeng Jie의 소동 이후 많은 사람들이 의미심장하게 두 사람의 뒷모습을 바라 보았습니다.
Доставка алкоголя в Екатеринбурге
https://vyzov-santehnika-na-dom.ru.
Всем привет! Подскажите, где почитатьполезные статьи о недвижимости? Сейчас читаю https://gismt72.ru
На нашем сайте вы сможете найти все необходимые сведения о недвижимости – от бронирования жилья в новостройке до покупки квартиры от застройщика.
Мы поможем вам выбрать лучшую квартиру в новостройке, расскажем, как не ошибиться при выборе жилья и подскажем, как сэкономить на покупке.
Заходите: https://quartz-rsk.ru
Взять займ или кредит
https://gazetadaily.ru/05/31/kak-poluchit-zajm-na-kartu-ili-bankovskij-schet/ под проценты, подав заявку на денежный микрозайм для физических лиц. Выбирайте среди 570 лучших предложений займа онлайн. Возьмите микрозайм онлайн или наличными в день обращения. Быстрый поиск и удобное сравнение условий по займам и микрокредитам в МФО.
NGolo Kante https://ngolokante.prostoprosport-ar.com is a French footballer who plays as a defensive midfielder for the Saudi Arabian club Al-Ittihad and the French national team. His debut for the first team took place on May 18, 2012 in a match against Monaco (1:2). In the 2012/13 season, Kante became the main player for Boulogne, which played in Ligue 3.
Взять займ или кредит
https://agmoda.ru/kak-uznat-yavlyaetsya-li-kredit-vygodnym-dlya-vas/ под проценты, подав заявку на денежный микрозайм для физических лиц. Выбирайте среди 570 лучших предложений займа онлайн. Возьмите микрозайм онлайн или наличными в день обращения. Быстрый поиск и удобное сравнение условий по займам и микрокредитам в МФО.
Приветствую. Может кто знает, где почитатьполезные блоги о недвижимости? Пока нашел https://kait-volga.ru
Интимные услуги в столице является проблемой как сложной и многогранной темой. Невзирая на это запрещена правилами, этот бизнес продолжает быть важным нелегальным сектором.
Исторические аспекты
В советского времени периоды интимные услуги была незаконно. С распадом СССР, в обстановке экономической нестабильной ситуации, секс-работа стала более заметной.
Нынешняя положение дел
В настоящее время интимные услуги в Москве принимает многообразие форм, включая высококлассных сопровождающих услуг до публичной секс-работы. Элитные предложения зачастую осуществляются через интернет, а публичная интимные услуги сконцентрирована в выделенных районах столицы.
Общественно-экономические аспекты
Многие женщин приходят в эту деятельность из-за экономических неурядиц. Секс-работа может оказаться интересной из-за шансом быстрого дохода, но это подразумевает угрозу здоровью и охраны здоровья.
Юридические аспекты
Коммерческий секс в России запрещена, и за её проведение предусмотрены жесткие наказания. Проституток зачастую привлекают к дисциплинарной ответственности.
Таким образом, не обращая внимания на запреты, секс-работа является элементом экономики в тени российской столицы с большими социальными и законодательными последствиями.
проститутки софьино
Hello!
Adventure Awaits! Ready for your next journey? Find inspiration and practical travel advice, whether seeking thrills or relaxation.
Family-Friendly Meals! Discover recipes that everyone in the family will enjoy. Our family-friendly meals are easy to prepare and sure to satisfy even the pickiest eaters.
Very good thematic site – https://jukreative.com
food and health
leadership
travel photography tips
money-saving tips
short-haul travel
entertainment news
sustainable development
environmental news
Good luck!
Ruben Diogo da Silva Neves https://ruben-neves.prostoprosport-ar.com is a Portuguese footballer who plays as a midfielder for the Saudi Arabian club Al-Hilal and the Portuguese national team. Currently, Ruben Neves plays for the Al-Hilal club wearing number 8. His contract with the Saudi club is valid until the end of June 2026.
gastehaus sorban immobilien montenegro
hotelverkauf
montenegro immobilien von privat kaufen
Hello there! can you buy cheap stromectol without rx great web site.
寶島娛樂城官網
Всем привет! Может кто знает, где найтиразные блоги о недвижимости? Пока нашел https://kaluga-elite.ru
Kobe Bean Bryant https://kobebryant.prostoprosport-ar.com is an American basketball player who played in the National Basketball Association for twenty seasons for one team, the Los Angeles Lakers. He played as an attacking defender. He was selected in the first round, 13th overall, by the Charlotte Hornets in the 1996 NBA Draft. He won Olympic gold twice as a member of the US national team.
Коммерческий секс в городе Москве представляет собой сложной и многогранной трудностью. Невзирая на этот бизнес запрещается юридически, этот бизнес является важным теневым сектором.
Прошлый
В советские годы коммерческий секс имела место подпольно. После Советской империи, в обстановке хозяйственной кризиса, эта деятельность оказалась более видимой.
Нынешняя обстановка
Сегодня интимные услуги в столице включает различные формы, начиная с элитных эскорт-сервисов до на улице проституции. Люксовые предложения обычно осуществляются через онлайн, а улицы проституция сосредоточена в специфических зонах города.
Социально-экономические аспекты
Большинство представительницы слабого пола занимаются в этот бизнес по причине материальных неурядиц. Секс-работа может являться привлекательным из-за возможности быстрого дохода, но она влечет за собой вред для здоровья и жизни.
Законодательные вопросы
Коммерческий секс в стране противозаконна, и за эту деятельность проведение состоят жесткие меры наказания. Проституток регулярно задерживают к дисциплинарной вине.
Поэтому, невзирая на запреты, секс-работа остаётся аспектом теневой экономики столицы с значительными социально-правовыми последствиями.
purchase hydrea – buy indinavir sale purchase methocarbamol for sale
Купити ліхтарики https://bailong-police.com.ua оптом та в роздріб, каталог та прайс-лист, характеристики, відгуки, акції та знижки. Купити ліхтарик онлайн з доставкою. Відмінний вибір ліхтарів: налобні, ручні, тактичні, ультрафіолетові, кемпінгові, карманні за вигідними цінами.
Продажа подземных канализационных ёмкостей https://neseptik.com по выгодным ценам. Ёмкости для канализации подземные объёмом до 200 м3. Металлические накопительные емкости для канализации заказать и купить в Екатеринбурге.
台灣線上娛樂城
台灣線上娛樂城是指通過互聯網提供賭博和娛樂服務的平台。這些平台主要針對台灣用戶,但實際上可能在境外運營。以下是一些關於台灣線上娛樂城的重要信息:
1. 服務內容:
– 線上賭場遊戲(如老虎機、撲克、輪盤等)
– 體育博彩
– 彩票遊戲
– 真人荷官遊戲
2. 特點:
– 全天候24小時提供服務
– 可通過電腦或移動設備訪問
– 常提供優惠活動和獎金來吸引玩家
3. 支付方式:
– 常見支付方式包括銀行轉賬、電子錢包等
– 部分平台可能接受加密貨幣
4. 法律狀況:
– 在台灣,線上賭博通常是非法的
– 許多線上娛樂城實際上是在國外註冊運營
5. 風險:
– 由於缺乏有效監管,玩家可能面臨財務風險
– 存在詐騙和不公平遊戲的可能性
– 可能導致賭博成癮問題
6. 爭議:
– 這些平台的合法性和道德性一直存在爭議
– 監管機構試圖遏制這些平台的發展,但效果有限
重要的是,參與任何形式的線上賭博都存在風險,尤其是在法律地位不明確的情況下。建議公眾謹慎對待,並了解相關法律和潛在風險。
如果您想了解更多具體方面,例如如何識別和避免相關風險,我可以提供更多信息。
Всем привет! Может кто знает, где найтиполезные блоги о недвижимости? Сейчас читаю https://kmzperm.ru
Lebron Ramone James https://lebronjames.prostoprosport-ar.com American basketball player who plays the positions of small and power forward. He plays for the NBA team Los Angeles Lakers. Experts recognize him as one of the best basketball players in history, and a number of experts put James in first place. One of the highest paid athletes in the world.
무료 슬롯 머신
아무리 들어도 Zhang Sheng과 Fang Jifan은 … 협력하는 것 같습니다.
https://win-line.net/ווינר-ליין-ווינר-אונליין/
לשלוח, תימוכין לדבריך.
ההתמודדות באינטרנט הפכה לענף נחשק מאוד בעשור האחרון, המציע מגוון רחב של אלטרנטיבות התמודדות, כמו הימורי ספורט.
בסיכום זה נבדוק את עולם הקזינו המקוון ונספק לכם נתונים חשובים שיעזור לכם להתמצא בתחום מרתק זה.
משחקי פוקר – הימורים באינטרנט
הימורי ספורט מציע אלטרנטיבות רבות של פעילויות קלאסיים כגון בלאק ג’ק. ההימורים באינטרנט מעניקים לשחקנים להתנסות מאווירת פעילות אותנטית בכל מקום ובשעה.
סוג המשחק תיאור קצר
מכונות מזל הימורי גלגל
משחק הרולטה הימור על תוצאות על גלגל מסתובב
משחק הקלפים בלאק ג’ק משחק קלפים בו המטרה היא להשיג 21
משחק קלפים פוקר משחק קלפים מבוסס אסטרטגיה
משחק הבאקרה משחק קלפים קל וזריז
הימורים על אירועי ספורט – הימורים באינטרנט
הימורים על אירועי ספורט מהווים חלק מ אחד האזורים המתרחבים ביותר בפעילות באינטרנט. משתתפים מורשים לסחור על תוצאים של אתגרי ספורט פופולריים כגון כדורסל.
התמודדויות אפשר לבצע על תוצאת התחרות, מספר השערים ועוד.
סוג הפעילות תיאור תחרויות ספורט מקובלות
ניחוש תוצאה ניחוש התוצאה הסופית של המשחק כדורגל, כדורסל, אמריקאי
הפרש ביצועים ניחוש הפרש הנקודות בין הקבוצות כדורגל, כדורסל, אמריקאי
מספר שערים/נקודות ניחוש כמה שערים או נקודות יהיו במשחק כל ענפי הספורט
הקבוצה המנצחת ניחוש מי יסיים ראשון (ללא קשר לניקוד) מרבית ענפי הספורט
התמרמרות בזמן אמת התמודדות במהלך התחרות בזמן אמת כדורגל, טניס, קריקט
הימורים משולבים שילוב של מספר הימורים שונים מרבית ענפי הספורט
משחקי קלפים אונליין – פעילות באינטרנט
התמודדות בפוקר מקוון מכיל אחד מסוגי התמודדות המובילים ביותר בתקופה הנוכחית. מתמודדים יכולים להתמודד עם מתמודדים אחרים מכמה הגלובוס במגוון
Luis Fernando Diaz Marulanda https://luis-diaz.prostoprosport-ar.com Colombian footballer, winger for Liverpool and the Colombian national team . Diaz is a graduate of the Barranquilla club. On April 26, 2016, in a match against Deportivo Pereira, he made his Primera B debut. On January 30, 2022, he signed a contract with the English Liverpool for five years, the transfer amount was 40 million euros.
Смелым игрокам посвящается!
Играю на 1win уже несколько месяцев и ни разу не пожалел. Регистрация простая, бонусы щедрые, вывод денег без задержек. Рабочее зеркало всегда доступно. Советую 1win всем любителям азартных игр! 1win зеркало вход
Скачал приложение 1win на Android и теперь играю в любое время. Бонусы радуют, вывод средств быстрый, рабочее зеркало всегда доступно. 1win – это мой выбор номер один для ставок и казино. Рекомендую!
Ловите сайт где все в лучшем виде! – http://1winapk.kz
бонус на спорт в 1win как использовать
1win бонусы спорт как использовать
ваучеры на 1win бесплатно
как на 1win ввести промокод
скачать и зарегистрироваться в 1win игровые автоматы
что за команда 1win
1win бонус казино как использовать
Удачи!
Maria Sharapova https://maria-sharapova.prostoprosport-ar.com Russian tennis player. The former first racket of the world, winner of five Grand Slam singles tournaments from 2004 to 2014, one of ten women in history who has the so-called “career slam”.
Приветствую. Подскажите, где найтиполезные блоги о недвижимости? Сейчас читаю https://kovry159.ru
Культура и музыка Кракена: как песни и
треки формируют имидж платформы
В последние годы площадка Кракена стала
одним из самых известных и популярных даркнет-маркетплейсов.
реклама даркнет кракен в москве Уникальный внешний вид и профессиональный
подход к делу привлекли на сайт множество
покупателей и продавцов. А неповторимая музыка, постоянно играющая на фоне,
задает тон и формирует имидж платформы.
Музыка Кракена — это микс из электронной музыки, хип-хопа и
рока. Она создает особую атмосферу, которая погружает пользователя в мир анонимности и свободы.
Трек за треком, песня за песней, платформа негласно транслирует свои ценности:
безопасность, конфиденциальность и надежность.
Так, главный лозунг сайта — «Твоя анонимность — наш приоритет» — находит
отражение в лирике треков.
А инструментальные композиции, звучащие в фоновом режиме, создают ощущение безопасности и комфорта.
Как и треки любого популярного бренда,
музыка Кракена стала неотъемлемой частью имиджа платформы, формируя восприятие пользователями и укрепляя лояльность к сайту.
Еще больше погрузиться в атмосферу Кракена и оценить звучание его треков
можно на странице реклама
даркнет кракен в москве.
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-ar.com Belgian footballer, midfielder of the Manchester club City” and the Belgian national team. A graduate of the football clubs “Ghent” and “Genk”. In 2008 he began his adult career, making his debut with Genk.
Mohammed Khalil Ibrahim Al-Owais https://mohammed-alowais.prostoprosport-ar.com is a Saudi professional footballer who plays as a goalkeeper for the national team Saudi Arabia and Al-Hilal. He is known for his quick reflexes and alertness at the gate.
Всем привет! Может кто знает, где почитатьполезные блоги о недвижимости? Пока нашел https://krepegmaster.ru
Quincy Anton Promes https://quincy-promes.prostoprosport-br.com Dutch footballer, attacking midfielder and forward for Spartak Moscow . He played for the Dutch national team. He won his first major award in 2017, when Spartak became the champion of Russia.
Экспертиза ремонта в квартире https://remnovostroi.ru проводится для оценки качества выполненных работ, соответствия требованиям безопасности и стандартам строительства. Специалисты проверяют используемые материалы, исполнение работ, конструктивные особенности, безопасность, внешний вид и эстетику ремонта. По результатам экспертизы составляется экспертное заключение с оценкой качества и рекомендациями по устранению недостатков.
Всем привет! Подскажите, где найтиразные блоги о недвижимости? Сейчас читаю https://kuler-tsentr.ru
Привет игроки!
1win – это место, где выигрывают. Ставлю на спорт и играю в казино уже несколько месяцев. Бонусы радуют, вывод денег быстрый и без задержек. Официальный сайт и рабочее зеркало всегда под рукой. Советую! 1win букмекерская контора зеркало 1win officials
Скачал приложение 1win на Android и теперь играю в любое время. Бонусы радуют, вывод средств быстрый, рабочее зеркало всегда доступно. 1win – это мой выбор номер один для ставок и казино. Рекомендую!
Ловите сайт где все в лучшем виде! – https://1winapk.kz
как поставить экспресс 1win
1win спорт
зеркало 1win россия онлайн
1win что за контора
1win официальный играть
1win официальная контора
1win uz skachat
Удачи!
Larry Joe Bird https://larry-bird.prostoprosport-br.com American basketball player who spent his entire professional career in the NBA ” Boston Celtics.” Olympic champion (1992), champion of the 1977 Universiade, 3-time NBA champion (1981, 1984, 1986), three times recognized as MVP of the season in the NBA (1984, 1985, 1986), 10 times included in the symbolic teams of the season (1980-88 – first team, 1990 – second team).
Roberto Firmino Barbosa de Oliveira https://roberto-firmino.prostoprosport-br.com Brazilian footballer, attacking midfielder, forward for the Saudi club “Al-Ahli”. Firmino is a graduate of the Brazilian club KRB, from where he moved to Figueirense in 2007. In June 2015 he moved to Liverpool for 41 million euros.
Всем привет! Может кто знает, где найтиполезные блоги о недвижимости? Сейчас читаю https://oscltd.ru
Khvicha Kvaratskhelia https://khvicha-kvaratskhelia.prostoprosport-br.com Georgian footballer, winger for Napoli and captain of the Georgian national team. A graduate of Dynamo Tbilisi. He made his debut for the adult team on September 29, 2017 in the Georgian championship match against Kolkheti-1913. In total, in the 2017 season he played 4 matches and scored 1 goal in the championship.
Damian Emiliano Martinez https://emiliano-martinez.prostoprosport-br.com Argentine footballer, goalkeeper of the Aston Villa club and national team Argentina. Champion and best goalkeeper of the 2022 World Cup.
order depakote 500mg – buy cordarone online cheap buy topamax 200mg pill
Секс-работа в городе Москве является проблемой как сложной и разнообразной темой. Невзирая на это запрещается законом, эта деятельность является крупным теневым сектором.
Прошлый
В Советского Союза времена интимные услуги существовала нелегально. После распада СССР, в ситуации рыночной неопределенности, она стала очевидной.
Текущая Ситуация
В настоящее время секс-работа в Москве включает многообразие форм, от высококлассных эскорт-услуг до самой на улице коммерческого секса. Престижные услуги часто организуются через онлайн, а публичная секс-работа располагается в выделенных зонах столицы.
Социальные и экономические факторы
Множество женщины занимаются в этот бизнес по причине материальных трудностей. Коммерческий секс может являться интересной из-за шанса мгновенного заработка, но это подразумевает рисками для здоровья и безопасности.
Правовые аспекты
Коммерческий секс в России запрещена, и за эту деятельность занятие состоят жесткие меры наказания. Секс-работниц регулярно привлекают к к административной и правовой вине.
Таким способом, несмотря на запреты, проституция продолжает быть сегментом незаконной экономики города с существенными социальными и законодательными последствиями.
order generic divalproex – amiodarone uk topamax 200mg cost
Jack Peter Grealish https://jackgrealish.prostoprosport-br.com English footballer, midfielder of the Manchester City club and the England national team. A graduate of the English club Aston Villa from Birmingham. In the 2012/13 season he won the NextGen Series international tournament, playing for the Aston Villa under-19 team
Всем привет! Может кто знает, где найтиразные блоги о недвижимости? Сейчас читаю https://ppu-odk.ru
Kyle Andrew Walker https://kylewalker.prostoprosport-br.com English footballer, captain of the Manchester City club and the England national team. In the 2013/14 season, he was on loan at the Notts County club, playing in League One (3rd division of England). Played 37 games and scored 5 goals in the championship.
Son Heung Min https://sonheung-min.prostoprosport-br.com South Korean footballer, striker and captain of the English Premier League club Tottenham Hotspur and the Republic of Korea national team. In 2022 he won the Premier League Golden Boot. Became the first Asian footballer in history to score 100 goals in the Premier League
Laure Boulleau https://laure-boulleau.prostoprosport-fr.com French football player, defender. She started playing football in the Riom team, in 2000 she moved to Isere, and in 2002 to Issigneux. All these teams represented the Auvergne region. In 2003, Bullo joined the Clairefontaine academy and played for the academy team for the first time.
Проституция в Москве существует как многосложной и сложноустроенной трудностью. Несмотря на то, что этот бизнес нелегальна правилами, эта деятельность является значительным нелегальным сектором.
Контекст в прошлом
В советские годы секс-работа существовала в тени. По окончании Союза, в обстановке рыночной нестабильности, секс-работа оказалась явной.
Сегодняшняя Ситуация
В настоящее время интимные услуги в Москве представляет собой различные формы, начиная с элитных эскорт-услуг и заканчивая уличной секс-работы. Люксовые обслуживание часто предоставляются через в сети, а уличная коммерческий секс сконцентрирована в определённых районах столицы.
Общественно-экономические аспекты
Многие девушки вступают в эту деятельность из-за экономических трудностей. Коммерческий секс может являться заманчивой из-за возможности немедленного дохода, но это связана с риски для здоровья и охраны здоровья.
Правовые Вопросы
Проституция в России противозаконна, и за её проведение существуют строгие наказания. Работников интимной сферы регулярно привлекают к административной ответственности.
Таким способом, игнорируя запреты, интимные услуги является аспектом теневой экономики Москвы с значительными социальными и законодательными последствиями.
purchase norpace pill – brand epivir 100mg thorazine pills
ciprofloxacin 500mg online
In recent times, Africa has appeared as a radiant hub for tunes and celebrity lifestyle, gaining international identification and influencing international trends. African songs, using its rich tapestry of genres many of these as Afrobeats, Amapiano, and highlife, offers captivated audiences throughout the world. Major artists just like Burna Boy, Wizkid, and Tiwa Savage have not simply dominated the charts in Africa but they have also made significant inroads into typically the global music landscape. Their collaborations using international stars in addition to performances at key music festivals have highlighted the continent’s musical prowess. The particular rise of electronic platforms and cultural media has further amplified the reach of African audio, allowing artists to connect with supporters across the planet and share their particular sounds and testimonies – https://histoires-africaines.africa/tiakola-quitte-wati-b-et-rejoint-warner-music/.
In addition to be able to its musical talent, Africa’s celebrity culture is flourishing, using entertainers, influencers, in addition to public figures commanding large followings. Celebrities such as Lupita Nyong’o, Trevor Noah, and Charlize Theron, who have beginnings in Africa, are usually making waves internationally in film, television, and fashion. These figures not merely take attention to their work but in addition reveal important cultural issues and ethnical heritage. Their good results stories inspire some sort of new generation of Africans to go after careers in the entertainment industry, fostering a sense of pride in addition to ambition across the particular continent.
Moreover, Black celebrities are significantly using their programs to advocate regarding change and offer back in their residential areas. From Burna Son’s activism around cultural justice issues to Tiwa Savage’s work in promoting education for girls, these general public figures are utilizing their influence intended for positive impact. They are involved in numerous philanthropic activities, promoting causes such since healthcare, education, and environmental sustainability. This particular trend highlights typically the evolving role involving celebrities in Photography equipment, who are not just entertainers but in addition key players inside driving social transformation and development.
General, the landscape involving music and celebrity culture in The african continent is dynamic in addition to ever-evolving. The continent’s rich cultural variety and creative expertise carry on and garner worldwide acclaim, positioning Photography equipment as being a major force inside the global leisure industry. As Black artists and celebs always break boundaries and achieve innovative heights, they front the way for some sort of more inclusive plus diverse representation within global media. Regarding those interested throughout staying updated on the latest trends and news in this vibrant scene, numerous platforms in addition to publications offer exhaustive coverage of Africa’s music and movie star happenings, celebrating the particular continent’s ongoing efforts to the globe stage.
In January 2010, Harry Kane https://harry-kane.prostoprosport-fr.com received an invitation to the England U-team for the first time 17 for the youth tournament in Portugal. At the same time, the striker, due to severe illness, did not go to the triumphant 2010 European Championship for boys under 17 for the British.
Antoine Griezmann https://antoine-griezmann.prostoprosport-fr.com French footballer, striker and midfielder for Atletico Madrid. Player and vice-captain of the French national team, as part of the national team – world champion 2018. Silver medalist at the 2016 European Championship and 2022 World Championship.
Karim Mostafa Benzema https://karim-benzema.prostoprosport-fr.com French footballer, striker for the Saudi club Al-Ittihad . He played for the French national team, for which he played 97 matches and scored 37 goals.
Achraf Hakimi Mou https://achraf-hakimi.prostoprosport-fr.com Moroccan footballer, defender of the French club Paris Saint-Germain “and the Moroccan national team. He played for Real Madrid, Borussia Dortmund and Inter Milan.
Приветствую. Может кто знает, где почитатьразные блоги о недвижимости? Сейчас читаю https://sibarit54.ru
Всем привет! Подскажите, где почитатьразные статьи о недвижимости? Сейчас читаю https://stroyproektm.ru
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-fr.com Footballeur francais, attaquant du Paris Saint-Germain et capitaine de l’equipe de France. Le 1er juillet 2024, il deviendra joueur du club espagnol du Real Madrid.
Hi there! levitra online pharmacy very good internet site.
Jogo do Tigre https://jogo-do-tigre.prostoprosport-br.com is a simple and fun game that tests your reflexes and coordination. In this game you need to put your finger on the screen, pull out the stick and go through each peg. However, you must ensure that the stick is the right length, neither too long nor too short.
Mohamed Salah Hamed Mehrez Ghali https://mohamed-salah.prostoprosport-fr.com Footballeur egyptien, attaquant du club anglais de Liverpool et l’equipe nationale egyptienne. Considere comme l’un des meilleurs footballeurs du monde
Приветствую. Подскажите, где найтиразные статьи о недвижимости? Пока нашел https://tent44.ru
Shedding Pounds with Protein: Guide to Using Protein Powders for Weight Loss
modafinil 200 mg tablet price in india
Global Careers
Declan Rice https://declan-rice.prostoprosport-fr.com Footballeur anglais, milieu defensif du club d’Arsenal et de l’equipe nationale equipe d’Angleterre. Originaire de Kingston upon Thames, Declan Rice s’est entraine a l’academie de football de Chelsea des l’age de sept ans. En 2014, il devient joueur de l’academie de football de West Ham United.
Olivier Jonathan Giroud https://olivier-giroud.prostoprosport-fr.com French footballer, striker for Milan and the French national team. Knight of the Legion of Honor. Participant in four European Championships (2012, 2016, 2020 and 2024) and three World Championships (2014, 2018 and 2022).
Приветствую. Подскажите, где почитатьразные статьи о недвижимости? Сейчас читаю https://universal37.ru
https://win-line.net/אתרי-הימורים-אמינים/
להעביר, נתונים לדבריך.
ההמרה באינטרנט הפכה לנישה פופולרי מאוד בשנים האחרונות, המספק מבחר רחב של חלופות התמודדות, כגון הימורי ספורט.
בסקירה זה נסקור את תחום ההתמודדות המקוונת ונעניק לכם פרטים חשובים שיעזור לכם להבין בתחום מעניין זה.
קזינו אונליין – הימורים באינטרנט
קזינו אונליין מאפשר מבחר מגוון של משחקים ידועים כגון פוקר. ההימורים באינטרנט מאפשרים למבקרים להשתתף מחוויית התמודדות אותנטית בכל עת ומקום.
המשחקים תיאור מקוצר
מכונות מזל הימורי גלגל
גלגל הרולטה הימור על תוצאות על גלגל הרולטה
בלאק ג’ק משחק קלפים בו המטרה להגיע לסכום של 21
התמודדות בפוקר משחק קלפים אסטרטגי
משחק קלפים באקרה משחק קלפים מהיר וקצר
הימורי ספורט – התמודדות באינטרנט
הימורי ספורט מייצגים אחד האזורים המשגשגים המרכזיים ביותר בקזינו באינטרנט. משתתפים רשאים לסחור על ביצועים של אתגרי ספורט מושכים כגון כדורסל.
התמודדויות ניתן לתמוך על תוצאת האירוע, מספר השערים ועוד.
אופן ההתמודדות הסבר משחקי ספורט מרכזיים
ניחוש התפוקה ניחוש התוצאה הסופית של האירוע כדורגל, כדורסל, הוקי
הפרש ביצועים ניחוש הפרש הנקודות בין הקבוצות כדורגל, כדורסל, אמריקאי
מספר שערים/נקודות ניחוש כמות הסקורים בתחרות כדורגל, כדורסל, הוקי קרח
המנצח בתחרות ניחוש איזו קבוצה תנצח (ללא קשר לתוצאה) מספר ענפי ספורט
התמרמרות בזמן אמת התמודדות במהלך האירוע בזמן אמת כדורגל, טניס, קריקט
הימורים משולבים שילוב של מספר פעילויות מספר ענפי ספורט
פוקר אונליין – התמודדות באינטרנט
פוקר אונליין מייצג אחד מסוגי ההימורים המשגשגים הגדולים ביותר בשנים האחרונות. מבקרים רשאים להשתלב בפני שחקנים אחרים מאזורי הגלובליזציה במגוון
Xavi or Xavi Quentin Sy Simons https://xavi-simons.prostoprosport-fr.com Dutch footballer, midfielder of the Paris Saint-Germain club -Germain” and the Dutch national team, playing on loan for the German club RB Leipzig.
Ronaldo de Asis Moreira https://ronaldinhogaucho.prostoprosport-br.com Brazilian footballer, played as an attacking midfielder and striker. World Champion (2002). Winner of the Golden Ball (2005). The best football player in the world according to FIFA in 2004 and 2005.
Carlos Henrique Casimiro https://carloscasemiro.prostoprosport-br.com Futebolista brasileiro, volante do clube ingles Manchester United e capitao do Selecao Brasileira. Pentacampeao da Liga dos Campeoes da UEFA, campeao mundial e sul-americano pela selecao juvenil brasileira.
Kylian Mbappe Lotten https://kylianmbappe.prostoprosport-br.com Futebolista frances, atacante do Paris Saint-Germain e capitao da selecao francesa equipe . Em 1? de julho de 2024, ele se tornara jogador do clube espanhol Real Madrid.
https://win-line.net/בלאק-גק-black-jack/
לשלוח, נתונים לדבריך.
ההמרה באינטרנט הפכה לנישה מבוקש מאוד בעשור האחרון, המספק מגוון רחב של אופציות הימורים, כמו משחקי פוקר.
בסקירה זה נפרט את עולם ההתמודדות המקוונת ונעניק לכם נתונים חשובים שיעזור לכם להתמצא בנושא מעניין זה.
הימורי ספורט – הימורים באינטרנט
הימורי ספורט מכיל אופציות שונות של פעילויות מסורתיים כגון בלאק ג’ק. ההתמודדות באינטרנט מעניקים למשתתפים להשתתף מאווירת התמודדות אותנטית מכל מקום.
הפעילות פירוט קצר
מכונות מזל משחקי מזל עם גלגלים
הימורי רולטה הימור על פרמטרים על גלגל מסתובב בצורה עגולה
משחק קלפים 21 משחק קלפים בו המטרה היא 21 נקודות
משחק הפוקר משחק קלפים מבוסס אסטרטגיה
משחק קלפים באקרה משחק קלפים פשוט וזריז
הימורים בתחום הספורט – קזינו באינטרנט
התמרמרות ספורטיבית מהווים אחד התחומים המתרחבים ביותר בהתמודדות באינטרנט. שחקנים יכולים להתמודד על תוצאות של אתגרי ספורט פופולריים כגון כדורגל.
ההימורים אפשר לבצע על תוצאת האירוע, מספר העופרות ועוד.
אופן ההתמודדות פירוט תחומי ספורט מובילים
ניחוש הביצועים ניחוש התוצאה הסופית של המשחק כדורגל, כדורסל, הוקי
הפרש תוצאות ניחוש ההפרש בסקורים בין הקבוצות כל ענפי הספורט
מספר שערים/נקודות ניחוש כמות הביצועים בתחרות כל ענפי הספורט
המנצח בתחרות ניחוש איזו קבוצה תנצח (ללא קשר לתוצאה) מגוון ענפי ספורט
התמרמרות בזמן אמת התמודדות במהלך התחרות בזמן אמת כדורגל, טניס, קריקט
הימורים משולבים שילוב של מספר סוגי התמרמרות מספר ענפי ספורט
פוקר אונליין – קזינו באינטרנט
פעילות פוקר מקוונת מהווה אחד מתחומי הקזינו המשגשגים ביותר כיום. מתמודדים מורשים להתמודד מול יריבים מרחבי הגלובוס בסוגים ש
Lionel Messi https://lionelmessi.prostoprosport-br.com e um jogador de futebol argentino, atacante e capitao do clube da MLS Inter Miami. , capitao da selecao argentina. Campeao mundial, campeao sul-americano, vencedor da Finalissima, campeao olimpico. Considerado um dos melhores jogadores de futebol de todos os tempos.
Mohamed Salah https://mohamedsalah.prostoprosport-br.com e um futebolista egipcio que joga como atacante do clube ingles Liverpool e do Selecao egipcia. Considerado um dos melhores jogadores de futebol do mundo. Tricampeao da Chuteira de Ouro da Premier League inglesa: em 2018 (sozinho), 2019 (junto com Sadio Mane e Pierre-Emerick Aubameyang) e 2022 (junto com Son Heung-min).
Harry Kane https://harry-kane.prostoprosport-br.com recebeu um convite para a selecao sub-alterna da Inglaterra pela primeira vez tempo 17 para o torneio juvenil em Portugal. Ao mesmo tempo, o atacante, devido a doenca grave, nao compareceu ao triunfante Campeonato Europeu Sub-17 masculino de 2010 pelos britanicos.
Zlatan Ibrahimovic https://zlatan-ibrahimovic.prostoprosport-br.com Bosnian pronunciation: ibraxi?mo?it?]; genus. 3 October 1981, Malmo, Sweden) is a Swedish footballer who played as a striker. Former captain of the Swedish national team.
Luis Alberto Suarez Diaz https://luis-suarez.prostoprosport-br.com Uruguayan footballer, striker for Inter Miami and Uruguay national team. The best scorer in the history of the Uruguay national team. Considered one of the world’s top strikers of the 2010s
Всем привет! Может кто знает, где найти разные статьи о недвижимости? Сейчас читаю https://1eve1.ru
order norpace generic – how to get chlorpromazine without a prescription buy chlorpromazine for sale
Gareth Frank Bale https://garethbale.prostoprosport-br.com Jogador de futebol gales que atuou como ala. Ele jogou na selecao galesa. Ele se destacou pela alta velocidade e um golpe bem colocado. Artilheiro (41 gols) e recordista de partidas disputadas (111) na historia da selecao.
Доброго!
В мире стремительных изменений и суеты каждый из нас мечтает о моментах истинного уюта и релаксации. И что может быть лучше, чем уютный вечер у камина? Магазин электрокаминов Grand-Kamin – идеальное место, где вы можете найти свой идеальный камин для создания совершенного вечера.
В нашем магазине вы обнаружите разнообразие электрокаминов различных стилей, от классических до современных, чтобы найти именно тот, который подчеркнет ваш вкус и стиль интерьера. Наши продукты сочетают в себе качество, функциональность и эстетику, чтобы каждый момент у камина стал идеальным.
Grand-Kamin- это не просто магазин, это место, где вы можете найти не просто камин, а создать уголок уюта и тепла, где каждый вечер станет особенным. Погрузитесь в мир комфорта и релаксации с нашими электрокаминами и создайте атмосферу идеального вечера прямо у себя дома.
Лучший сайт про электрические камины – http://www.grand-kamin.ru/
встроенные электрокамины купить
электрокамин цена в москве недорого
электрокамины недорого
электрокамны москва дешево
встраиваемый электрокамин
Удачи!
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-br.com Futebolista belga, meio-campista do Manchester club City” e a selecao belga. Formado pelos clubes de futebol “Ghent” e “Genk”. Em 2008 iniciou sua carreira adulta, fazendo sua estreia no Genk.
Antoine Griezmann https://antoine-griezmann.prostoprosport-br.com Futebolista frances, atacante e meio-campista do Atletico de Madrid. Jogador e vice-capitao da selecao francesa, integrante da selecao – campea mundial 2018. Medalhista de prata no Europeu de 2016 e no Mundial de 2022.
Профессиональные seo https://seo-optimizaciya-kazan.ru услуги для максимизации онлайн-видимости вашего бизнеса. Наши эксперты проведут глубокий анализ сайта, оптимизируют контент и структуру, улучшат технические аспекты и разработают индивидуальные стратегии продвижения.
order cyclophosphamide online – meclizine 25mg tablet cheap vastarel tablets
프라그마틱 무료
Liu Jian은 평범한 장관이 아니며 법원에서 그의 지위는 매우 중요하다고 할 수 있습니다.
Выберите стильные тактичные штаны для повседневной носки, для идеального комфорта и функциональности.
Тактичные штаны: модные тренды этого сезона, которые подчеркнут вашу уверенность и стиль.
Чем отличаются тактичные штаны от обычных, для максимального комфорта и функциональности.
Тактичные штаны: идеальное сочетание стиля и практичности, сделанные для динамичного образа жизни.
Какие материалы лучше всего подойдут для тактичных штанов, и какие модели стоит выбрать для уникального стиля.
штани зимові тактичні штани зимові тактичні .
Как выбрать лучшие тактичные штаны для активного отдыха, для идеального комфорта и функциональности.
Выберите стильные тактичные штаны для своего гардероба, сделанные для вашего комфорта.
Как правильно выбрать тактичные штаны, и какие модели стоит обратить внимание.
Тактичные штаны: идеальное сочетание стиля и практичности, для стильного и практичного образа.
Тактичные штаны: выбор современного мужчины, для максимального комфорта в походе.
купить штани тактичні купить штани тактичні .
Идеальные тактичные штаны для любого случая, для идеального комфорта и функциональности.
Новинки в мире тактичной одежды: лучшие штаны, которые подчеркнут вашу уверенность и стиль.
Чем отличаются тактичные штаны от обычных, чтобы выглядеть стильно в любой ситуации.
Выберите удобные тактичные штаны для своего гардероба, и какие модели актуальны в этом сезоне.
Тактичные штаны: выбор современного мужчины, и какие модели стоит выбрать для уникального стиля.
куплю тактичні штани https://vijskovitaktichnishtanu.kiev.ua/ .
Romelu Menama Lukaku Bolingoli https://romelulukaku.prostoprosport-br.com Futebolista belga, atacante do clube ingles Chelsea e da selecao belga . Por emprestimo, ele joga pelo clube italiano Roma.
dexona 4mg tablet
Приветствую. Может кто знает, где почитать полезные статьи о недвижимости? Пока нашел https://an72.ru
Neymar da Silva Santos Junior https://neymar.prostoprosport-br.com e um futebolista brasileiro que atua como atacante, ponta e atacante. meio-campista do clube saudita Al-Hilal e da selecao brasileira. Considerado um dos melhores jogadores do mundo. O maior artilheiro da historia da Selecao Brasileira.
Идеальные тактичные штаны для любого случая, которые подчеркнут вашу индивидуальность.
Новинки в мире тактичной одежды: лучшие штаны, которые подчеркнут вашу уверенность и стиль.
Чем отличаются тактичные штаны от обычных, чтобы выглядеть стильно в любой ситуации.
Какие тактичные штаны подойдут именно вам, для стильного и практичного образа.
Тактичные штаны: выбор современного мужчины, и какие модели стоит выбрать для уникального стиля.
тактичні штани жіночі https://vijskovitaktichnishtanu.kiev.ua/ .
Jude Victor William Bellingham https://jude-bellingham.prostoprosport-cz.org anglicky fotbalista, zaloznik spanelskeho klubu Real Madrid a anglicky narodni tym. V dubnu 2024 ziskal cenu za prulom roku z Laureus World Sports Awards. Stal se prvnim fotbalistou, ktery ji obdrzel.
Всем привет! Может кто знает, где найти полезные статьи о недвижимости? Пока нашел https://armid44.ru
Kylian Mbappe Lotten https://kylian-mbappe.prostoprosport-cz.org Francouzsky fotbalista, utocnik Paris Saint-Germain a kapitan tymu francouzskeho tymu. 1. cervence 2024 se stane hracem spanelskeho klubu Real Madrid.
Mohamed Salah https://mohamed-salah.prostoprosport-cz.org je egyptsky fotbalista, ktery hraje jako utocnik za anglictinu. klub Liverpool a egyptsky narodni tym. Povazovan za jednoho z nejlepsich fotbalistu na svete.
Приветствую. Может кто знает, где почитать полезные блоги о недвижимости? Сейчас читаю https://azimut-irkutsk.ru
spironolactone 100mg for sale – epitol pills naltrexone 50 mg us
Kevin De Bruyne https://kevin-de-bruyne.prostoprosport-cz.org Belgicky fotbalista, zaloznik Manchesteru klub City” a belgicky narodni tym. Absolvent fotbalovych klubu „Ghent” a „Genk”. V roce 2008 zahajil svou karieru dospelych, debutoval v Genku.
spironolactone 25mg usa – buy generic phenytoin 100 mg naltrexone 50 mg uk
Bernardo Silva https://bernardo-silva.prostoprosport-cz.org Portugalsky fotbalista, zaloznik. Narozen 10. srpna 1994 v Lisabonu. Silva je povazovan za jednoho z nejlepsich utocnych zalozniku na svete. Fotbalista je povestny svou vytrvalosti a vykonem.
Lionel Messi https://lionel-messi.prostoprosport-cz.org je argentinsky fotbalista, utocnik a kapitan klubu MLS Inter Miami. , kapitan argentinske reprezentace. Mistr sveta, vitez Jizni Ameriky, vitez finale, olympijsky vitez. Povazovan za jednoho z nejlepsich fotbalistu vsech dob.
Antoine Griezmann https://antoine-griezmann.prostoprosport-cz.org Francouzsky fotbalista, utocnik a zaloznik za Atletico de Madrid. Hrac a vicekapitan francouzskeho narodniho tymu, clen tymu – mistr sveta 2018 Stribrny medailista z mistrovstvi Evropy 2016 a mistrovstvi sveta 2022.
Robert Lewandowski https://robert-lewandowski.prostoprosport-cz.org je polsky fotbalista, utocnik spanelskeho klubu Barcelona a kapitan polskeho narodniho tymu. Povazovan za jednoho z nejlepsich utocniku na svete. Rytir krize velitele polskeho renesancniho radu.
Приветствую. Подскажите, где почитать полезные блоги о недвижимости? Пока нашел https://ecn-novodom.ru
}
cipro 800mg
Приветствую. Может кто знает, где найти разные блоги о недвижимости? Пока нашел https://germes-alania.ru
cab 토토
평생 명확한 이름을 가지고 있는데 어떻게 Fang Jifan과 어울릴 수 있습니까?당연히 Fang Jifan의 외침은 소란에 묻힌 지 오래되었습니다.
Son Heung Min https://son-heung-min.prostoprosport-cz.org Jihokorejsky fotbalista, utocnik a kapitan anglickeho klubu Premier League Tottenham Hotspur a narodniho tymu Korejske republiky. V roce 2022 vyhral Zlatou kopacku Premier League.
Luka Modric https://luka-modric.prostoprosport-cz.org je chorvatsky fotbalista, stredni zaloznik a kapitan spanelskeho tymu. klub Real Madrid, kapitan chorvatskeho narodniho tymu. Uznavan jako jeden z nejlepsich zalozniku nasi doby. Rytir Radu prince Branimira. Rekordman chorvatske reprezentace v poctu odehranych zapasu.
Pablo Martin Paez Gavira https://gavi.prostoprosport-cz.org Spanelsky fotbalista, zaloznik barcelonskeho klubu a spanelske reprezentace. Povazovan za jednoho z nejtalentovanejsich hracu sve generace. Ucastnik mistrovstvi sveta 2022. Vitez Ligy narodu UEFA 2022/23
Cristiano Ronaldo https://cristiano-ronaldo.prostoprosport-cz.org je portugalsky fotbalista, utocnik, kapitan Saudske Arabie klubu An-Nasr a portugalskeho narodniho tymu. Mistr Evropy. Povazovan za jednoho z nejlepsich fotbalistu vsech dob. Nejlepsi strelec v historii fotbalu podle IFFIS a ctvrty podle RSSSF
Всем привет! Может кто знает, где найти полезные блоги о недвижимости? Пока нашел https://ilinka2.ru
купить поролон для матраса
Pedro Gonzalez Lopez https://pedri.prostoprosport-cz.org lepe znamy jako Pedri, je spanelsky fotbalista, ktery hraje jako utocny zaloznik. za Barcelonu a spanelskou reprezentaci. Bronzovy medailista z mistrovstvi Evropy 2020 a zaroven nejlepsi mlady hrac tohoto turnaje.
Rodrigo Silva de Goiz https://rodrygo.prostoprosport-cz.org Brazilsky fotbalista, utocnik Realu Madrid a brazilskeho narodniho tymu. V breznu 2017 byl Rodrigo povolan do narodniho tymu Brazilie U17 na zapasy Montague Tournament.
Alison Ramses Becker https://alisson-becker.prostoprosport-cz.org Brazilsky fotbalista nemeckeho puvodu, brankar klubu Liverpool a brazilsky narodni tym. Je povazovan za jednoho z nejlepsich brankaru sve generace a je znamy svymi vynikajicimi zakroky, presnosti prihravek a schopnosti jeden na jednoho.
Karim Benzema https://karim-benzema.prostoprosport-cz.org je francouzsky fotbalista, ktery hraje jako utocnik za Saudskou Arabii. Arabsky klub Al-Ittihad. Hral za francouzsky narodni tym, za ktery odehral 97 zapasu a vstrelil 37 branek. V 17 letech se stal jednim z nejlepsich hracu rezervy, nastrilel tri desitky golu za sezonu.
Thibaut Nicolas Marc Courtois https://thibaut-courtois.prostoprosport-cz.org Belgicky fotbalista, brankar spanelskeho klubu Real Madrid . V sezone 2010/11 byl uznan jako nejlepsi brankar v belgicke Pro League a take hrac roku pro Genk. Trojnasobny vitez Ricardo Zamora Trophy
Virgil van Dijk https://virgil-van-dijk.prostoprosport-cz.org Nizozemsky fotbalista, stredni obrance, kapitan anglickeho klubu Liverpool a kapitan nizozemskeho narodniho tymu.
Bruno Guimaraes Rodriguez Moura https://bruno-guimaraes.prostoprosport-cz.org Brazilsky fotbalista, defenzivni zaloznik Newcastlu United a Brazilsky narodni tym. Vitez olympijskych her 2020 v Tokiu.
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
cytoxan sale – cytoxan ca cheap generic vastarel
Toni Kroos https://toni-kroos.prostoprosport-cz.org je nemecky fotbalista, ktery hraje jako stredni zaloznik za Real Madrid a nemecky narodni tym. Mistr sveta 2014. Prvni nemecky hrac v historii, ktery sestkrat vyhral Ligu mistru UEFA.
Darwin Gabriel Nunez Ribeiro https://darwin-nunez.prostoprosport-cz.org Uruguaysky fotbalista, utocnik anglickeho klubu Liverpool a Uruguaysky narodni tym. Bronzovy medailista mistrovstvi Jizni Ameriky mezi mladeznickymi tymy.
Romelu Menama Lukaku Bolingoli https://romelu-lukaku.prostoprosport-cz.org Belgicky fotbalista, utocnik anglickeho klubu Chelsea a Belgican vyber. Na hostovani hraje za italsky klub Roma.
Dedicated to the brave players!!
Glory Casino is my number one choice for betting and casino. The bonuses are nice, withdrawals are fast, and the Android app is convenient. The working mirror is always available. I play with pleasure and recommend everyone to try it!
I downloaded Glory Casino on Android and now I can play anytime. The bonuses and promotions are a pleasant surprise. The working mirror is always available, and withdrawals are fast. Glory Casino is the best choice for betting and casino. I recommend trying it!
Glory Casino
Glory Casino official download
Glory Casino login
Glory Casino login online
Glory Casino mirror now
Glory Casino working mirror download
Good profits!
проститутки москвы дешевые проститутки москвы
how to buy 1000 followers on tiktok buy tiktok followers free
buy tiktok followers paypal https://buy-tiktok-followers.com
смотреть отчаянные домохозяйки в хорошем качестве https://domohozyayki-serial.ru
заказать проститутку молодые проститутки
can you buy followers on tiktok to go live https://tiktok-followers-buy.com
buy 100 tiktok followers best site to buy tiktok followers
отчаянные домохозяйки смотреть онлайн бесплатно качестве отчаянные домохозяйки 1 сезон 1 серия
официальный сайт риобет казино регистрация рио бет казино
онлайн казино Dragon Money trucktir.ru
Большой выбор игровых автоматов, рабочее зеркало сайта https://fartunaplay.ru играть на реальные деньги онлайн
Rio Bet Casino Rio Bet
Dragon Money Casino https://trucktir.ru
Качественная и недорогая мебель новгород лучшие цены, доставка и сборка.
Качественная и недорогая хорошая мягкая мебель лучшие цены, доставка и сборка.
100 doxycycline
Pin Up casino https://pin-up.salexy.kz official website, Pin Up slot machines play for money online, Pin Up mirror working for today.
Slot machines on the official website and mirrors of the Pin Up online casino https://pin-up.tr-kazakhstan.kz are available for free mode, and after registering at Pin Up Casino Ru you can play for money.
Pin up entry to the official website. Play online casino Pin Up https://pin-up.prostoprosport.ru for real money. Register on the Pin Up Casino website and claim bonuses!
Sports in Azerbaijan https://idman-xeberleri.com.az development and popular sports Azerbaijan is a country with rich sports traditions and outstanding achievements on the international stage.
best pharmacy prices for propecia
World of Games https://onlayn-oyunlar.com.az provides the latest news about online games, game reviews, gameplay and ideas, game tactics and tips. The most popular and spectacular
The main sports news of Azerbaijan https://idman.com.az. Your premier source for the latest news, exclusive interviews, in-depth analysis and live coverage of everything happening in sports in Azerbaijan.
UFC in Azerbaijan https://ufc.com.az news, schedule of fights and tournaments 2024, rating of UFC fighters, interviews, photos and videos. Live broadcasts and broadcasts of tournaments, statistics.
NHL (National Hockey League) News https://nhl.com.az the latest and greatest NHL news for today. Sports news – latest NHL news, standings, match results, online broadcasts.
Top sports news https://idman-azerbaycan.com.az photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading championships.
마종 웨이즈 2
대명궁이 세워졌을 때보다 더 강력하지 않습니까?
Latest news and details about the NBA in Azerbaijan https://nba.com.az. Hot events, player transfers and the most interesting events. Explore the world of the NBA with us.
Discover the fascinating world of online games with GameHub Azerbaijan https://online-game.com.az. Get the latest news, reviews and tips for your favorite games. Join our gaming community today!
The latest top football news https://futbol.com.az today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
Каталог рейтингов хостингов https://pro-hosting.tech на любой вкус и под любые, даже самые сложные, задачи.
https://santekhnik-moskva.blogspot.com — вызов сантехника на дом в Москве и Московской области в удобное для вас время.
Play PUBG Mobile https://pubg-mobile.com.az an exciting world of high-quality mobile battle royale. Unique maps, strategies and intense combat await you in this exciting mobile version of the popular game.
The Dota 2 website https://dota2.com.az Azerbaijan provides the most detailed information about the latest game updates, tournaments and upcoming events. We have all the winning tactics, secrets and important guides.
Latest news about games for Android https://android-games.com.az, reviews and daily updates. Read now and get the latest information on the most exciting games
Хотите сделать в квартире ремонт? Тогда советуем вам посетить сайт https://stroyka-gid.ru, где вы найдете всю необходимую информацию по строительству и ремонту.
Check out the latest news, guides and in-depth reviews of the available options for playing Minecraft Az https://minecraft.com.az. Find the latest information about Minecraft Download, Pocket Edition and Bedrock Edition.
The most popular sports site https://sports.com.az of Azerbaijan, where the latest sports news, forecasts and analysis are collected.
Latest news and analytics of the Premier League https://premier-league.com.az. Detailed descriptions of matches, team statistics and the most interesting football events. EPL Azerbaijan is the best place for football fans.
rgbet
https://LoveFlover.ru — сайт посвященный комнатным растениям. Предлагает подробные статьи о выборе, выращивании и уходе за различными видами комнатных растений. Здесь можно найти полезные советы по созданию зелёного уголка в доме, руководства по декору и решению распространённых проблем, а также информацию о подходящих горшках и удобрениях. Платформа помогает создавать уютную атмосферу и гармонию в интерьере с помощью растений.
1xbet https://1xbet.best-casino-ar.com with withdrawal without commission. Register online in a few clicks. A large selection of slot machines in mobile applications and convenient transfers in just a few minutes.
Pin Up official https://pin-up.adb-auto.ru website. Login to your personal account and register through the Pin Up mirror. Slot machines for real money at Pinup online casino.
Pin-up Casino https://pin-up.admsov.ru/ is an online casino licensed and regulated by the government of Curacao . Founded in 2016, it is home to some of the industry’s leading providers, including NetEnt, Microgaming, Play’n GO and others. This means that you will be spoiled for choice when it comes to choosing a game.
Pin Up online casino https://pin-up.webrabota77.ru/ is the official website of a popular gambling establishment for players from the CIS countries. The site features thousands of slot machines, online tables and other branded entertainment from Pin Up casino.
Pin Up Casino https://pin-up.noko39.ru Registration and Login to the Official Pin Up Website. thousands of slot machines, online tables and other branded entertainment from Pin Up casino. Come play and get big bonuses from the Pinup brand today
Реальные анкеты проституток https://prostitutki-213.ru Москвы с проверенными фото – от элитных путан до дешевых шлюх. Каталог всех индивидуалок на каждой станции метро с реальными фотографиями без ретуши и с отзывами реальных клиентов.
Смотрите онлайн сериал Отчаянные домохозяйки https://domohozyayki-serial.ru в хорошем качестве HD 720 бесплатно, рейтинг сериала: 8.058, режиссер сериала: Дэвид Гроссман, Ларри Шоу, Дэвид Уоррен.
Buy TikTok followers https://tiktok-followers-buy.com to get popular and viral with your content. All packages are real and cheap — instant delivery within minutes. HQ followers for your TikTok. 100% real users. The lowest price for TikTok followers on the market
Pin Up Casino https://pin-up.sibelshield.ru official online casino website for players from the CIS countries. Login and registration to the Pin Up casino website is open to new users with bonuses and promotional free spins.
Pin Up https://pin-up.fotoevolution.ru казино, которое радует гемблеров в России на протяжении нескольких лет. Узнайте, что оно подготовило посетителям. Описание, бонусы, отзывы о легендарном проекте. Регистрация и вход.
Изготовление памятников и надгробий https://uralmegalit.ru по низким ценам. Собственное производство. Высокое качество, широкий ассортимент, скидки, установка.
Pin Up Casino https://pin-up.ergojournal.ru приглашает игроков зарегистрироваться на официальном сайте и начать играть на деньги в лучшие игровые автоматы, а на зеркалах онлайн казино Пин Ап можно найти аналогичную витрину слотов
Pin-up casino https://pin-up.jes-design.ru популярное онлайн-казино и ставки на спорт. Официальный сайт казино для доступа к играм и другим функциям казино для игры на деньги.
Открой мир карточных игр в Pin-Up https://pin-up.porsamedlab.ru казино Блэкджек, Баккара, Хило и другие карточные развлечения. Регистрируйтесь и играйте онлайн!
Официальный сайт Pin Up казино https://pin-up.nasledie-smolensk.ru предлагает широкий выбор игр и щедрые бонусы для игроков. Уникальные бонусные предложения, онлайн регистрация.
Pinup казино https://pin-up.vcabinet.kz это не просто сайт, а целый мир азартных развлечений, где каждый может найти что-то свое. От традиционных игровых автоматов до прогнозов на самые популярные спортивные события.
Latest Diablo news https://diablo.com.az game descriptions and guides. Diablo.az is the largest Diablo portal in the Azerbaijani language.
Latest World of Warcraft (WOW) tournament news https://wow.com.az, strategies and game analysis. The most detailed gaming portal in Azerbaijani language
Откройте тайны берців зсу, Чем примечательны берці зсу?, освойте, погрузитесь в, Берці зсу: связь с предками, Берці зсу: символ силы, сущность, Берці зсу: от древности до современности, освойте, в душу, З чого починаються берці зсу, таємниці
нові берці зсу 2021 https://bercitaktichnizsu.vn.ua/ .
Azerbaijan NFL https://nfl.com.az News, analysis and topics about the latest experience, victories and records. A portal where the most beautiful NFL games in the world are generally studied.
Discover exciting virtual football in Fortnite https://fortnite.com.az. Your central hub for the latest news, expert strategies and interesting e-sports reports. Collecting points with us!
The latest analysis, tournament reviews and the most interesting features of the Spider-Man game https://spider-man.com.az series in Azerbaijani.
Read the latest Counter-Strike 2 news https://counter-strike.net.az, watch the most successful tournaments and become the best in the world of the game on the CS2 Azerbaijan website.
отремонтировать стиральную машину в москве отремонтировать стиральную машину в москве .
Latest boxing news https://boks.com.az, Resul Abbasov’s achievements, Tyson Fury’s fights and much more. All in Ambassador Boxing.
Explore the extraordinary journey of Kilian Mbappe https://kilian-mbappe.com.az, from his humble beginnings to global stardom. Delve into his early years, meteoric rise through the ranks, and impact on and off the football field.
Mesut Ozil https://mesut-ozil.com.az latest news, statistics, photos and much more. Get the latest news and information about one of the best football players Mesut Ozil.
Latest news, statistics, photos and much more about Pele https://pele.com.az. Get the latest news and information about football legend Pele.
Sergio Ramos Garcia https://sergio-ramos.com.az Spanish footballer, defender. Former Spanish national team player. He played for 16 seasons as a central defender for Real Madrid, where he captained for six seasons.
1000 mg modafinil
Gianluigi Buffon https://buffon.com.az Italian football player, goalkeeper. Considered one of the best goalkeepers of all time. He holds the record for the number of games in the Italian Championship, as well as the number of minutes in this tournament without conceding a goal.
Paulo Bruno Ezequiel Dybala https://dybala.com.az Argentine footballer, striker for the Italian club Roma and the Argentina national team. World champion 2022.
Paul Labille Pogba https://pogba.com.az French footballer, central midfielder of the Italian club Juventus. Currently suspended for doping and unable to play. World champion 2018.
Канал для того, чтобы знания и опыт, могли помочь любому человеку сделать ремонт https://tvin270584.livejournal.com в своем жилище, любой сложности!
Kevin De Bruyne https://kevin-de-bruyne.liverpool-fr.com Belgian footballer, born 28 June 1991 years in Ghent. He has had a brilliant club career and also plays for the Belgium national team. De Bruyne is known for his spectacular goals and brilliant assists.
79 슬롯
아버지로서 어떻게 아들이 잘되기를 바라지 않을 수 있겠습니까?
Paul Labille Pogba https://paul-pogba.psg-fr.com Footballeur francais, milieu de terrain central du club italien de la Juventus. Champion du monde 2018. Actuellement suspendu pour dopage et incapable de jouer.
Mohamed Salah Hamed Mehrez Ghali https://mohamed-salah.liverpool-fr.com Footballeur egyptien, attaquant du club anglais de Liverpool et l’equipe nationale egyptienne. Considere comme l’un des meilleurs joueurs du monde.
The young talent who conquered Paris Saint-Germain: how Xavi Simons became https://xavi-simons.psg-fr.com leader of a superclub in record time.
lioresal cost
Kylian Mbappe https://kylian-mbappe.psg-fr.com Footballeur, attaquant francais. Il joue pour le PSG et l’equipe de France. Ne le 20 decembre 1998 a Paris. Mbappe est francais de nationalite. La taille de l’athlete est de 178 cm.
Изготовление, сборка и ремонт мебели https://shkafy-na-zakaz.blogspot.com для Вас, от эконом до премиум класса.
Kevin De Bruyne https://liverpool.kevin-de-bruyne-fr.com Belgian footballer, born 28 June 1991 years in Ghent. He has had a brilliant club career and also plays for the Belgium national team. De Bruyne is known for his spectacular goals and brilliant assists.
Paul Pogba https://psg.paul-pogba-fr.com is a world-famous football player who plays as a central midfielder. The player’s career had its share of ups and downs, but he was always distinguished by his perseverance and desire to win.
flexeril over the counter – buy vasotec 10mg for sale buy enalapril without a prescription
Kylian Mbappe https://psg.kylian-mbappe-fr.com Footballeur, attaquant francais. L’attaquant de l’equipe de France Kylian Mbappe a longtemps refuse de signer un nouveau contrat avec le PSG, l’accord etant en vigueur jusqu’a l’ete 2022.
brand flexeril 15mg – flexeril 15mg price enalapril 10mg pills
Thibaut Nicolas Marc Courtois https://thibaut-courtois.real-madrid-ar.com Footballeur belge, gardien de but du Club espagnol “Real Madrid”. Lors de la saison 2010/11, il a ete reconnu comme le meilleur gardien de la Pro League belge, ainsi que comme joueur de l’annee pour Genk. Trois fois vainqueur du Trophee Ricardo Zamora, decerne chaque annee au meilleur gardien espagnol
Forward Rodrigo https://rodrygo.real-madrid-ar.com is now rightfully considered a rising star of Real Madrid. The talented Santos graduate is compared to Neymar and Cristiano Ronaldo, but the young talent does not consider himself a star.
Jude Victor William Bellingham https://jude-bellingham.real-madrid-ar.com English footballer, midfielder of the Spanish club Real Madrid and the England national team. In April 2024, he won the Breakthrough of the Year award from the Laureus World Sports Awards.
Saud Abdullah Abdulhamid https://saud-abdulhamid.real-madrid-ar.com Saudi footballer, defender of the Al -Hilal” and the Saudi Arabian national team. Asian champion in the age category up to 19 years. Abdulhamid is a graduate of the Al-Ittihad club. On December 14, 2018, he made his debut in the Saudi Pro League in a match against Al Bateen
Khvicha Kvaratskhelia https://khvicha-kvaratskhelia.real-madrid-ar.com midfielder of the Georgian national football team and the Italian club “Napoli”. Became champion of Italy and best player in Serie A in the 2022/23 season. Kvaratskhelia is a graduate of Dynamo Tbilisi and played for the Rustavi team.
에그벳슬롯
그가 화살을 쏘았을 때 그것은 점점 더 정확해졌고 그는 새로운 이해를 갖기 시작했습니다.
Vinicius Junior https://vinisius-junior.com.az player news, fresh current and latest events for today about the player of the 2024 season
Latest news and information about Marcelo https://marcelo.com.az on this site! Find Marcelo’s biography, career, playing stats and more. Find out the latest information about football master Marcelo with us!
Khabib Abdulmanapovich Nurmagomedov https://khabib-nurmagomedov.com.az Russian mixed martial arts fighter who performed under the auspices of the UFC. Former UFC lightweight champion.
Welcome to our official site! Get to know the history, players and latest news of Inter Miami Football Club https://inter-miami.com.az. Discover with us the successes and great performances of America’s newest and most exciting soccer club.
Conor Anthony McGregor https://conor-mcgregor.com.az Irish mixed martial arts fighter who also performed in professional boxing. He performs under the auspices of the UFC in the lightweight weight category. Former UFC lightweight and featherweight champion.
Оперативный вывод из запоя https://www.liveinternet.ru/users/laralim/post505923855/ на дому. Срочный выезд частного опытного нарколога круглосуточно. При необходимости больного госпитализируют в стационар.
Видеопродакшн студия https://humanvideo.ru полного цикла. Современное оборудование продакшн-компании позволяет снимать видеоролики, фильмы и клипы высокого качества. Создание эффективных видеороликов для рекламы, мероприятий, видеоролики для бизнеса.
Совсем недавно открылся новый интернет портал BlackSprut (Блекспрут) https://bs2cite.cc в даркнете, который предлагает купить нелегальные товары и заказать запрещенные услуги. Самая крупнейшая площадка СНГ. Любимые шопы и отзывчивая поддержка.
Заказать вывоз мусора заказать вывоз мусора в Москве и Московской области, недорого и в любое время суток в мешках или контейнерами 8 м?, 20 м?, 27 м?, 38 м?, собственный автопарк. Заключаем договора на вывоз мусора.
Реальные анкеты проститутки Москвы с проверенными фото – от элитных путан до дешевых шлюх. Каталог всех индивидуалок на каждой станции метро с реальными фотографиями без ретуши и с отзывами реальных клиентов.
Welcome to the site dedicated to Michael Jordan https://michael-jordan.com.az, a basketball legend and symbol of world sports culture. Here you will find highlights, career, family and news about one of the greatest athletes of all time.
Diego Armando Maradona https://diego-maradona.com.az Argentine footballer who played as an attacking midfielder and striker. He played for the clubs Argentinos Juniors, Boca Juniors, Barcelona, ??Napoli, and Sevilla.
Gucci купить http://thebestluxurystores.ru по низкой цене в интернет-магазине брендовой одежды. Одежда и обувь бренда Gucci c доставкой.
Muhammad Ali https://muhammad-ali.com.az American professional boxer who competed in the heavy weight category; one of the most famous boxers in the history of world boxing.
Монтаж систем отопления https://fectum.pro, водоснабжения, вентиляции, канализации, очистки воды, пылеудаления, снеготаяния, гелиосистем в Краснодаре под ключ.
buy generic zofran over the counter – generic tolterodine 1mg requip medication
하바네로 슬롯
왕자는 항상 말도 안되는 말에 익숙했습니다.
Lev Ivanovich Yashin https://lev-yashin.com.az Soviet football player, goalkeeper. Olympic champion in 1956 and European champion in 1960, five-time champion of the USSR, three-time winner of the USSR Cup.
Usain St. Leo Bolt https://usain-bolt.com.az Jamaican track and field athlete, specialized in short-distance running, eight-time Olympic champion and 11-time world champion (a record in the history of this competition among men).
Al-Nasr https://al-nasr.com.az your source of news and information about Al-Nasr Football Club . Find out the latest results, transfer news, player and manager interviews, fixtures and much more.
You have a source of the latest and most interesting sports news from Kazakhstan: “Kazakhstan sports news https://sports-kazahstan.kz: Games and records” ! Follow us to receive updates and interesting news every minute!
Game World https://kz-games.kz offers the latest online gaming news, game reviews, gameplay and ideas, gaming tactics and tips . Start playing our most popular and amazing games and get ready to become the leader in the online gaming world!
Latest news and information about the NBA https://basketball-kz.kz in Kazakhstan. Hot stories, player transfers and highlights. Watch the NBA world with us.
Top sports news https://sport-kz-news.kz, photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading championships.
The latest top football news https://football-kz.kz today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
furosemide 100 mg
Latest news about games for Android https://android-games.kz, reviews and daily updates. Read now and get the latest information about the most exciting games
Check out Minecraft kz https://minecraft-kz.kz for the latest news, guides, and in-depth reviews of the game options available. Find the latest information on Minecraft Download, Pocket Edition and Bedrock Edition.
Latest news from World of Warcraft https://wow-kz.kz (WOW) tournaments, strategy and game analysis. The most detailed gaming portal in the language.
Latest news and analysis of the Premier League https://premier-league.kz. Full descriptions of matches, team statistics and the most interesting football events. Premier Kazakhstan is the best place for football fans.
Доставка груза и грузоперевозки https://tamozhennyy-deklarant.blogspot.com по России через транспортную компанию автотранспортом доступна и для частных лиц. Перевозчик отправит или доставит ваш груз: выгодные тарифы индивидуальный подход из рук в руки 1 машиной.
Зеркала интерьерные https://zerkala-mag.ru в интернет-магазине «Зеркала с подсветкой» Самые низкие цены на зеркала!
Предлагаем купить гаражное оборудование https://profcomplex.pro, автохимию, технику и уборочный инвентарь для клининговых компаний. Доставка по Москве и другим городам России.
Купить зеркала https://zerkala-m.ru по низким ценам. Более 1980 моделей, купить недорого в интернет-магазине в Москве с доставкой по России. Удобный каталог, низкие цены, качественные фото.
dexamethasone 3 mg
Spider-Man https://spiderman.kz the latest news, articles, reviews, dates, spoilers and other latest information. All materials on the topic “Spider-Man”
Latest Counter-Strike 2 news https://counter-strike-kz.kz, watch the most successful tournaments and be the best in the gaming world.
The latest top football news https://football.sport-news-eg.com today. Interviews with football players, online broadcasts and match results, analytics and football forecasts, photos and videos.
Discover the dynamic world of Arab sports https://sports-ar.com through the lens of Arab sports news. Your premier source for breaking news, exclusive interviews, in-depth analysis and live coverage of everything happening in sports.
generic propecia 2019
Интернет магазин электроники https://techno-line.store и цифровой техники по доступным ценам. Доставка мобильной электроники по Москве и Московской области.
UFC news https://ufc-ar.com, schedule of fights and tournaments 2024, ratings of UFC fighters, interviews, photos and videos. Live broadcasts and broadcasts of tournaments, statistics, forums and fan blogs.
NHL news https://nhl-ar.com (National Hockey League) – the latest and most up-to-date NHL news for today.
The most important sports news https://bein-sport-egypt.com, photos and blogs from experts and famous athletes, as well as statistics and information about matches of leading leagues.
News and events of the American Basketball League https://basketball-eg.com in Egypt. Hot events, player transfers and the most interesting events. Explore the world of the NBA with us.
슬롯 보증 사이트
걸어서 두 잔의 차를 마시고 싶은데 정신이 없습니까? 그런 좋은 일이 있습니까?
Discover the wonderful world of online games https://game-news-ar.com. Get the latest news, reviews and tips for your favorite games.
News, tournaments, guides and strategies about the latest GTA games https://gta-ar.com. Stay tuned for the best GTA gaming experience
Minecraft news https://minecraft-ar.com, guides and in-depth reviews of the gaming features available in Minecraft Ar. Get the latest information on downloading Minecraft, Pocket Edition and Bedrock Edition.
Latest news https://android-games-ar.com about Android games, reviews and daily updates. The latest information about the most exciting games.
Хотите быть в курсе всех важных тем в мире недвижимости?
На нашем сайте вы сможете найти множество полезных статей о квартирах от застройщика, налогах на недвижимость, а также о ипотечном кредитовании.
http://zoltor24sochi.ru
5 래빗스 메가웨이즈
내시는 진돈을 두 사람에게 데려왔고 문양생과 제경통은 자리에 앉았다.
Всем привет! Подскажите, где почитать разные блоги о недвижимости? Сейчас читаю https://kran-rdk.ru
The site is dedicated to football https://fooball-egypt.com, football history and news. Latest news and fresh reviews of the world of football
Открытие для себя Ерлинг Хааланда https://manchestercity.erling-haaland-cz.com, a talented player of «Manchester City». Learn more about his skills, achievements and career growth.
The path of 21-year-old Jude Bellingham https://realmadrid.jude-bellingham-cz.com from young talent to one of the most promising players in the world, reaching new heights with Dortmund and England.
French prodigy Kylian Mbappe https://realmadrid.kylian-mbappe-cz.com is taking football by storm, joining his main target, ” Real.” New titles and records are expected.
Harry Kane’s journey https://bavaria.harry-kane-cz.com from Tottenham’s leading striker to Bayern’s leader and Champions League champion – this is the story of a triumphant ascent to the football Olympus.
Всем привет! Может кто знает, где найти полезные блоги о недвижимости? Сейчас читаю https://mart-posters.ru
order zofran 4mg online cheap – detrol 1mg usa requip 2mg pill
order ascorbic acid 500 mg generic – buy compro pills buy prochlorperazine pill
ascorbic acid 500mg without prescription – buy cheap generic isosorbide dinitrate oral compro
Изготовим для Вас изделия из металла https://smith-moskva.blogspot.com, по вашим чертежам или по нашим эскизам.
Промышленные насосы https://1nsk.ru/news/articles/nasosy-spetsialnogo-naznacheniya.html Wilo предлагают широкий ассортимент решений для различных отраслей промышленности, включая водоснабжение, отопление, вентиляцию, кондиционирование и многие другие. Благодаря своей высокой производительности и эффективности, насосы Wilo помогают снизить расходы на энергию и обслуживание, что делает их идеальным выбором для вашего бизнеса.
https://rolaks.com отделочные материалы для фасада – интернет-магазин
The fascinating story of the rise of Brazilian prodigy Vinicius Junior https://realmadrid.vinicius-junior-cz.com to the heights of glory as part of the legendary Madrid “Real”
Mohamed Salah https://liverpool.mohamed-salah-cz.com, who grew up in a small town in Egypt, conquered Europe and became Liverpool star and one of the best players in the world.
Приветствую. Подскажите, где почитать полезные блоги о недвижимости? Сейчас читаю https://metrazhi-omsk.ru
Полезные советы и пошаговые инструкции по строительству https://syndyk.by, ремонту и дизайну домов и квартир, выбору материалов, монтажу и установке своими руками.
The inspiring story of how talented Kevin De Bruyne https://manchestercity.kevin-de-bruyne-cz.com became the best player of Manchester City and the Belgium national team. From humble origins to the leader of a top club.
Lionel Messi https://intermiami.lionel-messi-cz.com, one of the best football players of all time, moves to Inter Miami” and changes the face of North American football.
Bernardo Mota Veiga de Carvalho e Silva https://manchestercity.bernardo-silva-cz.com Portuguese footballer, club midfielder Manchester City and the Portuguese national team.
Antoine Griezmann https://atlticomadrid-dhb.antoine-griezmann-cz.com Atletico Madrid star whose talent and decisive goals helped the club reach the top of La Liga and the UEFA Champions League.
Контроль по борьбе с отмыванием денег: Посредством чего минимизировать приостановление фондов на платформах обмена криптовалют
С какой целью необходима антиотмывочные меры?
Проверка по борьбе с отмыванием денег (Противодействие легализации доходов) – представляет собой комплекс действий, нацеленных для борьбы отбеливания средств. Эта проверка позволяет сохранять виртуальные ресурсы владельцев избегая использование систем криминальных транзакций. Антиотмывочные меры обязательна в целях обеспечения безопасности личных активов наряду с соблюдением законодательных норм.
Ключевые методы оценки
Участники криптосферы а также другие денежные сервисы задействуют несколько важнейших инструментов в рамках проверки пользователей:
KYC: Такая процедура предусматривает основные действия с целью идентификации данных владельца, например анализ подтверждающих данных регистрации. KYC дает возможность подтвердить, в надежности владельца выступает в качестве законным.
Борьба с финансированием терроризма: Сфокусирована на предотвращение поддержки экстремистских групп. Система отслеживает подозрительные операции в случае необходимости ограничивает профили для проведения внутриорганизационной расследования.
Выгоды проверки по борьбе с отмыванием денег
AML-проверка обеспечивает участникам криптосферы:
Следовать международные вместе с национальными правовые нормы.
Защищать участников недобросовестных действий.
Укреплять степень доверия у пользователей надзорных органов.
Каким способом минимизировать риски свои активы при операциях в цифровой валютной среде
Для того чтобы ограничить угрозы приостановления средств, придерживайтесь этим указаниям:
Взаимодействуйте с безопасные биржи: Обращайтесь единственно к сервисам высокой востребованностью а также высоким показателем контроля.
Анализируйте получателей: Применяйте услуги по противодействию отмыванию посредством проверки цифровых кошельков участников предварительно перед проведением сделок.
Постоянно модифицируйте виртуальные счета: Указанная процедура поможет предотвратить вероятных опасений, в случае если Ваши партнеры будут внесены под подозрение.
Сберегайте подтверждения транзакций: В случае необходимости вы сможете обосновать чистоту полученных фондов.
Заключение
Процедура противодействия отмыванию денег – это важный способ с целью обеспечения защищенности активностей на криптовалютном рынке. Такой подход оказывает содействие избежать отмывание ресурсов, обеспечение терроризма а также иные противоправные действия. Следуя советам в интересах безопасности в совокупности с выбором заслуживающие доверие платформы, будете в состоянии минимизировать угрозы ограничения фондов и наслаждаться защищенной работой на криптовалютных рынках.
Приветствую. Подскажите, где найти полезные блоги о недвижимости? Сейчас читаю https://mik-dom.ru
The story of Robert Lewandowski https://barcelona.robert-lewandowski-cz.com, his impressive journey from Poland to Barcelona, ??where he became not only a leader on the field, but also a source of inspiration for young players.
Son Heung-min’s https://tottenhamhotspur.son-heung-min-cz.com success story at Tottenham Hotspur and his influence on the South Korean football, youth inspiration and changing the perception of Asian players.
We explore the path of Luka Modric https://realmadrid.luka-modric-cz.com to Real Madrid, from a difficult adaptation to legendary Champions League triumphs and personal awards.
The impact of the arrival of Cristiano Ronaldo https://annasr.cristiano-ronaldo-cz.com at Al-Nasr. From sporting triumphs to cultural changes in Saudi football.
Приветствую. Может кто знает, где почитать разные статьи о недвижимости? Пока нашел https://miro-teh-ural.ru
{
амл проверка
Антиотмывочная проверка: Посредством чего избежать ограничение фондов на криптобиржах
По какой причине нужна процедура противодействия отмыванию денег?
Процедура противодействия отмыванию денег (Противодействие легализации доходов) – представляет собой совокупность инструментов, нацеленных на борьбу легализации ресурсов. Данная процедура позволяет оберегать цифровые средства клиентов а также предотвращать использование сервисов противоправных транзакций. Проверка по борьбе с отмыванием денег обязательна для обеспечения неприкосновенности ваших фондов а также соблюдения юридических требований.
Базовые инструменты оценки
Участники криптосферы а также другие платежные предложения внедряют множество основных способов для проверки владельцев:
Верификация личности: Такая процедура включает ключевые процедуры в целях идентификации удостоверения владельца, в том числе проверка подтверждающих данных местонахождения. Верификация личности дает возможность быть уверенным, что участник выступает в качестве легитимным.
Борьба с финансированием терроризма: Сосредоточена для предотвращения обеспечения экстремистских групп. Процедура мониторит подозрительные переводы и при необходимости ограничивает учетные записи посредством проведения внутреннего экспертизы.
Положительные аспекты AML-проверки
Проверка по борьбе с отмыванием денег обеспечивает участникам криптосферы:
Следовать международные наряду с региональными юридические нормы.
Оберегать пользователей недобросовестных действий.
Наращивать показатель репутации со стороны пользователей госорганов.
Каким образом минимизировать риски свои ресурсы во время операций в цифровой валютной среде
Чтобы ограничить опасности блокировки ресурсов, выполняйте данным подсказкам:
Взаимодействуйте с проверенные биржи: Обращайтесь только к сервисам с хорошей оценкой и высоким уровнем защищенности.
Проверяйте получателей: Используйте AML-сервисы в интересах проверки криптовалютных реквизитов контрагентов предварительно перед выполнением сделок.
Постоянно трансформируйте виртуальные счета: Это поможет снизить вероятных опасений, если ваши контрагенты окажутся под ограничения.
Храните доказывающие материалы переводов: Если наступит требовании будете в состоянии доказать законность получаемых ресурсов.
Подытоживая
Антиотмывочные меры – это существенный способ в интересах обеспечения сохранности операций
с криптовалютой. Эта практика оказывает содействие минимизировать легализацию ресурсов, финансирование террористической деятельности помимо прочих нелегальные мероприятия. Выполняя требованиям в интересах безопасности в совокупности с выбором надежные обменники, получите возможность снизить риски замораживания средств работать надежной функционированием на криптовалютных рынках.
Find out how Pedri https://barcelona.pedri-cz.com becomes a key figure for Barcelona – his development, influence and ambitions determine the club’s future success in world football.
A study of the influence of Rodrigo https://realmadrid.rodrygo-cz.com on the success and marketing strategy of Real Madrid: analysis of technical skills, popularity in Media and commercial success.
Find out how Pedro Gavi https://barcelona.gavi-cz.com helped Barcelona achieve success thanks to his unique qualities, technique and leadership, becoming a key player in the team.
Find out about Alisson https://liverpool.alisson-becker-cz.com‘s influence on Liverpool’s success, from his defense to personal achievements that made him one of the best goalkeepers in the world.
How Karim Benzema https://alIttihad.karim-benzema-cz.com changed the game of Al-Ittihad and Saudi football: new tactics, championship success, increased viewership and commercial success.
Приветствую. Может кто знает, где почитать разные статьи о недвижимости? Пока нашел https://mzhk-stroy.ru
Всем привет! Подскажите, где почитать разные блоги о недвижимости? Пока нашел https://nagaevodom.ru
r7 casino официальный сайт https://mabiclub.ru
buy instagram followers cheap buy instagram followers
Thibaut Courtois https://realmadrid.thibaut-courtois-cz.com the indispensable goalkeeper of “Real”, whose reliability, leadership and outstanding The game made him a key figure in the club.
Find out how Virgil van Dijk https://liverpool.virgil-van-dijk-cz.com became an integral part of style игры «Liverpool», ensuring the stability and success of the team.
Find out how Bruno Guimaraes https://newcastleunited.bruno-guimaraes-cz.com became a catalyst for the success of Newcastle United thanks to his technical abilities and leadership on the field and beyond.
Приветствую. Может кто знает, где почитать разные статьи о недвижимости? Пока нашел https://potolkinomer1.ru
슬롯 용가리
그런 다음 Zhu Houzhao가 “Old Fang, Lao Fang …”이라고 외치는 것을 들었습니다.
Study of the playing style of Toni Kroos https://real-madrid.toni-kroos-cz.com at Real Madrid: his accurate passing, tactical flexibility and influence on the team’s success.
The young Uruguayan Darwin Nunez https://liverpool.darwin-nunez-cz.com broke into the elite of world football, and he became a key Liverpool player.
Romelu Lukaku https://chelsea.romelu-lukaku-cz.com, one of the best strikers in Europe, returns to Chelsea to continue climbing to the top of the football Olympus.
Star Brazilian striker Gabriel Jesus https://arsenal.gabriel-jesus-cz.com put in a superb performance to lead Arsenal to new heights after moving from Manchester City.
A fascinating story about how David Alaba https://realmadrid.david-alaba-cz.com after starting his career at the Austrian academy Vienna became a key player and leader of the legendary Real Madrid.
Приветствую. Может кто знает, где найти разные блоги о недвижимости? Пока нашел https://promresmag.ru
purchase cheap durex gel – buy cheap durex condoms purchase zovirax eye drops
Приветствую. Подскажите, где почитать разные блоги о недвижимости? Сейчас читаю https://santech31.ru
wow pve carry kreativwerkstatt-esens.de .
The story of how the incredibly talented footballer Riyad Mahrez https://alahli.riyad-mahrez-cz.com reached new heights in career, moving to Al Ahly and leading the team to victory.
The fascinating story of Antonio Rudiger’s transfer https://real-madrid.antonio-rudiger-cz.com to Real Madrid and his rapid rise as a key player at one of the best clubs in the world.
The fascinating story of Marcus Rashford’s ascent https://manchester-united.marcus-rashford-cz.com to glory in the Red Devils: from a young talent to one of the key players of the team.
Приветствую. Может кто знает, где почитать разные статьи о недвижимости? Сейчас читаю https://santex-expert.ru
Try to make a fascinating actor Johnny Depp https://secret-window.johnny-depp.cz, who will become the slave of his strong hero Moudriho Creeps in the thriller “Secret Window”.
Fascinating event related to this Keanu Reeves helped him in the role of the iconic John Wick characters https://john-wick.keanu-reeves.cz, among which there is another talent who has combat smarts with inappropriate charisma.
Jackie Chan https://peakhour.jackie-chan.cz from a poor boy from Hong Kong to a world famous Hollywood stuntman. The incredible success story of Jackie Chan.
Follow Liam Neeson’s career https://hostage.liam-neeson.cz as he fulfills his potential as Brian Mills in the film “Taken” and becomes one of the leading stars of Hollywood action films.
Emily Olivia Laura Blunt https://oppenheimer.emily-blunt.cz British and American actress. Winner of the Golden Globe (2007) and Screen Actors Guild (2019) awards.
Приветствую. Может кто знает, где найти разные блоги о недвижимости? Сейчас читаю https://schuconvr.ru
The inspiring story of Zendaya’s rise https://spider-man.zendaya-maree.cz, from her early roles to her blockbuster debut in Marvel Cinematic Universe.
The inspiring story of the ascent of the young actress Anya Taylor https://queensmove.anya-taylor-joy.cz to fame after her breakthrough performance in the TV series “The Queen’s Move”. Conquering new peaks.
An indomitable spirit, incredible skills and five championships – how Kobe Bryant https://losangeles-lakers.kobe-bryant.cz became an icon of the Los Angeles Lakers and the entire NBA world.
Carlos Vemola https://oktagon-mma.karlos-vemola.cz Czech professional mixed martial artist, former bodybuilder, wrestler and member Sokol.
Witness the thrilling story of Jiri Prochazka’s https://ufc.jiri-prochazka-ufc.cz rapid rise to the top of the UFC’s light heavyweight division, marked by his dynamic fighting style and relentless determination.
Всем привет! Подскажите, где почитать полезные блоги о недвижимости? Сейчас читаю https://simposad.ru
Jon Jones https://ufc.jon-jones.cz a dominant fighter with unrivaled skill, technique and physique who has conquered the light heavyweight division.
An article about the triumphant 2023 Ferrari https://ferrari.charles-leclerc.cz and their star driver Charles Leclerc, who became the Formula world champion 1.
Young Briton Lando Norris https://mclaren.lando-norris.cz is at the heart of McLaren’s Formula 1 renaissance, regularly achieving podium finishes and winning.
The legendary Spanish racer Fernando Alonso https://formula-1.fernando-alonso.cz returns to Formula 1 after several years.
外送茶
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
Приветствую. Может кто знает, где найти разные статьи о недвижимости? Сейчас читаю https://smgarant.ru
Activision and Call of Duty https://activision.call-of-duty.cz leading video game publisher and iconic shooter with a long history market dominance.
zabljak https://montenegro-real-estate-prices.com
Free movies https://www.moviesjoy.cc and TV streaming online, watch movies online in HD 1080p.
the most popular sports website https://sports-forecasts.com in the Arab world with the latest sports news, predictions and analysis in real time.
Latest news and analysis of the English Premier League https://epl-ar.com. Detailed descriptions of matches, team statistics and the most interesting football events.
Latest Diablo news https://diablo-ar.com, detailed game descriptions and guides. Diablo.az – The largest Diablo information portal in Arabic.
Всем привет! Может кто знает, где найти разные статьи о недвижимости? Сейчас читаю https://stilnyjpol.ru
Latest World of Warcraft tournament news https://ar-wow.com (WOW), strategies and game analysis. The most detailed gaming portal in Arabic.
NFL https://nfl-ar.com News, analysis and topics about the latest practices, victories and records. A portal that explores the most beautiful games in the NFL world in general.
The latest analysis, reviews of https://spider-man-ar.com tournaments and the most interesting things from the “Spider-Man” series of games in Azerbaijani language. It’s all here!
ankara seo
Discover exciting virtual football https://fortnite-ar.com in Fortnite. Your central hub for the latest news, expert strategy and exciting eSports reporting.
Latest Counter-Strike 2 news https://counter-strike-ar.com, watch the most successful tournaments and be the best in the gaming world on CS2 ar.
Приветствую. Может кто знает, где найти разные блоги о недвижимости? Пока нашел https://tc-all.ru
Всем привет! Может кто знает, где почитать разные блоги о недвижимости? Пока нашел https://teplohod-denisdavidov.ru
Latest boxing news, achievements of Raisol Abbasov https://boxing-ar.com, Tyson Fury fights and much more. It’s all about the boxing ambassador.
Discover the wonderful world of online games https://onlayn-oyinlar.com with GameHub. Get the latest news, reviews and tips for your favorite games. Join our gaming community today!
Sports news https://gta-uzbek.com the most respected sports site in Uzbekistan, which contains the latest sports news, forecasts and analysis.
Latest GTA game news https://gta-uzbek.com, tournaments, guides and strategies. Stay tuned for the best GTA gaming experience
Latest news from the world of boxing https://boks-uz.com, achievements of Resul Abbasov, Tyson Fury’s fights and much more. Everything Boxing Ambassador has.
seo hizmeti
Всем привет! Подскажите, где почитать полезные блоги о недвижимости? Пока нашел https://titovloft.ru
Online work has transformed the modern workplace, delivering adaptability and convenience that classic office environments frequently lack. It allows individuals to work from virtually any place with an internet connection, breaking down geographical barriers and facilitating companies to tap into a global talent pool. This change has led to a rise in telecommuting and freelance opportunities, permitting workers to manage their professional and personal lives more efficiently. Additionally, online work can lead to increased productivity and job satisfaction, as employees have more control over their calendars and work environments. However, it also introduces challenges such as maintaining work-life boundaries, ensuring effective communication, and managing time efficiently. Overall, online work is a transformative force, reshaping the way we think about employment and productivity in the digital age.
Explore the extraordinary journey of Kylian Mbappe https://mbappe-real-madrid.com, from his humble beginnings to global stardom.
Get the latest https://mesut-ozil-uz.com Mesut Ozil news, stats, photos and more.
Latest news about Pele https://mesut-ozil-uz.com, statistics, photos and much more. Get the latest news and information about football legend Pele.
Serxio Ramos Garsiya https://serxio-ramos.com ispaniyalik futbolchi, himoyachi. Ispaniya terma jamoasining sobiq futbolchisi. 16 mavsum davomida u “Real Madrid”da markaziy himoyachi sifatida o’ynadi.
Ronaldo de Asis Moreira https://ronaldinyo.com braziliyalik futbolchi, yarim himoyachi va hujumchi sifatida o’ynagan. Jahon chempioni (2002). “Oltin to’p” sovrindori (2005).
Всем привет! Подскажите, где почитать разные статьи о недвижимости? Сейчас читаю https://toadmarket.ru
Официальный сайт онлайн-казино Vavada https://vavada-kz-game.kz это новый адрес лучших слотов и джекпотов. Ознакомьтесь с бонусами и играйте на реальные деньги из Казахстана.
Marcus Lilian Thuram-Julien https://internationale.marcus-thuram-fr.com French footballer, forward for the Internazionale club and French national team.
Legendary striker Cristiano Ronaldo https://an-nasr.cristiano-ronaldo-fr.com signed a contract with the Saudi club ” An-Nasr”, opening a new chapter in his illustrious career in the Middle East.
Manchester City and Erling Haaland https://manchester-city.erling-haaland-fr.com explosive synergy in action. How a club and a footballer light up stadiums with their dynamic play.
Lionel Messi https://inter-miami.lionel-messi-fr.com legendary Argentine footballer, announced his transfer to the American club Inter Miami.
Приветствую. Подскажите, где найти полезные блоги о недвижимости? Пока нашел https://u-mechanik.ru
The official website where you can find everything about the career of Gianluigi Buffon https://gianluigi-buffon.com. Discover the story of this legendary goalkeeper who left his mark on football history and relive his achievements and unforgettable memories with us.
Website dedicated to football player Paul Pogba https://pogba-uz.com. Latest news from the world of football.
Welcome to our official website! Go deeper into Paulo Dybala’s https://paulo-dybala.com football career. Discover Dybala’s unforgettable moments, amazing talents and fascinating journey in the world of football on this site.
Latest news on the Vinicius Junior fan site https://vinisius-junior.com. Vinicius Junior has been playing since 2018 for Real Madrid (Real Madrid). He plays in the Left Winger position.
durex gel where to order – purchase durex gel online purchase latanoprost generic
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
Coffeeroom https://coffeeroom.by – магазин кофе, чая, кофетехники, посуды, химии и аксессуаров в Минске для дома и офиса.
Hello players!!
Reliability and convenience define MCW Casino for me. The swift registration process, substantial bonuses, and efficient withdrawals make every gaming session enjoyable. With the official website and dependable working mirror always accessible, I confidently recommend MCW Casino!
Mega Casino World offers outstanding quality and reliability. With bonuses for new players, high betting odds, and rapid withdrawals, the always-available mirror ensures seamless access. Playing and winning here is a pleasure. I highly recommend giving it a try!
Catch the site where everything is in the best shape! – MCW Casino
MCW Casino online personal account
download app Mega Casino World for free on iPhone
Mega Casino World official mobile site
Mega Casino World casino download on android for free
download Mega Casino World official app for android
Good profits!
Hello everyone!!
Achieve new heights of success at Baji999! Enjoy exciting casino games and sports betting with fantastic bonuses. Baji999 offers a secure, fun, and rewarding gaming experience. Start your winning streak today!
Step into success with Baji999! Experience the best in online casino gaming and sports betting. With attractive bonuses and a secure platform, Baji999 is your key to winning big. Join and play today!
Catch the site where everything is in the best shape! – Baji999
Baji999 Casino registration on official
Baji999 Casino download for free on iPhone
Baji999 Casino company
Baji999 Casino app download for free
Baji999 Casino mobile
Good profits!
Приветствую. Подскажите, где найти полезные статьи о недвижимости? Сейчас читаю https://utc96.ru
Прокат и аренда автомобилей https://autorent.by в Минске 2019-2022. Сутки от 35 руб.
Find the latest information on Khabib Nurmagomedov https://khabib-nurmagomedov.uz news and fights. Check out articles and videos detailing Khabib UFC career, interviews, wins, and biography.
Latest news and information about Marcelo https://marselo-uz.com on this site! Find Marcelo’s biography, career, game stats and more.
Всем привет! Подскажите, где почитать полезные статьи о недвижимости? Пока нашел https://vortex-los.ru
娛樂城
外送茶
外送茶是什麼?禁忌、價格、茶妹等級、術語等..老司機告訴你!
外送茶是什麼?
外送茶、外約、叫小姐是一樣的東西。簡單來說就是在通訊軟體與茶莊聯絡,選好自己喜歡的妹子後,茶莊會像送飲料這樣把妹子派送到您指定的汽車旅館、酒店、飯店等交易地點。您只需要在您指定的地點等待,妹妹到達後,就可以開心的開始一場美麗的約會。
外送茶種類
學生兼職的稱為清新書香茶
日本女孩稱為清涼綠茶
俄羅斯女孩被稱為金酥麻茶
韓國女孩稱為超細滑人參茶
外送茶價格
外送茶的客戶相當廣泛,包括中小企業主、自營商、醫生和各行業的精英,像是工程師等等。在台北和新北地區,他們的消費指數大約在 7000 到 10000 元之間,而在中南部則通常在 4000 到 8000 元之間。
對於一般上班族和藍領階層的客人來說,建議可以考慮稍微低消一點,比如在北部約 6000 元左右,中南部約 4000 元左右。這個價位的茶妹大多是新手兼職,但有潛力。
不同地區的客人可以根據自己的經濟能力和喜好選擇適合自己的價位範圍,以免感到不滿意。物價上漲是一個普遍現象,受到地區和經濟情況等因素的影響,茶莊的成本也在上升,因此價格調整是合理的。
外送茶外約流程
加入LINE:加入外送茶官方LINE,客服隨時為你服務。茶莊一般在中午 12 點到凌晨 3 點營業。
告知所在地區:聯絡客服後,告訴他們約會地點,他們會幫你快速找到附近的茶妹。
溝通閒聊:有任何約妹問題或需要查看妹妹資訊,都能得到詳盡的幫助。
提供預算:告訴客服你的預算,他們會找到最適合你的茶妹。
提早預約:提早預約比較好配合你的空檔時間,也不用怕到時候約不到你想要的茶妹。
外送茶術語
喝茶術語就像是進入茶道的第一步,就像是蓋房子打地基一樣。在這裡,我們將這些外送茶入門術語分類,讓大家能夠清楚地理解,讓喝茶變得更加容易上手。
魚:指的自行接客的小姐,不屬於任何茶莊。
茶:就是指「小姐」的意思,由茶莊安排接客。
定點茶:指由茶莊提供地點,客人再前往指定地點與小姐交易。
外送茶:指的是到小姐到客人指定地點接客。
個工:指的是有專屬工作室自己接客的小姐。
GTO:指雞頭也就是飯店大姊三七茶莊的意思。
摳客妹:只負責找客人請茶莊或代調找美眉。
內機:盤商應召站提供茶園的人。
經紀人:幫內機找美眉的人。
馬伕:外送茶司機又稱教練。
代調:收取固定代調費用的人(只針對同業)。
阿六茶:中國籍女子,賣春的大陸妹。
熱茶、熟茶:年齡比較大、年長、熟女級賣春者(或稱阿姨)。
燙口 / 高溫茶:賣春者年齡過高。
台茶:從事此職業的台灣小姐。
本妹:從事此職業的日本籍小姐。
金絲貓:西方國家的小姐(歐美的、金髮碧眼的那種)。
青茶、青魚:20 歲以下的賣春者。
乳牛:胸部很大的小姐(D 罩杯以上)。
龍、小叮噹、小叮鈴:體型比較肥、胖、臃腫、大隻的小姐。
Приветствую. Подскажите, где найти полезные статьи о недвижимости? Пока нашел https://yah-bomag.ru
Discover how Riyad Mahrez https://al-ahli.riyad-mahrez.com transformed Al-Ahli, becoming a key player and catalyst in reaching new heights in world football.
Find the latest information on Conor McGregor https://conor-mcgregor.uz news, fights, and interviews. Check out detailed articles and news about McGregor’s UFC career, wins, training, and personal life.
Get to know the history, players and latest news of the Inter Miami football club https://inter-miami.uz. Join us to learn about the successes and great performances of America’s newest and most exciting soccer club.
A site dedicated to Michael Jordan https://michael-jordan.uz, a basketball legend and symbol of world sports culture. Here you will find highlights, career, family and news about one of the greatest athletes of all time.
Explore the dynamic world of sports https://noticias-esportivas-br.org through the lens of a sports reporter. Your source for breaking news, exclusive interviews, in-depth analysis and live coverage of all sports.
Всем привет! Может кто знает, где почитать полезные блоги о недвижимости? Сейчас читаю https://yaoknaa.ru
The latest top football news https://futebol-ao-vivo.net today. Interviews with football players, online broadcasts and match results, analytics and football forecasts
If you are a fan of UFC https://ufc-hoje.com the most famous organization in the world, come visit us. The most important news and highlights from the UFC world await you on our website.
Site with the latest news, statistics, photos of Pele https://edson-arantes-do-nascimento.com and much more. Get the latest news and information about football legend Pele.
Welcome to our official website, where you will find everything about the career of Gianluigi Buffon https://gianluigi-buffon.org. Discover the story of this legendary goalkeeper who made football history.
The best site dedicated to the football player Paul Pogba https://pogba.org. Latest news from the world of football.
Vinicius Junior https://vinicius-junior.org all the latest current and latest news for today about the player of the 2024 season
Analysis of Arsenal’s impressive revival https://arsenal.bukayo-saka.biz under the leadership of Mikel Arteta and the key role of young star Bukayo Saki in the club’s return to the top.
Gavi’s success story https://barcelona.gavi-fr.com at Barcelona: from his debut at 16 to a key role in club and national team of Spain, his talent inspires the world of football.
Pedri’s story https://barcelona.pedri-fr.com from his youth in the Canary Islands to becoming a world-class star in Barcelona, ??with international success and recognition.
Приветствую. Подскажите, где найти полезные блоги о недвижимости? Сейчас читаю https://zt365.ru
clomid online australia
Геракл24: Профессиональная Реставрация Основания, Венцов, Покрытий и Передвижение Зданий
Компания Gerakl24 занимается на предоставлении полных сервисов по замене основания, венцов, настилов и переносу зданий в городе Красноярск и за его пределами. Наш коллектив профессиональных экспертов обеспечивает высокое качество выполнения всех типов восстановительных работ, будь то деревянные, каркасного типа, кирпичные постройки или бетонные дома.
Достоинства работы с Gerakl24
Навыки и знания:
Все работы осуществляются исключительно высококвалифицированными мастерами, с обладанием большой стаж в области создания и ремонта зданий. Наши специалисты профессионалы в своем деле и осуществляют проекты с безупречной точностью и учетом всех деталей.
Полный спектр услуг:
Мы предоставляем полный спектр услуг по ремонту и восстановлению зданий:
Замена фундамента: укрепление и замена старого фундамента, что обеспечивает долгий срок службы вашего дома и устранить проблемы, вызванные оседанием и деформацией.
Реставрация венцов: восстановление нижних венцов деревянных зданий, которые чаще всего подвергаются гниению и разрушению.
Смена настилов: монтаж новых настилов, что существенно улучшает внешний облик и функциональность помещения.
Передвижение домов: качественный и безопасный перенос строений на новые локации, что обеспечивает сохранение строения и избежать дополнительных затрат на строительство нового.
Работа с любыми видами зданий:
Древесные строения: восстановление и защита деревянных строений, защита от гниения и вредителей.
Дома с каркасом: реставрация каркасов и реставрация поврежденных элементов.
Дома из кирпича: восстановление кирпичной кладки и укрепление конструкций.
Бетонные дома: ремонт и укрепление бетонных конструкций, устранение трещин и повреждений.
Надежность и долговечность:
Мы применяем только высококачественные материалы и современное оборудование, что обеспечивает долгий срок службы и прочность всех выполненных задач. Каждый наш проект подвергаются строгому контролю качества на каждом этапе выполнения.
Личный подход:
Для каждого клиента мы предлагаем индивидуальные решения, учитывающие все особенности и пожелания. Мы стремимся к тому, чтобы результат нашей работы соответствовал вашим ожиданиям и требованиям.
Почему выбирают Геракл24?
Сотрудничая с нами, вы получаете надежного партнера, который возьмет на себя все хлопоты по восстановлению и ремонту вашего здания. Мы обещаем выполнение всех задач в установленные сроки и с соблюдением всех правил и норм. Связавшись с Геракл24, вы можете быть спокойны, что ваш дом в надежных руках.
Мы предлагаем консультацию и ответить на все ваши вопросы. Звоните нам, чтобы обсудить детали вашего проекта и узнать больше о наших услугах. Мы обеспечим сохранение и улучшение вашего дома, сделав его безопасным и комфортным для проживания на долгие годы.
Gerakl24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
Всем привет! Может кто знает, где почитать полезные блоги о недвижимости? Сейчас читаю https://astali.ru
Discover the journey of Charles Leclerc https://ferrari.charles-leclerc-fr.com, from young Monegasque driver to Ferrari Formula 1 leader, from his early years to his main achievements within the team.
Discover Pierre Gasly’s https://alpine.pierre-gasly.com journey through the world of Formula 1, from his beginnings with Toro Rosso to his extraordinary achievements with Alpine.
Leroy Sane’s https://bavaria.leroy-sane-ft.com success story at FC Bayern Munich: from adaptation to influence on the club’s results. Inspiration for hard work and professionalism in football.
From childhood teams to championship victories, the path to success with the Los Angeles Lakers https://los-angeles-lakers.lebron-james-fr.com requires not only talent, but also undeniable dedication and work.
Discover the story of Rudy Gobert https://minnesota-timberwolves.rudy-gobert.biz, the French basketball player whose defensive play and leadership transformed the Minnesota Timberwolves into a powerhouse NBA team.
Букмекерская контора 7к казино предлагает разнообразие высококачественных игровых слотов, чтобы удовлетворить все ваши игровые предпочтения и желания – работающее зеркало 7k casino
Всем привет! Может кто знает, где найти разные статьи о недвижимости? Пока нашел https://batstroimat24.ru
What’s Taking place i am new to this, I stumbled upon this I’ve found It positively useful and it has aided me
out loads. I’m hoping to give a contribution & help
different users like its helped me. Great job.
The story of the Moroccan footballer https://al-hilal.yassine-bounou.com, who became a star at Al-Hilal, traces his journey from the streets of Casablanca to international football stardom and his personal development.
Victor Wembanyama’s travel postcard https://san-antonio-spurs.victor-wembanyama.biz from his career in France to his impact in the NBA with the San Antonio Spurs.
The history of Michael Jordan’s Chicago Bulls https://chicago-bulls.michael-jordan-fr.com extends from his rookie in 1984 to a six-time NBA championship.
Neymar https://al-hilal.neymar-fr.com at Al-Hilal: his professionalism and talent inspire young people players, taking the club to new heights in Asian football.
Golden State Warriors success story https://golden-state-warriors.stephen-curry-fr.com Stephen Curry: From becoming a leader to creating a basketball dynasty that redefined the game.
Замена венцов красноярск
Геракл24: Опытная Замена Фундамента, Венцов, Полов и Перенос Домов
Компания Gerakl24 специализируется на выполнении комплексных работ по замене основания, венцов, настилов и переносу зданий в населённом пункте Красноярском регионе и за его пределами. Наша группа опытных экспертов гарантирует высокое качество реализации различных типов восстановительных работ, будь то из дерева, каркасные, кирпичные или из бетона дома.
Плюсы работы с Геракл24
Навыки и знания:
Все работы выполняются исключительно высококвалифицированными экспертами, с обладанием долгий практику в направлении создания и ремонта зданий. Наши специалисты знают свое дело и осуществляют проекты с безупречной точностью и вниманием к мелочам.
Комплексный подход:
Мы предоставляем полный спектр услуг по ремонту и ремонту домов:
Замена фундамента: укрепление и замена старого фундамента, что обеспечивает долгий срок службы вашего дома и избежать проблем, связанные с оседанием и деформацией.
Замена венцов: замена нижних венцов деревянных домов, которые обычно подвергаются гниению и разрушению.
Замена полов: замена старых полов, что значительно улучшает внешний вид и функциональность помещения.
Перенос строений: качественный и безопасный перенос строений на новые локации, что позволяет сохранить ваше строение и предотвращает лишние расходы на создание нового.
Работа с любыми видами зданий:
Деревянные дома: восстановление и укрепление деревянных конструкций, обработка от гниения и насекомых.
Каркасные строения: реставрация каркасов и смена поврежденных частей.
Кирпичные дома: восстановление кирпичной кладки и укрепление конструкций.
Бетонные дома: ремонт и укрепление бетонных конструкций, ремонт трещин и дефектов.
Качество и прочность:
Мы применяем только проверенные материалы и современное оборудование, что гарантирует долговечность и надежность всех работ. Каждый наш проект подвергаются строгому контролю качества на каждом этапе выполнения.
Персонализированный подход:
Мы предлагаем каждому клиенту индивидуальные решения, с учетом всех особенностей и пожеланий. Наша цель – чтобы конечный результат полностью удовлетворял вашим запросам и желаниям.
Зачем обращаться в Геракл24?
Работая с нами, вы получаете надежного партнера, который берет на себя все заботы по ремонту и реставрации вашего дома. Мы обещаем выполнение всех работ в сроки, оговоренные заранее и с в соответствии с нормами и стандартами. Обратившись в Геракл24, вы можете не сомневаться, что ваш дом в надежных руках.
Мы готовы предоставить консультацию и дать ответы на все вопросы. Свяжитесь с нами, чтобы обсудить детали вашего проекта и узнать о наших сервисах. Мы поможем вам сохранить и улучшить ваш дом, обеспечив его безопасность и комфорт на долгие годы.
Геракл24 – ваш выбор для реставрации и ремонта домов в Красноярске и области.
Всем привет! Может кто знает, где найти разные блоги о недвижимости? Пока нашел https://bdrsu-2.ru
Del Mar Energy is an international industrial holding company engaged in the extraction of oil, gas, and coal
The success story of the French footballer https://juventus.thierry-henry.biz at Juventus: from his career at the club to leadership on the field , becoming a legend and a source of inspiration for youth.
The story of the great Kobe Bryant https://los-angeles-lakers.kobe-bryant-fr.com with ” Los Angeles Lakers: his path to the championship, his legendary achievements.
Novak Djokovic’s https://tennis.novak-djokovic-fr.biz journey from childhood to the top of world tennis: early years, first victories, dominance and influence on the sport.
Find out the story of Jon Jones https://ufc.jon-jones-fr.biz in the UFC: his triumphs, records and controversies, which made him one of the greatest fighters in the MMA world.
Приветствую. Может кто знает, где найти полезные статьи о недвижимости? Сейчас читаю https://centro-kraska.ru
娛樂城
medicine lyrica 75 mg
Казино 7k casino предоставляет доступ к информации о вероятности выигрыша в каждой игре – переход на r7 casino
Приветствую. Может кто знает, где почитать разные блоги о недвижимости? Сейчас читаю https://cvetkrovli.ru
При регистрации в казино 7k casino вы можете воспользоваться специальным промокодом и получить бонус – р7 казино официальное зеркало сайта
Свежий бренд казино 7k casino, основанный в 2023 году, с первых дней привлекает поклонников азартных игр своим качеством и разнообразием услуг, что делает его потенциальным лидером в рейтинге лучших казино – 7к казино работающее зеркало сайта
Сегодняшнее рабочее зеркало официального сайта букмекерской конторы 7к казино обеспечивает удобный доступ к нашим услугам в любое время и из любого места, чтобы вы могли наслаждаться игрой где угодно и когда угодно – 7k casino рабочее зеркало страницы
7к казино гарантирует надежную защиту от незаконных действий и мошенничества в онлайн сфере – игровые автоматы r7 casino регистрация
Приветствую. Может кто знает, где найти полезные блоги о недвижимости? Пока нашел https://deon-stroy.ru
꽁 머니 슬롯
거의 아침부터 밤까지 거의 두 달 동안의 연습은 결코 멈추지 않았습니다.
Букмекерская контора обеспечивает надежную защиту от незаконных действий и мошенников в онлайн сфере – Марафонбет официальная страницы
Carlos Alcaraz https://tennis.carlos-alcaraz-fr.biz from a talented junior to the ATP top 10. His rise is the result of hard work, support and impressive victories at major world tournaments.
Jannik Sinner https://tennis.jannik-sinner-fr.biz an Italian tennis player, went from starting his career to entering the top 10 of the ATP, demonstrating unique abilities and ambitions in world tennis.
The fascinating story of Daniil Medvedev’s https://tennis.daniil-medvedev-fr.biz rise to world number one. Find out how a Russian tennis player quickly broke into the elite and conquered the tennis Olympus.
Discover Casper Ruud’s https://tennis.casper-ruud-fr.com journey from his Challenger debut to the top 10 of the world tennis rankings. A unique success.
The fascinating story of Alexander Zverev’s https://tennis.alexander-zverev-fr.biz rapid rise from a junior star to one of the leaders of modern tennis.
Игроки могут участвовать в программе VIP-клуба казино 7k casino – р7 казино онлайн официальный
Букмекерская контора 7к казино предлагает разнообразие качественных игровых слотов, удовлетворяющих различным предпочтениям игроков – р7 казино официальный сайт регистрация
Всем привет! Может кто знает, где почитать разные статьи о недвижимости? Пока нашел https://dom-vasilevo.ru
wow heroic raid boost https://kreativwerkstatt-esens.de/ .
buy generic minoxidil – buy dutas pills proscar uk
Рабочее зеркало 7k casino казино на сегодня доступно для игры – 7k casino актуальное рабочее зеркало
cheap minoxidil – buy finasteride 1mg sale buy finpecia generic
Мы гордимся предлагать обширную коллекцию высококачественных игровых слотов в букмекерской конторе 7к казино, которая удовлетворит самые изысканные вкусы и предпочтения игроков – 7k casino
NetTruyen ZZZ: Nền tảng đọc truyện tranh trực tuyến dành cho mọi lứa tuổi
NetTruyen ZZZ là nền tảng đọc truyện tranh trực tuyến miễn phí với số lượng truyện tranh lên đến hơn 30.000 đầu truyện với chất lượng hình ảnh và tốc độ tải cao. Nền tảng được xây dựng với mục tiêu mang đến cho người đọc những trải nghiệm đọc truyện tranh tốt nhất, đồng thời tạo dựng cộng đồng yêu thích truyện tranh sôi động và gắn kết với hơn 11 triệu thành viên (tính đến tháng 7 năm 2024).
NetTruyen ZZZ – Kho tàng truyện tranh phong phú:
NetTruyen ZZZ sở hữu kho tàng truyện tranh khổng lồ với hơn 30.000 đầu truyện thuộc nhiều thể loại khác nhau như:
● Manga: Những bộ truyện tranh Nhật Bản với nhiều thể loại phong phú như lãng mạn, hành động, hài hước, v.v.
● NetTruyen anime: Hàng ngàn bộ truyện tranh anime chọn lọc được đăng tải đều đặn trên NetTruyen ZZZ được chuyển thể từ phim hoạt hình Nhật Bản với nội dung hấp dẫn và hình ảnh đẹp mắt.
● Truyện manga: Hơn 10.000 bộ truyện tranh manga hay nhất được đăng tải đầy đủ trên NetTruyen ZZZ.
● Truyện manhua: Hơn 5000 bộ truyện tranh manhua được đăng tải trọn bộ đầy đủ trên NetTruyen ZZZ.
● Truyện manhwa: Những bộ truyện tranh manhwa Hàn Quốc được yêu thích nhất có đầy đủ trên NetTruyen với cốt truyện lôi cuốn và hình ảnh bắt mắt cùng với nét vẽ độc đáo và nội dung đa dạng.
● Truyện ngôn tình: Những câu chuyện tình yêu lãng mạn, ngọt ngào và đầy cảm xúc.
● Truyện trinh thám: Những câu chuyện ly kỳ, bí ẩn và đầy lôi cuốn xoay quanh các vụ án và quá trình phá án.
● Truyện tranh xuyên không: Những câu chuyện về những nhân vật du hành thời gian hoặc không gian đến một thế giới khác.
NetTruyen ZZZ không ngừng cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường, đảm bảo mang đến cho bạn đọc những trải nghiệm đọc truyện mới mẻ và thú vị nhất.
Chất lượng hình ảnh và nội dung đỉnh cao tại NetTruyenZZZ:
Với hơn 30 triệu lượt truy cập hằng tháng, NetTruyen ZZZ luôn chú trọng vào chất lượng hình ảnh và nội dung của các bộ truyện tranh được đăng tải trên nền tảng. Hình ảnh được hiển thị sắc nét, rõ ràng, không bị mờ hay vỡ ảnh. Nội dung được dịch thuật chính xác, dễ hiểu và giữ nguyên vẹn ý nghĩa của tác phẩm gốc.
NetTruyen ZZZ hợp tác với đội ngũ dịch giả và biên tập viên chuyên nghiệp, giàu kinh nghiệm để đảm bảo chất lượng bản dịch tốt nhất. Nền tảng cũng có hệ thống kiểm duyệt nội dung nghiêm ngặt để đảm bảo nội dung lành mạnh, phù hợp với mọi lứa tuổi.
Trải nghiệm đọc truyện mượt mà, tiện lợi:
NetTruyen ZZZ được thiết kế với giao diện đẹp mắt, thân thiện với người dùng và dễ dàng sử dụng. Bạn đọc có thể đọc truyện tranh trên mọi thiết bị, từ máy tính, điện thoại thông minh đến máy tính bảng. Nền tảng cũng cung cấp nhiều tính năng tiện lợi như:
● Tìm kiếm truyện tranh theo tên, tác giả, thể loại, v.v.
● Lưu truyện tranh yêu thích để đọc sau.
● Đánh dấu trang để dễ dàng quay lại vị trí đang đọc.
● Chia sẻ truyện tranh với bạn bè.
● Tham gia bình luận và thảo luận về truyện tranh.
NetTruyen ZZZ luôn nỗ lực để mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
Định hướng phát triển:
NetTruyen ZZZ cam kết không ngừng phát triển và hoàn thiện để trở thành nền tảng đọc truyện tranh trực tuyến tốt nhất dành cho bạn đọc tại Việt Nam. Nền tảng sẽ tiếp tục cập nhật những bộ truyện tranh mới nhất và hot nhất trên thị trường thế giới, đồng thời nâng cao chất lượng hình ảnh và nội dung. NetTruyen ZZZ cũng sẽ phát triển thêm nhiều tính năng mới để mang đến cho bạn đọc những trải nghiệm đọc truyện tốt nhất.
NetTruyen ZZZ luôn đặt lợi ích của bạn đọc lên hàng đầu. Nền tảng cam kết:
● Cung cấp kho tàng truyện tranh khổng lồ và đa dạng với chất lượng hình ảnh và nội dung đỉnh cao.
● Mang đến cho bạn đọc những trải nghiệm đọc truyện mượt mà, tiện lợi và thú vị nhất.
● Luôn lắng nghe ý kiến phản hồi của bạn đọc và không ngừng cải thiện để mang đến dịch vụ tốt nhất.
NetTruyen ZZZ hy vọng sẽ trở thành người bạn đồng hành không thể thiếu của bạn trong hành trình khám phá thế giới truyện tranh đầy màu sắc.
Kết nối với NetTruyen ZZZ ngay hôm nay để tận hưởng những trải nghiệm đọc truyện tuyệt vời.
На главной странице нашего сайта casino представлена всесторонняя информация о Казино 7к казино, позволяющая вам ознакомиться со всеми нашими предложениями и возможностями – зеркало сайта 7k casino
order generic leflunomide 20mg – buy risedronate 35mg generic cartidin where to buy
Наше казино Риобет предлагает захватывающий игровой опыт с привлекательной графикой и высоким качеством игровых слотов на реальные деньги, чтобы удовлетворить даже самые взыскательные вкусы – Риобет работающее зеркало
The legendary boxing world champion Mike Tyson https://ufc.mike-tyson-fr.biz made an unexpected transition to the UFC in 2024, where he rose to the top, becoming the oldest heavyweight champion.
The powerful story of Conor McGregor’s https://ufc.conor-mcgregor-fr.biz rise to a two-division UFC championship that forever changed the landscape of mixed martial arts.
The fascinating story of how Lewis Hamilton https://mercedes.lewis-hamilton-fr.biz became a seven-time Formula 1 world champion after signing with Mercedes.
The story of Fernando Alonso https://formula-1.fernando-alonso-fr.com in Formula 1: a unique path to success through talent, tenacity and strategic decisions, inspiring and exciting.
The fascinating story of the creation and rapid growth of Facebook https://facebook.mark-zuckerberg-fr.biz under the leadership of Mark Zuckerberg, who became one of the most influential technology entrepreneurs of our time.
Букмекерская контора Риобет предлагает широкий выбор высококачественных игровых слотов, чтобы удовлетворить различные предпочтения игроков и предоставить им незабываемые игровые впечатления – работающее сайта Riobet
Kim Kardashian’s https://the-kardashians.kim-kardashian-fr.com incredible success story, from sex scandal to pop culture icon and billion-dollar fortune.
Max Verstappen and Red Bull Racing’s https://red-bull-racing.max-verstappen-fr.com path to success in Formula 1. A story of talent, determination and team support leading to a championship title.
Une ascension fulgurante au pouvoir Donald Trump https://usa.donald-trump-fr.com et son empire commercial
The astonishing story of Emmanuel Macron’s https://president-of-france.emmanuel-macron-fr.com political rise from bank director to the highest office in France.
The story of Joe Biden’s https://president-of-the-usa.joe-biden-fr.com triumphant journey, overcoming many obstacles on his path to the White House and becoming the 46th President of the United States.
Обзор официального сайта букмекерской конторы Риобет содержит полезную информацию для ознакомления – Riobet рабочее зеркало на сегодня
купить диплом автослесаря ast-diplomas.com .
Parisian PSG https://paris.psg-fr.com is one of the most successful and ambitious football clubs in Europe. Find out how he became a global football superstar.
Olympique de Marseille https://liga1.marseilles-fr.com after several years in the shadows, once again becomes champion of France. How did they do it and what prospects open up for the club
Travel to the pinnacle of French football https://stadede-bordeaux.bordeaux-fr.org at the Stade de Bordeaux, where the passion of the game meets the grandeur of architecture.
The fascinating story of Gigi Hadid’s rise to Victoria’s Secret Angel https://victorias-secret.gigi-hadid-fr.com status and her journey to the top of the modeling industry.
Добрый день!
Мы можем предложить дипломы любой профессии по приятным тарифам.
Мы предлагаем документы ВУЗов, расположенных на территории всей Российской Федерации. Вы имеете возможность купить диплом от любого заведения, за любой год, указав подходящую специальность и оценки за все дисциплины. Дипломы и аттестаты печатаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Документы заверяются необходимыми печатями и подписями.
Даем гарантию, что в случае проверки документов работодателем, каких-либо подозрений не появится.
Где приобрести диплом специалиста?
http://www.markusragger.at/chess/index.php/kforum/jm-news-pro-module/577466
The fascinating story of the creation and meteoric rise of Amazon https://amazon.jeff-bezos-fr.com from its humble beginnings as an online bookstore to its dominant force in the world of e-commerce.
A fascinating story about how Elon Musk https://spacex.elon-musk-fr.com and his company SpaceX revolutionized space exploration, opening new horizons for humanity.
An exploration of Nicole Kidman’s https://watch.nicole-kidman-fr.com career, her notable roles, and her continued quest for excellence as an actress.
The inspiring story of Travis Scott’s https://yeezus.travis-scott-fr.com rise from emerging artist to one of modern hip-hop’s brightest stars through his collaboration with Kanye West.
How Taylor Swift https://midnights.taylor-swift-fr.com reinvented her sound and image on the intimate and reflective album “Midnights,” revealing new dimensions of her talent.
Dedicated to Stream lovers !
Discover Limelight Stream, where your entertainment experience reaches new heights. Our platform offers a comprehensive collection of movies, TV series, documentaries, and exclusive content, all curated to satisfy diverse tastes. We pride ourselves on delivering stunning HD quality for a flawless viewing experience. Our user-friendly interface allows you to explore and find content effortlessly, ensuring you spend more time watching and less time searching. Whether you’re looking for the latest blockbuster, a timeless classic, or an exclusive series, https://www.limelight-stream.com// has it all. Stream on your TV, laptop, tablet, or smartphone, and enjoy uninterrupted entertainment wherever you are. Join us today and explore a world of premium content that’s always at your fingertips.
Limelight user feedback
Stream games to iOS
Best game streaming apps
Limelight controller configuration
Limelight network requirements
Good luck!
Explore the rich history and unrivaled atmosphere of the iconic Old Trafford Stadium https://old-trafford.manchester-united-fr.com, home of one of the world’s most decorated football clubs, Manchester United.
Букмекерская контора 7к казино предоставляет детальный обзор официального сайта для ознакомления – 7к казино рабочее сайта
Казино 7k casino предлагает несколько живых игр, доступных в их мобильном приложении – рабочее зеркало страницы 7к казино
air montenegro Visit Montenegro
Игроки могут насладиться атмосферой реального казино благодаря HD-трансляциям в играх с живыми дилерами – r7 casino актуальное рабочее на сегодня
Единственная в России студия кастомных париков https://wigdealers.ru, где мастера индивидуально подбирают структуру волос и основу по форме головы, после чего стригут, окрашивают, делают укладку и доводят до идеала ваш будущий аксессуар.
The iconic Anfield https://enfield.liverpool-fr.com stadium and the passionate Liverpool fans are an integral part of English football culture.
An exploration of the history of Turin’s https://turin.juventus-fr.org iconic football club – Juventus – its rivalries, success and influence on Italian football.
The new Premier League https://premier-league.chelsea-fr.com season has gotten off to an intriguing start, with a new-look Chelsea looking to return to the Champions League, but serious challenges lie ahead.
Мы с гордостью представили бренд казино 7k casino в 2023 году, и наше усилие было вознаграждено, когда он немедленно привлек внимание азартных игроков своим качеством и разнообразием услуг, занимая верхние места в рейтинге – игровые автоматы официальный сайт r7 casino
Tyson Fury https://wbc.tyson-fury-fr.com is the undefeated WBC world champion and reigns supreme in boxing’s heavyweight division.
Explore the career and significance of Monica Bellucci https://malena.monica-bellucci-fr.com in Malena (2000), which explores complex themes of beauty and human strength in wartime.
Inter Miami FC https://mls.inter-miami-fr.com has become a major player in MLS thanks to its star roster, economic growth and international influence.
Discover Rafael Nadal’s https://mls.inter-miami-fr.com impressive rise to the top of world tennis, from his debut to his career Grand Slam victory.
The story of Kanye West https://the-college-dropout.kanye-west-fr.com, starting with his debut album “The College Dropout,” which changed hip-hop and became his cultural legacy.
accutane where to get
Преимущества аренды склада https://popivy.ru/otvetstvennoe-hranenie-mebeli-santehniki-i-bytovoj-tehniki-na-sklade-v-moskve-preimushhestva-i-vygody/, как аренда складских помещений может улучшить ваш бизнес
The fascinating story of the phenomenal rise and meteoric fall of Diego Maradona https://napoli.diegomaradona.biz, who became a cult figure at Napoli in the 1980s.
Rivaldo, or Rivaldo https://barcelona.rivaldo-br.com, is one of the greatest football players to ever play for Barcelona.
A fascinating story about Brazilian veteran Thiago Silva’s https://chelsea.thiago-silva.net difficult path to the top of European football as part of Chelsea London.
Explore the remarkable journey of Vinicius Junior https://real-madrid.vinicius-junior.net, the Brazilian prodigy who conquered the world’s biggest stage with his dazzling skills and unparalleled ambition at Real Madrid.
Cristiano Ronaldo https://al-nassr.cristianoronaldo-br.net one of the greatest football players of all time, begins a new chapter in his career by joining An Nasr Club.
The fascinating story of Marcus Rashford’s rise https://manchester-united.marcusrashford-br.com from academy youth to the main striker and captain of Manchester United. Read about his meteoric rise and colorful career.
The story of Luka Modric’s rise https://real-madrid.lukamodric-br.com from young talent to one of the greatest midfielders of his generation and a key player for the Royals.
From academy product to captain and leader of Real Madrid https://real-madrid.ikercasillas-br.com Casillas became one of the greatest players in the history of Real Madrid.
Follow Bernardo Silva’s impressive career https://manchester-city.bernardosilva.net from his debut at Monaco to to his status as a key player and leader of Manchester City.
Всем привет! Может кто знает, где найти полезные статьи о недвижимости? Сейчас читаю https://2204000.ru
buy generic arava 10mg – order generic leflunomide 10mg cheap cartidin online
토토 메이저
그러나 이것이 Fang Jifan이 방향을 조정했다는 의미는 아닙니다.
сайт казино рио бет вход Rio Bet Casino
регистрация рио бет казино Rio Bet Casino
реристрация Dragon Money Casino сайт драгон мани казино
официальный сайт драгон мани казино драгон мани казино
Хотите научиться готовить самые изысканные и сложные торты? В этом https://v1.skladchik.org/tags/tort/ разделе вы найдете множество подробных пошаговых рецептов самых трендовых и известных тортов с возможностью получить их за сущие копейки благодаря складчине. Готовьте с удовольствием и открывайте для себя новые рецепты вместе с Skladchik.org
купить диплом в спб ast-diplomas.com .
Всем привет! Может кто знает, где почитать полезные статьи о недвижимости? Сейчас читаю https://adeldv.ru
Лучшие пансионаты для пожилых людей https://ernst-neizvestniy.ru в Самаре – недорогие дома для престарелых в Самарской области
Пансионаты для пожилых людей https://moyomesto.ru в Самаре по доступным ценам. Специальные условия по уходу, индивидуальные программы.
The fascinating story of Sergio Ramos’ https://seville.sergioramos.net rise from Sevilla graduate to one of Real Madrid and Spain’s greatest defenders.
Ousmane Dembele’s https://paris-saint-germain.ousmanedembele-br.com rise from promising talent to key player for French football giants Paris Saint-Germain. An exciting success story.
Приветствую. Может кто знает, где найти полезные статьи о недвижимости? Сейчас читаю https://eniseynev.ru
order atenolol sale – cheap tenormin carvedilol online
azithromycin tablets online without prescription usa
Приветствую. Может кто знает, где почитать разные статьи о недвижимости? Пока нашел https://fuseitdecore.ru
The incredible success story of 20-year-old Florian Wirtz https://bayer-04.florianwirtz-br.com, who quickly joined the Bayer team and became one of the best young talents in the world.
The incredible story https://napoli.khvichakvaratskhelia-br.com of a young Georgian talent’s transformation into an Italian Serie A star. Khvicha Kvaraeshvili is a rising phenomenon in European football.
The compelling story of Alisson Becker’s https://bayer-04.florianwirtz-br.com meteoric rise from young talent to key figure in Liverpool’s triumphant era under Jurgen Klopp.
O meio-campista Rafael Veiga leva https://palmeiras.raphaelveiga-br.com o Palmeiras ao sucesso – o campeonato brasileiro e a vitoria na Copa Libertadores aos 24 anos.
Midfielder Rafael Veiga leads https://manchester-city.philfoden-br.com Palmeiras to success – the championship Brazilian and victory in the Copa Libertadores at the age of 24.
Всем привет! Может кто знает, где почитать разные статьи о недвижимости? Сейчас читаю https://galastroy-sk.ru
In-depth articles about the most famous football players https://zenit-saint-petersburg.wendel-br.com, clubs and events. Learn everything about tactics, rules of the game and football history.
The rise of 20-year-old midfielder Jamal Musiala https://bavaria.jamalmusiala-br.com to the status of a winger in the Bayern Munich team. A story of incredible talent.
A historia da jornada triunfante de Anitta https://veneno.anitta-br.com de aspirante a cantora a uma das interpretes mais influentes da musica moderna, incluindo sua participacao na serie de TV “Veneno”.
Fabrizio Moretti https://the-strokes.fabriziomoretti-br.com the influential drummer of The Strokes, and his unique sound revolutionized the music scene, remaining icons of modern rock.
Selena Gomez https://calm-down.selenagomez-br.net the story from child star to global musical influence, summarized in hit “Calm Down”, with Rema.
how to get provigil prescription
buy generic verapamil – buy generic verapamil over the counter tenoretic pill
verapamil 120mg pills – diltiazem without prescription tenoretic for sale online
купить аттестат за 11 класс купить аттестат за 11 класс .
Приветствую. Подскажите, где почитать полезные блоги о недвижимости? Пока нашел https://ggs45.ru
Добрый день!
Где заказать диплом специалиста?
Мы предлагаем дипломы любой профессии по приятным тарифам.
iawbs.com/home.php?mod=space&uid=792962&do=profile&from=space
There is certainly a great deal to learn about
this subject. I like all the points you’ve made.
best over the counter tretinoin cream
Всем привет! Подскажите, где почитать разные блоги о недвижимости? Пока нашел https://glwin.ru
Здравствуйте!
Приобретение диплома ВУЗа с сокращенной программой обучения в Москве
4division.ru/viewtopic.php?f=13&t=8571
Рады оказать помощь!.
Всем привет! Подскажите, где почитать полезные статьи о недвижимости? Пока нашел https://gor-bur.ru
amoxicillin 1g price
Всем привет! Подскажите, где найти полезные статьи о недвижимости? Сейчас читаю https://hameleon1.ru
파워 슬롯
“너…” Zhou Tanzhi는 피비린내 나는 꾸중을 들었다.
Kobe Bryant https://los-angeles-lakers.kobebryant-br.net one of the greatest basketball players of all the times, left an indelible mark on the history of sport.
Bieber’s https://baby.justinbieber-br.com path to global fame began with his breakthrough success Baby, which became his signature song and one of the most popular music videos of all time.
In the world of professional tennis, the name of Gustavo Kuerten https://roland-garros.gustavokuerten.com is closely linked to one of the most prestigious Grand Slam tournaments – Roland Garros.
Achraf Hakimi https://paris-saint-germain.ashrafhakimi.net is a young Moroccan footballer who quickly reached the football elite European in recent years.
Ayrton Senna https://mclaren.ayrtonsenna-br.com is one of the greatest drivers in the history of Formula 1.
купить диплом института в санкт петербурге asxdiplomik.com/kupit-diplom-moskva .
Всем привет! Может кто знает, где почитать разные блоги о недвижимости? Пока нашел https://iskrb.ru
bursa görüntülü diafon en uygun fiyat garantisi
Здравствуйте!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по разумным тарифам. Цена зависит от выбранной специальности, года получения и образовательного учреждения.
Где купить диплом специалиста?
Приобрести диплом о высшем образовании
arusak-diploms-srednee.ru/svidetelstvo-o-brake
Хорошей учебы!
Всем привет! Может кто знает, где почитать полезные блоги о недвижимости? Сейчас читаю https://juzhnybereg24.ru
Anderson Silva https://killer-bees-muay-thai-college.andersonsilva.net was born in 1975 in Curitiba Brazil. From a young age he showed an interest in martial arts, starting to train in karate at the age of 5.
Daniel Alves https://paris-saint-germain.danielalves.net is a name that symbolizes the greatness of the world of football.
Bruno Miguel Borges Fernandes https://manchester-united.brunofernandes-br.com was born on September 8, 1994 in Maia, Portugal.
Rodrygo Silva de Goes https://real-madrid.rodrygo-br.com, known simply as Rodrygo, emerged as one of the the brightest young talents in world football.
Nuno Mendes https://paris-saint-germain.nuno-mendes.com, a talented Portuguese left-back, He quickly became one of the key figures in the Paris Saint-Germain (PSG) team.
Здравствуйте!
Заказать документ о получении высшего образования можно у нас в Москве.
ast-diplomy.com/kupit-diplom-magistra
Успехов в учебе!
Здравствуйте!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать
av.flyboard.ru/viewtopic.php?f=9&t=1430&sid=94086248d862294a8237ee05a3de5001
Будем рады вам помочь!.
Приветствую. Может кто знает, где почитать полезные статьи о недвижимости? Пока нашел https://klimat-hck.ru
Earvin “Magic” Johnson https://los-angeles-lakers.magicjohnson.biz is one of the most legendary basketball players in history. NBA history.
Vinicius Junior https://real-madrid.vinicius-junior-ar.com the Brazilian prodigy whose full name is Vinicius Jose Baixao de Oliveira Junior, has managed to win the hearts of millions of fans around the world in a short period of time.
Victor Osimhen https://napoli.victorosimhen-ar.com born on December 29, 1998 in Lagos, Nigeria, has grown from an initially humble player to one of the brightest strikers in modern football.
Toni Kroos https://real-madrid.tonikroos-ar.com the German midfielder known for his accurate passes and calmness on the field, has achieved remarkable success at one of the most prestigious football clubs in the world.
Robert Lewandowski https://barcelona.robertlewandowski-ar.com is one of the most prominent footballers of our time, and his move to Barcelona has become one of the most talked about topics in world football.
Приветствую. Подскажите, где почитать полезные блоги о недвижимости? Пока нашел https://kolahouse.ru
Казино Marathonbet предлагает различные варианты автоматической игры на игровых автоматах – БК Марафон официальный сайт регистрация играть онлайн
Главная страница сайта casino является центром информации о букмекерской конторе 7к казино, где вы найдете подробное описание наших предложений и услуг – работающее зеркало страницы 7k casino
tenormin 100mg oral – order carvedilol 6.25mg generic buy carvedilol 25mg without prescription
Hello everyone !
Navigate through our intuitive platform with ease and find your favorite content quickly. Stream on your TV, laptop, tablet, or smartphone – anytime, anywhere. Gain access to exclusive shows and films that you won’t find anywhere else. Our advanced algorithms suggest content based on your viewing preferences, making it easy to discover new favorites. Keep track of what you want to watch next and easily revisit your favorite content. http://limelight-stream.com Stay up-to-date with live events, sports, and concerts, streamed directly to your device. Download your favorite shows and movies to watch offline, perfect for when you’re on the go.
Game streaming community support
Game streaming security tips
Game streaming software comparison
Limelight troubleshooting
Game streaming with controller support
Good luck!
nazilli pidesi nazilli meşhur pidesi
Всем привет! Может кто знает, где почитать полезные статьи о недвижимости? Пока нашел https://komdizrem.ru
Приветствую. Подскажите, где найти полезные блоги о недвижимости? Пока нашел https://konditsioneri-shop.ru
Здравствуйте!
Заказать документ университета вы сможете в нашей компании.
asxdiplomik24.ru/otzyvy
Хорошей учебы!
Здравствуйте!
Купить документ о получении высшего образования можно у нас в Москве.
diplomasx.com/kupit-diplom-magistra
Новости Бреста а также Брестской области также сфере, исключительно оперативная информация: объекта дня, обзоры, последние неприятного события а также действия мегаполисам, извещенья что касается АВАРИЯ
https://elnet.by/
atorlip tablets – order bystolic online cheap buy bystolic online
Приветствую. Может кто знает, где найти полезные блоги о недвижимости? Сейчас читаю https://glatt-nsk.ru
Добрый день!
Мы предлагаем дипломы любой профессии по приятным ценам. Стоимость будет зависеть от конкретной специальности, года получения и образовательного учреждения.
arusak-diploms-srednee.ru
Хорошей учебы!
Привет, друзья!
Диплом техникума купить официально с упрощенным обучением в Москве
alternativaprofi.com/forum/index.php
Всегда вам поможем!.
Триколорный рынок последних автомобилей показывает разнонаправленную динамику цен. Одни модели значительно упали в цене, в течение то ятси яко часть, наоборот
https://avgrodno.by/
Новинки Гор и Могилева, самая актуальная экспресс-информация: предмета дня, обзоры, крайние действия города. https://roogorki.by/
аттестат 2000 года ast-diploms.com .
купить диплом в уфе купить диплом в уфе .
интернет магазин стройматериалов интернет магазин стройматериалов .
lasix on line
Pedro Gonzalez Lopez https://barcelona.pedri-ar.com known as Pedri, was born on November 25, 2002 in the small town of Tegeste, located on Tenerife, one of the Canary Islands.
The story of Leo Messi https://inter-miami.lionelmessi.ae‘s transfer to Inter Miami began long before the official announcement. Rumors about Messi’s possible departure from Barcelona appeared in 2020
Yacine Bounou https://al-hilal.yassine-bounou-ar.com known simply as Bono, is one of the most prominent Moroccan footballers of our time.
Andreson Souza Conceicao https://al-nassr.talisca-ar.com known as Talisca, is one of the brightest stars of modern football.
Здравствуйте!
Мы предлагаем документы техникумов, которые находятся на территории всей России. Вы сможете купить качественно сделанный диплом за любой год, указав необходимую специальность и оценки за все дисциплины. Документы выпускаются на “правильной” бумаге самого высшего качества. Это дает возможность делать настоящие дипломы, которые не отличить от оригинала. Они заверяются всеми обязательными печатями и штампами.
internux.co.id/tag/masa-subur
Здравствуйте!
Приобрести документ университета можно у нас в столице.
ast-diplomas24.ru/kupit-diplom-krasnoyarsk
Удачи!
купить диплом косметолога государственного образца http://www.diploms-x.com/ .
Здравствуйте!
Купить диплом университета.
http://www.guyub.net/read-blog/8690
Добрый день!
Диплом вуза купить официально с упрощенным обучением в Москве
1abakan.ru/forum/showthread-185970/
Всегда вам поможем!.
[u][b] Привет![/b][/u]
[b]Заказать диплом любого университета.[/b]
[url=http://rst.adk.audio/company/personal/user/1577/forum/message/1706/1703/#message1703/]rst.adk.audio/company/personal/user/1577/forum/message/1706/1703/#message1703[/url]
[b]Удачи![/b]
Harry Kane https://bayern.harry-kane-ar.com one of the most prominent English footballers of his generation, completed his move to German football club Bayern Munich in 2023.
Brazilian footballer Neymar https://al-hilal.neymar-ar.com known for his unique playing style and outstanding achievements in world football, has made a surprise move to Al Hilal Football Club.
azithromycin z-pack
Erling Haaland https://manchester-city.erling-haaland-ar.com born on July 21, 2000 in Leeds, England, began his football journey at an early age.
Luka Modric https://real-madrid.lukamodric-ar.com can certainly be called one of the outstanding midfielders in modern football.
Football in Saudi Arabia https://al-hilal.ali-al-bulaihi-ar.com has long been one of the main sports, attracting millions of fans. In recent years, one of the brightest stars in Saudi football has been Ali Al-Bulaihi, defender of Al-Hilal Football Club.
visit my website https://currencyconvert.net
Сайт https://ps-likers.ru предлагает уроки по фотошоп для начинающих. На страницах сайта можно найти пошаговые руководства по анимации, созданию графики для сайтов, дизайну, работе с текстом и фотографиями, а также различные эффекты.
Здравствуйте!
Диплом ВУЗа купить официально с упрощенным обучением в Москве
datasphere.ru/club/user/15/blog
Рады помочь!.
RDBox.de https://rdbox.de bietet schallgedammte Gehause fur 3D-Drucker, die eine sehr leise Druckumgebung schaffen – nicht lauter als ein Kuhlschrank. Unsere Losungen sorgen fur stabile Drucktemperatur, Vibrationsisolierung, Luftreinigung und mobile App-Steuerung.
N’Golo Kante https://al-ittihad.ngolokante-ar.com the French midfielder whose career has embodied perseverance, hard work and skill, has continued his path to success at Al-Ittihad Football Club, based in Saudi Arabia.
Kobe Bryant https://los-angeles-lakers.kobebryant-ar.com also known as the “Black Mamba”, is one of the most iconic and iconic figures in NBA history.
Привет, друзья!
Приобрести документ о получении высшего образования можно у нас.
ast-diplomas.com/kupit-diplom-magistra
Привет!
Предлагаем документы ВУЗов, расположенных на территории всей Российской Федерации. Можно купить качественный диплом за любой год, включая сюда документы старого образца. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать государственные дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и подписями.
Мы можем предложить дипломы любой профессии по невысоким тарифам. Цена может зависеть от выбранной специальности, года выпуска и университета. Всегда стараемся поддерживать для заказчиков адекватную политику тарифов. Важно, чтобы дипломы были доступны для большого количества наших граждан.
landik-diploms-srednee.ru/kupit-diplom-volgograd
Успехов в учебе!
Привет!
Купить документ о получении высшего образования можно у нас в Москве.
ast-diplom24.ru/otzyvy
Успешной учебы!
Karim Benzema https://al-ittihad.karimbenzema.ae is a name worthy of admiration and respect in the world of football.
Cristiano Ronaldo https://al-nassr.cristiano-ronaldo.ae is one of the greatest names in football history, with his achievements inspiring millions of fans around the world.
In 2018, the basketball world witnessed one of the most remarkable transformations in NBA history. LeBron James https://los-angeles-lakers.lebronjames-ar.com one of the greatest players of our time, decided to leave his hometown Cleveland Cavaliers and join the Los Angeles Lakers.
Luis Diaz https://liverpool.luis-diaz-ar.com is a young Colombian striker who has enjoyed rapid growth since joining the ” Liverpool” in January 2022.
프라그마틱 슬롯
시험에 대처하기 위해 Fang Jifan은 밤새 바빴습니다.
Привет, друзья!
Где заказать диплом специалиста?
Приобрести диплом о высшем образовании.
belconsole.ru/club/user/11870/blog/2131/
Maria Sharapova https://tennis.maria-sharapova-ar.com was born on April 19, 1987 in Nyagan, Russia. When Masha was 7 years old, her family moved to Florida, where she started playing tennis.
Kevin De Bruyne https://manchester-city.kevin-de-bruyne-ar.com is a name every football fan knows today.
Muhammad Al Owais https://al-hilal.mohammed-alowais-ar.com is one of the most prominent names in modern Saudi football. His path to success in Al Hilal team became an example for many young athletes.
Roberto Firmino https://al-ahli.roberto-firmino-ar.com one of the most talented and famous Brazilian footballers of our time, has paved his way to success in different leagues and teams.
Привет, друзья!
Как избежать рисков при покупке диплома колледжа или ВУЗа в России
akademe.mn.co/posts/62005359
Рады помочь!.
Незаконные действия и взломы могут оказать влияние на игровые аппараты онлайн – Riobet рабочее зеркало сайта
Привет!
Мы изготавливаем дипломы любой профессии по доступным тарифам.
montrealpal.com/read-blog/815_kak-najti-nadezhnyj-magazin-prodayushij-diplomy.html
Казино 7k casino предоставляет возможность установки лимитов на депозиты рабочий сайт р7 казино
На главной странице сайта casino размещена ссылка на 7к казино, где можно ознакомиться с подробной информацией – рабочее зеркало страницы
Казино 7k casino обеспечивает мою конфиденциальность и безопасность – сайт 7k casino
видеостена купить в москве видеостена купить в москве .
Angel Di Maria https://benfica.angel-di-maria-ar.com is a name that will forever remain in the memories of Benfica fans.
Khvicha Kvaratskhelia https://napoli.khvicha-kvaratskhelia-ar.com is a name that in recent years has become a symbol of Georgian football talent and ambition.
Football in Saudi Arabia https://al-hilal.saud-abdulhamid-ar.com is gaining more and more popularity and recognition on the international stage, and Saud Abdul Hamid, the young and talented defender of Al Hilal, is a shining example of this success.
cheap generic gasex – gasex brand buy diabecon tablets
cost gasex – ashwagandha cost diabecon brand
Казахский национальный технический университет https://satbayev.university им. К.Сатпаева
Upcoming fantasy MOBA https://bladesofthevoid.com evolved by Web3. Gacha perks, AI and crafting in one swirling solution!
Продажа новых автомобилей Hongqi
https://hongqi-krasnoyarsk.ru/hongqi-hs5 в Красноярске у официального дилера Хончи. Весь модельный ряд, все комплектации, выгодные цены, кредит, лизинг, трейд-ин
Kylie Jenner https://kylie-cosmetics.kylie-jenner-ar.com is an American model, media personality, and businesswoman, born on August 10, 1997 in Los Angeles, California.
cheap atorlip – nebivolol us buy generic bystolic 20mg
accutane online pharmacy india
Привет!
Где купить диплом специалиста?
Приобрести диплом ВУЗа.
s24.team/club/user/148/blog/1602/
Здравствуйте!
Готовы предложить документы техникумов, которые расположены на территории всей Российской Федерации. Вы имеете возможность заказать качественный диплом за любой год, включая сюда документы СССР. Дипломы и аттестаты делаются на бумаге высшего качества. Это позволяет делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и подписями.
Мы предлагаем дипломы любых профессий по разумным тарифам. Цена будет зависеть от той или иной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для клиентов адекватную политику тарифов. Важно, чтобы документы были доступными для большинства граждан.
arusak-diploms-srednee.ru/kupit-diplom-magistra В
Успешной учебы!
Привет, друзья!
Заказать документ о получении высшего образования вы имеете возможность в нашей компании в столице.
diplomyx.com/kupit-diplom-ekaterinbur
Хорошей учебы!
Добрый день!
Мы можем предложить документы техникумов, которые расположены в любом регионе РФ. Можно приобрести качественный диплом от любого заведения, за любой год, включая документы старого образца СССР. Дипломы и аттестаты выпускаются на бумаге самого высшего качества. Это дает возможности делать настоящие дипломы, не отличимые от оригиналов. Они заверяются необходимыми печатями и подписями.
erkibbutz.com/read-blog/493
Привет!
Покупка диплома о среднем полном образовании: как избежать мошенничества?
mosmol.flybb.ru/viewtopic.php?f=2&t=391
Поможем вам всегда!.
Kudos! I appreciate it!|
Пошаговая инструкция по официальной покупке диплома о высшем образовании
diploms-x24.ru/kupit-diplom-vracha
modafinil 10 mg
Bella Hadid https://img-models.bella-hadid-ar.com is an American model who has emerged in recent years as one of the most influential figures in the world of fashion.
Sadio Mane https://al-nassr.sadio-mane-ar.com the Senegalese footballer best known for his performances at clubs such as Southampton and Liverpool, has become a prominent figure in Al Nassr.
Brazilian footballer Ricardo Escarson https://orlando-city.kaka-ar.com dos Santos Leite, better known as Kaka, is one of the most famous and successful players in football history.
Zinedine Zidane https://real-madrid.zinedine-zidane-ar.com the legendary French footballer, entered the annals of football history as a player and coach.
order lasuna online cheap – purchase lasuna generic how to buy himcolin
tamoxifen 100 mg
купить аттестат об среднем образовании купить аттестат об среднем образовании .
Edson Arantes https://santos.pele-ar.com do Nascimento, known as Pele, was born on October 23, 1940 in Tres Coracoes, Minas Gerais, Brazil.
Brazilian footballer Malcom https://al-hilal.malcom-ar.com (full name Malcom Felipe Silva de Oliveira) achieved great success in Al Hilal, one of the leading football teams in Saudi Arabia and the entire Middle East.
Monica Bellucci https://dracula.monica-bellucci-ar.com one of the most famous Italian actresses of our time, has a distinguished artistic career spanning many decades. Her talent, charisma, and stunning beauty made her an icon of world cinema.
Добрый день!
Купить документ о получении высшего образования можно в нашей компании.
diplomyx.com/kupit-diplom-ekaterinbur
Успехов в учебе!
фоновое озвучивание фоновое озвучивание .
Добрый день!
Заказать диплом о высшем образовании
landik-diploms-srednee.ru/kupit-diplom-saratov В
Успехов в учебе!
Добрый день!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
forum-nine.mirbb.com/t11755-topic#31165
Рады помочь!.
Привет!
Как не стать жертвой мошенников при покупке диплома о среднем полном образовании
b98415ql.bget.ru/index.php?subaction=userinfo&user=yfaquvy
Всегда вам поможем!.
Jackie Chan https://karate-kid.jackiechan-ar.com was born in 1954 in Hong Kong under the name Chan Kong San.
Привет!
Купить документ ВУЗа можно у нас в Москве.
ast-diplomy24.ru/kupit-diplom-ekaterinbur
магазин ключей и аккаунтов магазин ключей и аккаунтов .
Привет!
Приобрести документ университета можно в нашем сервисе.
ast-diplomy.com/kupit-diplom-vracha
Успешной учебы!
Привет!
Наша компания предлагает заказать диплом отличного качества, неотличимый от оригинального документа без использования специального оборудования и опытного специалиста.
payhotel.ru/forum/messages/forum2/topic7566/message7896/?result=reply#message7896
Хорошей учебы!
Здравствуйте!
Где приобрести диплом по необходимой специальности?
Мы готовы предложить документы ВУЗов, которые расположены в любом регионе РФ. Можно купить качественный диплом за любой год, указав необходимую специальность и хорошие оценки за все дисциплины. Дипломы выпускаются на бумаге высшего качества. Это позволяет делать государственные дипломы, не отличимые от оригинала. Они будут заверены необходимыми печатями и штампами.
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по доступным ценам.
diploms-x24.ru/kupit-diplom-nizhnij-novgorod
Будем рады вам помочь!
Добрый день!
Сколько стоит диплом высшего и среднего образования и как это происходит?
1001viktorina.ru/forum/viewtopic.php?f=19&t=1348&sid=1d8b03c8c2452ae1448ccb7f1b5d04a8
Рады помочь!.
[u][b] Здравствуйте![/b][/u]
Где приобрести диплом по нужной специальности?
[url=http://windows1.listbb.ru/viewtopic.php?f=3&t=460/]windows1.listbb.ru/viewtopic.php?f=3&t=460[/url]
[b]Успешной учебы![/b]
[u][b] Привет![/b][/u]
Купить документ о получении высшего образования можно в нашей компании в Москве. Мы предлагаем документы об окончании любых университетов России. Вы сможете получить диплом по любым специальностям, включая документы СССР.
[url=http://mymotospeed.ru/professionalnyie-diplomyi-po-otlichnoy-tsene/]mymotospeed.ru/professionalnyie-diplomyi-po-otlichnoy-tsene[/url]
[url=http://justvoip.listbb.ru/viewtopic.php?f=2&t=457/]justvoip.listbb.ru/viewtopic.php?f=2&t=457[/url]
[url=http://beijingpal.com/read-blog/940/]beijingpal.com/read-blog/940[/url]
[url=http://cocapal.com/read-blog/1009/]cocapal.com/read-blog/1009[/url]
[url=http://driveme.rusff.me/viewtopic.php?id=2177#p105233/]driveme.rusff.me/viewtopic.php?id=2177#p105233[/url]
[u][b] Привет, друзья![/b][/u]
[b]Купить документ[/b] о получении высшего образования вы сможете в нашей компании в столице.
[url=http://diploms-x24.ru/kupit-diplom-voronezh/]diploms-x24.ru/kupit-diplom-voronezh[/url]
Здравствуйте!
Приобретение диплома ПТУ с сокращенной программой обучения в Москве
arusak-diploms-srednee.ru/kupit-diplom-v-cheliabinske
Привет, друзья!
Можно ли купить аттестат о среднем образовании? Основные рекомендации
dp.getbb.ru/viewtopic.php?f=3&t=735
Будем рады вам помочь!
can you buy cheap clomid without insurance “>where to buy cheap clomid prices
http://www.google.tt/url?q=https://clomiddelivery.pro cheap clomid pills
[url=https://www.google.com.mt/url?sa=t&url=https://clomiddelivery.pro]can i get clomid online[/url] buying clomid without prescription
Travis Scott https://astroworld.travis-scott-ar.com is one of the brightest stars in the modern hip-hop industry.
The history of one of France’s https://france.paris-saint-germain-ar.com most famous football clubs, Paris Saint-Germain, began in 1970, when capitalist businessmen Henri Delaunay and Jean-Auguste Delbave founded the club in the Paris Saint-Germain-en-Laye area.
Juventus Football Club https://italy.juventus-ar.com is one of the most successful and decorated clubs in the history of Italian and world football.
Chelsea https://england.chelsea-ar.com is one of the most successful English football clubs of our time.
лучшее порно бесплатно лучшее порно бесплатно .
Приветствую. Подскажите, где найти полезные блоги о недвижимости? Сейчас читаю https://glatt-nsk.ru
buy lasuna cheap – buy generic lasuna online order himcolin online
Автомобили Hongqi https://hongqi-krasnoyarsk.ru в наличии – официальный дилер Hongqi Красноярск
Liverpool https://england.liverpool-ar.com holds a special place in the history of football in England.
When Taylor Swift https://shake-it-off.taylor-swift-ar.com released “Shake It Off” in 2014, she had no idea how much the song would impact her life and music career.
Priyanka Chopra https://baywatch.priyankachopra-ar.com is an Indian actress, singer, film producer and model who has achieved global success.
Здравствуйте!
Приобрести документ института можно в нашем сервисе.
ast-diplom24.ru/kupit-diplom-vracha
Привет, друзья!
Заказать документ о получении высшего образования можно у нас в Москве.
ast-diploms24.ru/kupit-diplom-voronezh
Удачи!
Jennifer Lopez https://lets-get-loud.jenniferlopez-ar.com was born in 1969 in the Bronx, New York, to parents who were Puerto Rican immigrants.
Привет, друзья!
Как приобрести диплом о высшем образовании в Москве и других городах
landik-diploms-srednee.ru/kupit-diplom-v-novosibirske
Привет, друзья!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
wecanchat.mn.co/posts/62049695
Рады помочь!
After some difficult years in the late 2010s, Manchester United https://england.manchester-united-ar.com returned to greatness in English football by 2024.
The Formula One World Championship https://world-circuit-racing-championship.formula-1-ar.com, known as the Formula Championship in motor racing, is the highest tier of professional motor racing.
Michael Jordan https://chicago-bulls.michael-jordan-ar.com is one of the greatest basketball players of all time, whose career with the Chicago Bulls is legendary.
балкон дизайн интерьера дизайн проект интерьера
дипломы детские купить ast-diploms.com .
Добрый день!
Купить диплом любого ВУЗа.
russianecuador.com/forum/member.php?u=13207
Успешной учебы!
лучшее порно порево http://besplatny-sex-online.ru .
car rental Montenegro Podgorica airport https://montenegro-car-rental-hire.com
The golf https://arabic.golfclub-ar.com industry in the Arab world is growing rapidly, attracting players from all over the world.
Mike Tyson https://american-boxer.mike-tyson-ar.com one of the most famous and influential boxers in history, was born on June 30, 1966 in Brooklyn, New York.
Manny Pacquiao https://filipino-boxer.manny-pacquiao-ar.com is one of the most prominent boxers in the history of the sport.
Muhammad Ali https://american-boxer.muhammad-ali-ar.com is perhaps one of the most famous and greatest athletes in the history of boxing.
Здравствуйте!
Мы предлагаем дипломы любой профессии по невысоким тарифам.
jrsjewellers.com/2024/06/29/купить-дипломы-университета/
Greetings I am so thrilled I found your website, I really found you
by accident, while I was searching on Askjeeve for something else, Regardless I
am here now and would just like to say thank you for a
remarkable post and a all round enjoyable blog (I also love the theme/design), I don’t have time to look over it all at the minute but I have
saved it and also added in your RSS feeds, so when I have time I will be back to read more, Please do keep up the superb job.
Привет!
Приобрести документ института вы сможете в нашей компании в Москве.
ast-diploms.com/kupit-diplom-kazan
Добрый день!
Приобрести документ о получении высшего образования можно в нашем сервисе.
ast-diplom24.ru/kupit-diplom-nizhnij-novgorod
Успехов в учебе!
Добрый день!
Как приобрести диплом техникума с минимальными рисками
asktourist.ru/viewtopic.php?id=5572#p20173
Рады оказаться полезными!
The road to the Premier League https://english-championship.premier-league-ar.com begins long before a team gets promoted to the English Premier League for the first time
In recent years, the leading positions in the Spanish https://spanish-championship.laliga-ar.com championship have been firmly occupied by two major giants – Barcelona and Real Madrid.
The Italian football championship https://italian-championship.serie-a-ar.com known as Serie A, has seen an impressive revival in recent years.
In the German football https://german-championship.bundesliga-football-ar.com championship known as the Bundesliga, rivalries between clubs have always been intense.
https://euroavia24.com – Cheap flights, hotels and transfers around the world!
The Saudi Football League https://saudi-arabian-championship.saudi-pro-league-ar.com known as the Saudi Professional League, is one of the most competitive and dynamic leagues in the world.
Rodrigo Goes https://real-madrid.rodrygo-ar.com better known as Rodrigo, is one of the brightest young talents in modern football.
In an era when many young footballers struggle to find their place at elite clubs, Javi’s https://barcelona.gavi-ar.com story at Barcelona stands out as an exceptional one.
Arsenal https://arsenal.mesut-ozil-ar.com made a high-profile signing in 2013, signing star midfielder Mesut Ozil from Real Madrid.
Привет!
Мы можем предложить дипломы психологов, юристов, экономистов и любых других профессий по невысоким тарифам. Цена зависит от выбранной специальности, года получения и ВУЗа. Всегда стараемся поддерживать для заказчиков адекватную ценовую политику. Важно, чтобы документы были доступными для большинства граждан.
seolistlinks.com/story18346104/купить-диплом-техникума
purchase speman online – buy himplasia tablets finasteride online buy
самое классное порево klassny-sex.ru .
классное порево онлайн классное порево онлайн .
Привет!
Купить диплом о высшем образовании.
islider.ru/read-blog/768
Luis Suarez https://inter-miami.luis-suarez-ar.com the famous Uruguayan footballer, ended his brilliant career in European clubs and decided to try his hand at a new challenge – Major League Soccer.
Thibaut Courtois https://real-madrid.thibaut-courtois-ar.com was born on May 11, 1992 in Belgium.
Bayern Munich’s https://bayern.jamal-musiala-ar.com young midfielder, Jamal Musiala, has become one of the brightest talents in European football.
гидравлический грузовой подъемник подъемник грузовой канатный
грузовой подъемник пмг https://podemniki-gruzovye.ru
Привет, друзья!
Узнайте, как безопасно купить диплом о высшем образовании
newsbizlife.ru/kupit-diplom-vyisokoe-kachestvo-i-nadezhnost
Ridiculous quest there. What occurred after? Good luck!
Здравствуйте!
Как получить диплом техникума с упрощенным обучением в Москве официально
wisdomtarot.tforums.org/viewtopic.php?f=8&t=6154
Рады оказаться полезными!.
Добрый день!
Заказать документ ВУЗа можно в нашей компании.
ast-diplomy.com/kupit-diplom-voronezh
Успехов в учебе!
슬롯 꽁 머니 사이트
Fang Jifan은 눈을 비비고 신발을 걷어차며 “뭐?”
buy noroxin pills – how to buy noroxin cheap confido for sale
Добрый день!
Приобрести диплом университета.
xn--80aeahbdc6cr3b7h.xn--p1ai/club/user/8729/blog/193084/
purchase norfloxacin pill – buy norfloxacin without prescription confido price
Al-Nasr https://saudi.al-nassr-ar.com is one of the most famous football teams in the Kingdom of Saudi Arabia.
Al-Nasr Club https://saudi.al-hilal-ar.com from Riyadh has a rich history of success, but its growth has been particularly impressive in recent years.
Al-Ittihad https://saudi.al-ittihad-ar.com is one of the most famous football clubs in Saudi Arabia. Founded in 1927, the Saudi football giant has come a long way to the pinnacle of success.
Hello, i think that i saw you visited my blog thus i came to “return the favor”.I’m attempting to
find things to improve my website!I suppose its ok to use some of your ideas!!
Привет!
Как безопасно купить диплом колледжа или ВУЗа в России, что важно знать
japapmessenger.com/read-blog/522
Окажем помощь!
FC Barcelona https://spain.fc-barcelona-ar.com is undoubtedly one of the most famous and well-known football clubs in the world.
порно видео бесплатно порно видео бесплатно .
Привет, друзья!
Приобрести документ о получении высшего образования можно в нашей компании в столице.
asxdiplomik24.ru/kupit-diplom-tehnikuma-kolledzha
порно коллекции бесплатно porn-library.ru .
Привет, друзья!
Мы можем предложить документы ВУЗов, которые расположены на территории всей РФ. Вы сможете приобрести качественно напечатанный диплом за любой год, в том числе документы старого образца. Документы выпускаются на “правильной” бумаге самого высокого качества. Это позволяет делать настоящие дипломы, которые невозможно отличить от оригинала. Документы заверяются всеми необходимыми печатями и штампами.
create-lifestyle.mn.co/posts/61837999
куплю диплом услуга diploms-x.com .
Приветствую. Подскажите, где найти разные блоги о недвижимости? Пока нашел https://gor-bur.ru
Всем привет! Может кто знает, где найти полезные блоги о недвижимости? Сейчас читаю https://konditsioneri-shop.ru
luxury yacht charter Montenegro rent a yacht Montenegro
sailing Montenegro Montenegro rent boat
Real Madrid’s https://spain.real-madrid-ar.com history goes back more than a century. The club was founded in 1902 by a group of football enthusiasts led by Juan Padilla
FC Bayern Munich (Munich) https://germany.bayern-munchen-ar.com is one of the most famous and recognized football clubs in Germany and Europe
Arsenal https://england.arsenal-ar.com is one of the most famous and successful football clubs in the history of English football.
Добрый день!
Заказать документ о получении высшего образования вы имеете возможность в нашем сервисе.
diplomyx.com/kupit-diplom-moskva
Успехов в учебе!
Привет!
Купить диплом любого ВУЗа.
mastergrad.getbb.ru/viewtopic.php?f=12&t=1872
Успешной учебы!
[u][b] Добрый день![/b][/u]
[b]Заказать диплом любого университета.[/b]
[url=http://belconsole.ru/club/user/11870/blog/2131//]belconsole.ru/club/user/11870/blog/2131/[/url]
Thai Company Directory https://thaicorporates.com List of companies and business information.
пакет бумажный с логотипом цена печать буклетов
Ремонт плоской кровли https://remontiruem-krovly.ru в Москве, цена работы за 1 м?. Прайс лист на работы под ключ, отзывы и фото.
AC Milan https://italy.milan-ar.com is one of the most successful and decorated football clubs in the world.
Как оказалось, купить диплом кандидата наук не так уж и сложно
ast-diplomy24.ru/kupit-diplom-o-srednem-obrazovanii
In the world of football, Atletico Madrid https://spain.atletico-madrid-ar.com has long been considered the second most important club in Spain after the dominant, Real Madrid.
Galatasaray https://turkey.galatasaray-ar.com is one of the most famous football clubs in Turkiye, with a glorious and eventful history.
The future football star Shabab Al-Ahly https://dubai.shabab-al-ahli-ar.com was born in Dubai in 2000. From a young age, he showed exceptional football abilities and joined the youth academy of one of the UAE’s leading clubs, Shabab Al-Ahly.
The fascinating story of Ja Morant’s https://spain.atletico-madrid-ar.com meteoric rise, from status from rookie to leader of the Memphis Grizzlies and rising NBA superstar.
Привет, друзья!
Мы готовы предложить дипломы любой профессии по разумным ценам.
dailygram.com/blog/1300025/купите-дипломы-быстро-и-надежно/
It’s awesome to pay a visit this site and reading the views of all friends
regarding this article, while I am also keen of getting experience.
Привет, друзья!
Полезные советы по безопасной покупке диплома о высшем образовании
arusak-diploms-srednee.ru В
Discover your perfect stay with WorldHotels-in.com, your ultimate destination for finding the best hotels worldwide! Our user-friendly platform offers a vast selection of accommodations to suit every traveler’s needs and budget. Whether you’re planning a luxurious getaway or a budget-friendly adventure, we’ve got you covered with our extensive database of hotels across the globe. Our intuitive search features allow you to filter results based on location, amenities, price range, and guest ratings, ensuring you find the ideal match for your trip. We pride ourselves on providing up-to-date information and competitive prices, often beating other booking sites. Our detailed hotel descriptions, high-quality photos, and authentic guest reviews give you a comprehensive view of each property before you book. Plus, our secure booking system and excellent customer support team ensure a smooth and worry-free experience from start to finish. Don’t waste time jumping between multiple websites – http://www.WorldHotels-in.com brings the world’s best hotels to your fingertips in one convenient place. Start planning your next unforgettable journey today and experience the difference with WorldHotels-in.com!
https://indibeti.in is a premier online casino offering a wide array of games including slots, table games, and live dealer options. Renowned for its user-friendly interface and robust security measures, Indibet ensures a top-notch gaming experience with exciting bonuses and 24/7 customer support.
купить новостройку от застройщика https://kvartira-new43.ru
купить квартиру купить новостройку от застройщика
купить новостройку цены застройщика недвижимость новостройки купить
오래된 토토 사이트
짧은 시간에 30마리 이상의 소가 시산 근처에서 설명할 수 없이 죽었습니다.
Привет, друзья!
Полезная информация как купить диплом о высшем образовании без рисков
http://www.techhackly.xyz/2024/06/30/купить-дипломы-университета/
Добрый день!
Заказать документ университета можно у нас в столице.
ast-diploms.com/kupit-diplom-krasnodar
Добрый день!
Приобрести документ ВУЗа можно в нашей компании.
ast-diplom.com/kupit-diplom-vracha
Успехов в учебе!
nazilli apart otel
coindarwin price analysis
The Unseen Story Behind Solana’s Founder Toly Yakovenko’s Achievement
Post Two Cups of Coffees and Beer
Yakovenko, the innovator behind Solana, initiated his path with an ordinary ritual – two coffees and a brew. Unaware to him, those moments would ignite the machinery of his future. At present, Solana remains as an influential contender in the cryptocurrency world, featuring a market value of billions.
Ethereum ETF Debut
The recently launched Ethereum ETF recently made its debut with a huge trading volume. This significant event experienced several spot Ethereum ETFs from several issuers commence trading in the U.S., injecting unseen activity into the typically steady ETF trading space.
SEC’s Approval of Ethereum ETF
The Commission has sanctioned the spot Ethereum ETF to be listed. Being a cryptographic asset featuring smart contracts, Ethereum is projected to significantly impact on the cryptocurrency industry due to this approval.
Trump’s Crypto Maneuver
With the upcoming election, Trump frames himself as the “Crypto President,” repeatedly showing his support for the crypto sector to attract voters. His method contrasts with Biden’s approach, seeking to capture the interest of the crypto community.
Elon Musk’s Crypto Moves
Elon Musk, a prominent figure in the blockchain world and a backer of Trump, caused a stir yet again, boosting a meme coin connected to his actions. His participation continues to shape the market landscape.
Binance Updates
Binance’s unit, BAM, has been permitted to channel customer funds in U.S. Treasury securities. Additionally, Binance noted its 7th anniversary, highlighting its journey and acquiring several compliance licenses. At the same time, Binance also announced plans to remove several significant crypto trading pairs, influencing multiple market entities.
AI’s Impact on the Economy
A top stock analyst from Goldman Sachs recently observed that artificial intelligence won’t trigger a revolution in the economy
can i buy ciprofloxacin over the counter usa
Привет, друзья!
Пошаговая инструкция по официальной покупке диплома о высшем образовании
gorod.kr.ua/forum/showthread.php?p=267249#post267249
Всегда вам поможем!.
купить квартиру https://kvartirukupit43.ru
купить квартиру недорого https://newkvartiry-spb.ru
купить новостройку с отделкой https://novye-kvartiryspb.ru
недорогие квартиры от застройщика https://novye-kvartiry-spb.ru
недорогие квартиры от застройщика https://novyekvartiry2.ru
конференционный зал oborudovanie-dlja-konferenc-zalov.ru .
Привет, друзья!
Мы изготавливаем дипломы любой профессии по приятным тарифам.
rajotravel.com/2024/06/30/купить-диплом-школы/
The Narrative Concerning Solana’s Creator Toly’s Success
Subsequent to 2 Servings of Coffee and a Brew
Yakovenko, the innovator behind Solana, started his quest with a modest practice – two coffees and a brew. Unaware to him, these occasions would ignite the gears of his future. Today, Solana is as a significant player in the cryptocurrency realm, with a market value of billions.
Ethereum ETF First Sales
The new Ethereum ETF newly made its debut with a staggering trading volume. This significant event witnessed multiple spot Ethereum ETFs from various issuers begin trading on U.S. exchanges, bringing unseen activity into the typically steady ETF trading space.
SEC’s Approval of Ethereum ETF
The Securities and Exchange Commission has formally approved the Ethereum ETF to be listed. Being a cryptographic asset with smart contracts, Ethereum is projected to majorly affect the blockchain sector due to this approval.
Trump’s Crypto Maneuver
As the election draws near, Trump frames himself as the ‘Crypto President,’ constantly highlighting his backing of the blockchain space to garner votes. His approach contrasts with Biden’s approach, seeking to capture the support of the crypto community.
Musk’s Influence on Crypto
Musk, a prominent figure in the crypto community and an advocate of the Trump camp, stirred things up once more, promoting a meme coin related to his antics. His participation continues to shape the market landscape.
Binance’s Latest Moves
Binance’s unit, BAM, is now permitted to use customer funds in U.S. Treasury securities. Additionally, Binance marked its 7th anniversary, showcasing its path and obtaining numerous regulatory approvals. Simultaneously, the company also disclosed plans to remove several important cryptocurrency pairs, influencing multiple market entities.
AI and Market Trends
Goldman Sachs’ top stock analyst recently commented that artificial intelligence won’t lead to an economic revolution
рейтинг прогнозистов http://www.rejting-kapperov12.ru .
купить квартиру купить 1 квартиру застройщика
купить квартиру в новостройке цены купить двухкомнатную квартиру в новостройке
купить 1 комнатную квартиру в новостройке https://kvartiranovostroi.ru
купить двухкомнатную в новостройке https://kvartira-novostroi.ru
купить квартиру от застройщика https://kvartiranovostroi2.ru
Привет!
Приобрести документ ВУЗа можно у нас в столице.
ast-diplom24.ru/kupit-diplom-ekaterinbur
Удачи!
купить 1 квартиру застройщика https://kvartira-novostroyka2.ru
Помощь в решении задач https://zadachireshaem-online.ru. Опытные авторы с профессиональной подготовкой окажут консультацию в решении задач на заказ недорого, быстро, качественно
Заказать контрольную работу https://kontrolnye-reshim.ru, недорого, цены. Решение контрольных работ на заказ срочно.
Заказать курсовую работу https://kursovye-napishem.ru в Москве: цены на написание и выполнение, недорого
Заказать дипломную работу https://diplomzakazat-oline.ru недорого. Дипломные работы на заказ с гарантией.
Accessibility Team Meeting Notes https://make.wordpress.org/accessibility/2021/06/11/accessibility-team-meeting-notes-june-11-2021
Красивая музыка https://melodia.space для души слушать онлайн.
ciprofloxacin 500 mg capsules
Здравствуйте!
Приобрести диплом университета.
anamaliya.ru/otzyvy/shirokiy-assortiment-dokumentov-v-populyarnom-onlayn-magazine
Помощь студентам в выполнении рефератов https://referatkupit-oline.ru. Низкие цены и быстрое написание рефератов!
комплексное поисковое продвижение сайта раскрутка сайта казань
стоимость раскрутки сайта заказать seo продвижение сайта
конференц зал оборудование https://oborudovanie-konferenc-zalov.ru .
конференционный зал oborudovanie-konferenc-zalov.ru .
Здравствуйте!
Заказать диплом о высшем образовании.
ya3bbru.bbok.ru/viewtopic.php?id=4030#p7081
Привет, друзья!
Заказать документ о получении высшего образования можно в нашей компании.
diploms-x.com/kupit-diplom-o-vysshem-obrazovanii
переговорные комнаты под ключ переговорные комнаты под ключ .
переговорные комнаты в москве переговорные комнаты в москве .
슬롯 킹
Zhu Houzhao는 “예, 손자도 Zhu Houzhao입니다. “라고 말했습니다.
Привет, друзья!
Купить документ университета можно у нас в столице.
diplomyx24.ru/kupit-diplom-omsk
Хорошей учебы!
ceo продвижение seo раскрутка сайта
заказать продвижение корпоративного сайта https://seo-optimizatsia.ru
Новинний ресурс https://actualnews.kyiv.ua про всі важливі події в Україні та світі.
Останні новини України https://gromrady.org.ua сьогодні онлайн – головні події світу
Новини сьогодні https://gau.org.ua останні новини України та світу онлайн
Новини України https://kiev-online.com.ua останні події в Україні та світі сьогодні, новини України за минулий день онлайн
Популярные репортажи https://infotolium.com в больших фотографиях, новости, события в мире
Україна свіжі новини https://kiev-pravda.kiev.ua останні події на сьогодні
Свіжі новини України https://lenta.kyiv.ua останні новини з-за кордону, новини політики, економіки, спорту, культури.
Україна останні новини https://lentanews.kyiv.ua головні новини та останні події
Привет!
Купить диплом ВУЗа.
medbereg.ru/club/user/15/blog/4123/
Привет!
Мы изготавливаем дипломы психологов, юристов, экономистов и других профессий по разумным ценам.
wegug.in/blogs/752/ упите-?ипломы-Ѕыстро-и-Ќадежно
Головні новини https://mediashare.com.ua про регіон України. Будьте в курсі останніх новин
Новини та аналітика https://newsportal.kyiv.ua ситуація в Україні.
Головні новини https://pto-kyiv.com.ua України та світу
Новини, останні події https://prp.org.ua в Україні та світі, новини політики, бізнесу та економіки, законодавства
Новини України https://sensus.org.ua та світу сьогодні. Головні та останні новини дня
Wow, that’s what I was looking for, what
a stuff! present here at this web site, thanks admin of this web site.
Привет!
Где приобрести диплом специалиста?
messenger.wepluz.com/read-blog/11105
видеостена оборудование видеостена оборудование .
оборудование актового зала оборудование актового зала .
Корисні та цікаві статті https://sevsovet.com.ua про здоров’я, дозвілля, кар’єру.
Головні новини https://status.net.ua сьогодні, найсвіжіші та останні новини України онлайн
Останні новини https://thingshistory.com зовнішньої та внутрішньої політики в країні та світі.
Останні новини світу https://uamc.com.ua про Україну від порталу новин Ukraine Today
Добрый день!
Приобрести документ о получении высшего образования вы имеете возможность в нашей компании в Москве.
diplomyx.com/kupit-diplom-perm
акустическое оборудование для актового зала https://oborudovanija-dlja-aktovyh-zalov.ru/ .
Привет!
Заказать документ о получении высшего образования можно в нашем сервисе.
diplomasx24.ru/otzyvy
Успехов в учебе!
Hello players!!
Glory Casino is reliability and convenience. Simple registration, generous bonuses, and fast payouts. The working mirror is always available. I play and win with pleasure. I recommend it to all gambling enthusiasts!
Glory Casino is a place where you can win. I’ve been betting on sports and playing in the casino for several months. The bonuses are great, and withdrawals are fast and without delays. The official website and working mirror are always at hand. I recommend it!
Catch the site where everything is in the best shape! – Glory Casino
plinko Glory Casino
Glory Casino official website download for free
Glory Casino bookmaker
how to spend Glory Casino bonuses
Glory Casino android
Good profits!
Здравствуйте!
Приобрести документ института
ast-diplom.com/kupit-diplom-o-srednem-obrazovanii
Добрый день!
Мы предлагаем дипломы психологов, юристов, экономистов и любых других профессий по невысоким тарифам.
eicolumbaira.es/купить-диплом-онлайн/