Welcome to my second blog post about my annual heart transplant check-up. It takes two days to complete so I guess that warranted two separate posts. If you haven’t seen my last post which featured information about my heart biopsy and right heart cath, you can find that at Annual Heart Transplant Check-Up Pt. 1.
Today we are picking back up right after the chest X-ray following my biopsy and right heart cath. Next up is the clinic appointment.
Thursday, February 18, 2021
2:00pm
After the chest X-ray, I head to the Heart Institute located inside of the hospital for my clinic visit. The clinic is running ahead of schedule because they bring me back 40 minutes early. Today is actually the first time I am meeting this nurse practitioner since the one I had previously been working with had moved on to a new position.

During the visit, we discuss my medications, the results from my blood draw, and any concerns I may have. One that I brought up was genetic testing. This is something my husband and I have talked about getting for a while but hadn’t brought up with my medical team. Besides it being interesting to possibly find out more about what caused my peripartum cardiomyopathy, most importantly I am concerned about my children’s health. My children could be at risk if there was a genetic basis to my PPCM. This is information that I need to know. Luckily, she was on board and put in a referral.
In my previous post, I mentioned that I am always want to know what my creatinine value is from my bloodwork. My kidney function has slowly been decreasing since my transplant. Unfortunately, these values have not changed. I still have stage 4 chronic kidney disease. However, with a chronic illness, not getting worse is a victory. I’m grateful for stability. I’ll take stability.
2:30pm
Right after my clinic appointment, I have an echocardiogram. The American Heart Association has a great explanation about what happens during an echocardiogram. It is essentially an ultrasound of your heart. Ejection fraction (EF) is often a key-value in the other Heart Stories on this blog. An echocardiogram is where we get this value. I’m always anxious to find out the results of this test.
After this test is complete I’m finally free to go home for the day. I’m very tired and hungry at this point and spent the rest of the evening relaxing at home. I head to bed early because tomorrow will be another full day.
Friday, February 19, 2021
5:30am
I wake up earlier today because the check-in for my left heart cath is at 8 am. I’ve once again packed all of the items I brought for yesterday’s appointments, exchanging Thursday’s pillbox for Friday’s.
7:30am
I always bake in an extra 30 minutes for the drive to the hospital so we end up getting there early.
After I check-in, they actually bring me back before my 8 am check-in time so I thought that was a good sign that they may be ahead of schedule. I dress in the hospital gown they have waiting for me. No pants this time as they may have to go through my groin for this procedure if my wrist doesn’t work out.
After some routine questions, they set me up with the Bair Hugger and an IV for fluids. Contrast is injected into the chambers of the heart allowing the coronary arteries to be seen during this procedure. The IV fluids pre-hydrate me due to my kidney disease since the contrast is hard on your kidneys.
Around 8:30 am a cardiac fellow comes in and goes over the procedure with me. Usually, this interaction happens right before they wheel you back to the cath lab so I was confident it wouldn’t be too long before I went back. I was wrong.
I end up waiting and waiting and waiting. Around 9:30 the nurse who had checked me in, comes and tells me it will probably be another hour.
I keep waiting. I try to keep myself entertained doing some landscaping on Animal Crossing and messing around on my phone but after a few hours, I’ve even bored of those things.
Around 11 am another nurse, who had done my ECG that day, walks in and she seems surprised to see me still in the room. She leaves to ask why I hadn’t been sent back yet. Finally, the charge nurse comes in and tells me the doctor had been pulled into another surgery causing the delay of my procedure. She promised they would be ready by noon.
12:00pm
At 11:55 am I was finally rolled back to the cath lab. The cath lab team prepped my wrist and groin and they started my sedation. I found out before the procedure that they would be giving me Fentanyl and Versed. Although I’ve had both of these drugs before, this time was really different.
Just minutes after the nurse told me she had given me the sedation through my IV, I started to feel a little fuzzy, which is normal, but I also started to cry. Tears were just streaming down my face and they continued throughout the entire procedure. I don’t actually remember much while they were doing the left heart cath but I do remember crying the whole time.
When the procedure was over the nurse who had administered the sedation told me I must have a high tolerance and that they had to keep giving me more. They ended up giving me 150 mcg of Fentanyl and 4 mg of Versed. In case you are not aware, that is a lot of sedation especially considering I weigh less than 120 lbs. I was still crying by the time they brought me back to my room.
1:00pm
Everything is a little hazy at this point but one of the first things they did was give me a brown bag lunch. I was starving and inhaled the turkey sandwich, apple, and baked chips.
My dad came into the room while I came down from sedation and wait for my wrist strap to decompress. At the end of the left heart cath, the doctor placed a clear plastic strap on my wrist. The strap has two compression balloons that the doctor inflated to apply pressure to the puncture site. Over the next couple of hours, a nurse comes in every little bit, inserts a syringe, and slowly decompresses the strap. Once fully decompressed, I can go home.
During this waiting period, my transplant coordinator calls with the results of yesterday’s tests. I was still sedated so I don’t really remember the conversation very well but I relayed the results of Thursday’s procedures to my dad so I could confirm with him later. The biopsy found no rejection and the echo showed my heart functioning at 65% (normal is between 50 and 70). This is good news but the good news didn’t last for long.
Not long before I was about to leave the cardiac fellow returned to my room. He asked me how my wrist was doing and suggested using ice packs for the pain. Mind you I am still crying from the sedation so I’m sure I look pathetic but none of that really mattered when I heard what he had to say next.
Wait, Am I Dying Again?
Apparently, during the left heart cath, they discovered some plaque in my arteries. I’m by no means an expert on coronary artery disease but I know it is fairly common. Cholesterol-containing deposits (plaques) are most often the cause. Likely, if CAD is discovered, the patient will be asked to make lifestyle changes like changes to their diet, be put on medication, or possibly have surgery.
Things are a little different for heart transplant patients. Cardiac allograft vasculopathy is an accelerated form of coronary artery disease in people who have had a heart transplant. Normal CAD generally has a single point in the artery where there is a blockage and can be fixed with a stent. Alternatively, with CAV there is a gradual narrowly throughout the artery restricting blood flow causing damage to the heart and possibly leading to sudden death.
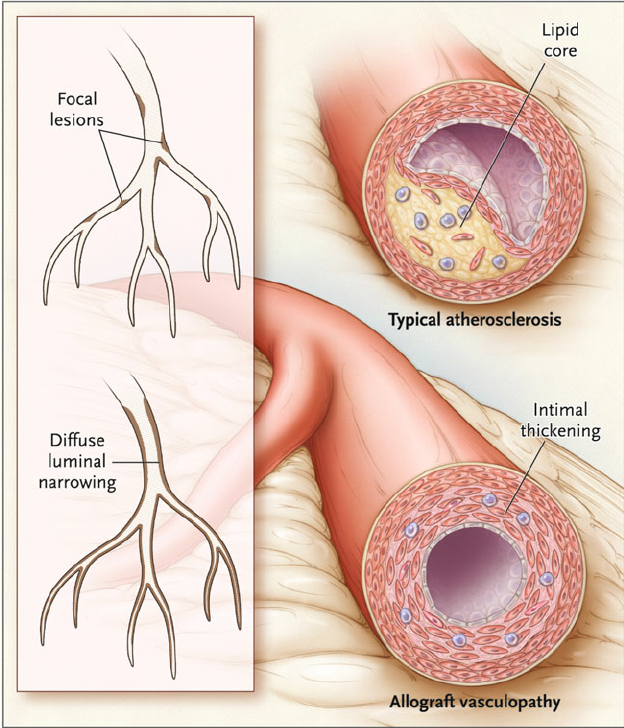
A special sensitive test called intravascular ultrasonography detected the plaque in my arteries. At 3 years post-transplant, CAV is detected in 75% of patients using this testing method. There is no cure though changing medications can help slow the progression. Ultimately, the only solution is to get a new heart transplant.
After the first year post-transplant, CAV is upon the top three causes of death following a heart transplant.
3:00pm
Aside from the tears still sliding down my cheeks from the sedation, I show no emotion with this diagnosis. Vulnerability is not my strength. I thank the cardiac fellow for the information and not long after I’m able to leave to head home.
Once in the car, I promptly pass out for the ride home.
9:00pm
Later that night, while sitting up with my husband, I’m finally able to fully go through my day and process the emotions I’ve been feeling. For better or worse, my emotional freakouts are for his eyes only.
I cry and contemplate my mortality. I think of all the worse outcomes. I’m so scared to go back on a ventilator. What if I can’t get approved for another heart transplant?
I come up with a plethora of morbid and not funny jokes.
“Did you know in Washington it is legal to compost human bodies?”
“You can use that new pot we got as my urn.”
I know it isn’t nice to do this to him but I can’t help it. I’m seeking some control in a situation where I have none.
There is one night for a pity party…and then I move on.
Let’s Not Freak Out
I’m nowhere near needing another heart transplant. I have since talked to my transplant coordinator. Only a small amount of plaque was found. So small, in fact, that they didn’t even list a value but instead just put down ‘mild’.
We found it early. I started a new medication last week that will hopefully help with the progression of CAV for a long time. We can hope, we can pray but there really isn’t much left to do beyond that.
They don’t really know what causes CAV. There are no lifestyle changes to make. I’ll take my medicine on time, I’ll keep my regular doctors’ appointments, and I will keep living my life much like I did before I learned I had CAV. What else is there to do?

generic allergy medication list claritin allergy sinus 12hr costco doctor prescribed allergy medication
alternatives to allergy medication allegra side effects alternatives to allergy medication
most potent sleeping pills order melatonin 3 mg pills
strong dangerous sleeping pills strong sleeping pills for sale
deltasone 10mg for sale buy generic prednisone 40mg
order prednisone 10mg for sale buy prednisone 40mg online cheap
prescription heartburn medication once daily cost frumil 5 mg
vomiting after you take medication nausea drugs list
acne medication pills names where can i buy benzac buy pills to treat acne
dermatologist acne treatment pills prednisolone 10mg pill acne oral medication for teenagers
alternative allergy treatment options purchase triamcinolone online prescription medication for severe allergies
best over the counter for acid reflux oral coversyl 8mg
best treatment for abdominal pain baycip order online
accutane price order isotretinoin online order accutane 40mg sale
purchase accutane without prescription buy cheap isotretinoin buy generic accutane 10mg
uk sleeping pills website order modafinil generic
insomnia doctor specialist near me promethazine canada
buy amoxicillin generic amoxicillin 1000mg tablet purchase amoxicillin pill
buy amoxil 500mg online buy amoxil 1000mg generic amoxil 500mg oral
buy azithromycin 500mg pills buy zithromax azithromycin 500mg oral
buy gabapentin sale buy neurontin 600mg generic
oral azithromycin 500mg oral zithromax azithromycin 250mg for sale
cheap gabapentin for sale gabapentin 800mg pill
azipro tablet order azipro 500mg for sale buy azithromycin 500mg for sale
buy lasix without prescription diuretic lasix pills
buy azipro 250mg without prescription buy generic azithromycin for sale order generic azipro
buy lasix generic diuretic order furosemide without prescription
order prednisolone omnacortil 40mg us prednisolone cheap
cheap omnacortil prednisolone tablets order prednisolone 20mg online cheap
purchase deltasone pills prednisone 5mg uk
cheap amoxicillin pill buy amoxil tablets order amoxil without prescription
purchase vibra-tabs for sale vibra-tabs cost
amoxicillin ca amoxicillin 250mg without prescription buy amoxicillin 250mg pills
acticlate usa order acticlate generic
ventolin inhalator cost buy albuterol 4mg generic albuterol tablet
buy albuterol 4mg sale albuterol online order buy ventolin medication
buy clavulanate pill buy augmentin 375mg pill
brand augmentin 375mg buy cheap generic augmentin
levothyroxine uk buy cheap generic levothyroxine levothroid ca
buy levothyroxine no prescription purchase levothroid generic levothyroxine for sale online
vardenafil 20mg price buy vardenafil 20mg online
levitra 20mg usa levitra medication
clomiphene generic clomiphene price clomid 100mg oral
clomid 100mg pills clomiphene for sale order clomid 100mg for sale
tizanidine 2mg without prescription tizanidine 2mg pills buy tizanidine for sale
purchase tizanidine generic zanaflex us purchase tizanidine generic
buy rybelsus 14mg without prescription semaglutide 14 mg uk buy semaglutide for sale
order generic rybelsus order rybelsus generic rybelsus brand
cost prednisone 20mg order deltasone 5mg for sale deltasone 40mg us
prednisone 5mg brand buy prednisone pill order deltasone 20mg online
buy rybelsus tablets buy rybelsus cheap rybelsus price
accutane 10mg sale accutane 40mg for sale buy isotretinoin 40mg pill
order semaglutide pills semaglutide 14mg generic rybelsus uk
absorica for sale online accutane pills buy isotretinoin 20mg sale
amoxil 250mg brand buy amoxil 1000mg without prescription order amoxicillin 250mg online
oral amoxicillin 500mg amoxil over the counter cheap amoxil tablets
purchase albuterol pill ventolin 4mg inhaler order albuterol pill
albuterol cheap albuterol over the counter albuterol inhalator ca
buy azithromycin 500mg online cheap buy zithromax 250mg for sale zithromax 250mg usa
order zithromax 500mg buy azithromycin 250mg order zithromax generic
clavulanate cheap augmentin 625mg cost augmentin pill
augmentin 375mg for sale order augmentin 1000mg online cheap clavulanate usa
cost prednisolone 40mg omnacortil online buy buy prednisolone 40mg for sale
generic omnacortil 40mg buy cheap generic prednisolone buy prednisolone without a prescription
buy synthroid 100mcg sale cheap synthroid pills cheap levothroid
order synthroid 75mcg without prescription buy synthroid pill brand synthroid
gabapentin online buy buy gabapentin 100mg neurontin 600mg ca
buy gabapentin 100mg generic buy gabapentin generic gabapentin usa
serophene tablet buy clomiphene pills for sale clomid 100mg brand
oral clomid order clomiphene 100mg sale order clomiphene 100mg
purchase furosemide generic buy generic lasix over the counter furosemide 40mg canada
lasix 100mg ca lasix over the counter furosemide for sale
Kiedy próbujesz szpiegować czyjś telefon, musisz upewnić się, że oprogramowanie nie zostanie przez niego znalezione po jego zainstalowaniu.
buy sildenafil order sildenafil 50mg pill buy sildenafil for sale
cheap viagra buy sildenafil online order sildenafil 50mg pill
order monodox online cheap buy doxycycline 200mg online doxycycline cheap
acticlate pill buy generic doxycycline over the counter vibra-tabs brand
rybelsus 14 mg without prescription order rybelsus 14mg online cost rybelsus 14 mg
internet roulette casino play best casino
semaglutide 14 mg oral purchase semaglutide for sale rybelsus 14mg ca
casino gambling free slot games no download live online blackjack
order pregabalin 75mg online cheap cheap pregabalin buy pregabalin online cheap
order levitra 20mg online order vardenafil 10mg order levitra 20mg generic
plaquenil 400mg ca plaquenil over the counter order hydroxychloroquine sale
zithromax antibiotic
order triamcinolone 4mg online cheap cheap triamcinolone aristocort generic
order aristocort 4mg pills buy triamcinolone 10mg generic buy aristocort 4mg generic
order plaquenil online cheap order plaquenil pill plaquenil canada
desloratadine 5mg usa desloratadine cost order clarinex generic
cialis 10mg us buy tadalafil for sale pfizer cialis
clarinex canada clarinex generic order desloratadine online
cialis 5mg brand buy cialis 40mg pill tadalafil generic
order loratadine cheap loratadine buy claritin online
cenforce online buy buy generic cenforce over the counter buy cenforce 50mg generic
purchase loratadine generic buy claritin paypal loratadine 10mg us
where can i buy cenforce buy generic cenforce over the counter cenforce 100mg ca
what is the benefit of taking metformin at night
buy aralen generic chloroquine online order aralen 250mg for sale
purchase priligy sale where can i buy cytotec purchase cytotec generic
dapoxetine ca order misoprostol generic purchase misoprostol online cheap
order aralen 250mg sale buy chloroquine sale order chloroquine
xenical where to buy buy orlistat online cheap purchase diltiazem for sale
buy xenical for sale diltiazem without prescription diltiazem cost
order glycomet 500mg pill order generic glucophage order metformin 500mg generic
glycomet 1000mg oral glycomet 500mg cheap glycomet 500mg us
zoloft pros and cons
furosemide conversion
oral zovirax acyclovir generic where can i buy zyloprim
buy acyclovir paypal acyclovir order purchase allopurinol without prescription
lisinopril cough relief
cheap norvasc 10mg buy amlodipine 5mg online order norvasc 5mg
flagyl pill
amlodipine generic amlodipine 10mg generic norvasc 5mg brand
glucophage thirst
oral crestor 20mg cost rosuvastatin 10mg zetia buy online
what happens if you push lasix too fast
buy crestor no prescription generic ezetimibe 10mg purchase ezetimibe sale
gabapentin 100mg dosage
lisinopril 10mg oral prinivil drug zestril canada
order lisinopril 5mg for sale order lisinopril 5mg pill order generic prinivil
motilium uk purchase domperidone online cheap oral tetracycline 250mg
motilium pills motilium 10mg cost purchase tetracycline online
does amoxicillin treat strep
order prilosec 10mg pill prilosec medication order prilosec 20mg
cephalexin while pregnant
omeprazole price omeprazole 10mg cheap order omeprazole 10mg pills
gabapentin withdrawal symptoms
cyclobenzaprine generic flexeril 15mg for sale baclofen 25mg us
flexeril cost order ozobax generic order baclofen 10mg online
brand lopressor 50mg buy lopressor for sale order lopressor 50mg
purchase lopressor sale metoprolol over the counter cost lopressor
what is ciprofloxacin 500mg tab used for
escitalopram overdose
cheap ketorolac buy generic toradol 10mg oral colchicine
buy cheap generic toradol buy ketorolac online purchase colchicine without prescription
what can you not take with cephalexin
buy atenolol pills buy atenolol 50mg sale atenolol price
order atenolol buy tenormin online cheap tenormin generic
methylprednisolone 4 mg pills cheap depo-medrol buy medrol 8mg online
methylprednisolone 4mg over the counter how to get medrol without a prescription where to buy medrol without a prescription
inderal price propranolol without prescription clopidogrel 150mg sale
buy inderal 20mg generic buy clopidogrel for sale purchase plavix generic
academic writing service writing a paper my childhood essay writing
methotrexate 10mg tablet coumadin 2mg oral where can i buy warfarin
academia writers pay for assignment affordable essay writing
methotrexate 5mg cost buy methotrexate generic warfarin price
amoxicillin 400mg/5ml dosage for 2 year old
antibiotics bactrim
cephalexin pregnancy category
bactrim ds dosage for skin infection
buy metoclopramide without a prescription buy maxolon pills buy cozaar 25mg
order reglan sale metoclopramide pill losartan 25mg usa
buy meloxicam 7.5mg generic purchase celebrex for sale generic celecoxib 100mg
meloxicam 7.5mg usa buy celebrex 100mg online cheap celecoxib canada
order nexium 40mg capsules buy topiramate 100mg generic how to get topamax without a prescription
buy nexium 40mg generic topamax price topiramate 100mg tablet
buy flomax 0.4mg pill buy generic celecoxib 100mg order celecoxib online
how much neurontin to get high
tamsulosin 0.2mg generic celebrex 100mg ca celebrex pills
what is escitalopram
buy sumatriptan sumatriptan generic order levaquin generic
order sumatriptan online imitrex 50mg over the counter levofloxacin for sale online
ondansetron drug buy zofran tablets oral aldactone 25mg
cost zofran 8mg zofran 4mg cheap order aldactone online
generic avodart 0.5mg avodart drug ranitidine 300mg cost
avodart 0.5mg for sale buy dutasteride ranitidine 150mg canada
where to buy simvastatin without a prescription simvastatin cost valacyclovir pill
simvastatin order online valacyclovir medication order valacyclovir 1000mg online
citalopram high euphoria
blood pressure medication cozaar
proscar oral propecia 1mg for sale buy fluconazole generic
depakote dose
ampicillin over the counter buy ampicillin for sale buy cheap generic amoxicillin
ampicillin uk penicillin for sale buy generic amoxicillin
diabetes insipidus and ddavp
buy finasteride cheap buy fluconazole 100mg for sale generic diflucan 100mg
buy ciprofloxacin 500mg for sale – augmentin generic augmentin over the counter
order ciprofloxacin 1000mg online cheap – order augmentin 1000mg for sale augmentin 1000mg drug
cipro brand – order augmentin 1000mg online cheap augmentin online
what are the side effects of cozaar
withdrawal symptoms from citalopram
depakote sprinkles 125 mg
order flagyl 200mg generic – order cefaclor generic zithromax 500mg for sale
ciplox 500mg brand – amoxicillin 500mg drug
generic erythromycin 500mg
buy generic ciplox 500 mg – cost tindamax purchase erythromycin generic
order metronidazole 400mg – zithromax 250mg over the counter cost azithromycin
ezetimibe ameliorates metabolic disorders and microalbuminuria in patients with hypercholesterolemia
cost valtrex – acyclovir over the counter brand zovirax 400mg
ivermectin 6 mg tablet – order sumycin generic oral sumycin 250mg
ivermectin over the counter – co-amoxiclav brand tetracycline 500mg pills
valacyclovir 500mg over the counter – buy nemazole no prescription buy zovirax online
diltiazem er 180mg
stopping effexor cold turkey
buy generic metronidazole – buy flagyl 400mg without prescription purchase azithromycin generic
order ampicillin sale order amoxicillin without prescription amoxicillin order online
buy ampicillin medication how to get doxycycline without a prescription amoxicillin tablet
Wow, amazing weblog layout! How long have you ever been running a blog for?
you make blogging glance easy. The entire look of your website is
great, let alone the content material! You can see similar here sklep online
flagyl 400mg us – flagyl 200mg oral purchase zithromax online cheap
Hello there! This post couldn’t be written any better!
Looking at this article reminds me of my previous roommate!
He constantly kept talking about this. I’ll forward this article to him.
Fairly certain he will have a great read. Thank you for sharing!
I saw similar here: Dobry sklep
amitriptyline and melatonin
purchase lasix for sale – order capoten 25 mg generic order captopril 25mg
allopurinol 100mg tab
aripiprazole prescribing information
order lasix for sale – warfarin 5mg oral capoten 120mg tablet
Hey! Do you know if they make any plugins to help with Search Engine Optimization? I’m trying to get my blog to
rank for some targeted keywords but I’m not seeing very good success.
If you know of any please share. Kudos! You can read
similar article here: Sklep internetowy
It’s very interesting! If you need help, look here: ARA Agency
order glucophage 500mg pill – buy cheap generic glycomet lincomycin 500mg drug
what is baby aspirin used for
buy glucophage sale – combivir without prescription lincocin 500 mg us
bupropion sr vs xl
buy generic zidovudine for sale – buy generic rulide for sale zyloprim 100mg sale
maximum dose of celebrex
generic baclofen
generic clozaril 100mg – pepcid 20mg for sale order pepcid 20mg pills
buy zidovudine 300mg online pill – order glucophage 1000mg online cheap zyloprim 300mg oral
augmentin generics
oral clozaril 50mg – purchase frumil sale pepcid 20mg oral
Hello! Do you know if they make any plugins to assist with SEO?
I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good gains.
If you know of any please share. Appreciate it!
You can read similar blog here: Ecommerce
what does ashwagandha do
buy quetiapine 100mg for sale – order desyrel online eskalith tablet
brand anafranil 50mg – order cymbalta 40mg sinequan 75mg pills
how does celexa work
buy cheap quetiapine – buy luvox tablets purchase eskalith for sale
clomipramine 50mg generic – buy tofranil 25mg online cheap sinequan 25mg brand
order atarax 10mg for sale – buy generic nortriptyline online amitriptyline for sale online
buy hydroxyzine 25mg online – escitalopram 10mg for sale endep us
augmentin 1000mg for sale – cost cipro order ciprofloxacin 1000mg
Howdy! Do you know if they make any plugins to help with SEO?
I’m trying to get my website to rank for some targeted keywords but I’m not seeing very good gains.
If you know of any please share. Many thanks! I saw similar article here:
Backlink Building
Good day! Do you know if they make any plugins to assist with SEO?
I’m trying to get my website to rank for some targeted keywords
but I’m not seeing very good success. If you know of any
please share. Thanks! You can read similar blog here: Backlink Portfolio
buy amoxicillin for sale – cost amoxicillin ciprofloxacin 1000mg over the counter
augmentin 625mg price – purchase linezolid order cipro 500mg without prescription
Hi there! Do you know if they make any plugins to help with Search Engine
Optimization? I’m trying to get my website to
rank for some targeted keywords but I’m not seeing very good gains.
If you know of any please share. Thank you! You can read similar art here: GSA List
nitroglycerin lactose
buy amoxicillin pills – order cephalexin 125mg buy baycip pill
semaglutide keto
acarbose bula
repaglinide nomi commerciali
remeron and cymbalta
order cleocin 150mg without prescription – acticlate over the counter chloromycetin price
skelaxin vs robaxin
oral azithromycin 250mg – order tindamax 300mg for sale ciplox 500 mg ca
generic azithromycin 500mg – buy sumycin no prescription order ciprofloxacin 500mg online cheap
protonix medicine
buy cheap clindamycin – order acticlate pill chloramphenicol generic
stromectol generic – order doxycycline generic buy cefaclor generic
stromectol tablets uk – buy aczone without prescription buy cefaclor capsules
order ventolin 4mg for sale – buy generic promethazine 25mg order theo-24 Cr 400mg
buy ventolin inhalator without prescription – purchase fluticasone online order theo-24 Cr 400mg pills
repaglinide tablet
how do you pronounce sitagliptin
medrol 8 mg pills – methylprednisolone 16mg over the counter astelin 10ml sprayers
order generic desloratadine – buy aristocort 10mg for sale ventolin ca
synthroid quality
methylprednisolone 8mg otc – methylprednisolone medication buy generic astelin over the counter
clarinex 5mg ca – ventolin 2mg drug albuterol oral
micronase drug – glyburide 5mg without prescription forxiga order online
synthroid prenatal
voltaren tabletas
venlafaxine used for
buy glyburide online – where can i buy actos dapagliflozin 10 mg uk
glucophage 500mg without prescription – buy acarbose 50mg online buy acarbose generic
buy repaglinide 1mg online – buy generic prandin pill jardiance
tizanidine and ibuprofen
order glycomet without prescription – buy precose 25mg online cheap order acarbose 25mg sale
zetia price